ESIN (retrograde)
1. General considerations
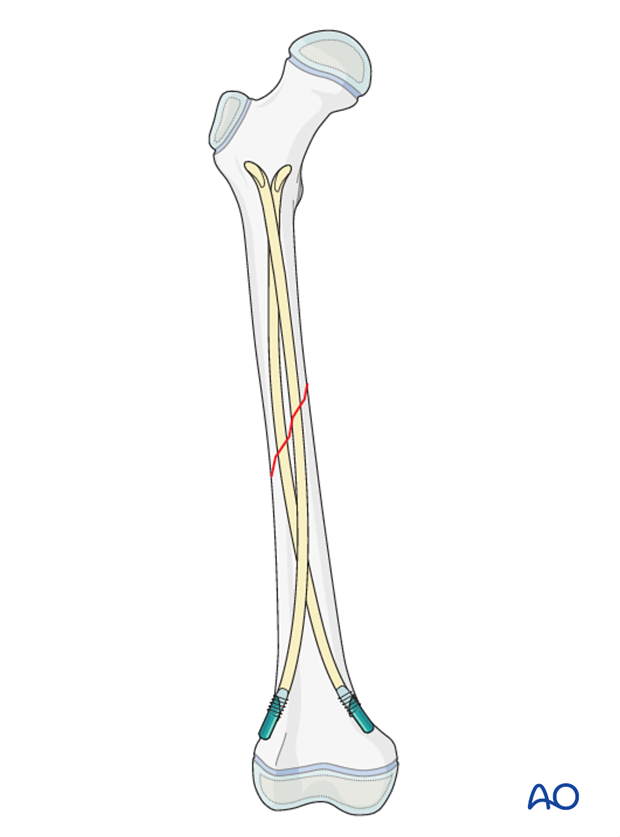
The ESIN method involves closed reduction and internal fixation with elastic nails.
It is difficult to treat shaft fractures of the middle and proximal third with antegrade nail insertion as the nail entry sites are close to the fracture and the configuration of the nails does not produce sufficient stability.
Using a retrograde nail construct will provide sufficient stability in these fractures.
2. Instruments and implants
Instrument set for ESIN
- 2.5–4.0 mm elastic nails
- Awl or drill
- Inserter
- Hammer
- End caps and insertion device
- Impactor
- Extraction plier
- Nail cutter
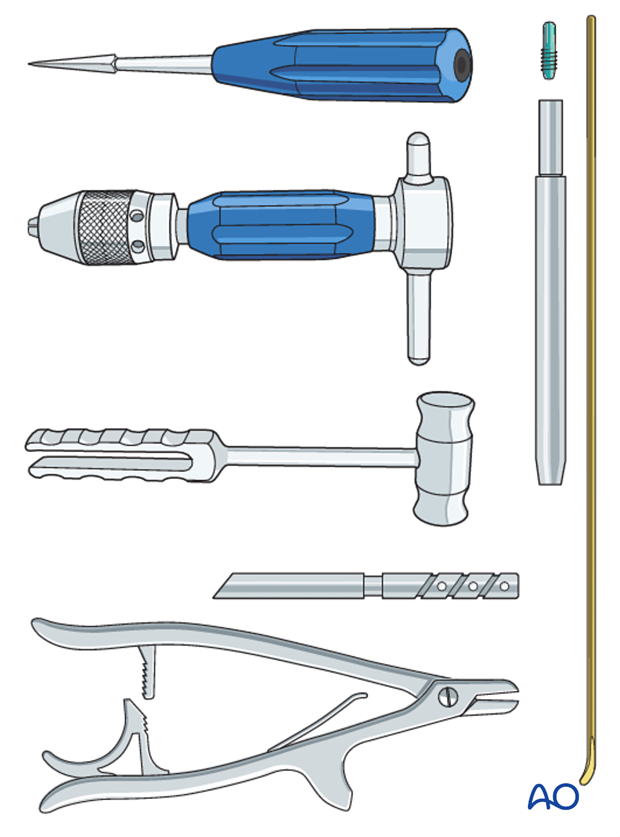
The end cutter is useful to avoid sharp ends and soft-tissue irritation.
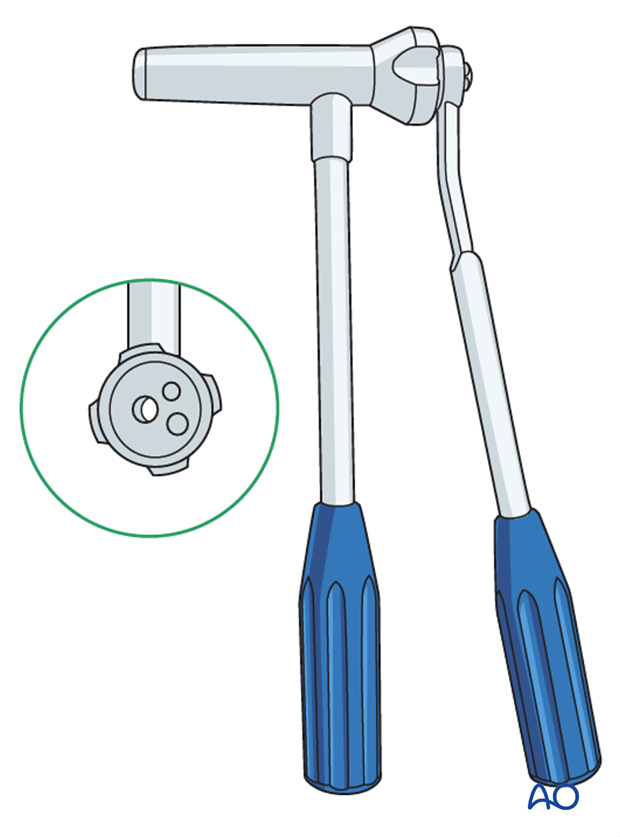
The F-tool can be helpful to align the femur.

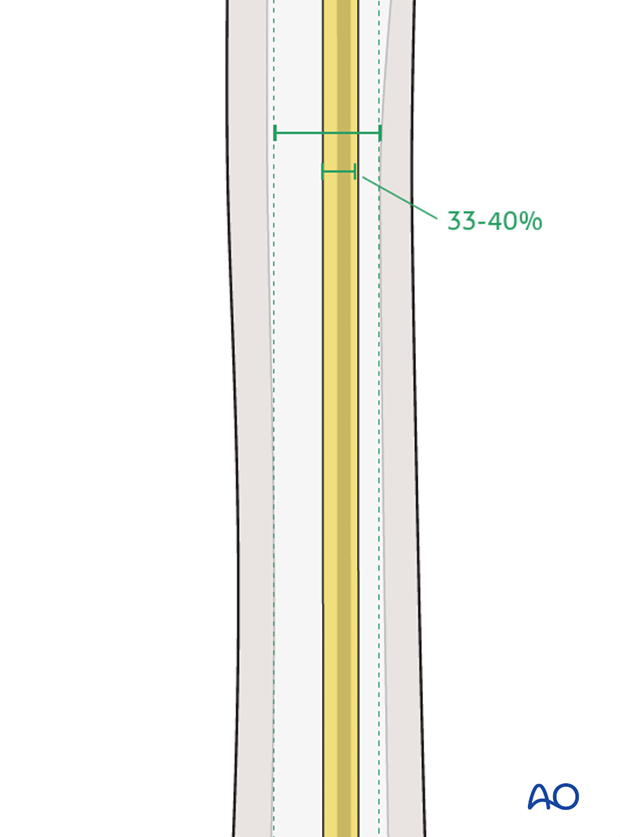
Nail diameter
For optimal stability, the nail diameter should be between 33% and 40% of the narrowest part (isthmus) of the medullary canal.
Both nails need to be of the same diameter.
For later precontouring mark the level of the fracture site on the nail.
3. Patient preparation and approach
Patient positioning
Place the patient in a supine position on a radiolucent fracture table with or without traction.
When positioning the patient check the rotational alignment of the uninjured femur.
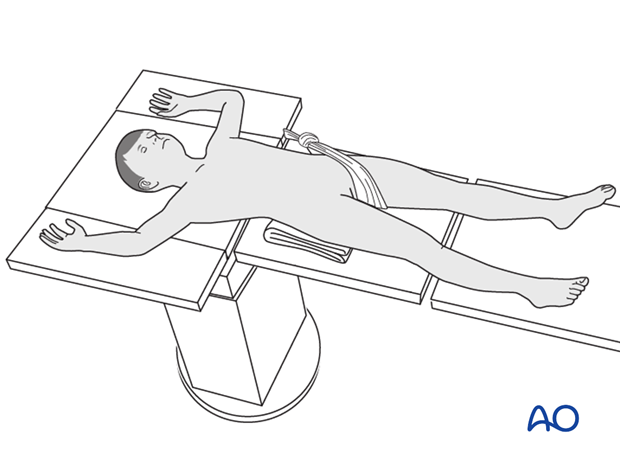
Approach
Expose the bone at both entry points.
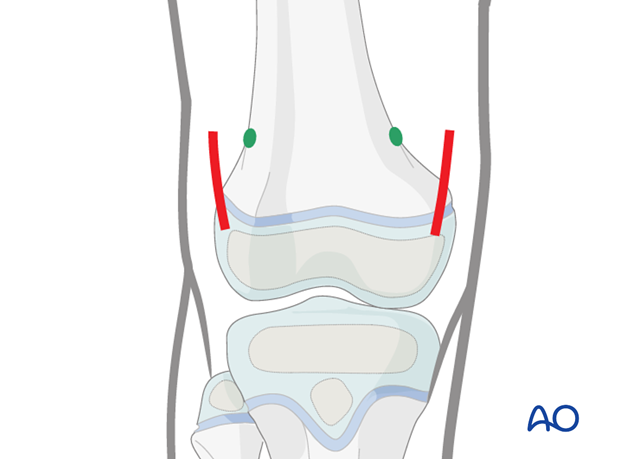
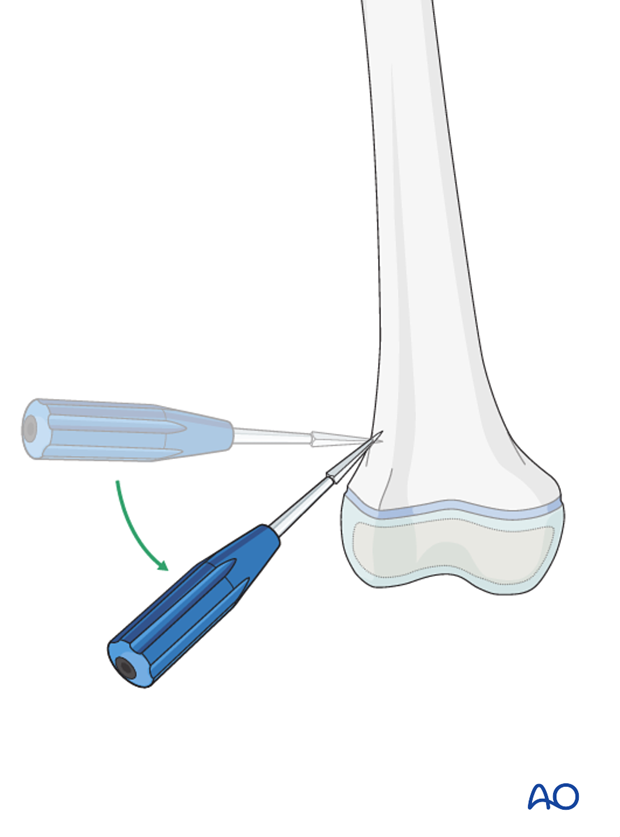
4. Opening the canal
Place the awl or drill directly onto the bone and perforate the near cortex, under direct vision, perpendicular to the bone.
Do not hammer the awl to avoid perforation of the far cortex.
When the medullary canal is entered, lower the awl or drill 45° to the shaft axis. Advance it with oscillating movements to produce an oblique canal.
5. Nail insertion
Precontour both nails with the apex at the level of the fracture site.
The nail bend should be about three times the diameter of the medullary canal.
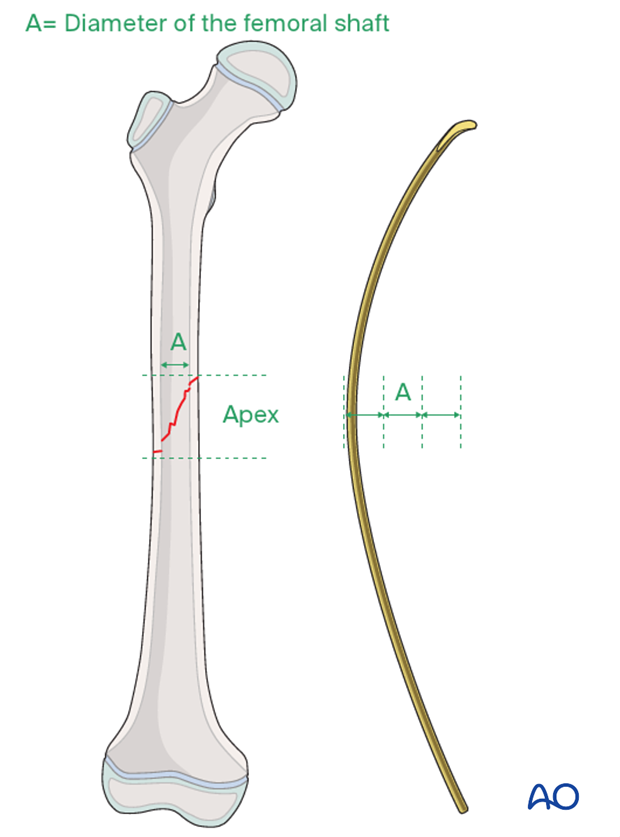
Insert the first nail through the lateral entry point into the intramedullary canal and advance it towards the fracture site with an oscillating maneuver.
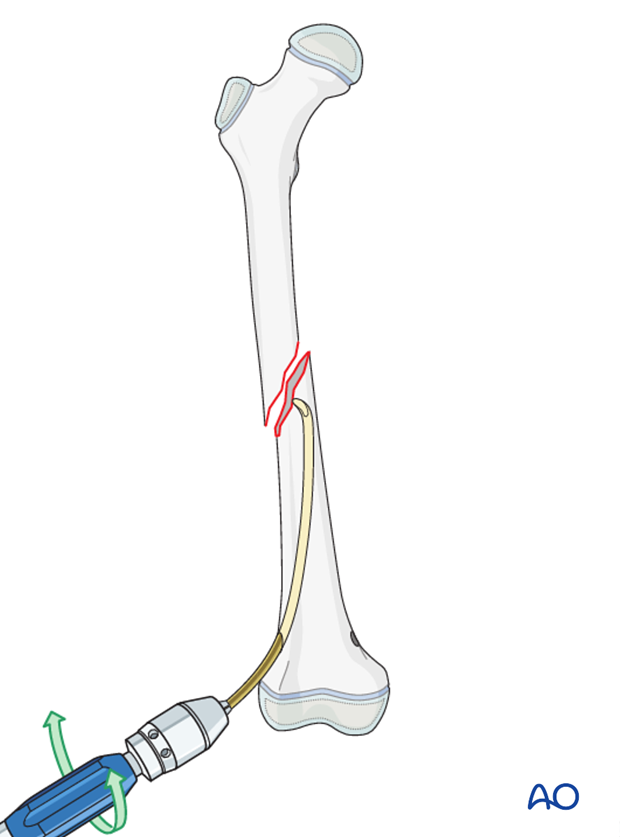
If the tip is stuck in the far cortex and cannot be advanced, remove the nail and bend the tip to give a slightly more pronounced curvature.
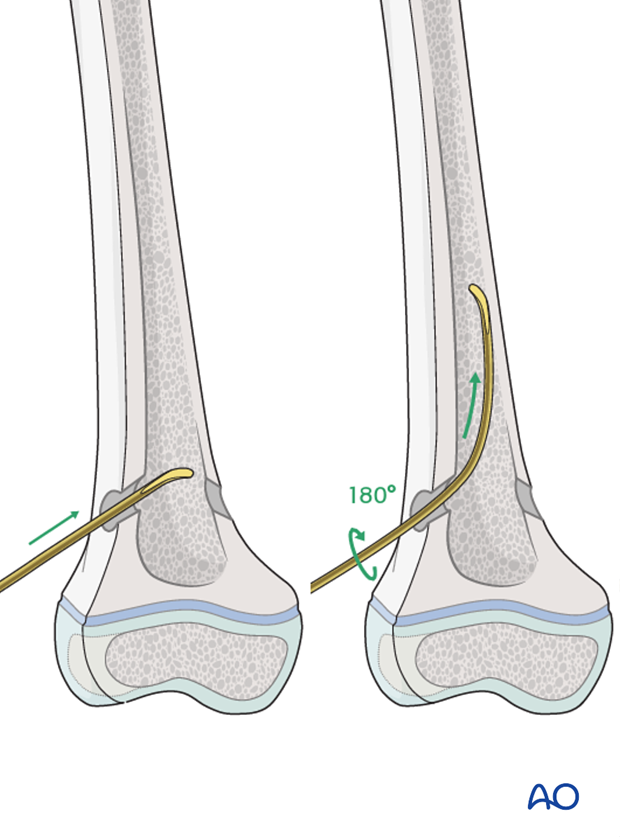
Insert the second nail into the medial entry point in an identical manner.
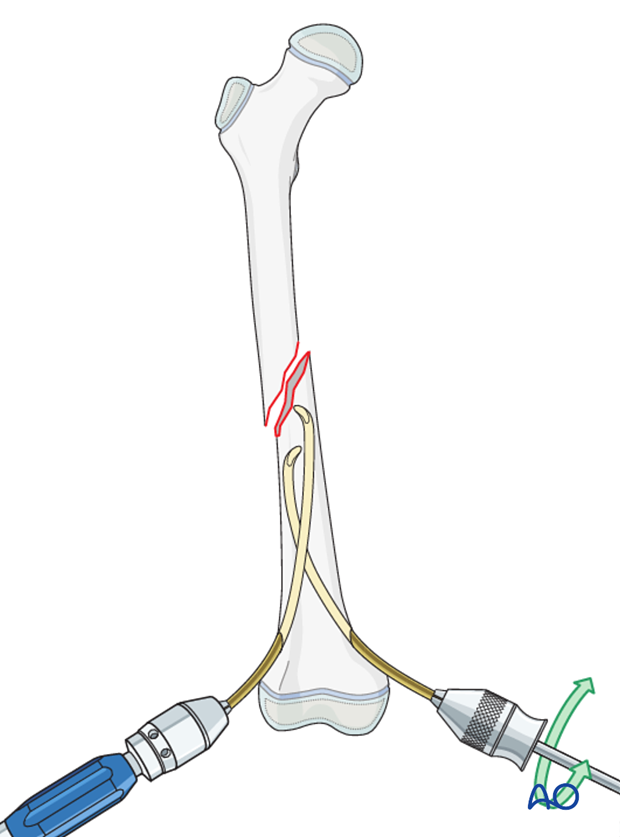
If this happens reinsert a new nail.
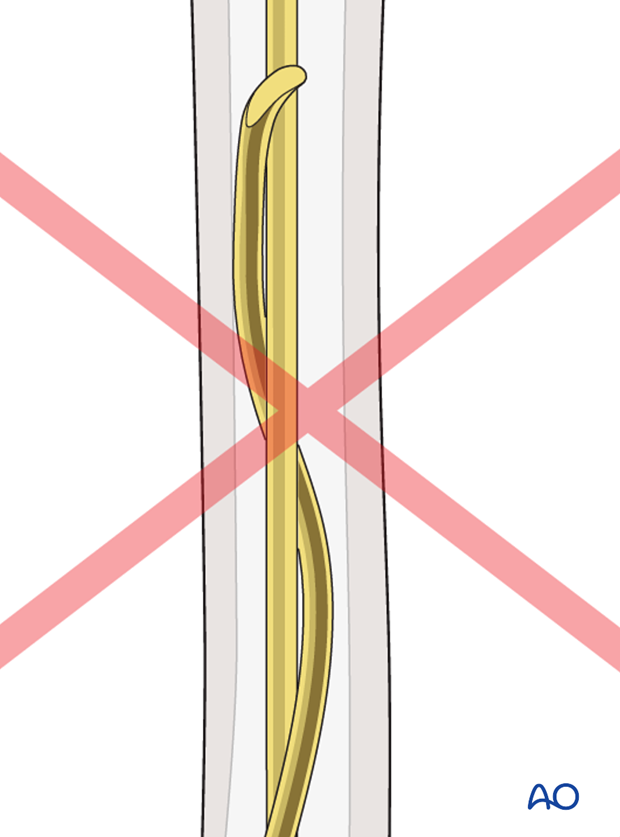
6. Proximal fragment advancement
Advance the first nail past the fracture zone and into the distal fragment with an oscillating maneuver.
Advance the second nail in the same way.
Use the nails as joysticks to reduce the main fragments.
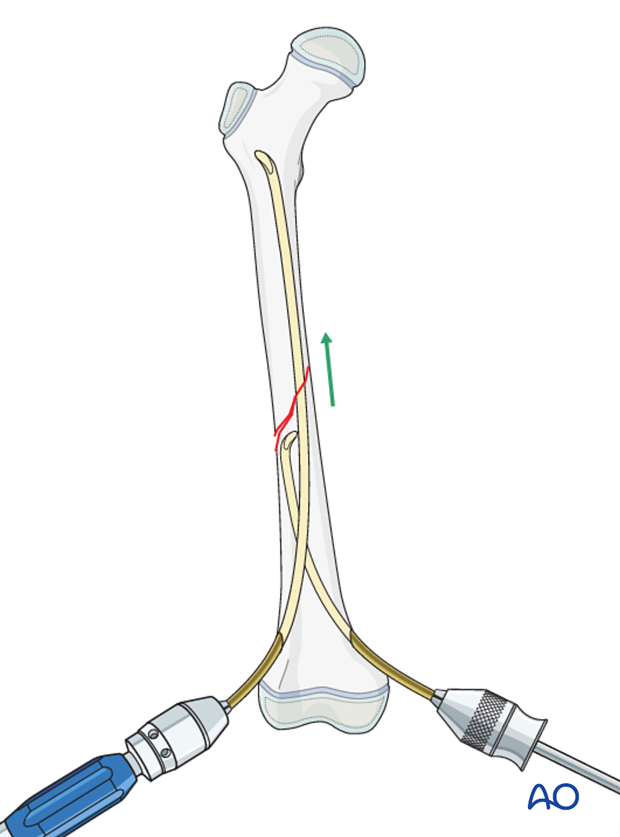
If necessary, use an F-tool to align both fragments.
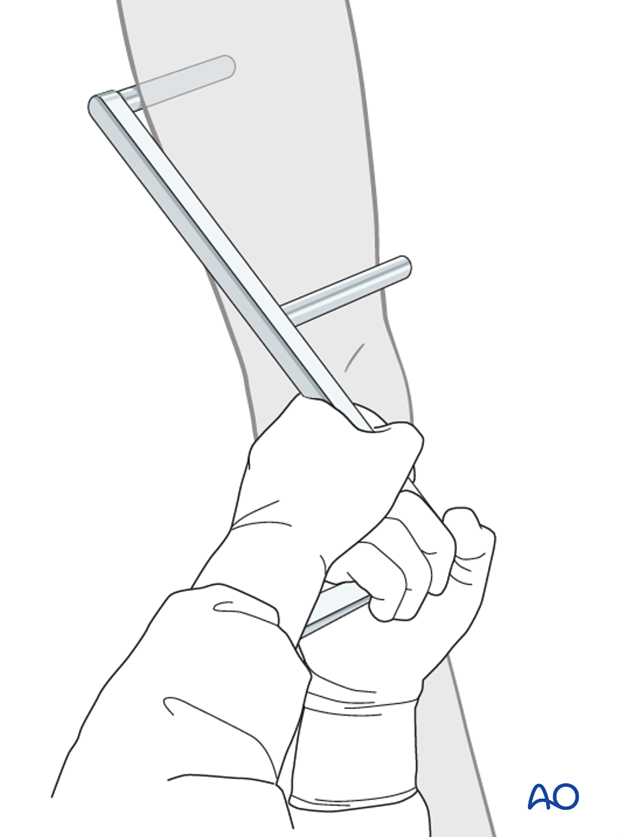
If this is unsuccessful use a bone hook or Steinmann pin through a small incision.
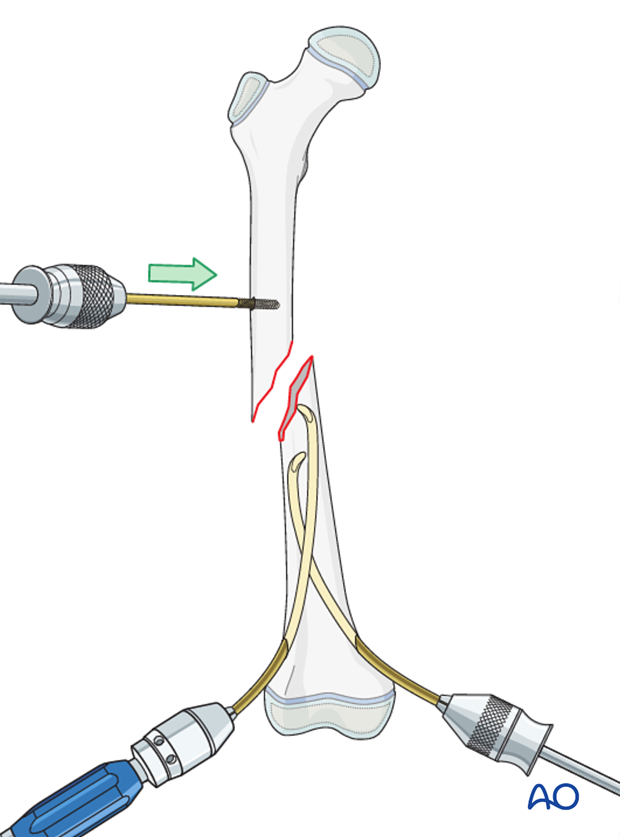
Open reduction (through a limited lateral approach) may be necessary if closed reduction cannot be achieved.
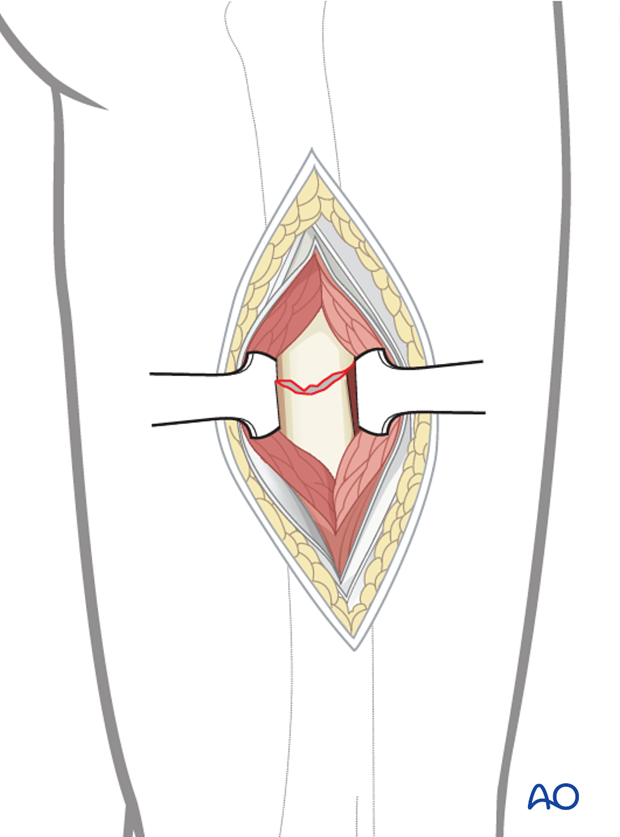
Assessment of rotational alignment
Confirm rotational alignment of the femur clinically and radiographically before fixing the second fragment. This can be done by:
- Fluoroscopy of the fracture site (matching shaft diameters)
- Comparing internal and external rotation to the contralateral side (consider preparing and draping the uninjured side as well)
- Fluoroscopy of proximal femur (lesser trochanter profile)
For more detail see the additional material on assessment of rotation.
7. Final seating
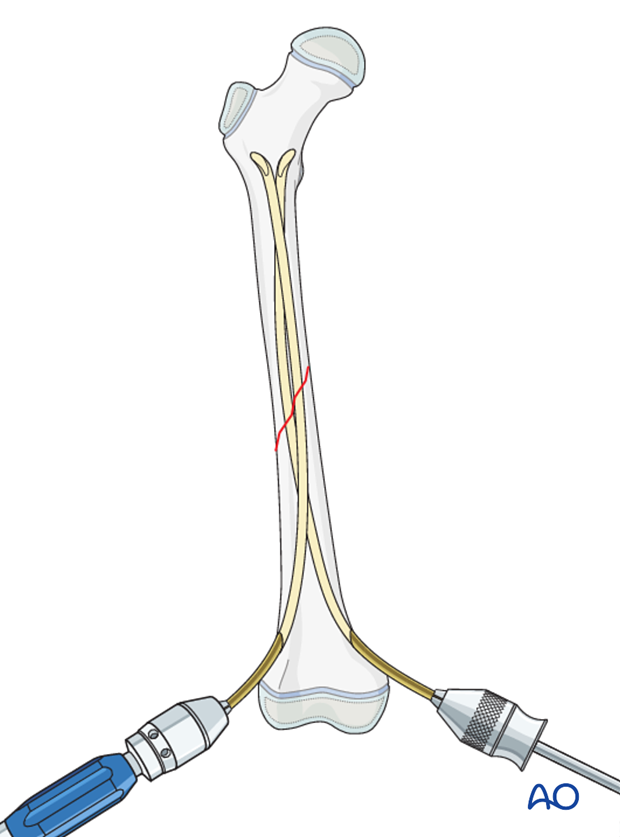
Advance the nail started on the medial side and impact it at least to the level of the lesser trochanter.
Impact the nail started on the lateral side towards the greater trochanter. Optimally the nail tips are at the same level.
Align the nail tips so that they diverge.
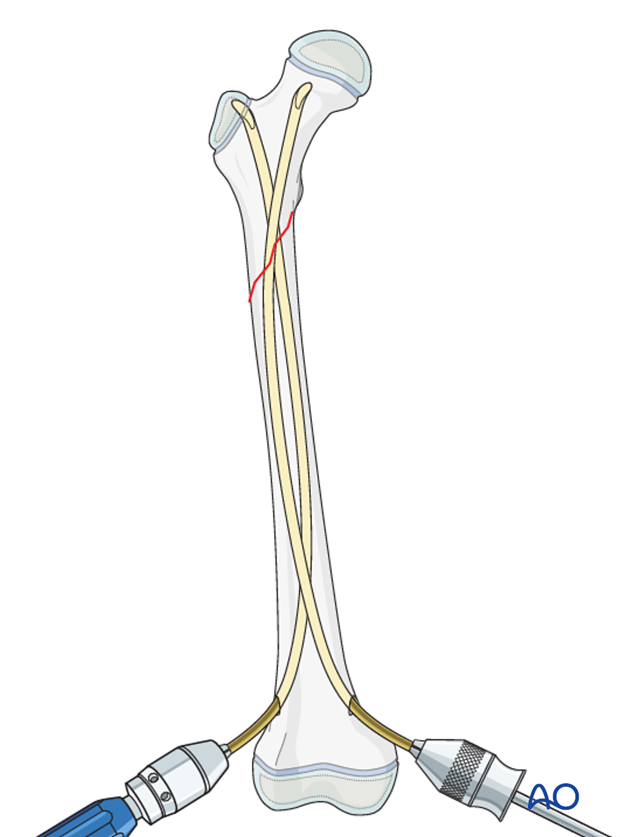
For a fracture in the proximal third advance the medial nail into the femoral neck and the lateral nail into the greater trochanter.
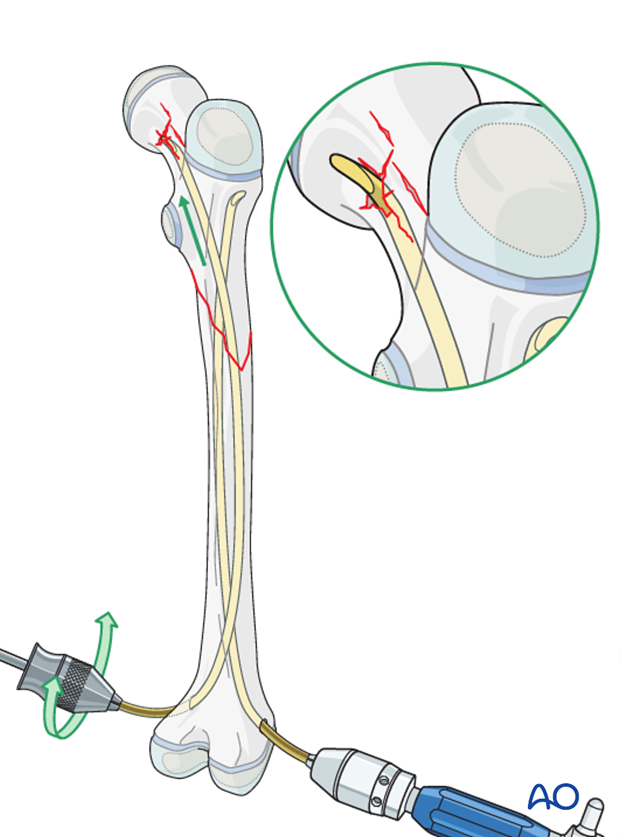
Pitfall: penetration of femoral neck
Use lateral image intensifier views to confirm correct position.
8. Cutting the nails
Cut the nails with the dedicated nail cutter.
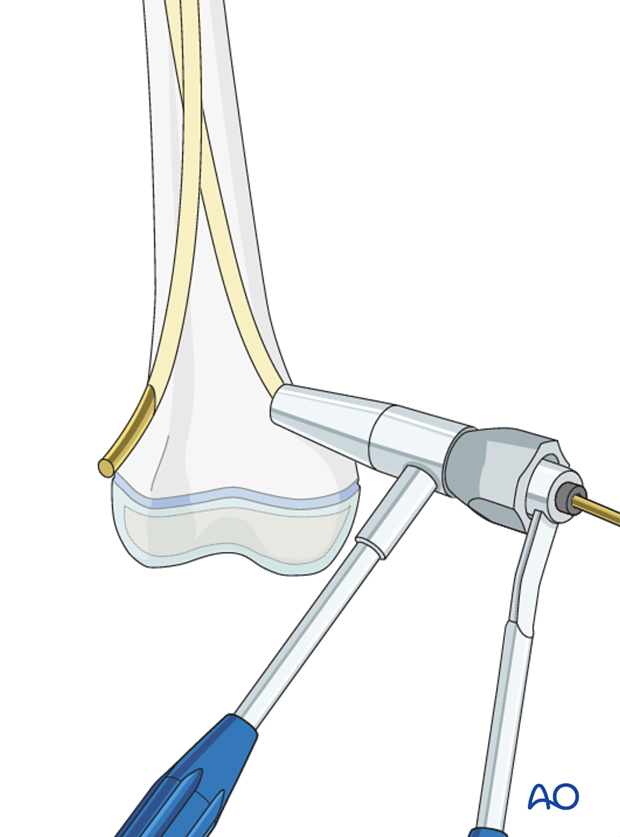
If this is not available, withdraw the nails far enough to apply the nail cutter.
Reinsert the nails so at least 1 cm of the nail remains outside the bone.
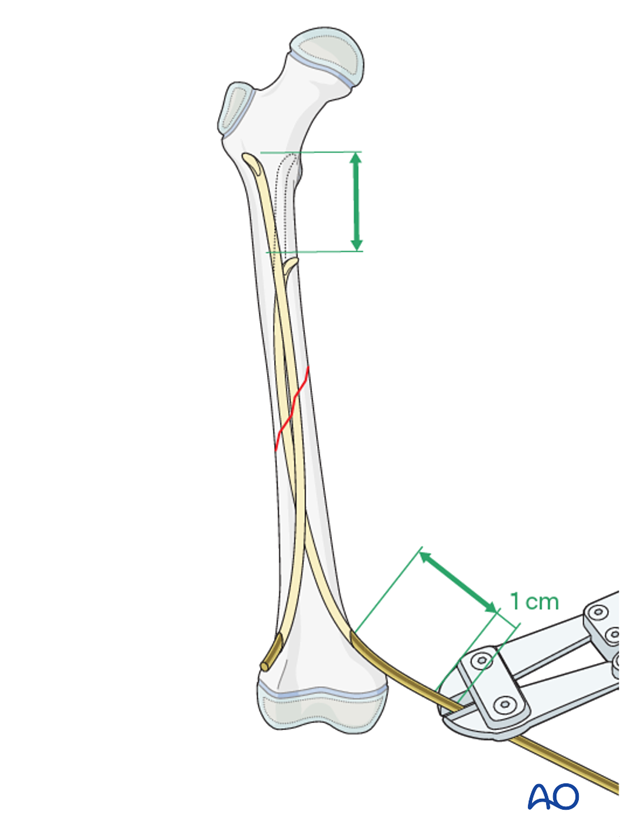
The ESIN impactor can be used to ensure the optimal length of the nail outside the bone to apply an end cap.
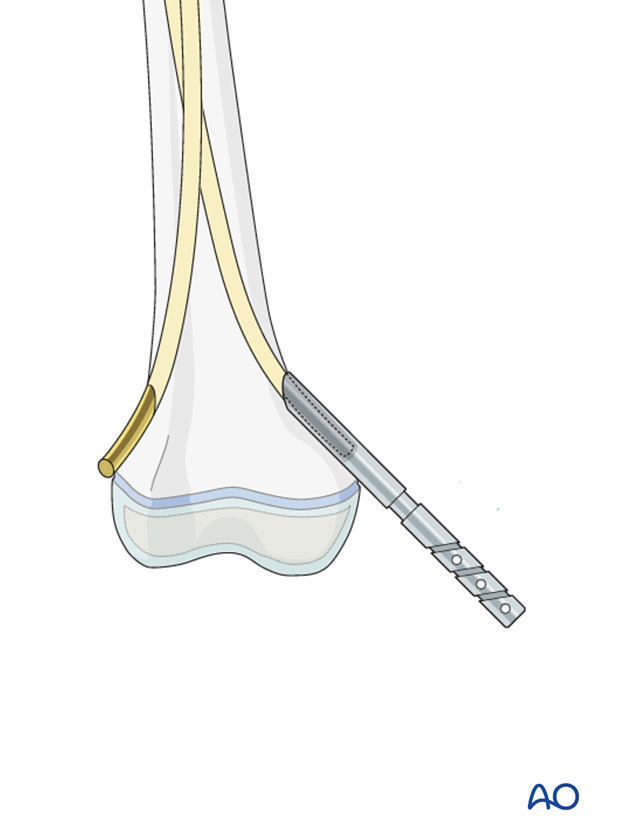
End caps
End caps can be used to increase axial stability.
They will also protect soft tissues.
Insert the end cap over the cut end of the nail and screw it into the metaphysis.
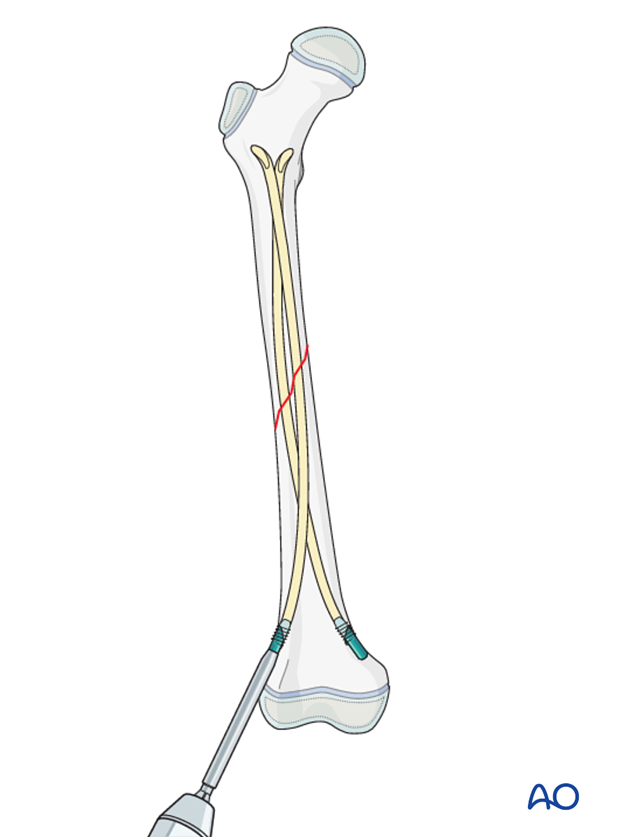
Confirm that the end cap is covering the nail and fixed to the bone with image intensification.

9. Final assessment
Check the range of internal and external rotation of the leg and compare with the contralateral limb.
Obtain final AP and lateral fluoroscopic views.
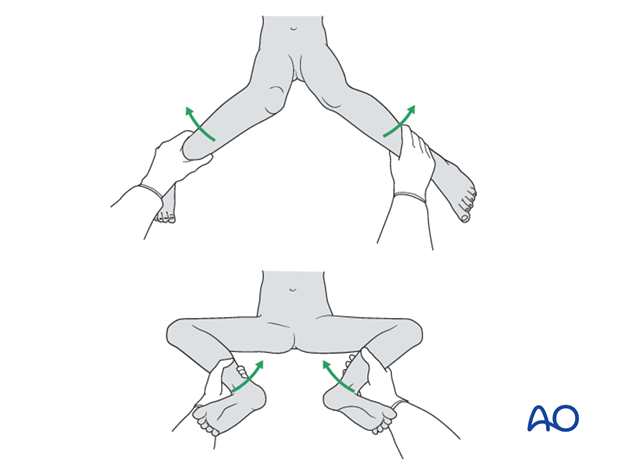
10. Aftercare
Immediate postoperative care
The patient should get out of bed and begin ambulation with crutches on the first postoperative day.
In most cases the postoperative protocol will be protected weight bearing for the first 4 weeks.

Analgesia
Routine pain medication is prescribed for 3–5 days postoperatively.
Neurovascular examination
The patient should be examined frequently, to exclude distal neurovascular compromise.
Compartment syndrome, although rare, should be considered in the presence of severe swelling, increasing pain, and changes to neurovascular signs.
Discharge care
Discharge from hospital follows local practice and is usually possible after 1–3 days.
Mobilization
The patient should ambulate with crutches and begin knee range-of-motion exercises.
Follow-up
Clinical and radiological follow-up is usually undertaken every 2–8 weeks until radiographic healing and restoration of function.
Clinical assessment of leg length and alignment is recommended at one-year.
Clinical assessment of leg length uses a tape measure from the ASIS to the medial malleolus.
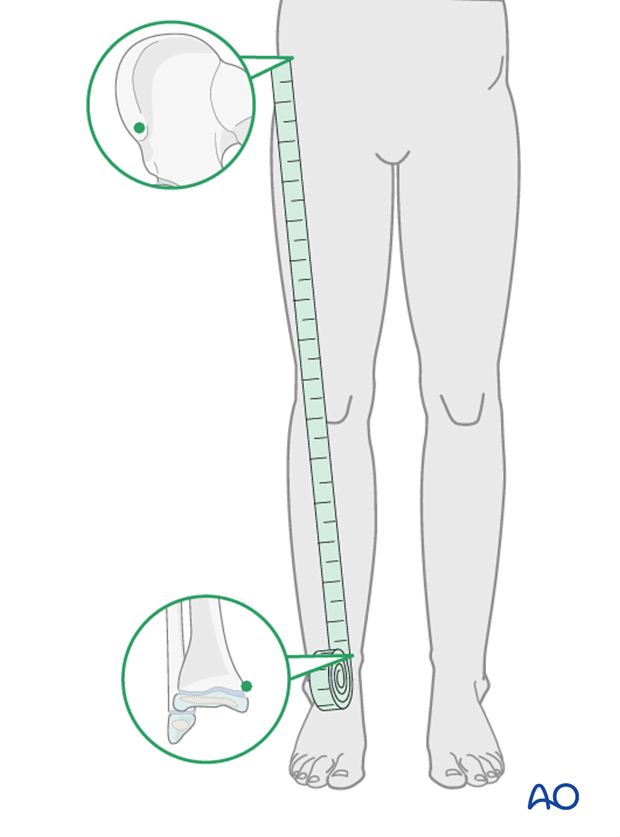
If there is any concern about leg length discrepancy or malalignment, long-leg x-rays are recommended.
Leg length is measured from the femoral head to the ankle joint.
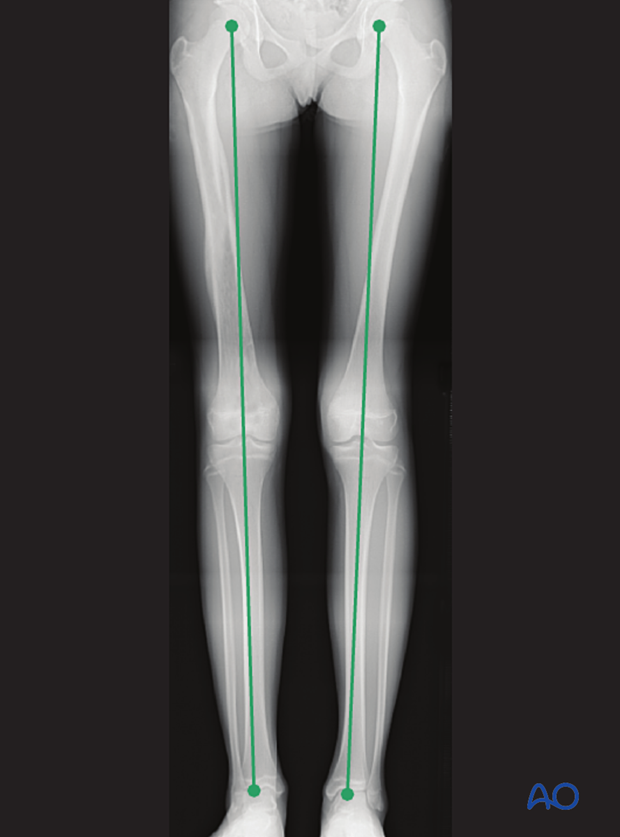
Implant removal
If the patient develops symptoms related to the implant, it can be removed once the fracture is completely healed, usually 6–12 months following injury.













