ORIF - Headless screw fixation
1. General considerations
The fragment is stabilized with headless screws depending on the fracture characteristics.
In a simple capitellar fracture, an anterior-to-posterior screw trajectory is often used and described in this procedure.
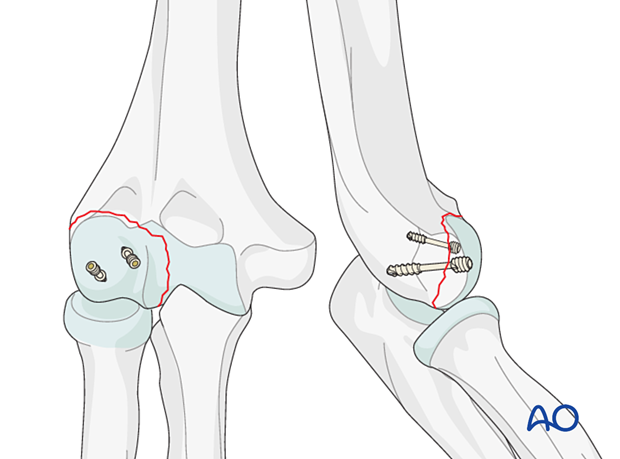
Extent of fracture extension into the trochlea
Involvement of the trochlea requires more central and medial exposure for fracture reduction and screw placement.
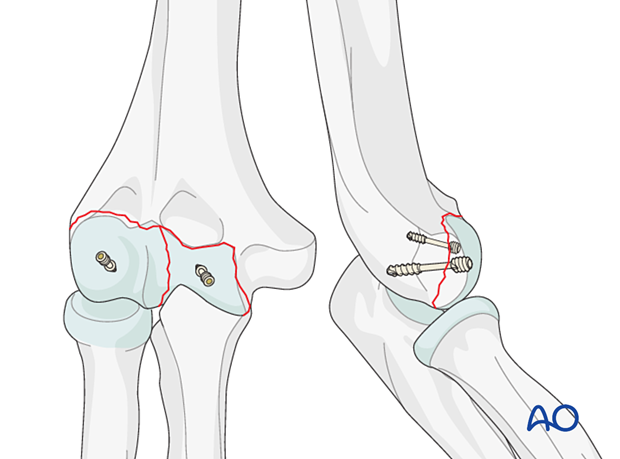
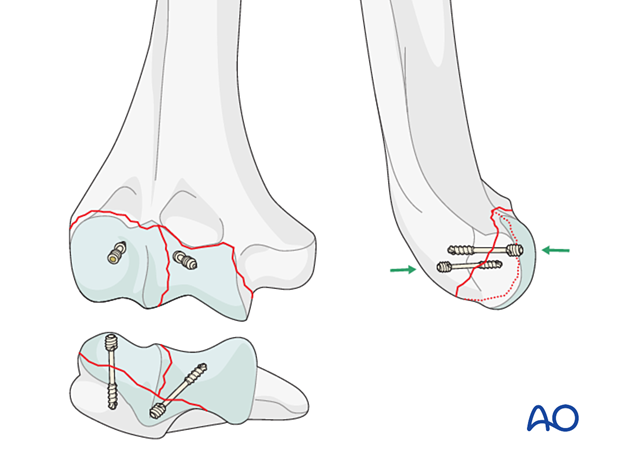
Extent of posterior fracture extension
If there is posterior trochlear comminution of a posterior transverse fracture of the capitellum or trochlea, then a posterior approach extended into the olecranon fossa is recommended (eg, olecranon osteotomy).
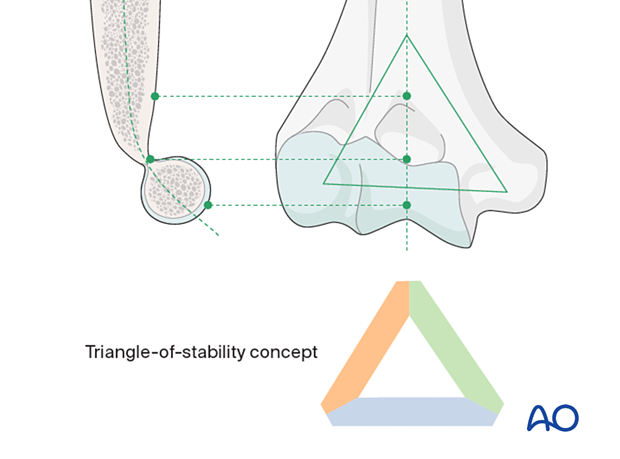
Triangle-of-stability concept
The mechanical properties of the distal humerus are based on a triangle of stability, comprising the medial and lateral columns and the articular block (see also the anatomical concepts).
Screw selection
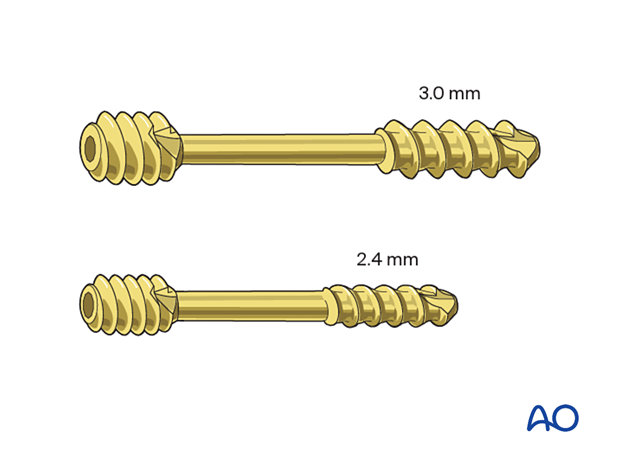
Screw fixation can be achieved with cannulated headless compression screws or traditional noncannulated screws.
Headless screws (2.4 or 3.0 mm) are used in the articular segments.
Insertion of a cannulated headless screw is described in this procedure.
2. Patient preparation and approaches
Patient positioning
This procedure is usually performed with the patient in a supine position.
For the treatment of a posterior fracture extension, a lateral decubitus or prone position is needed for a posterior approach.

Approaches
The lateral approach is the most commonly used and is detailed here.
Elevate the origins of the extensor carpi radialis longus (ECRL) and extensor carpi radialis brevis (ECRB) from the anterior aspect of the humerus, along with the brachioradialis.
Split the interval between the ECRB and the extensor digitorum communis (EDC). Take care not to extend posteriorly to the midpoint of the radial head to protect the lateral collateral ligament.
Take care when extending the EDC split distally to protect the posterior interosseous nerve.
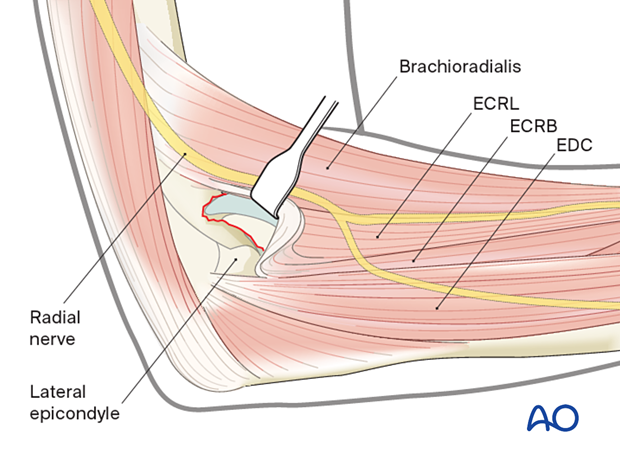
The anterior approach may be used if there is no posterior involvement.
For the treatment of a posterior fracture extension, a posterior approach with olecranon osteotomy or triceps-elevating approach can be used.
3. Open reduction
The fracture fragment should be apparent in the anterior aspect of the joint.
With trochlear fracture involvement, the brachioradialis also needs to be elevated.
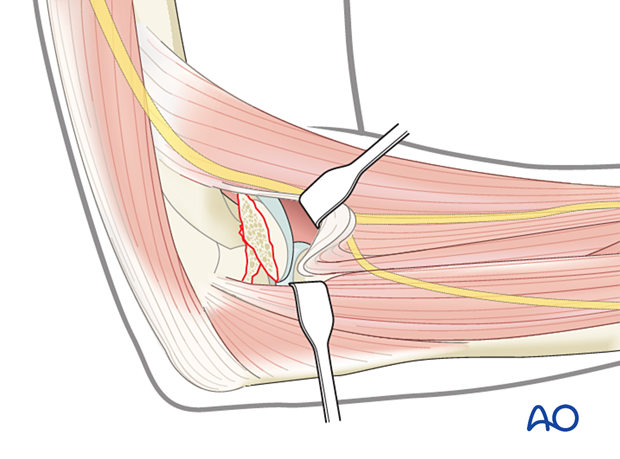
Clearing the fracture site
Clear the fracture of any hematoma, loose pieces of bone, or interposed tissue.
Inspect the joint surfaces to ensure that there is no additional intraarticular fracture extension.
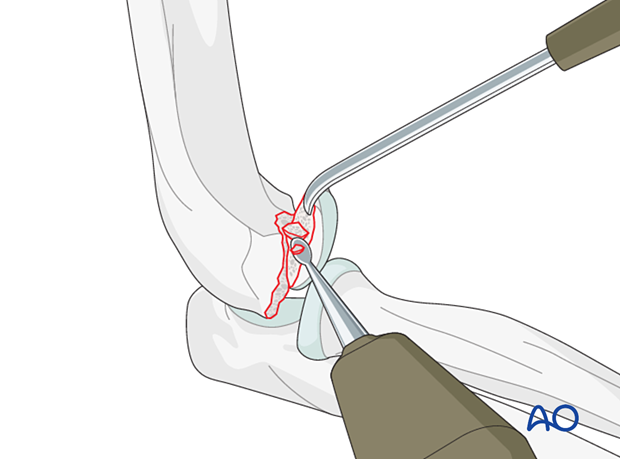
Reduction
Align the fracture and maintain reduction with a small hook or pick.
Monitor fracture reduction by realigning the metaphyseal and articular fracture lines.
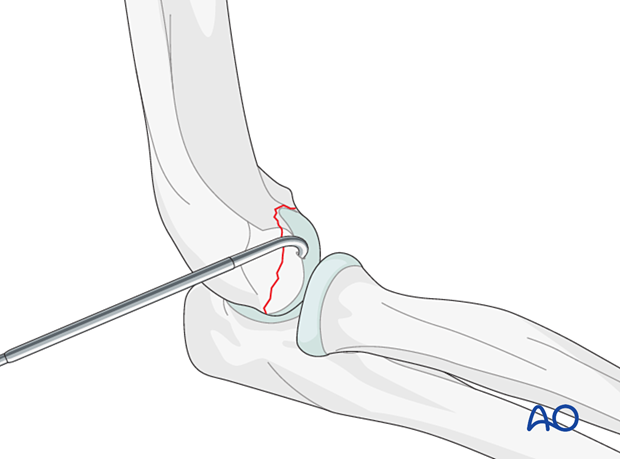
Temporary fixation
Insert K-wires in an AP direction across the fracture site to stabilize the reduction.
The guide wires for the cannulated headless screws may act as the provisional fixation wires.
If necessary, check the reduction and provisional fixation with image intensification.
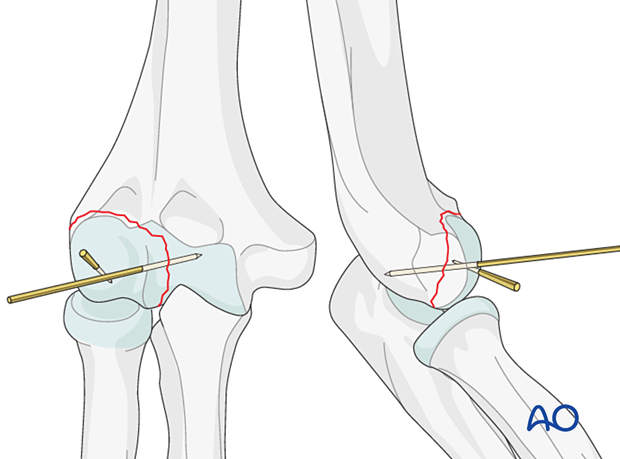
4. Headless screw fixation
Planning for screw position
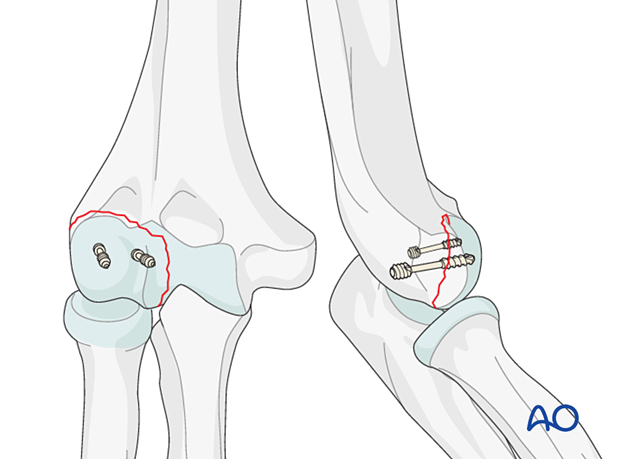
The screw trajectory in a simple capitellar fracture is usually anterior to posterior perpendicular to the fracture plane, if possible.
The more lateral screw can be angled in a proximal direction to avoid the articular surface.
The headless screw needs to be below the articular surface and should not penetrate the posterior articular surface.
Principle
Complete the entire sequence of drilling and screw insertion for each screw before inserting the next screw.
Drilling
Insert the guide wire.
Drill the pilot hole for the screw to the appropriate depth, using the cannulated drill bit placed over the guide wire.
Take care when removing the drill not to dislodge or remove the K-wire.
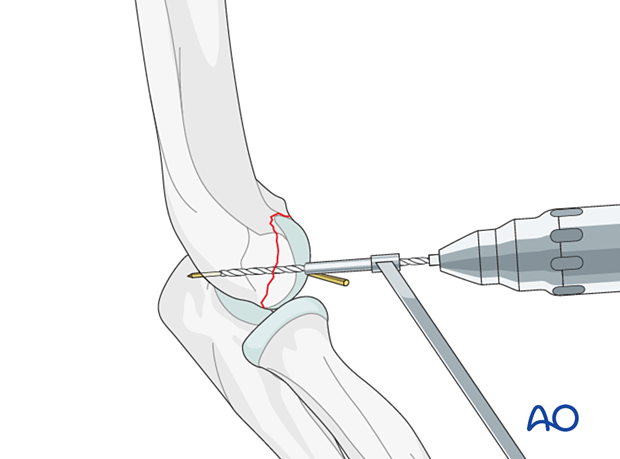
Screw insertion
Insert the chosen screw over the wire, then remove the guide wire.
Insert the subsequent screws in the same way.
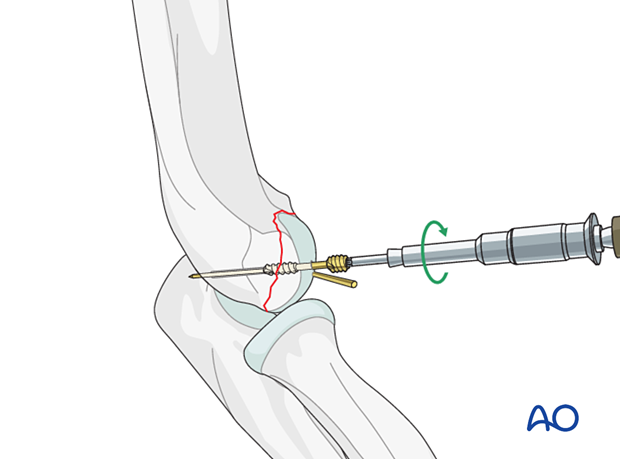
Final construct

5. Alternative: posterior screw fixation
Posterior screw placement can be possible after elevation of the anconeus and the triceps from the humerus.
This allows for anterior and posterior screw placement.
6. Final assessment
Visually inspect the fixation and manually check for fracture stability.
Repeat the manual check under image intensification.
7. Aftercare
Introduction
The rehabilitation protocol consists usually of three phases:
- Rehabilitation until wound healing
- Rehabilitation until bone healing
- Functional rehabilitation after bone healing
Immediate aftercare
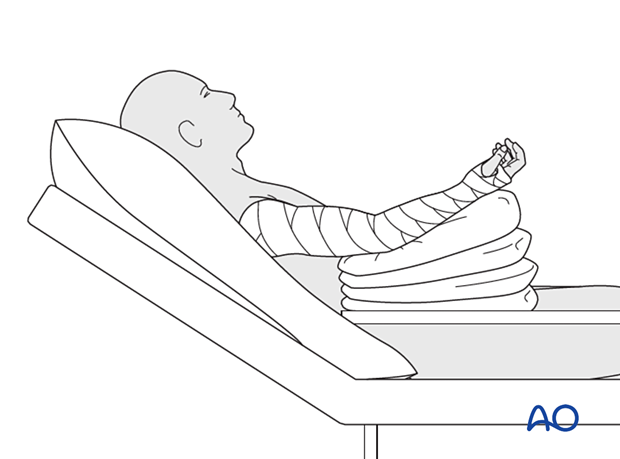
The arm is bandaged to support and protect the surgical wound.
The arm is rested on pillows in slight flexion of the elbow so that the hand is positioned above the level of the heart.
Short-term splinting may be applied for soft-tissue support.
Neurovascular observations are made frequently.
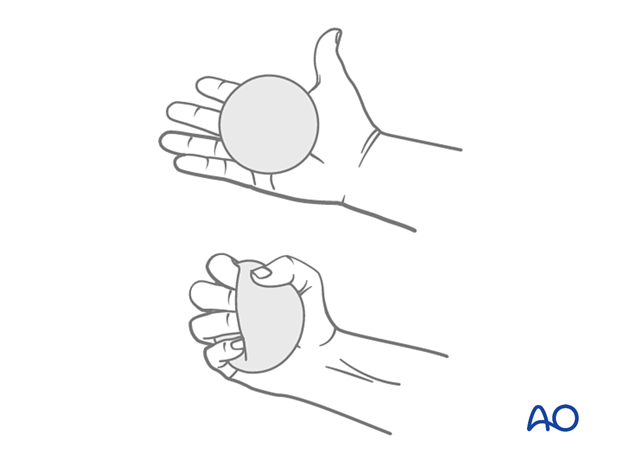
Hand pumping and forearm rotation exercises are started as soon as possible to reduce lymphedema and to improve venous return in the limb. This helps to reduce postoperative swelling.
Mobilization until wound healing
Gravity-eliminated active assisted exercises of the elbow should be initiated as soon as possible, as the elbow is prone to stiffness:
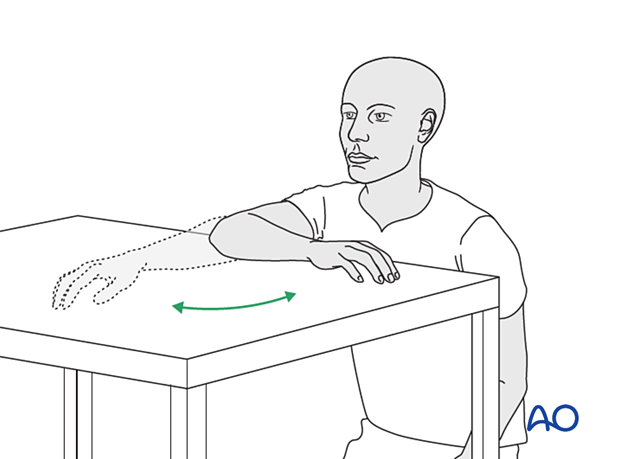
- The bandages are removed, and the arm rested on a side table
- Flexion/extension of the arm at the elbow is encouraged in a gentle sweeping movement on the tabletop as far as comfort permits (as illustrated)
- Full pronation and supination in protected arm position is encouraged
- Exercises are performed hourly in repetitions, the number of which is governed by comfort
- Between periods of exercise, the elbow is rested in the elevated position for at least the first 48 hours postoperatively
- Keep the arm elevated between periods of exercise until the wound has healed
Rehabilitation until bone healing
Active patient-directed range-of -motion exercises should be encouraged without the routine use of splintage or immobilization.
Avoid forceful motion, repetitive loading, or weight-bearing through the arm.
A simple compressive sleeve can provide proprioceptive feedback which can help regain motion and avoid cocontraction.
No load-bearing (ie, pushing, pulling, or carrying weights) or strengthening exercises are allowed until early fracture healing is established by x-ray and clinical examination.
This is usually a minimum of 8–12 weeks after injury. Weight-bearing on the arm should be avoided until bony union is assured.
The patient should avoid resisted extension activities, especially after a triceps-elevating approach or olecranon osteotomy.
Rehabilitation after bone healing
When the fracture has united, a combination of active functional motion and kinetic chain rehabilitation can be initiated.
Active assisted elbow motion exercises are continued. The patient bends the elbow as much as possible using his/her muscles while simultaneously using the opposite arm to gently push the arm into further flexion. This effort should be sustained for several minutes; the longer, the better.
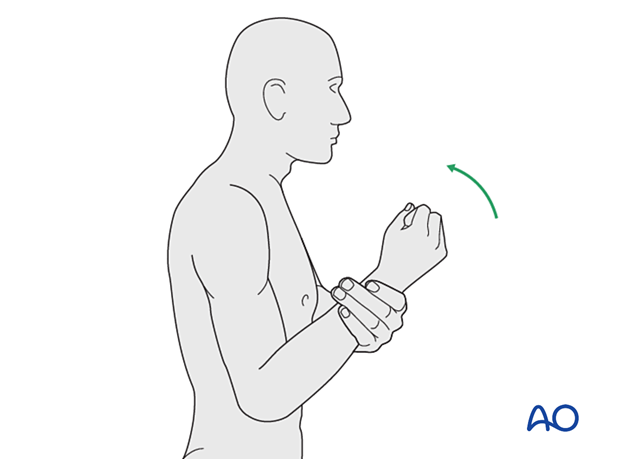
Next, a similar exercise is performed for extension.

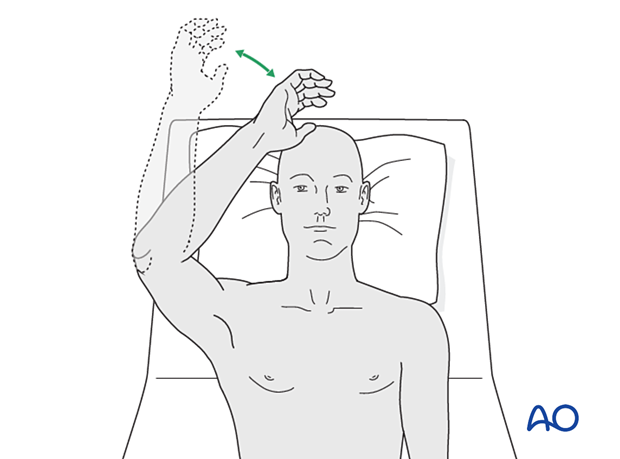
If the patient finds it difficult to accomplish these exercises when seated, then performing the same exercises when lying supine can be helpful.
Implant removal
Generally, the implants are not removed. If symptomatic, hardware removal may be considered after consolidated bony healing, usually no less than 6 months for metaphyseal fractures and 12 months when the diaphysis is involved. The avoidance of the risk of refracture requires activity limitation for some months after implant removal.













