Cervicothoracic junction - posterior fixation
1. Introduction
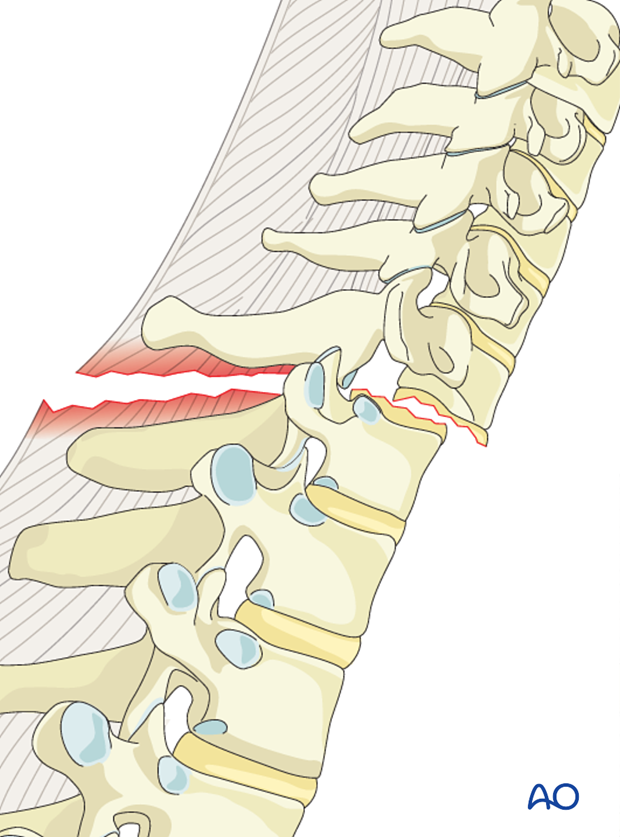
C type injuries are high impact injuries that result in translational or/and rotational displacement of the vertebral column. Most fractures are associated with severe cord injury and complete neurologic deficit. More than 50% of the fractures are associated with dural injuries and cerebrospinal fluid leak. Associated esophagus, trachea, or vertebral artery dissections at this level are common.
Management is aimed at resuscitation, control of life threatening organ injuries, spinal stabilization, and rehabilitation.
Surgical complications
More details on surgical complications can be found here.
2. Positioning and approach
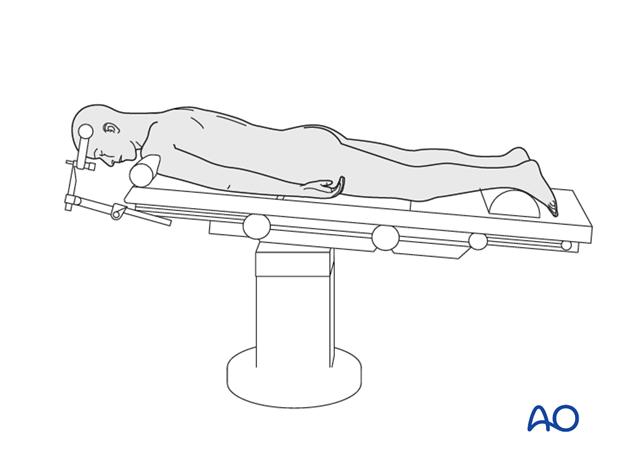
Posterior fixation is achieved with the patient in the prone position, through the posterior access to the thoraco cervical junction.
3. Screw insertion
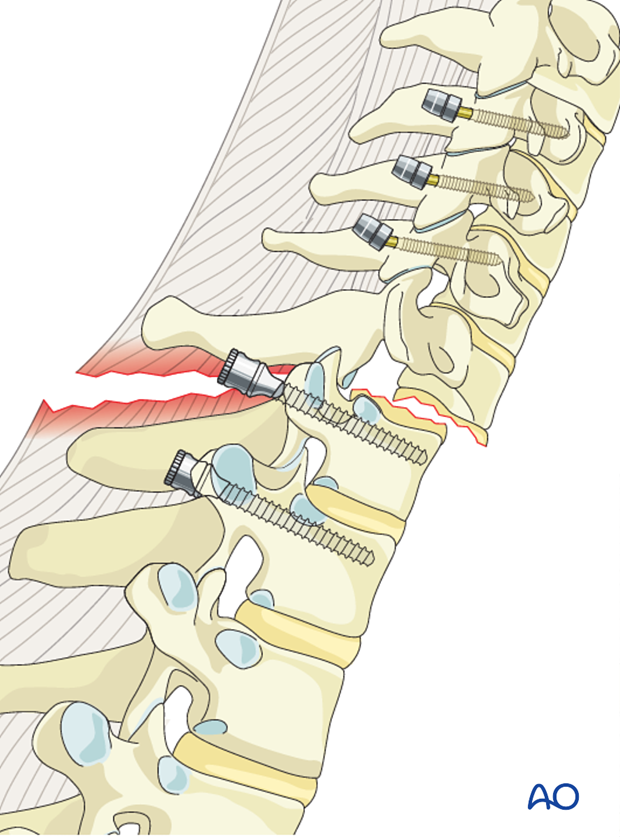
Screws are inserted at least two or three segments above and below the dislocation.
Cervical screws
In the lower cervical levels the following screws can be used:
Due to safety, lateral mass screws are preferred from C6 to cranial. If the lateral mass is compromised an additional level can be included in the fixation or pedicle screws may also be considered.
A lateral mass screw can also be used at the level of the fracture if the lateral mass is intact.
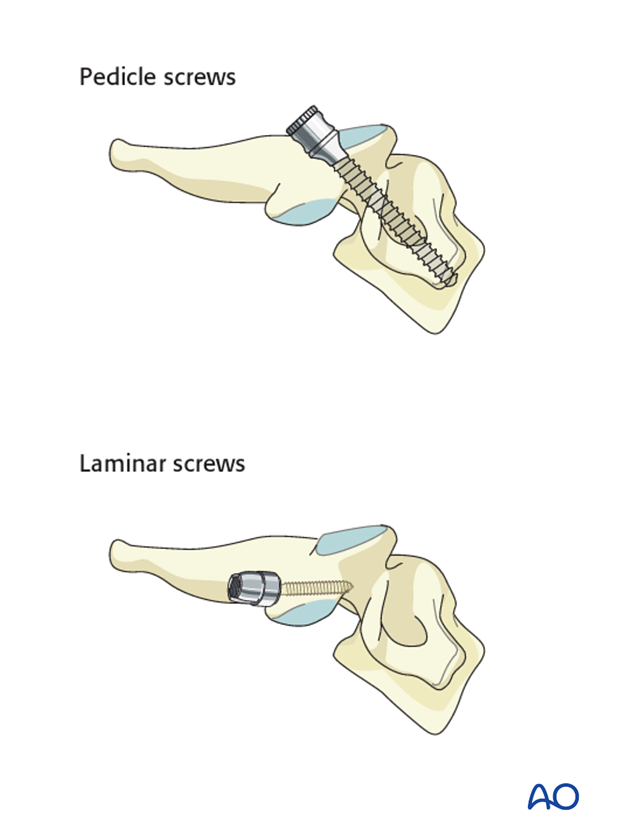
Thoracic screws
In the upper thoracic spine the following screws can be used:
Pedicle screws are biomechanically stronger and preferred; however, if the pedicles are too small, laminar screws can be used as an alternative at the level of T1-T2.
Inserting of the screws before decompression is recommended to prevent extensive epidural bleeding.
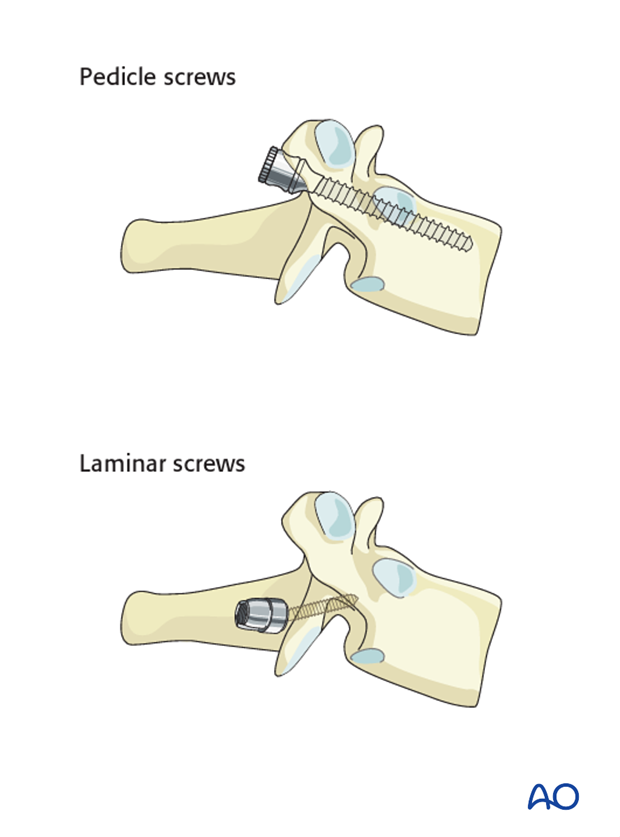
4. Decompression
If the spinal cord needs to be decompressed or a fractured lamina needs to be removed, this should be performed after screw insertion.
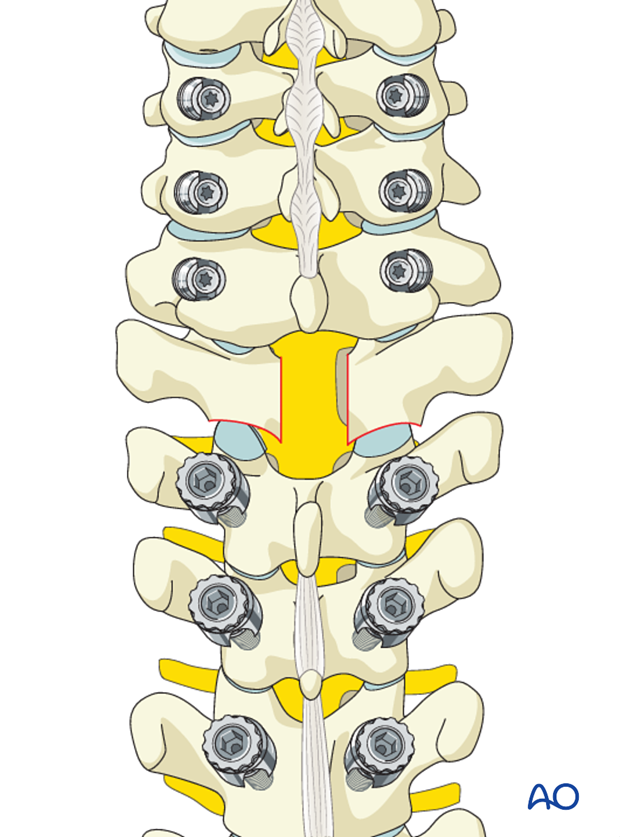
5. Facet joint reduction
If the facet joints are locked they can be reduced without distraction by removing the cranial part of the superior articular process of the caudal vertebra.
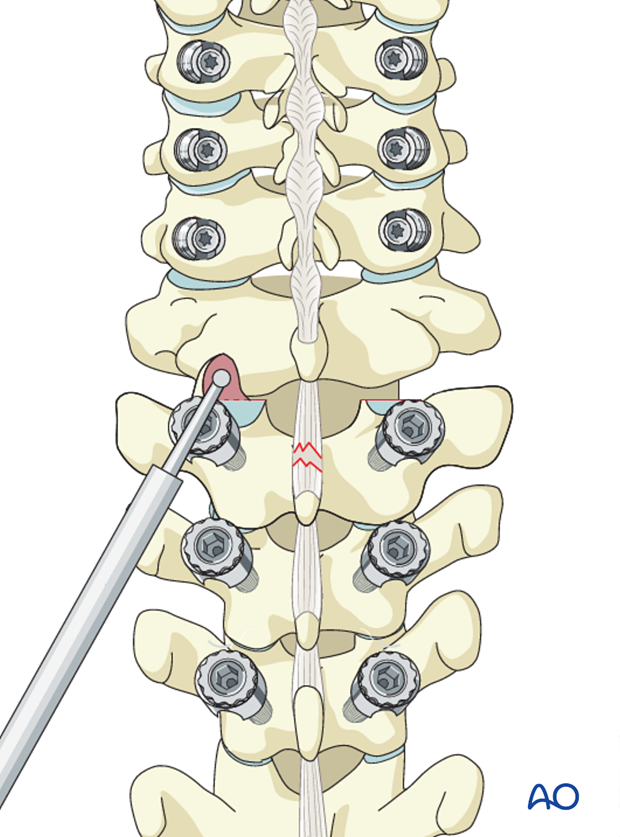
Open reduction of unilateral facet joint dislocation
A unilateral facet dislocation can be unlocked with gentle manual distraction applied across clamps placed on the spinous processes above and below the injury.
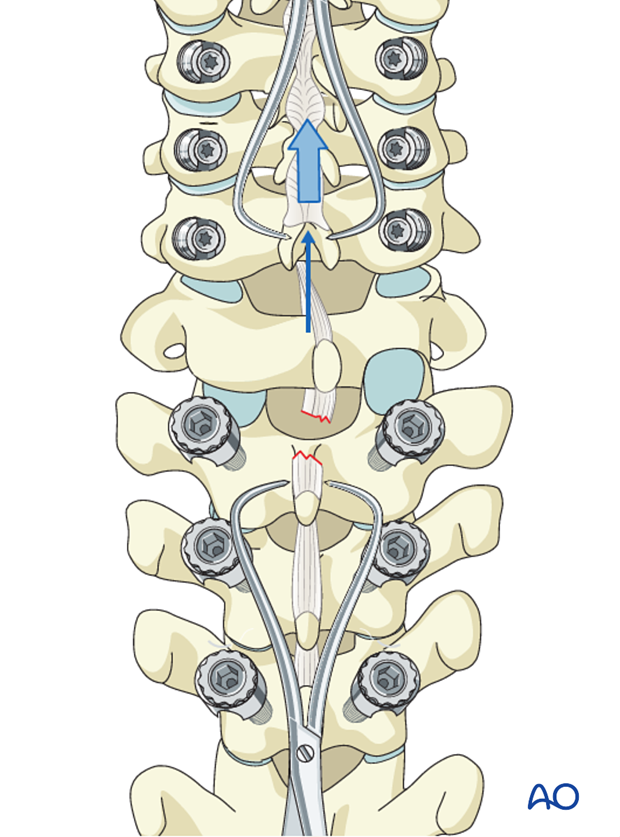
Manual rotation of the spinous process above the level of injury away from the side of the dislocation will reduce the joint and restore the spinal alignment.
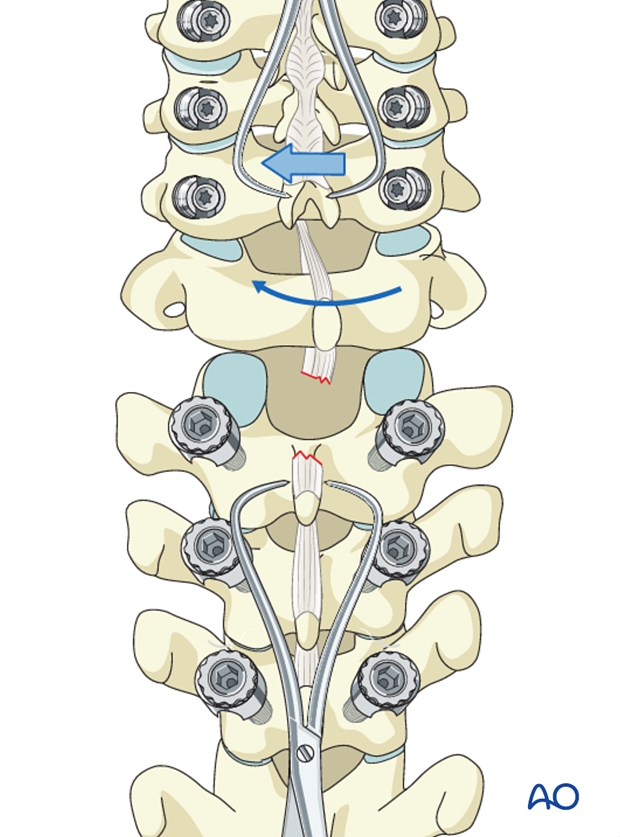
An elevator can be placed between the dislocated facet joints to facilitate reduction
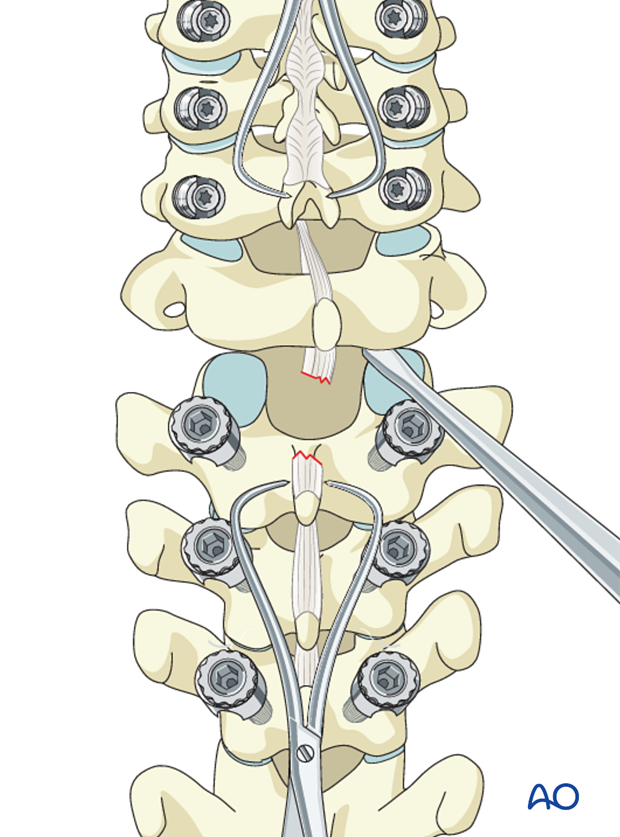
Bilateral dislocations
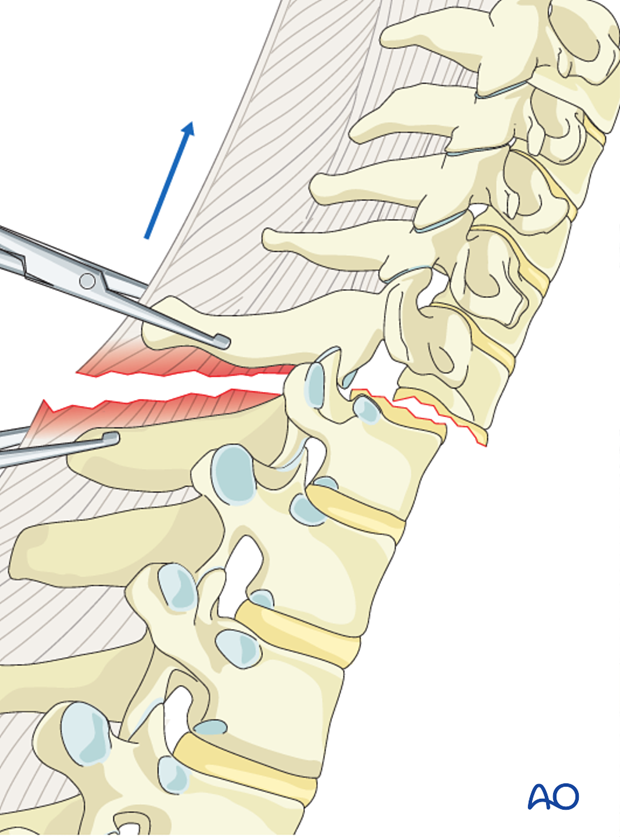
A bilateral facet dislocation can be unlocked with gentle manual distraction applied across clamps placed on the spinous processes above and below the injury.
In specific situations, this can be facilitated by prying the facets apart directly with an elevator or partial resection of the superior facet as described above for unilateral facet dislocations
Once reduction has been achieved, posterior instrumentation should be applied.
6. Rod preparation
Rod selection
For this procedure there are two rod options.
Option 1: Double diameter tapered rod (6mm at the thoracic end, 3.5 mm at the cervical end) may be used if available. In this case no rod connectors are needed.
This is the preferred option as it easier to install and reduces operating time.
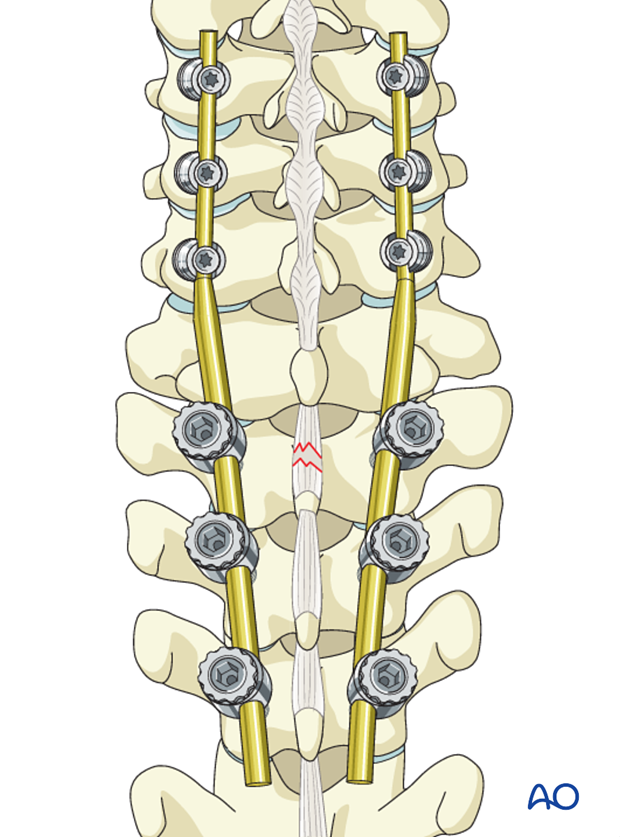
Option 2: A rod with a uniform diameter (3.4 or 4.0 mm) combined with a site to site connector between the cervical and thoracic spine. The rod connectors will have different diameters.
The rod connectors at this level are usually bulky and may cause problems with the wound closure.
Transverse connectors can be used in case of severe torsional instability, but they also may cause problems with wound closure at this level.
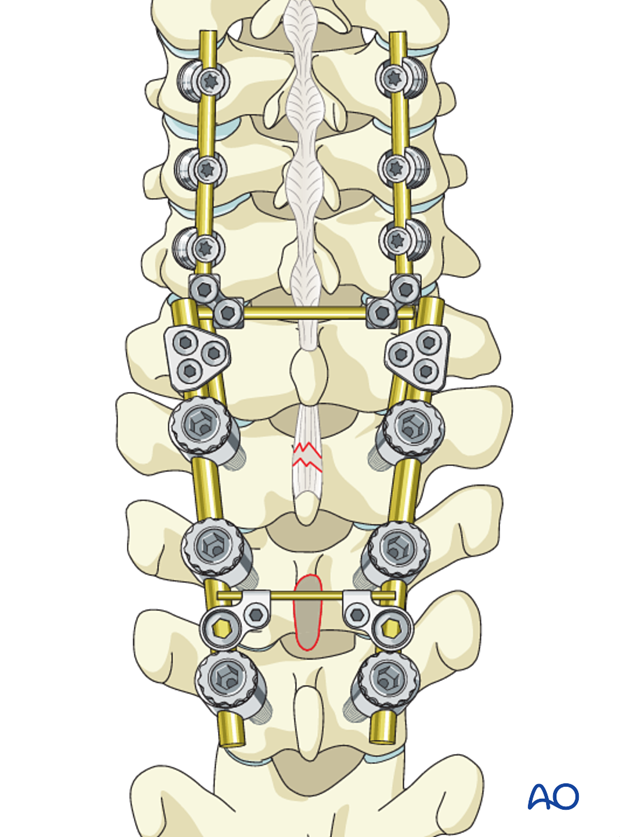
Rod contouring
Rods should be contoured to a slight lordosis in the cervical part and a slight kyphosis in the thoracic part.
Ideally the correct contouring should be achieved in the first attempt. Continuous adjustments will eventually lead to material fatigue.
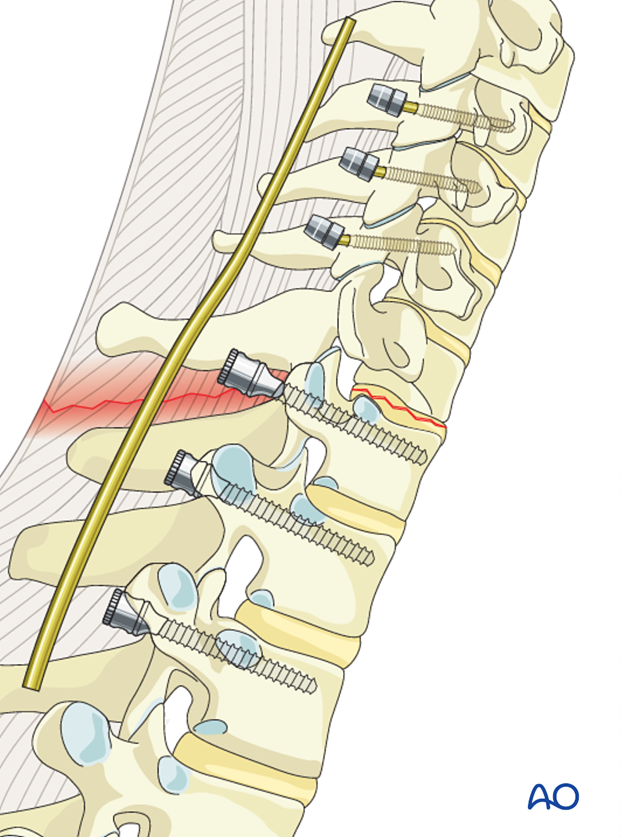
7. Reduction and fixation
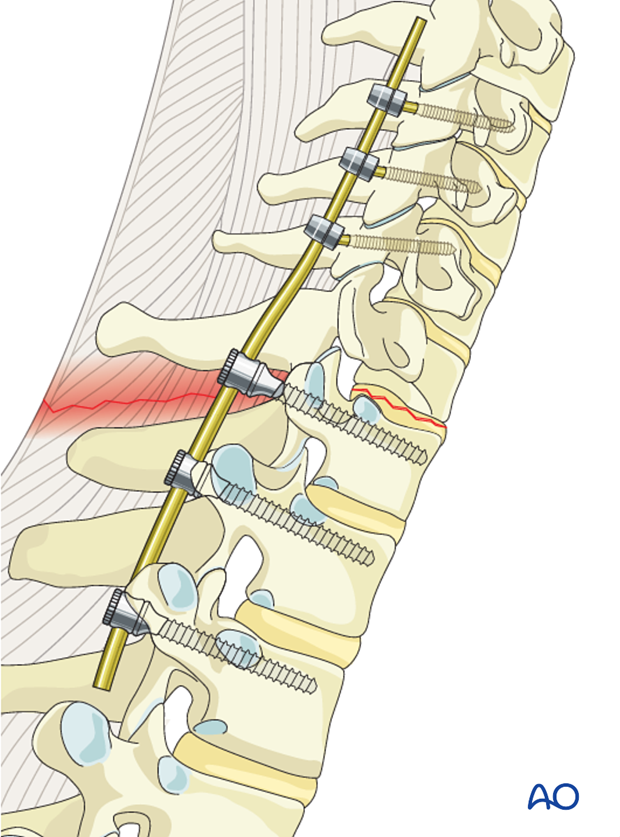
The rod is first attached to the cervical screws.
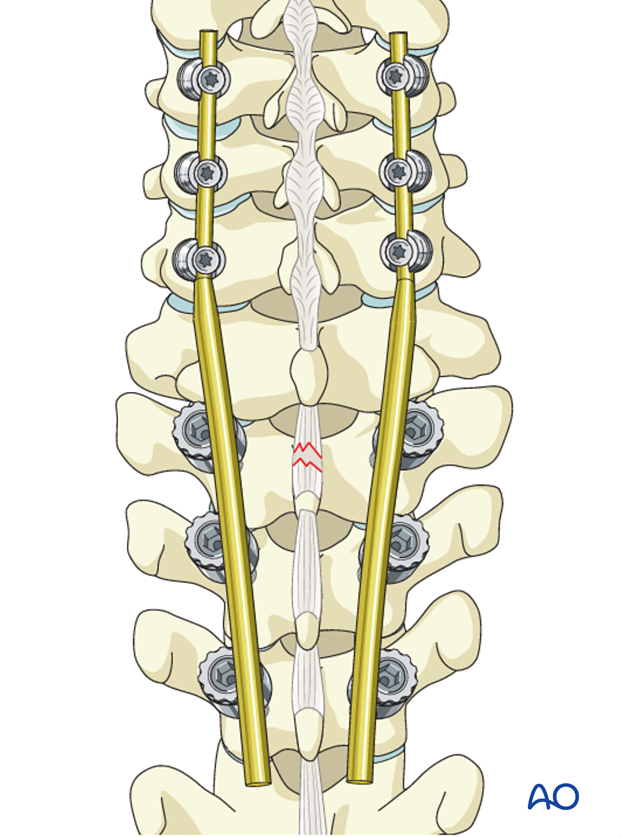
The fracture is reduced by the cantilever maneuver as the rod is attached to the thoracic screws.
It is usually not necessary to perform a distraction if there is sufficient removal of the facet joints. If necessary gentle distraction may be used to reduce the fracture.
In very unstable injuries, transverse rod connectors should be considered.
8. Fusion
Decision
Although fusion was routinely performed for all spinal fractures, its indications are now being restricted to fractures that are highly unstable.
If the surgeon plans for a fusion, the facet capsule is excised and the joint cartilage surfaces are denuded/curetted.
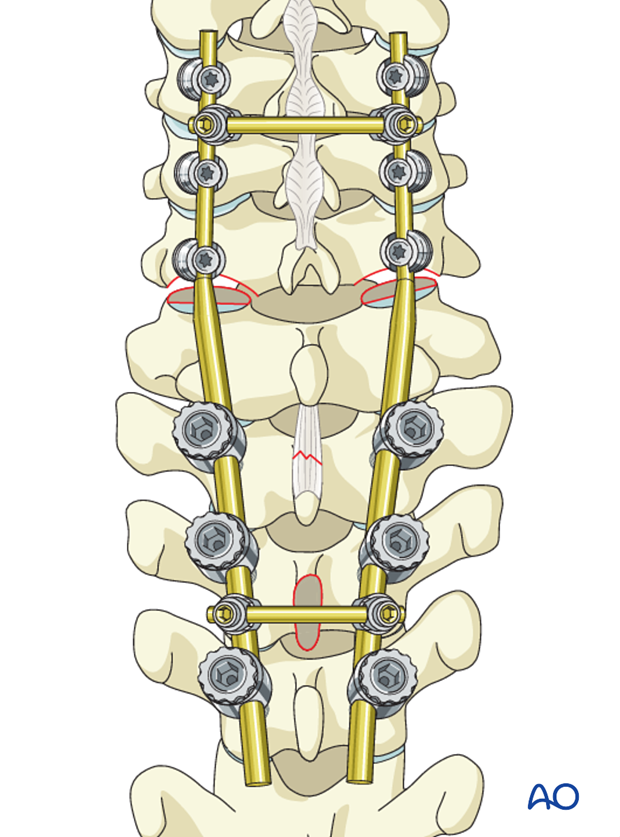
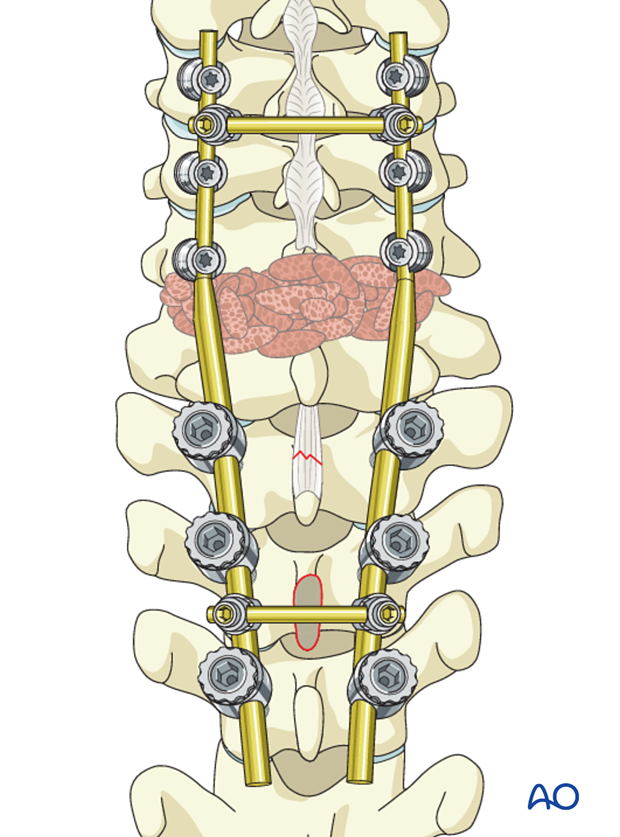
Pieces of bone graft (autograft, allograft) are inserted into the decorticated facet joint for fusion.
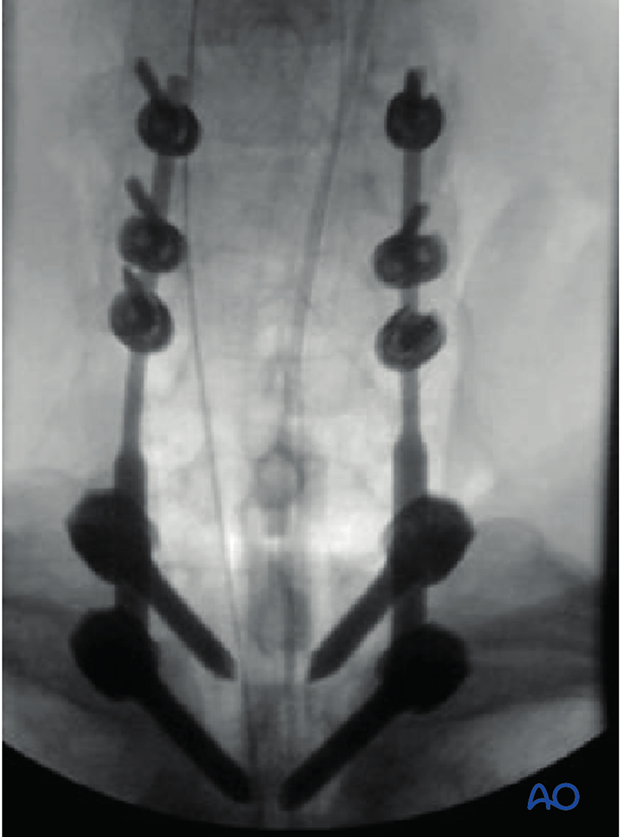
9. Postoperative imaging
Postoperative AP views should be obtained. As lateral views are not available in this area, a CT scan should be obtained as soon as possible after surgery to confirm the placement of the instrumentation and sufficient reduction.
10. Aftercare
Patients are made to sit up in bed on the first day after surgery.
A collar is commonly used following surgical stabilization to moderate patient activity.
The purpose of a collar is to prevent ranges of motion outside of limits deemed unfavorable for fracture healing. Collar is optional.
Patients with intact neurological status are made to stand and walk on the second day after surgery. Patients can be discharged when medically stable or sent to a rehabilitation center if further care is necessary. This depends on the comfort levels and presence of other associated injuries.
Patients are generally followed with periodical x-rays at 6 weeks, 3 months, 6 months, and 1 year.