Lag screw and buttress plate
1. Principles
Lag screw principles
As the thread advances in the main body of the tibia, the head pushes the medial fragment towards the tibia.
The smooth shaft of the screw prevents any significant hold between the screw and the surrounding bone.
The length of the screw shaft must be chosen so that the threaded part of the screw lies fully beyond the fracture line and within the epiphyseal cancellous bone of the distal tibia.
To prevent the screw head from sinking into the thin cortex, the use of a washer is recommended.
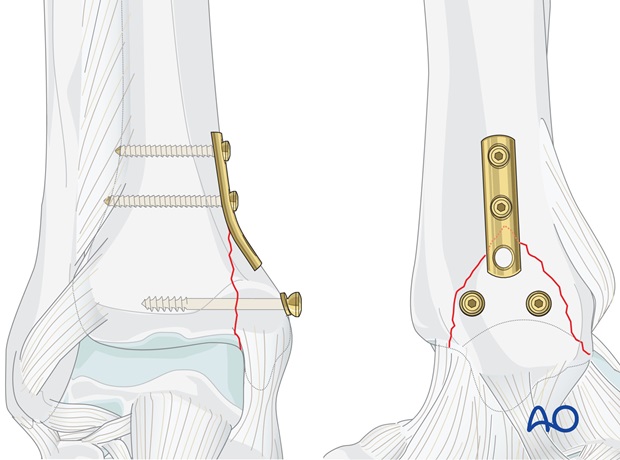
Buttress plate
The function of a buttress plate is to neutralize any vertical shearing force.
2. Patient preparation and approach
The patient may be placed in the following positions:
For this procedure a medial approach is normally used.
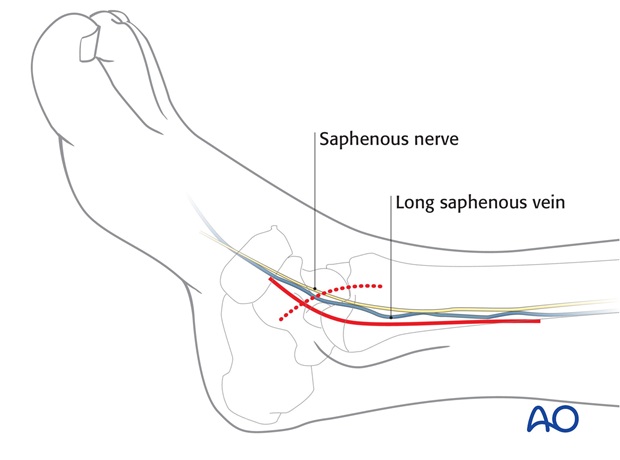
3. Reduction
Cleaning the fracture site
Remove any small, loose fragments which may prevent anatomic reduction and free the periosteum from the bone edges.
It is important to visualize and inspect the joint, searching for bone and cartilage fragments detached from the medial malleolus or from the talus, and any impaction of the articular surface at the margin of the fracture. If the articular surface has been impacted, this must carefully disimpacted before the medial fragment is reduced.
Anatomical reduction
Reduce the fracture anatomically with the help of small pointed reduction forceps. Take care with the soft tissues.
Depending on fracture configuration and size of the fragment you may need to use large pointed reduction forceps through a lateral stab incision.
Do not strip the periosteum more than necessary.
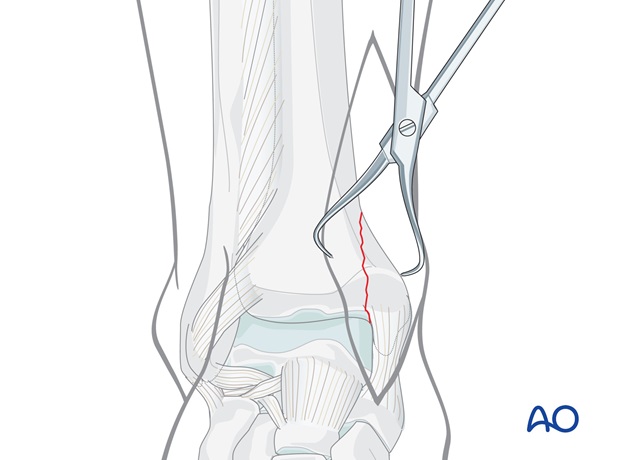
In the presence of an impacted medial corner fragment, gently open the main vertical fracture plane by retraction of the medial malleolus medially (opening the book). The impacted “corner” fragment, usually identifiable by its articular cartilage, after irrigation if necessary, can then be seen.
Disimpact and carefully tease back the fragment into its anatomical position.
Then close the book by careful reduction of the medial malleolus.

Preliminary fixation
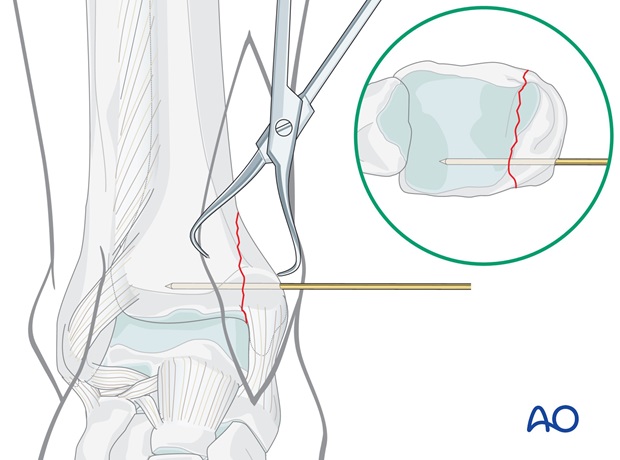
Insert a 1.6 mm K-wire as perpendicularly as possible to the fracture plane, about 1 cm proximal to the level of the horizontal tibiotalar joint line.
As decided in preoperative planning, this K-wire should be placed posteriorly in order not to interfere with the planned position of the plate.
Check the reduction under image intensification.
4. Fixation
Drilling
With the protection of a drill sleeve, drill a 2.5 mm hole as perpendicularly as possible to the fracture plane and parallel to the K-wire. Do not drill the far lateral cortex.
Avoid penetration of the ankle joint and the syndesmosis.

Tap cortical bone
Measure the drill depth and then tap the near cortex only with the 4.0 mm cancellous bone tap, using the protection sleeve.
Insert anterior lag screw
Insert the chosen 4.0 mm cancellous bone screw so that it comes to rest with its threads completely in main body of the distal tibia.
The use of a washer is recommended, especially in osteoporotic bone.
Insert the screw without excessive tightening.
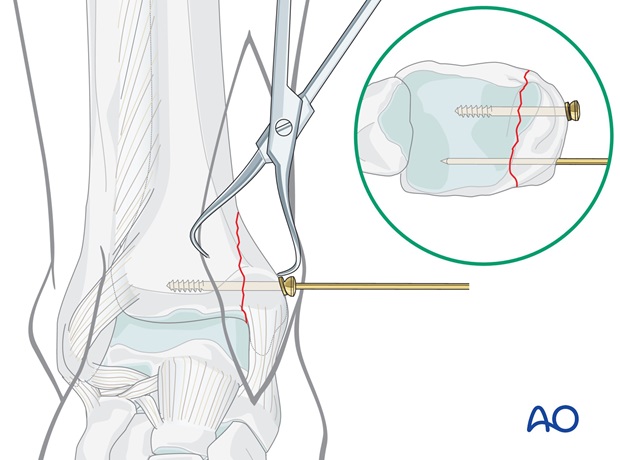
Insert posterior lag screw
Remove the K-wire and widen its track with a 2.5 mm drill through a protection sleeve.
After measuring the length and tapping the near cortex, insert the second 4.0 mm cancellous bone screw, fitted with a washer.
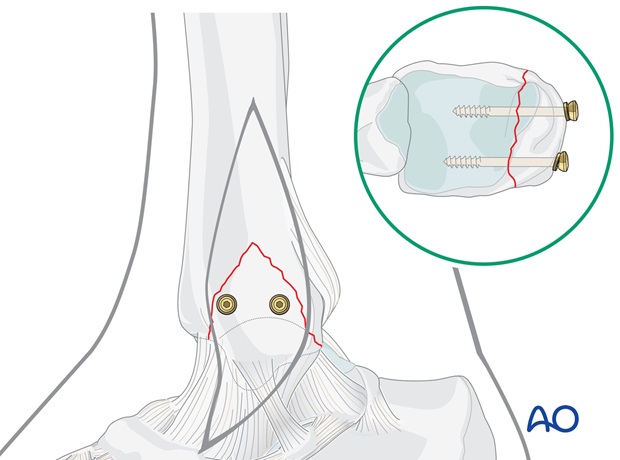
Prepare plate application
Use a 3 hole one-third tubular plate to buttress this shear fracture.
Position the plate firmly by hand so that two holes lie on the main body of the tibia and one hole on the malleolar fragment. Plan the position of the first proximal screw near the fracture. This screw must be located in the main fragment, 3 mm proximal to the apex of the fracture plane.
Use the 2.5 mm drill bit and protection sleeve. Drill both cortices, but exercise great care not to over-penetrate laterally.
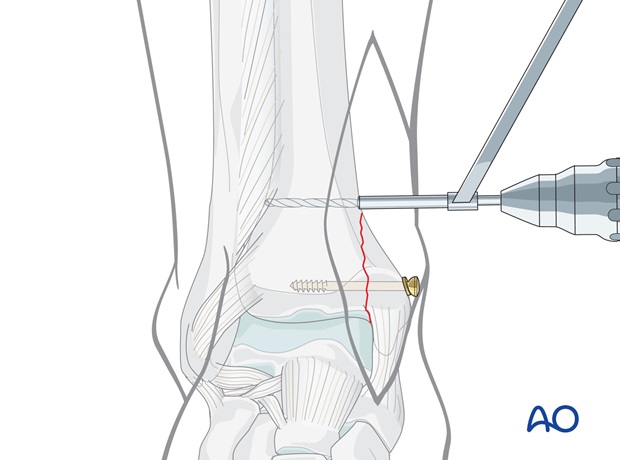
Buttressing effect
Measure the depth and tap both cortices with the 3.5 mm tap, using the protection sleeve.
Carefully apply the uncontoured plate. Insert the first, more distal cortex screw. By tightening the screw, the plate will act as a buttress on the distal fragment.
Finally, insert the second 3.5 mm cortex screw as described above.
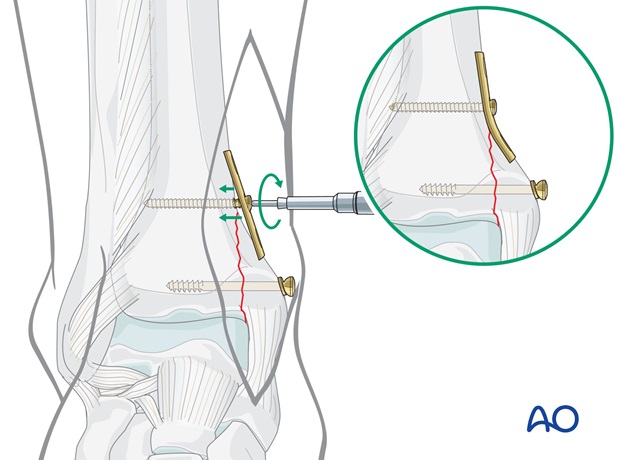
5. Postoperative treatment of infra- and trans-syndesmotic malleolar fractures
A bulky compression dressing and a lower leg backslab, or a splint, are applied, and the limb is kept elevated for the first 24 hours or so, in order to avoid swelling and to decrease pain.
In anatomically reconstructed, stable malleolar fractures, early active exercises and light partial weight bearing are encouraged after day one. In osteoporotic bone, weight bearing should be postponed.
X-ray evaluation is made after 1 week and then monthly until full healing has occurred. Progressive weight bearing is recommended as tolerated.













