Closed treatment
1. Splint application
A decision has to be made whether or not the reduction of the palatal fracture is to be performed using a palatal splint. A palatal splint is recommended if the segments of tooth–bone units are relatively intact.
If the tooth–bone units are severely damaged or comminuted then a palatal splint alone may be insufficient.
In complex (comminuted) palatal fractures where the tooth–bone units are relatively intact, most surgeons consider utilization of a palatal splint critical. In these cases, it is necessary to take dental impressions, make dental models, and from these models make a palatal splint. (If dental models are available from previous treatment, this may be helpful.)
In these complex cases, cuts need to be made in the maxillary portion of the dental model to determine the premorbid contour of the maxillary arch. This is achieved by using the mandibular model. Once the maxillary cast model has been adjusted to its premorbid shape, the palatal splint is made using that maxillary model.
The palatal splint is then fixed on the palate, also using arch bars and peridental wires. Depending on the stability of the palatal unit, and of the postoperative airway, as well as any complicating issues of other midface fractures, the surgeon may choose to leave the patient in postoperative MMF.
In this photograph, dental impressions have been taken, models have been made, …
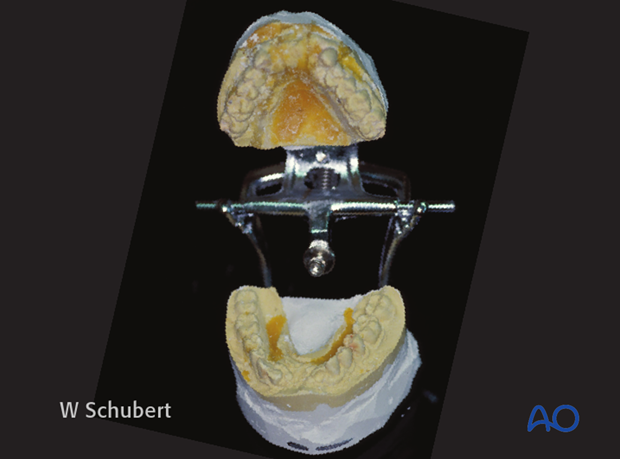
… and a clear plastic palatal splint has been made.
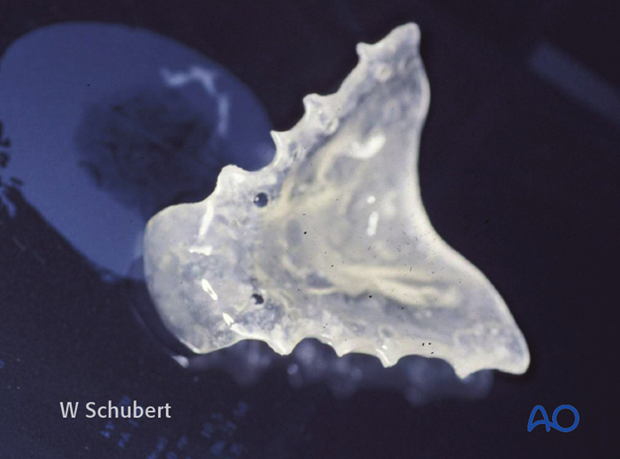
2. Reduction
Closed treatment of complex palatoalveolar injuries preserves the blood supply of the comminuted segments.
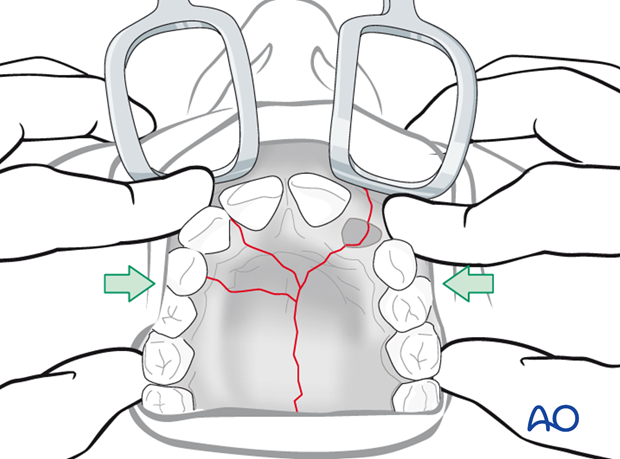
Perform reduction by applying pressure laterally on the two maxillary halves to reduce the splayed fracture. This maneuver needs to be performed while the palatal splint is in place, as the splint offers the best guide as to whether an adequate reduction has been achieved. It may be necessary to continue this pressure while applying the arch bars. There may be an advantage of applying wires from the splint to the arch bar. It may be necessary in some cases to wire the splint to the teeth, and the arch bars to the teeth independently.
Depending on the degree of dentoalveolar trauma one may not be able to use a palatal splint.
Note: The focus has to be on to reestablishing occlusion and the transverse bony dimension.
In this photograph, the palatal splint has been inserted. Holes have been drilled through the palatal splint. These holes have been used to fix the wires to the arch bar.
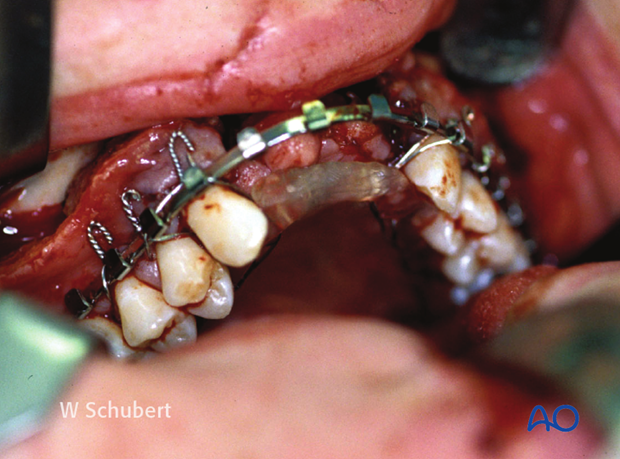
3. Aftercare following closed treatment of Le Fort I and palatoalveolar fractures
Postoperative positioning
Keeping the patient’s head in an upright position both preoperatively and postoperatively may significantly improve periorbital edema and pain.
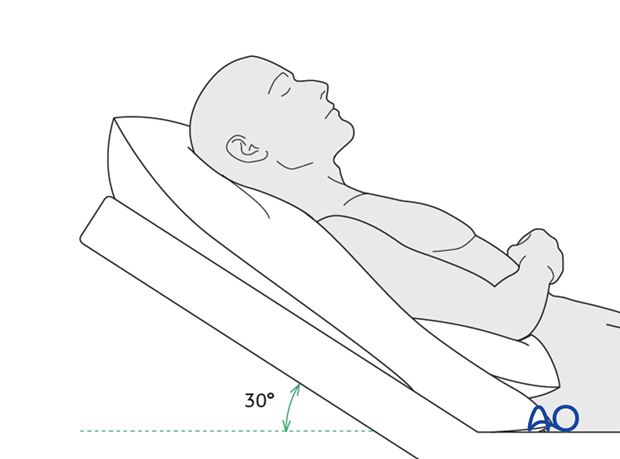
Medication
The use of the following perioperative medication is controversial. There is little evidence to make strong recommendations for postoperative care.
- No aspirin or nonsteroidal antiinflammatory drugs (NSAIDs) for 7 days
- Analgesia as necessary
- Antibiotics (many surgeons use perioperative antibiotics. There is no clear advantage of any one antibiotic, and the recommended duration of treatment is debatable.)
- Nasal decongestant may be helpful for symptomatic improvement in some patients.
- Steroids, in cases of severe orbital trauma, may help with postoperative edema. Some surgeons have noted increased complications with perioperative steroids.
- Ophthalmic ointment should follow local and approved protocol. This is not generally required in case of periorbital edema. Some surgeons prefer it. Some ointments have been found to cause significant conjunctival irritation.
- Regular perioral and oral wound care has to include disinfectant mouth rinse, lip care, etc.
Ophthalmological examination
Postoperative examination by an ophthalmologist may be requested. The following signs and symptoms are usually evaluated:
- Vision (except for alveolar ridge fracture, palatal fracture)
- Extraocular motion (motility) (except alveolar ridge fracture, palatal fracture)
- Diplopia (except Le Fort I, alveolar ridge fracture, palatal fracture)
- Globe position (except Le Fort I, alveolar ridge fracture, palatal fracture)
- Perimetric examination (except Le Fort I, alveolar ridge fracture, palatal fracture)
- Lid position
- If the patient complains of epiphora (tear overflow), the lacrimal duct must be checked.
Note: In case of postoperative double vision, ophthalmological assessment has to clarify the cause. Use of prism foils on existing glasses may be helpful as an early aid.
Postoperative imaging
Postoperative imaging has to be performed within the first days after surgery. 3-D imaging (CT, cone beam) is recommended to assess complex fracture reductions. An exception may be made for centers capable of intraoperative imaging.
Especially in fractures involving the alveolar area, orthopantomograms (OPG) are helpful.
Diet
Diet depends on the fracture pattern.
Soft diet can be taken as tolerated until there has been adequate healing of the maxillary vestibular incision.
Intranasal feeding may be considered in cases with oral bone exposure and soft-tissue defects.
Patients in MMF will remain on a liquid diet until such time the MMF is released.
Clinical follow-up
Clinical follow-up depends on the complexity of the surgery, and whether the patient has any postoperative problems.
With patients having fracture patterns including periorbital trauma, issues to consider are the following:
- Globe position
- Double vision
- Other vision problems
Other issues to consider are:
- Facial deformity (incl. asymmetry)
- Sensory nerve compromise
- Problems of scar formation
Issues to consider with Le Fort fractures, palatal fractures and alveolar ridge fractures include:
- Problems of dentition and dental sensation
- Problems of occlusion
- Problems of the temporomandibular joint (TMJ), (lack of range of motion, pain)
MMF
The duration and/or use of MMF is controversial and highly dependent on the particular patient and complexity of the trauma. In some cases where long-term MMF may be recommended, the surgeon may choose to leave the patient out of MMF immediately postoperatively because of concerns of edema, postoperative sedation, and airway. In these cases the surgeon may choose to place the patient in MMF after these concerns have been resolved.
The need and duration of MMF is very much dependent on:
- Fracture morphology
- Type and stability of fixation (including palatal splints)
- Dentition
- Coexistence of mandibular fractures
- Premorbid occlusion
Oral hygiene
Patients with arch bars and/or intraoral incisions and/or wounds must be instructed in appropriate oral hygiene procedures. The presence of the arch bars or elastics makes this a more difficult procedure. A soft toothbrush (dipped in warm water to make it softer) should be used to clean the surfaces of the teeth and arch bars. Elastics are removed for oral hygiene procedures. Chlorhexidine oral rinses should be prescribed and used at least 3 times a day to help sanitize the mouth.
For larger debris, a 1:1 mixture of hydrogen peroxide/chlorhexidine can be used. The bubbling action of the hydrogen peroxide helps remove debris. A Waterpik® is a very useful tool to help remove debris from the wires. If a Waterpik is used, care should be taken not to direct the jet stream directly over intraoral incisions as this may lead to wound dehiscence.












