Screw fixation
1. Principles and general considerations
Arthroscopic control
Screw insertion is routinely done under arthroscopic control.
Reduction and screw configuration
Prognosis is dependent on accurate articular reduction and, in turn, minimal postoperative osteoarthritis.
Nondisplaced fractures do not require reduction.
Many incomplete fractures are repaired with one screw; depending on the distance of the fracture two are used. Most complete fractures are repaired with two screws; occasionally three are used.
Use 4.5 mm screws (there is no real need for 5.5 mm screws).
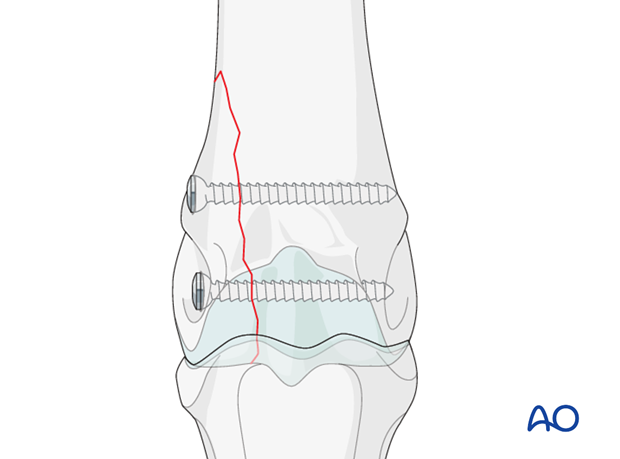
Drilling in dense bone
The bone is very dense in the condylar region, therefore, one needs to avoid drill overheating, which causes bone necrosis. Frequent cleaning of drill bits as well as tapping is necessary.
2. Patient positioning
This procedure is performed with the patient placed either in dorsal recumbency or lateral recumbency.

3. Positioning and approach
Positioning
The horse is positioned in dorsal recumbency with the leg extended. The lateral position is an option favored by some surgeons.
The author prefers dorsal recumbency over lateral recumbency because 1) taking dorsopalmar (plantar) and lateral to medial radiographs is more convenient and 2) there is less hemorrhage. The author always does arthroscopy in this joint in dorsal recumbency.

Approach
Only stab incisions are used for fixation of lateral nondisplaced fractures supervised arthroscopically.
4. Surgical technique
Insertion of the needles
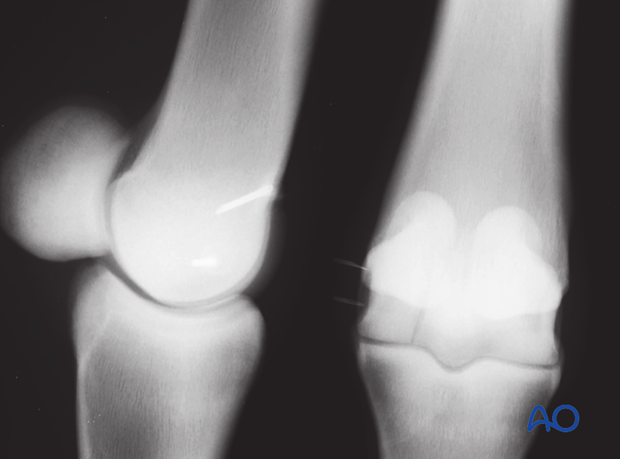
Two needles are placed in the area of the lateral condylar fossa around the estimated position of the distal screw.
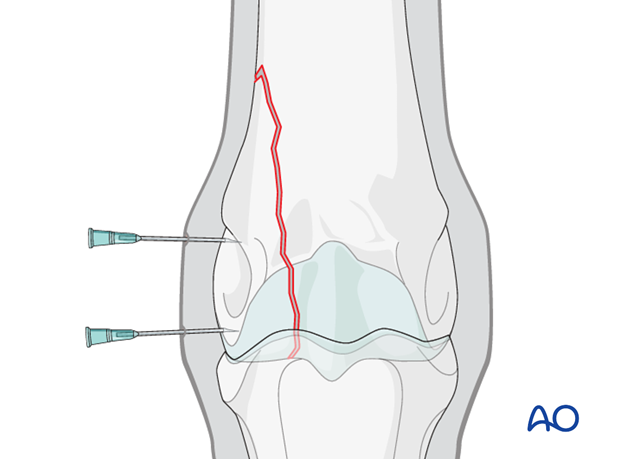
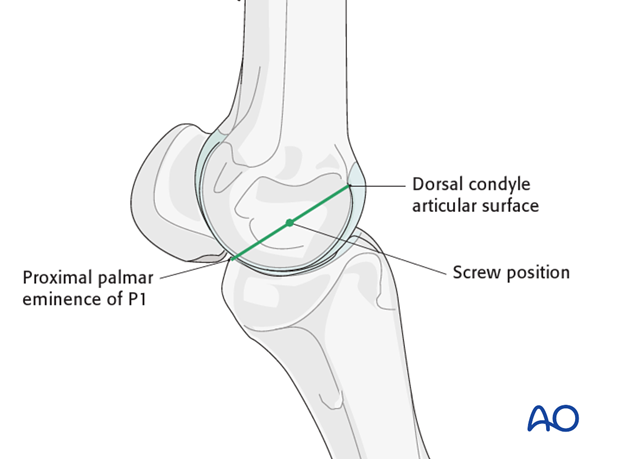
The position of the distal screw can be approximated by drawing a line from the top of the dorsal condyle articular surface to the proximal palmar eminence of the proximal phalanx. The screw location is half way along this line.
In this clinical photograph, two needles have been used as this facilitates making the stab incision in the most appropriate space.
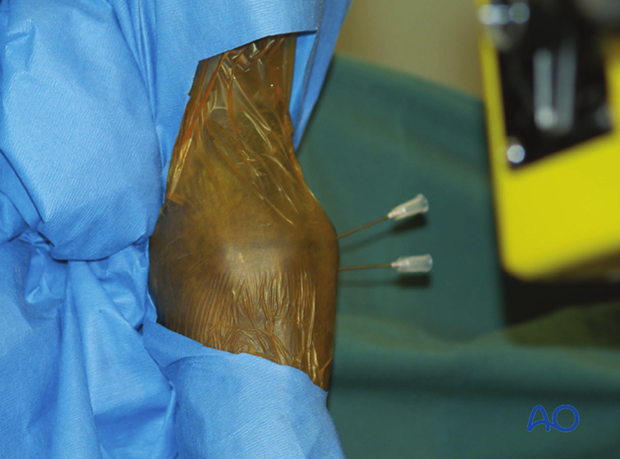
Radiographic view of the same situation.
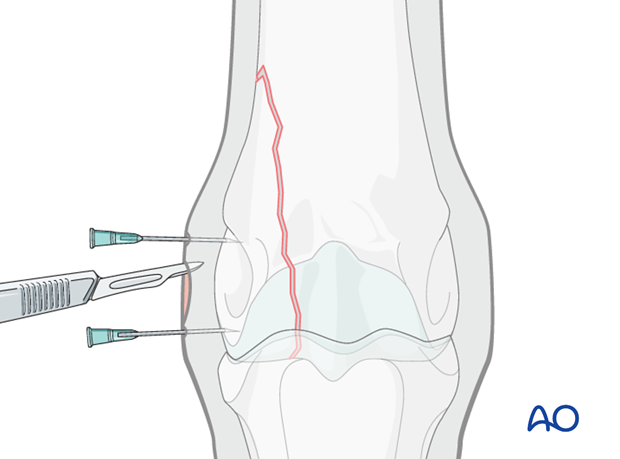
Stab incision
A 10-15 mm stab incision is made between the two needles through the skin and the lateral collateral ligament.
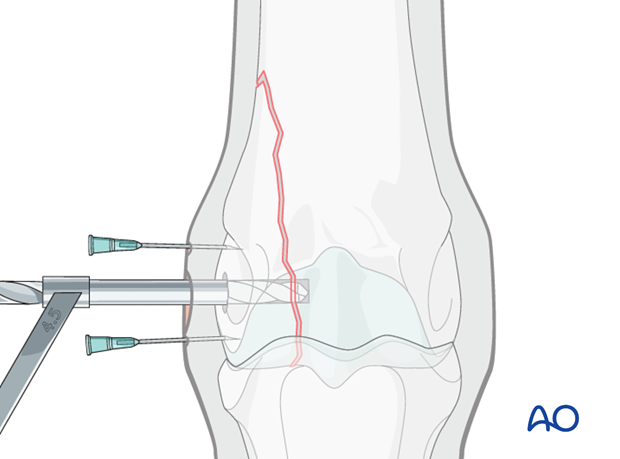
Drilling the glide hole
A 4.5 mm glide hole is drilled (protected by the appropriate drill sleeve) parallel to the articular surface of the metacarpus/metatarsus for approximately 2 cm (until immediately beyond fracture line).
With nondisplaced fractures this is usually done before inserting the arthroscope.
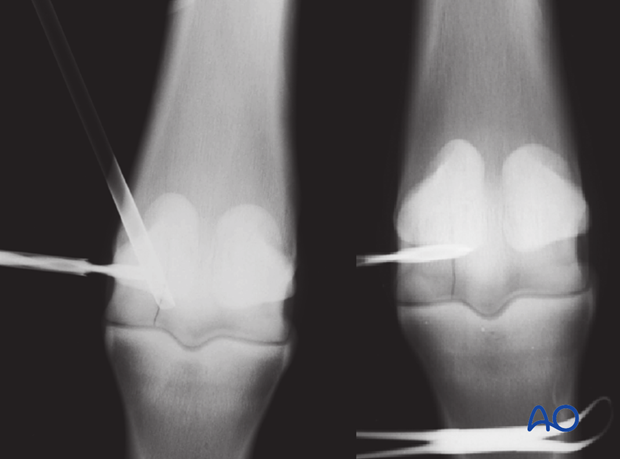
The two radiographs show the 4.5 mm drill before the fracture line with or without the arthroscopic sleeve in the joint.
Pearl: measuring drill depth
The advancement of the drill is measured by placing a ruler on the top of the drill sleeve and determine the distance to the tip of the drill.
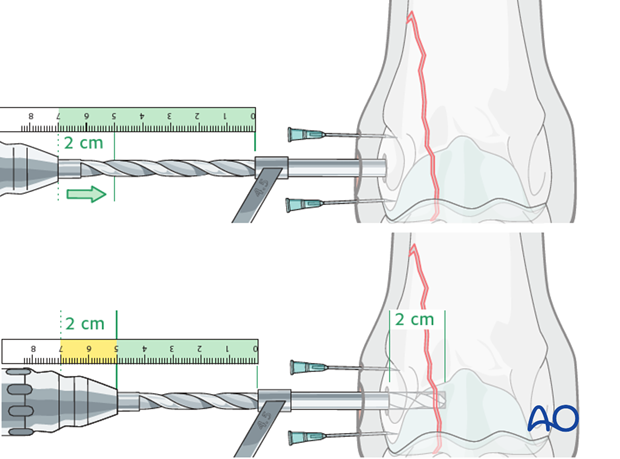
Drilling 3.2 mm hole
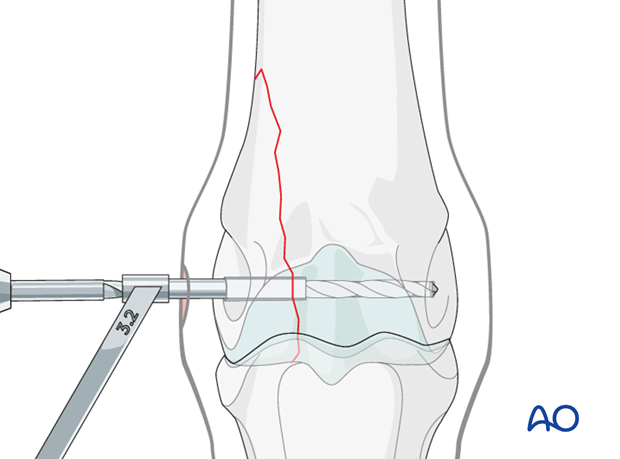
The 3.2 mm drill guide is inserted into the glide hole using rotating motions and a 3.2 mm hole is drilled through the remainder distal metacarpus.
This is facilitated by placing a Steinmann pin into the glide hole prior to removing the 4.5mm drill sleeve. The 3.2 mm drill sleeve is subsequently inserted over the Steinmann pin. The Steinmann pin is removed.
It is recommended that the hole is drilled completely through the whole bone.
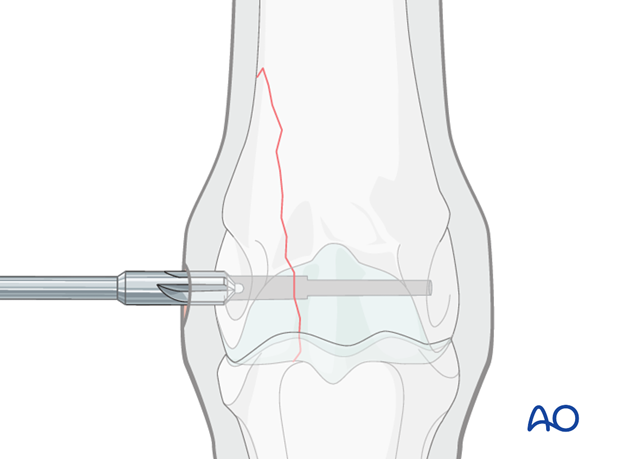
Countersinking
The hole in the lateral condylar fossa is lightly countersunk and debris is flushed.
Some surgeons do not countersink the distal hole based on the concave curvature of the fossa. However, such practice risks bending the screw head because of the lack of seating of the head of the screw; the author does not consider significant damage to the collateral ligament is created and has never seen any negative consequences.
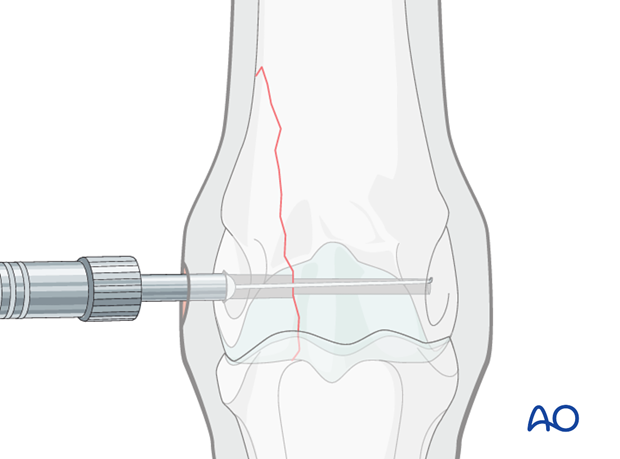
Determining screw length
The depth of the metacarpal condyle is consistent enough that a 54 mm screw can be routinely inserted to provide good fixation without protrusion out the other side. Additionally, the use of the depth gauge is optional because it is difficult to seat the bottom of the depth gauge easily in the (countersunk) fossa. A 52 mm screw is commonly used in 2 year old Thoroughbreds unless they are unusual large.
Tapping the hole
The hole is tapped with a 4.5 mm tap through the 4.5 mm drill guide. Hand or power tapping can be applied.
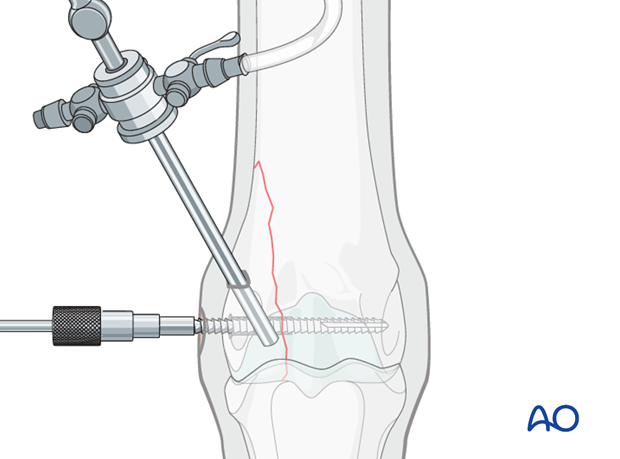
Inserting the arthroscope
Te arthroscope is inserted in the proximal lateral aspect of the dorsal pouch of the metacarpo/metatarsophalangeal joint.
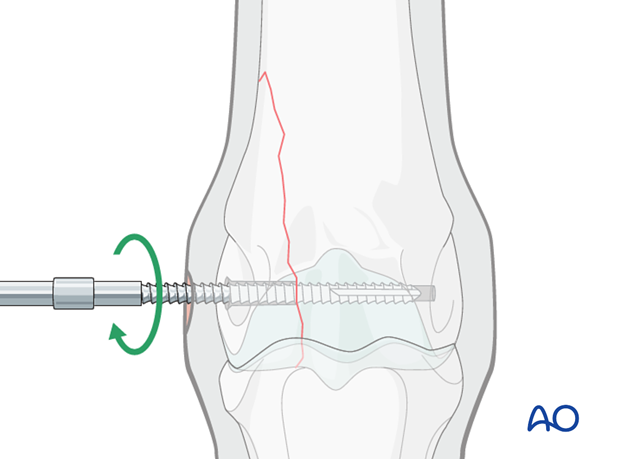
Inserting screw
A 4.5 mm screw of appropriate length is inserted. The screw is tightened under arthroscopic visualization. Applying excess of torque could risk breaking the screw head off. After the screw is tightened any granulation tissue squeezed out through the fracture line or elevated cartilage at the fracture line (amount of separated cartilage is usually very small) is removed.
It is recommended that the arthroscope also be placed in the palmar pouch to evaluate articular reduction of the fracture in the distal palmar/plantar metacarpus/metatarsus and, also, evaluate the articular surfaces of the proximal sesamoid bones. Presence of articular cartilage erosions on the condyles and proximal sesamoid bones will lead to decreased prognosis for racing soundness.
It is to be noted that there is no cortical demarcation in this region of the distal metacarpus/metatarsus because of uniformity in the bone structure.
Intraoperative radiographs should be taken to confirm screw length and correct positioning.
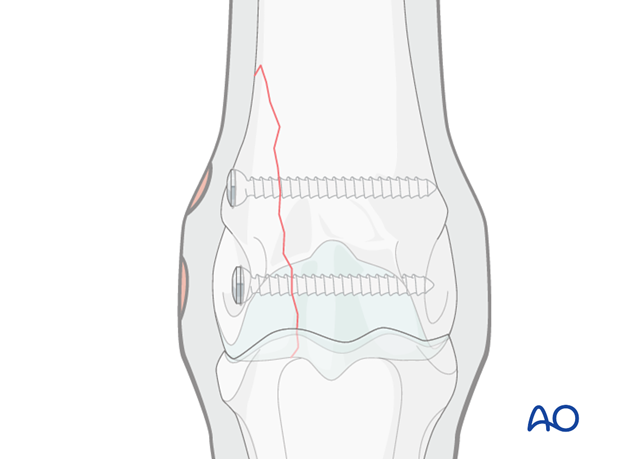
Additional screws
The procedure is repeated for insertion of the second screw, placing it approximately 2 cm proximal to the first screw and parallel to the first screw.
The procedure is the same as for the first screw except
- Countersinking is always performed.
- After countersinking the depth gauge is always used.
- The screw needs to engage the far cortex of distal metacarpus/metatarsus.
Occasionally, in long fractures, a third screw is inserted.
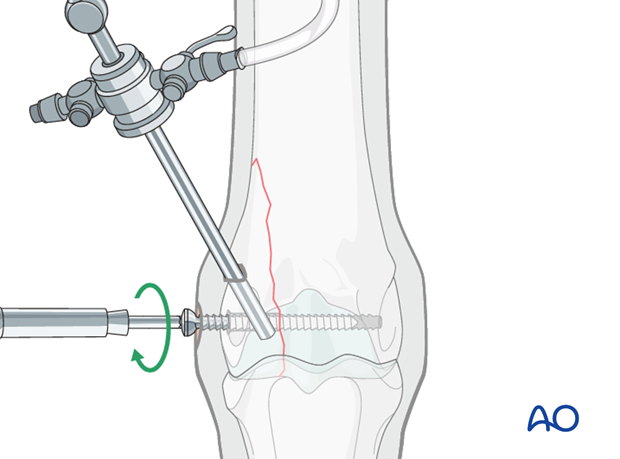
Pearl: screw driver while drilling for additional screws
The screw driver can be inserted in the distal screw while drilling the glide hole for the second screw to ensure the second screw being parallel to the first one.
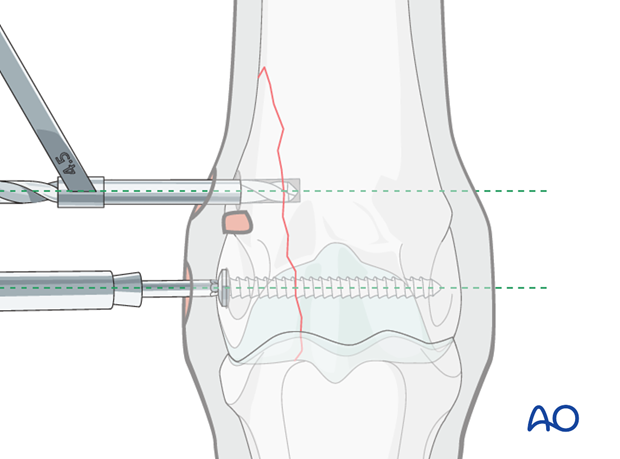
5. Case example
Case: 3-year old Thoroughbred colt with lateral incomplete nondisplaced fracture
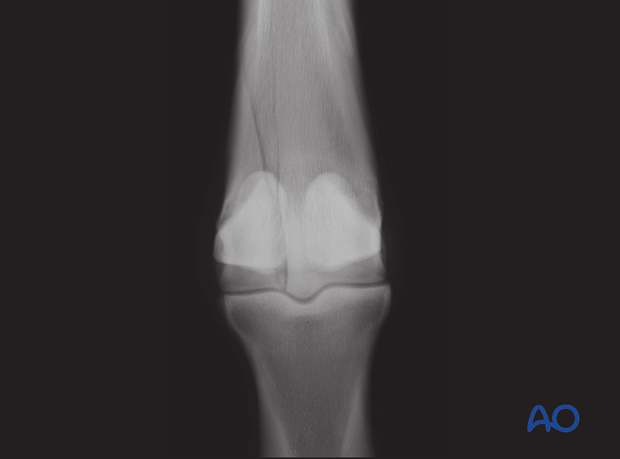
Preoperative dorsopalmar radiograph of a lateral incomplete nondisplaced fracture of the third metacarpal condyle in a three year old Thoroughbred colt.
Note: It is a long incomplete fracture.
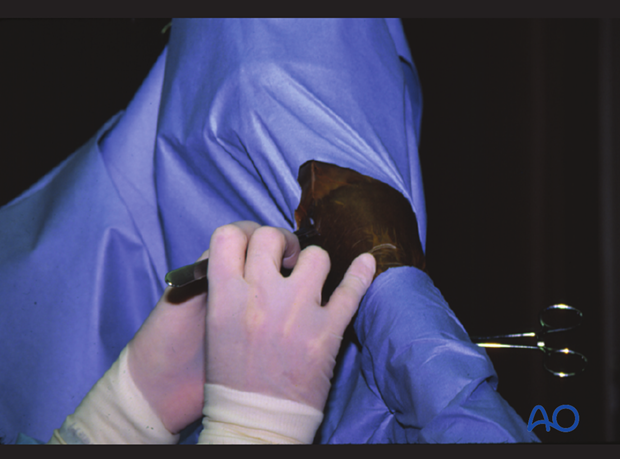
The horse is positioned in dorsal recumbency. The stab incision is performed over the lateral condylar fossa.
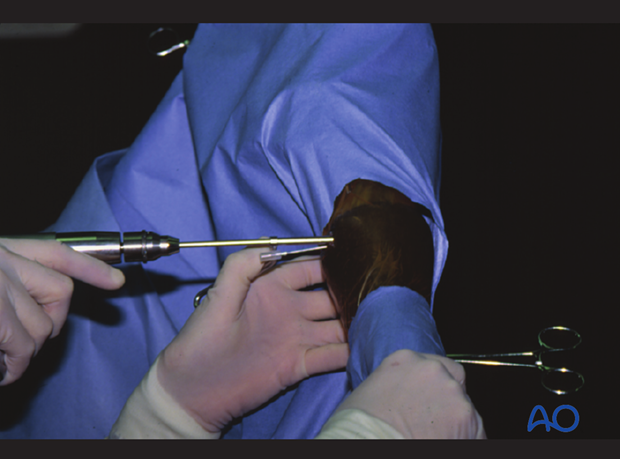
Drilling of the 4.5 mm glide hole.
Using a ruler to estimate depth of glide hole.
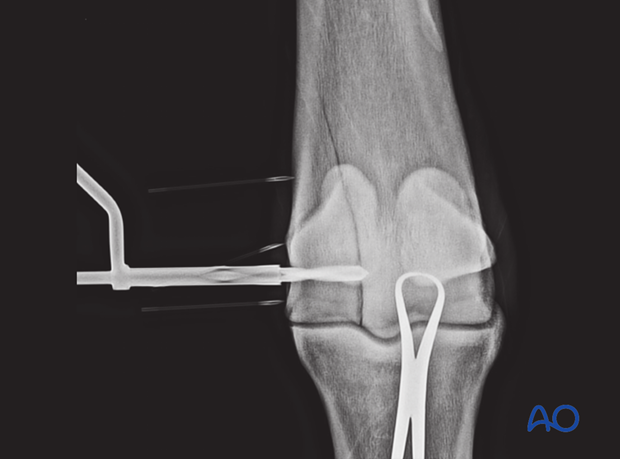
Dorsoplamar radiograph to check that glide hole passes the fracture line.
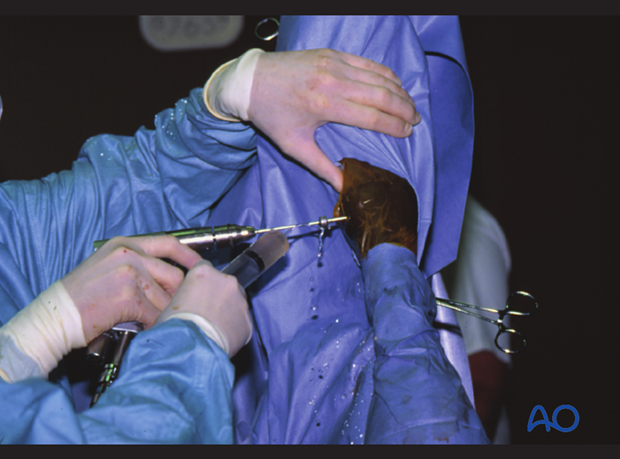
Drilling the 3.2 mm hole through the 3.2 mm drill guide, inserted into the glide hole. Note: the use of fluid irrigation keeps drill bit lubricated.
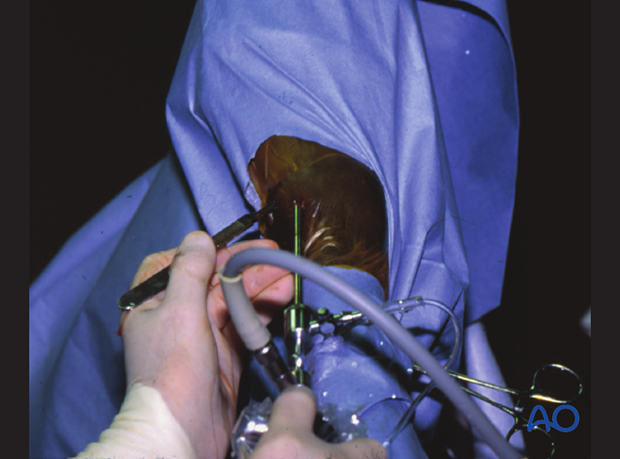
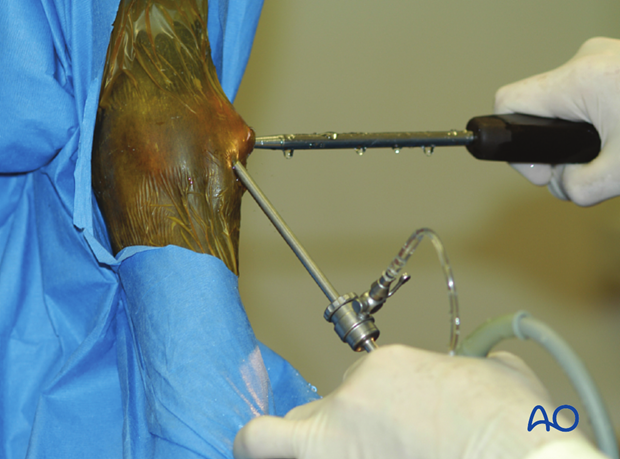
After countersinking and tapping the arthroscope is inserted into the dorsal pouch of the metacarpophalangeal joint to observe anatomic closure of the fracture as the screw is tightened.
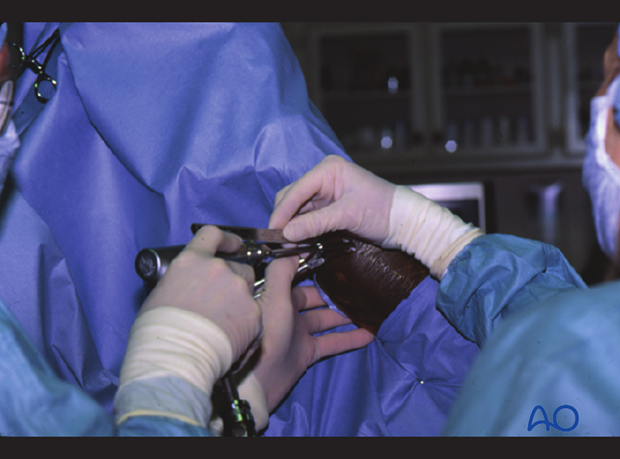
Tightening of screw under arthroscopic visualization.
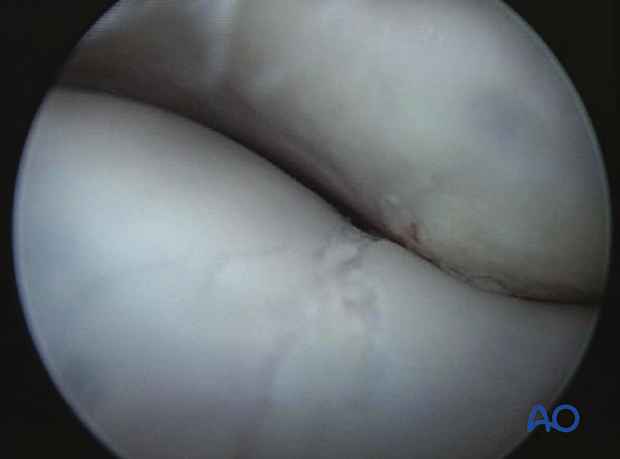
Arthroscopic view of fracture in lateral condyle prior to compression.
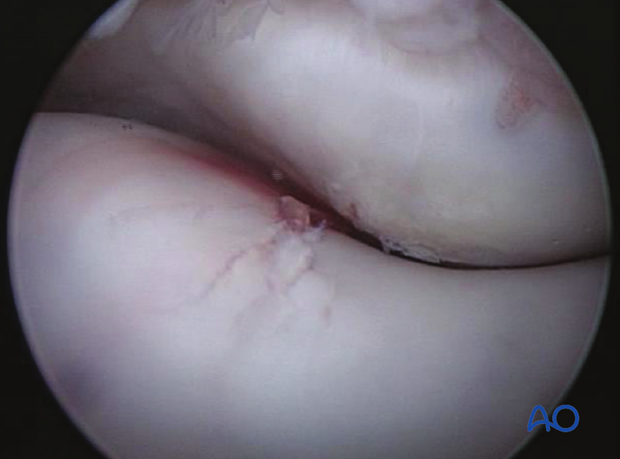
Arthroscopic view of fracture in lateral condyle as fracture is tightened. Note blood coming from fracture line and small area of elevated cartilage that will be removed with a small rongeur.
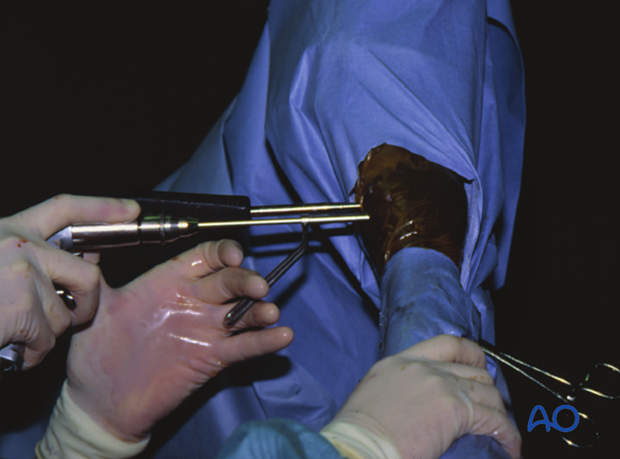
Drilling the 4.5 mm glide hole for second screw. Note the screw driver in the distal screw serving as a guide to ensure the second screw is approximately parallel to the first screw.
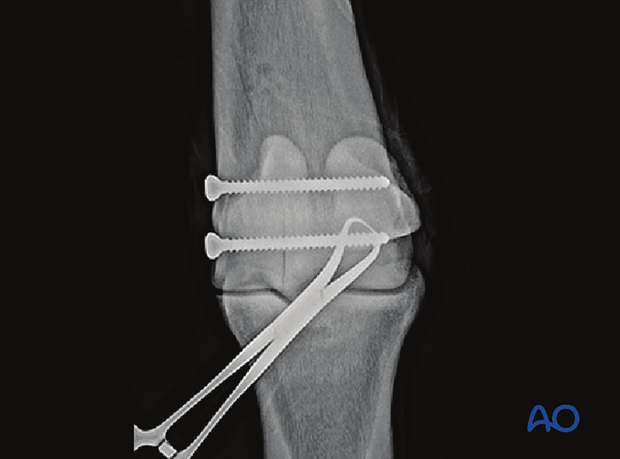
Intraoperative dorsopalmar radiograph after both screws have been inserted and tightened. The fracture line is still visible towards the articular surface.
6. Aftertreatment
Suture all incisions (only skin sutures are necessary). Place a sterile bandage on the fetlock joint. Use perioperative antibiotics for 24 hours and place the horse on antiinflammatory medication for 5 – 7 days. The horse should be confined to a stall (box) but hand walking is commenced at 2 weeks.
Horses can usually go back into race training at 4 months but only after clinical and radiographic examination and clearance by a veterinary surgeon.














