Complete tibial revision with hinged knee
1. Introduction
A hinged knee implant system is required when the collateral ligaments are absent.
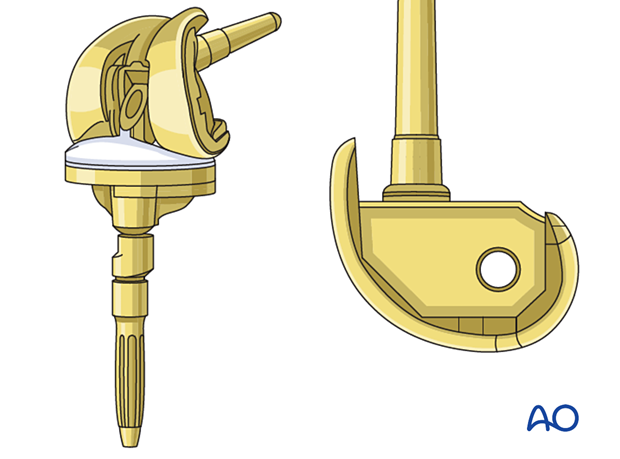
2. Preoperative planning
Tibial component revision to a hinged system is necessary when the fracture fragments compromise the integrity of the collateral ligaments.
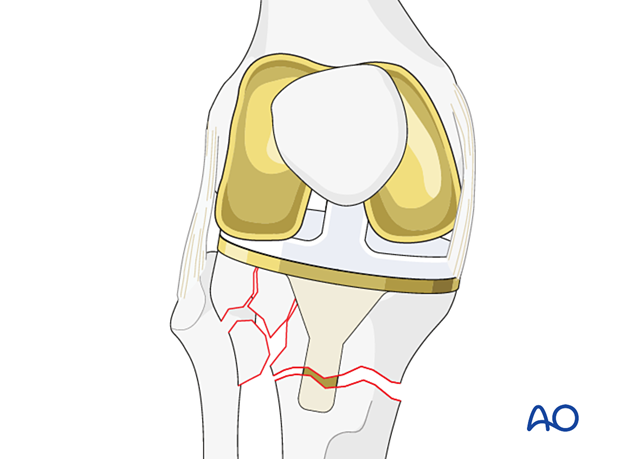
Femoral component
The femoral component also requires revision because the standard femoral component cannot be coupled to the hinged articulation.
An intramedullary stem is required for the hinged femoral component. It is typically 100-125 mm.
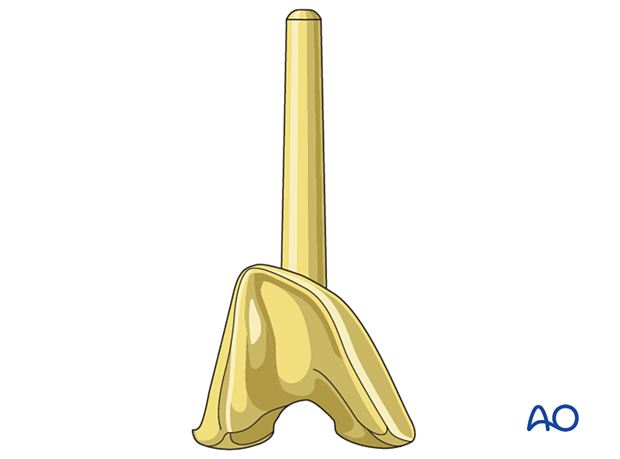
Tibial component
The length of the stem for the tibial component is typically determined depending on the specific system selected.
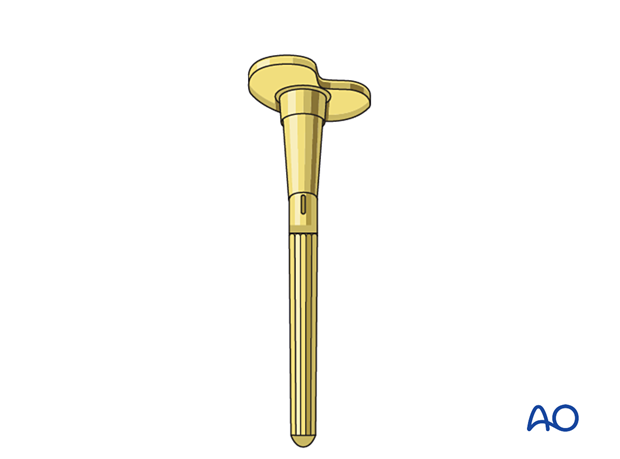
Supplemental metaphyseal fixation
The surgeon may consider using supplemental metaphyseal fixation of the tibia with a cone or a sleeve.
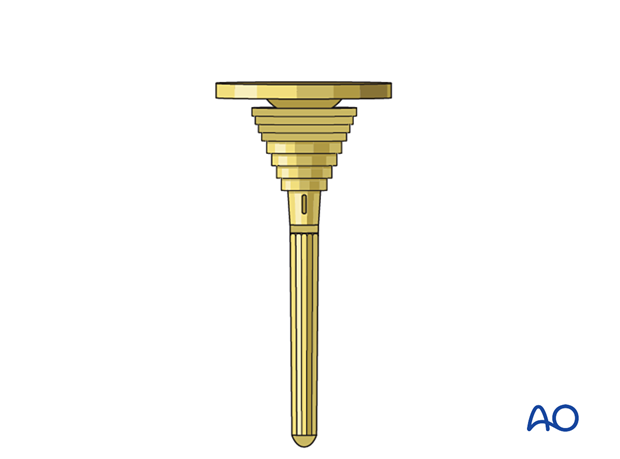
3. Patient preparation
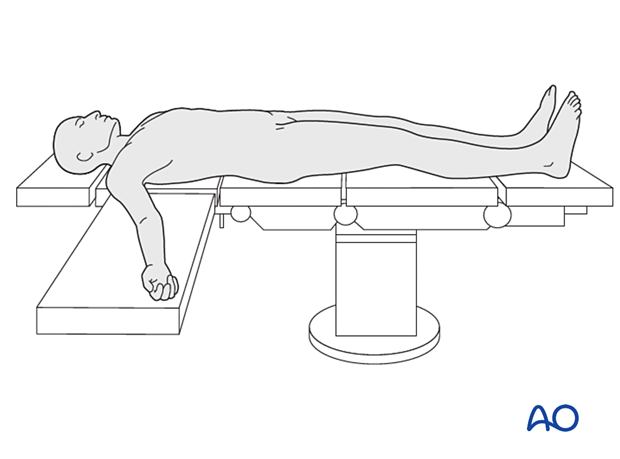
The patient is placed in the supine position. A radiolucent table may facilitate intraoperative fluoroscopy if required.
4. Surgical approach
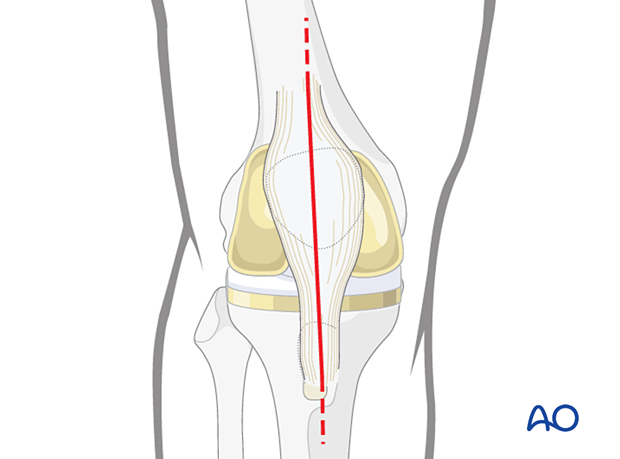
This procedure requires an adequate visualization of the knee joint. The most commonly used is a midline skin incision followed by a medial parapatellar arthrotomy. A proximal and distal extension may be necessary to achieve sufficient visualization and soft tissue releases.
5. Tibia
Tibial component removal
The tibial fracture should be stabilized with provisional fixation prior to the component removal.
Care should be taken to avoid excessive bone removal and/or fracture propagation when the component is removed.
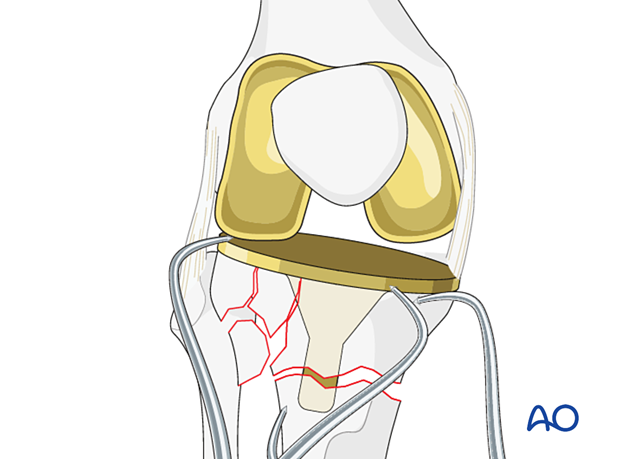
Tibial component removal is performed using a combination of a small oscillating saw and the cement osteotomes on the undersurface of the tibial tray.
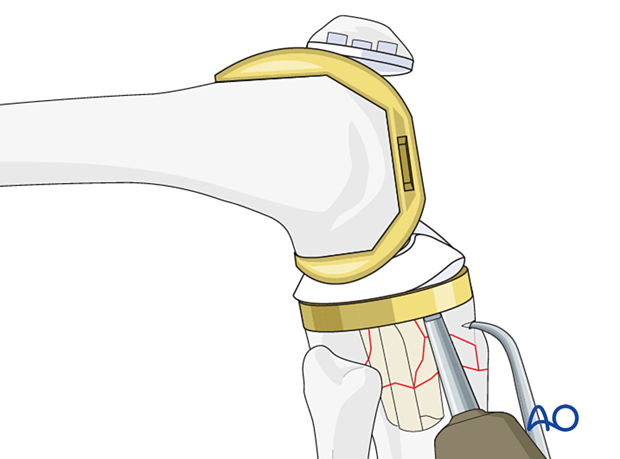
Cement in the tibial metaphysis around the keel of the tray is removed using cement osteotomes and cement hooks.
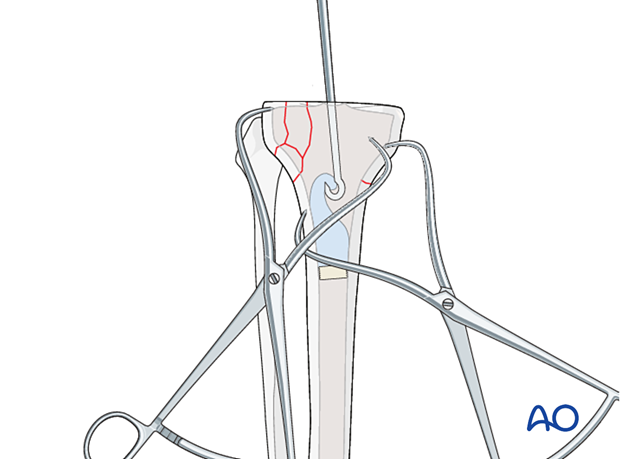
Preparation of the tibia
The tibial canal is prepared using reamers of increasing size.
The depth of the reaming is determined by the length of the selected stem.
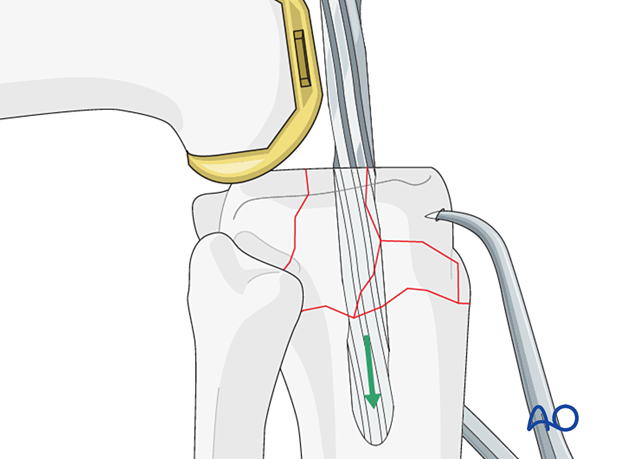
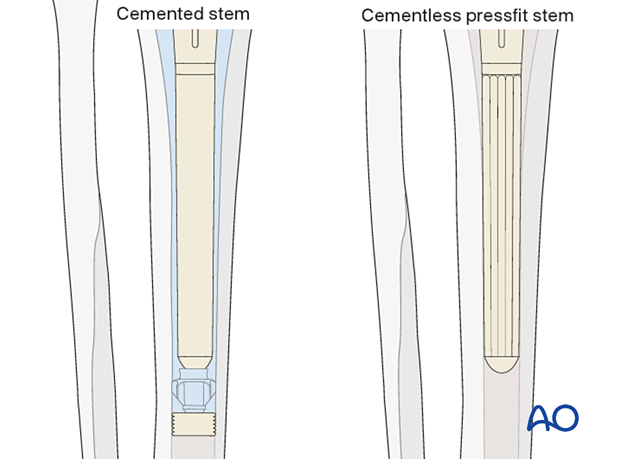
The diameter of the stem is determined by the reamer diameter which achieves cortical contact with the diaphyseal bone. One should allow for at least 2 mm of cement mantle around the stem if cement fixation is used.
If cementless stem fixation is selected, line to line fit of the reamer to the final stem diameter is used.
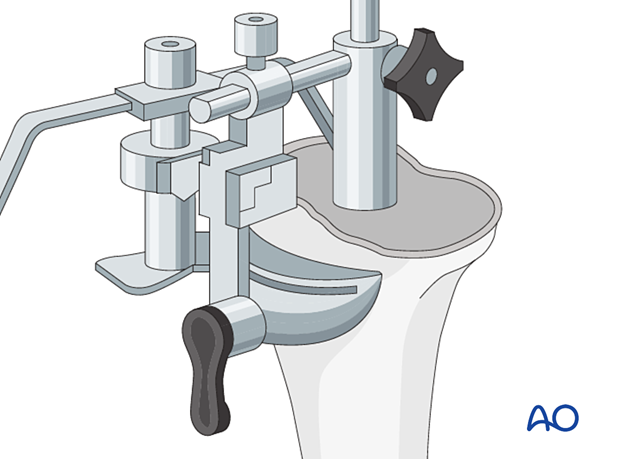
Using the reamer and the intramedullary tibial cutting jig, the upper tibia is recut to establish the proper coronal and sagittal alignment.
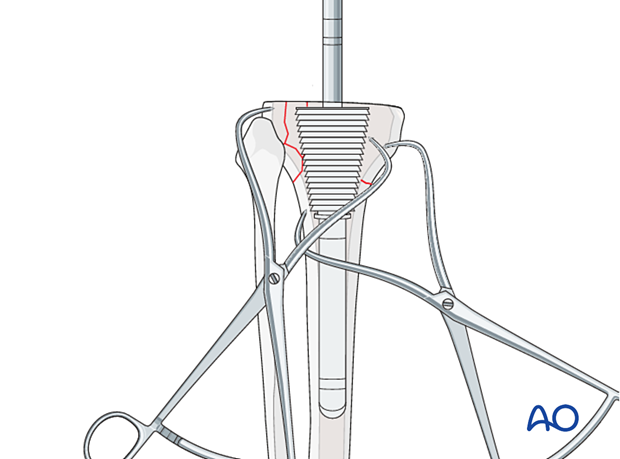
If there is bone deficiency due to fracture fragmentation, additional bone cuts may be required to remove the fragments and to accommodate the use of augments or wedges under the tibial tray.
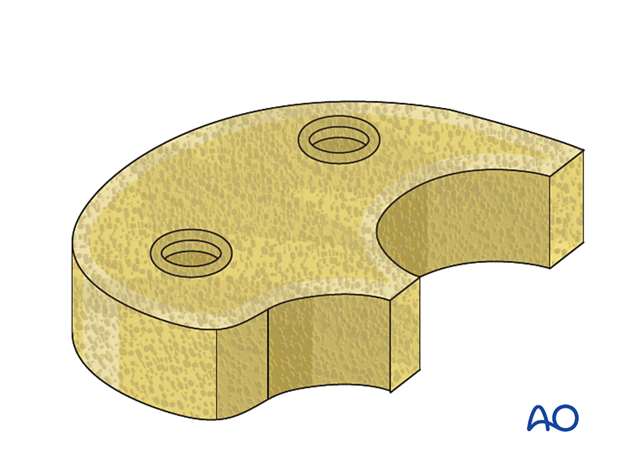
The tibial metaphysis is prepared with the proper instruments if a metaphyseal cone or a sleeve is to be used.
6. Femur
Femur revision techniques are described under the treatment: complete femoral revision with hinged knee.
7. Trial
The trial components are assembled, and a trial reduction is performed.
Leg length equalization is assessed with the proper polyethylene insert thickness.
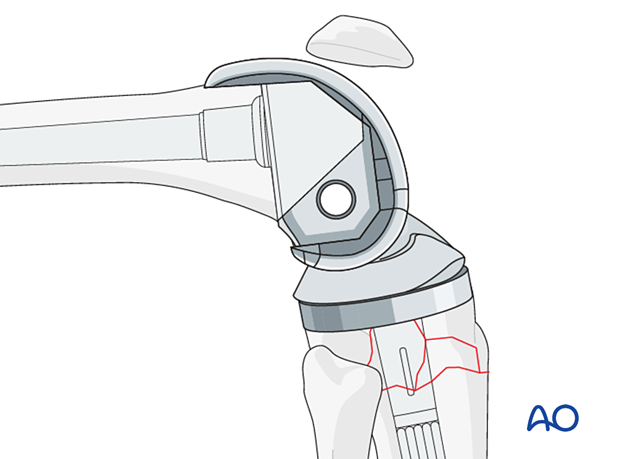
Patella tracking is carefully assessed to ensure no instability or impingement throughout the entire range of knee motion.
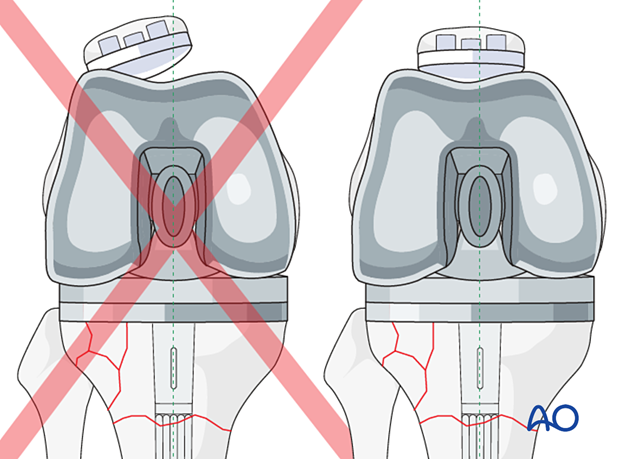
8. Component insertion
Bone preparation for cementing
The bone surface and canal are lavaged to remove any debris. The bone surfaces are dried before proceeding.
Cement restrictors
The cement restrictor is inserted into the tibial canal to allow for a 1 cm cement mantle between the stem tip and the restrictor.
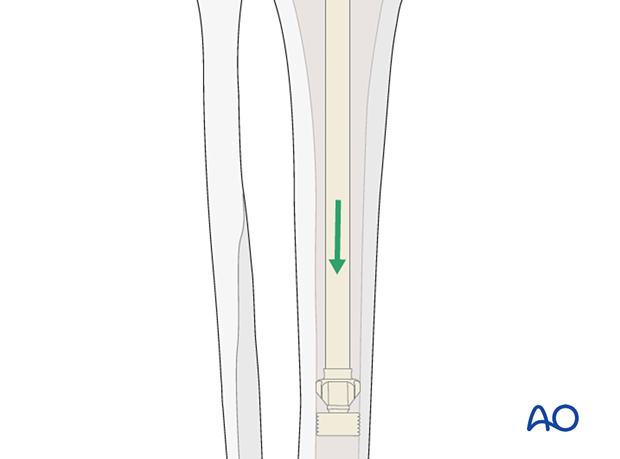
Supplemental metaphyseal fixation
If supplemental tibial metaphyseal fixation is selected, the cone is inserted first.
If a sleeve is selected, the sleeve is impacted on the tibial component and inserted as a monobloc implant.
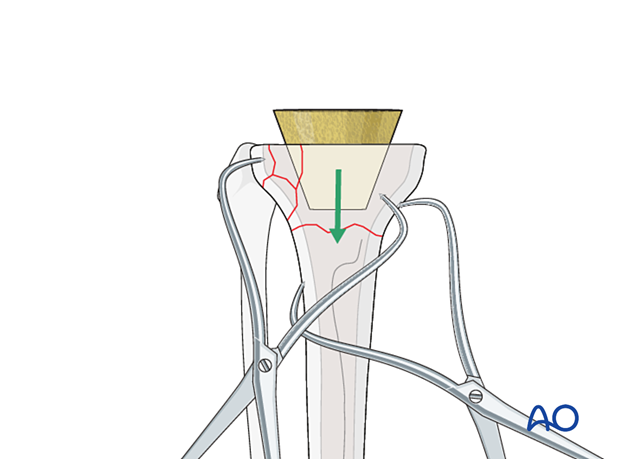
Cementation
Cement is mixed using standard techniques and injected into the canal with retrograde filling and pressurization, using a cement gun.
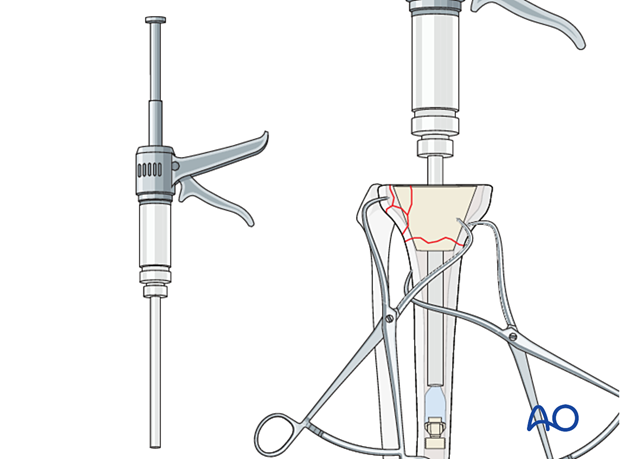
Insertion of tibial component
The tibial component (including any augment or wedge), is seated with rotational alignment to the tibial tubercle.
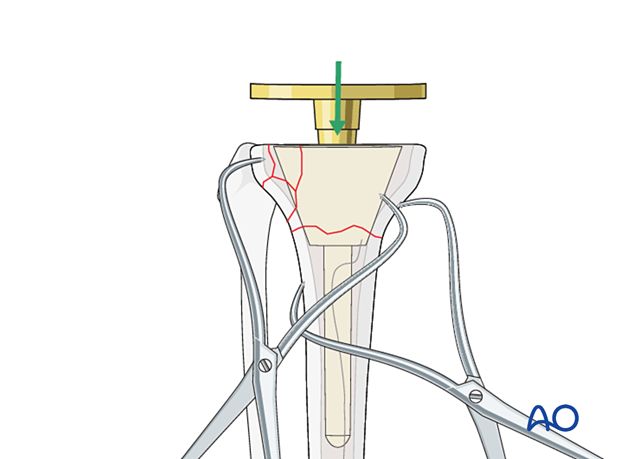
9. Final reduction
The selected polyethylene bearing along with the bushings for hinged articulation are assembled and coupled together. The knee is reduced, and patellar tracking is assessed.
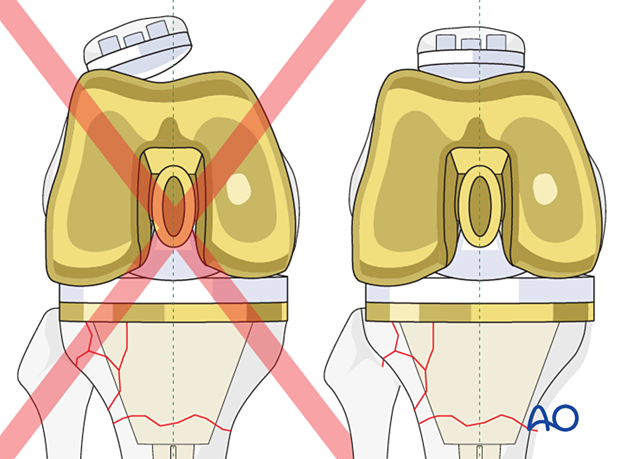
If patellar tracking is not ideal, a lateral retinacular release and medial imbrication can be performed.

10. Aftercare
The patient can be mobilized with full weight-bearing and active range of motion immediately after surgery.