Percutaneous pedicle screw insertion in the thoracolumbar spine
1. Skin incision
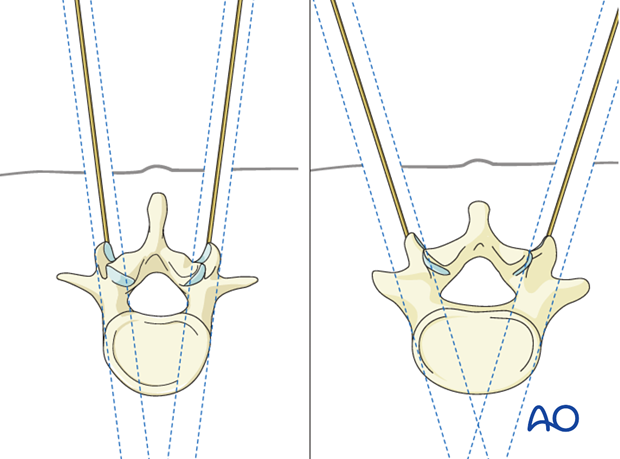
The skin incision is lateral to the image projection of the pedicle. The distance from the skin incision to the image projection varies depending on the various levels of the spine. It also depends on the convergence of the pedicles.
It is necessary to confirm the correct level of the approach with fluoroscopy.

In the middle thoracic spine, the skin incision is close to the image projection of the pedicle in the upper thoracic, and in the lumbar spine it is more lateral.
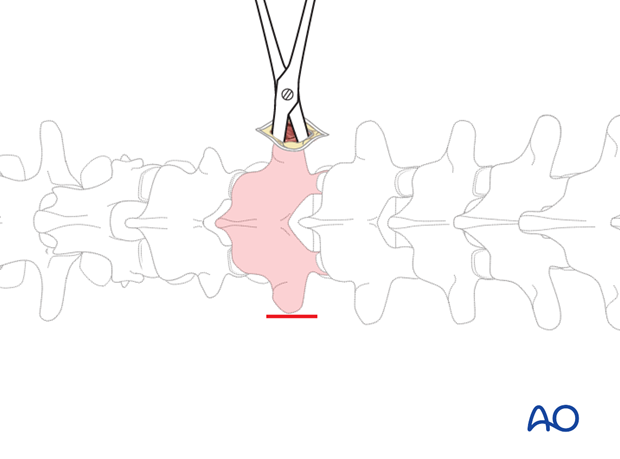
2. Exposure
Using scissors, a blunt dissection of the subcutaneous tissue, the fascia, and the muscles is performed down to the bony structures of the vertebra.
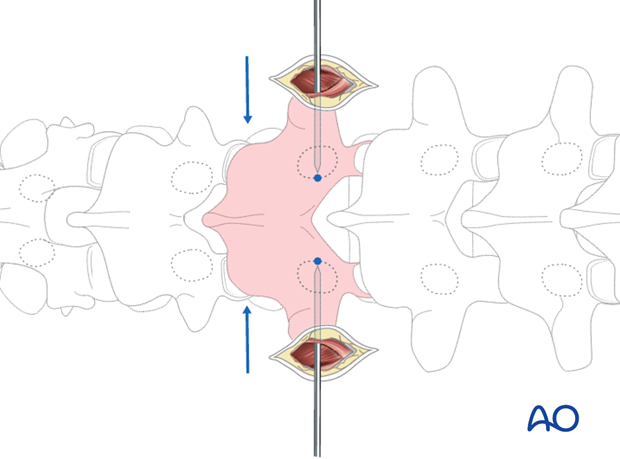
Cannulated needles are inserted both at a 3 o' clock on the right side and a 9 o' clock position on the left side.
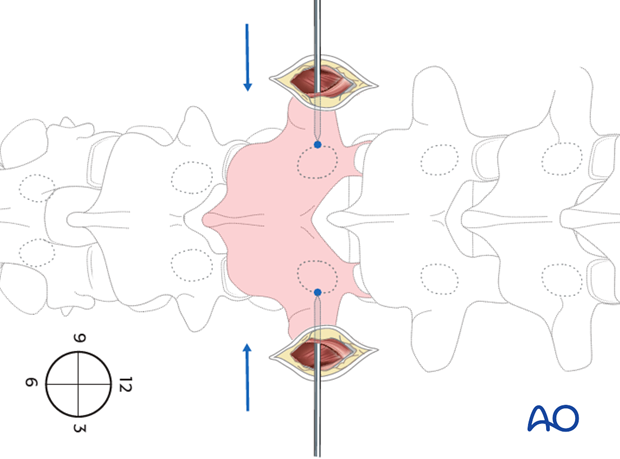
The cannulated needles are tapped in until they reach the medial border of the pedicle image projection.
More information about the entry point can be accessed here:
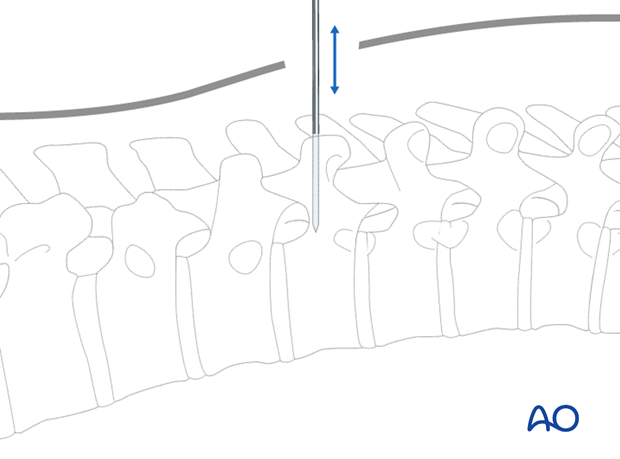
A lateral X-ray is then performed.
If the tip of the needle has not passed the posterior wall of the vertebral body in the lateral projection, retract and reposition the needle.
If the tip of the needle has passed the posterior wall of the vertebral body in the lateral projection, the needle can be advanced to the center of the vertebral body.
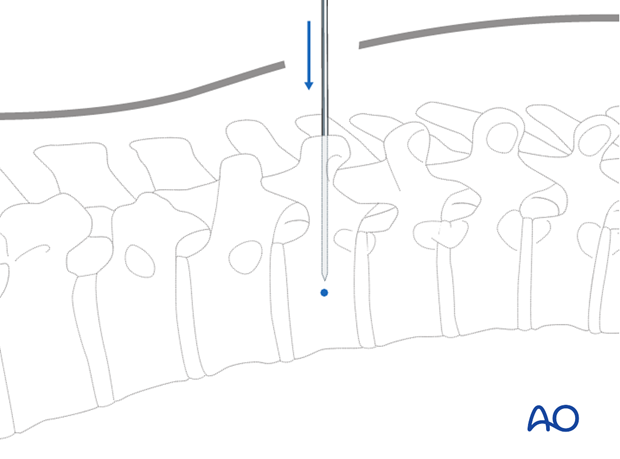
A K-wire is introduced via the cannulated needle. Then, the cannulated needle is removed leaving the K-wire in place.
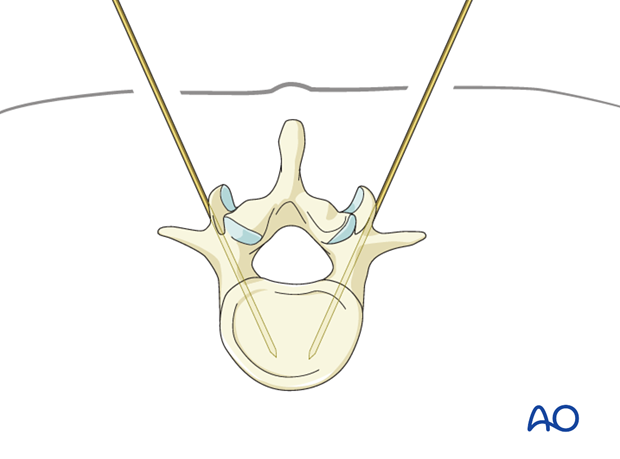
After dilatation of the soft tissue, the cannulated pedicle screw is inserted over the k-wire.
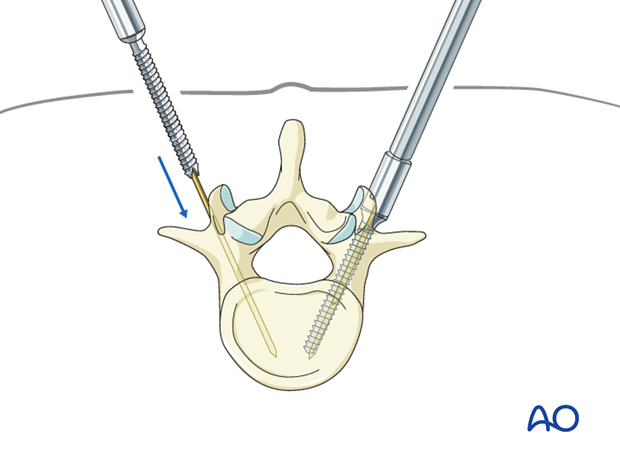
These steps are repeated, depending on the number of vertebrae that have to be instrumented.
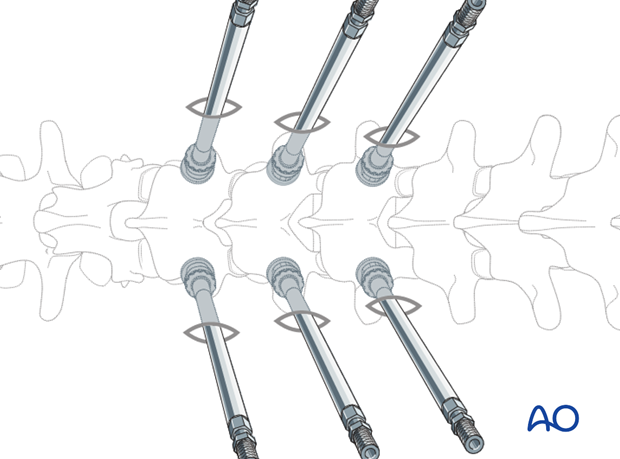
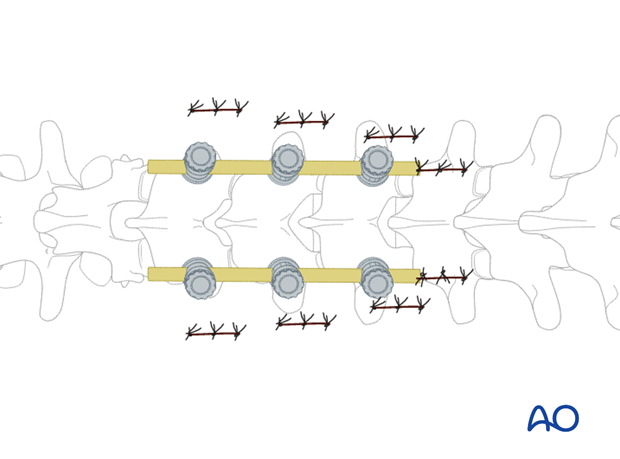
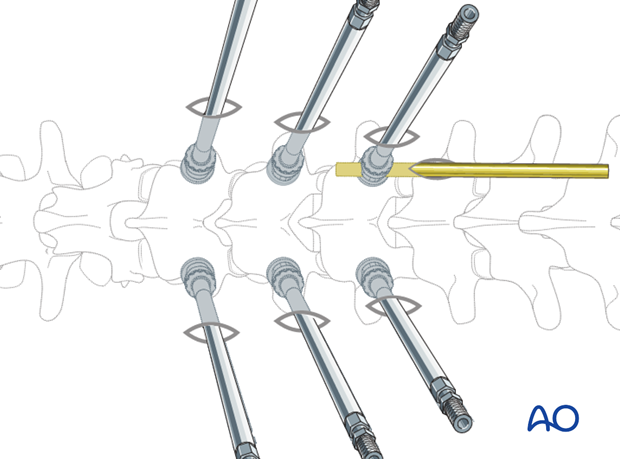
3. Rod placement
The rod is placed percutaneously through a separate stab incision. Depending on the used instrumentation, different techniques are in use.
4. Wound closure
For patients undergoing revision metastatic spine tumor surgery and/or with history of radiation, plastic surgery should perform the soft tissue reconstruction to decrease the risk of wound complications.
The wound is closed in layers.