Closed elbow reduction; splint immobilization
1. Introduction
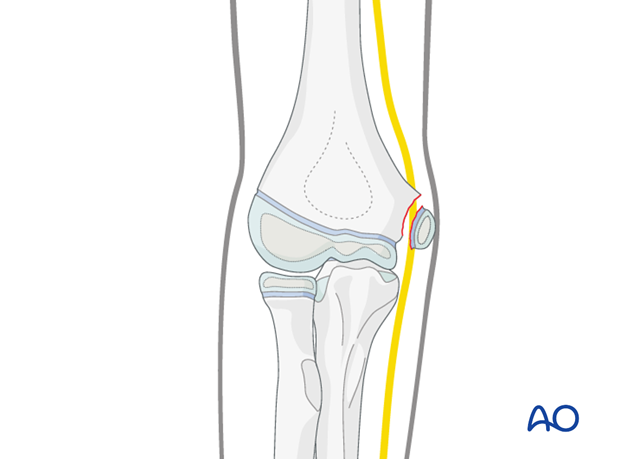
The medial epicondyle fracture is an avulsion fracture of the apophysis and often accompanies elbow dislocation. Closed reduction of the medial epicondyle is most successful if done at the time of reduction of the elbow dislocation itself.
If the medial epicondylar fragment is trapped in the joint, open reduction is often necessary, although the following closed reduction maneuver can be attempted.
The main soft tissue attachments of the medial epicondyle are the flexor-pronator muscles of the forearm. These remain attached to the fragment and can be used to aid closed reduction.
Percutaneous fixation is not recommended due to vulnerability of the ulnar nerve.
2. Patient preparation
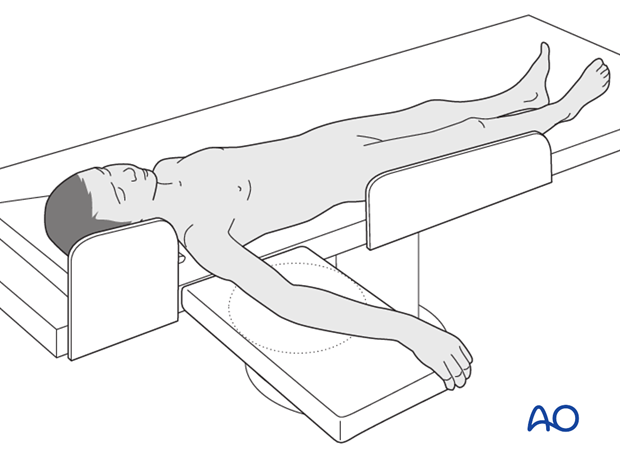
This procedure is normally performed with the patient in a supine position.
3. Closed extraction of the medial epicondyle from the elbow
With the elbow near full extension, a gentle valgus force is applied to open the medial side of the joint.
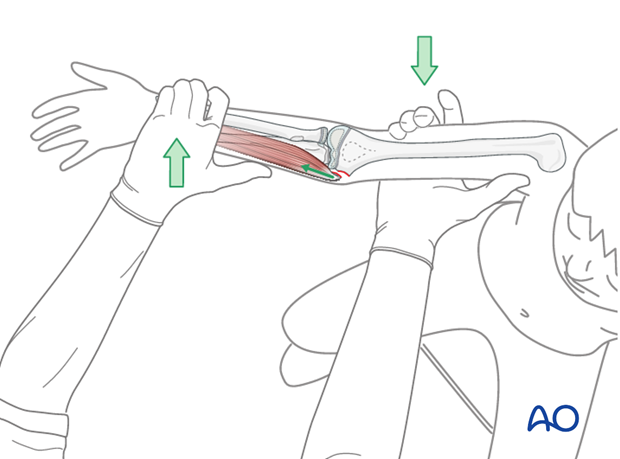
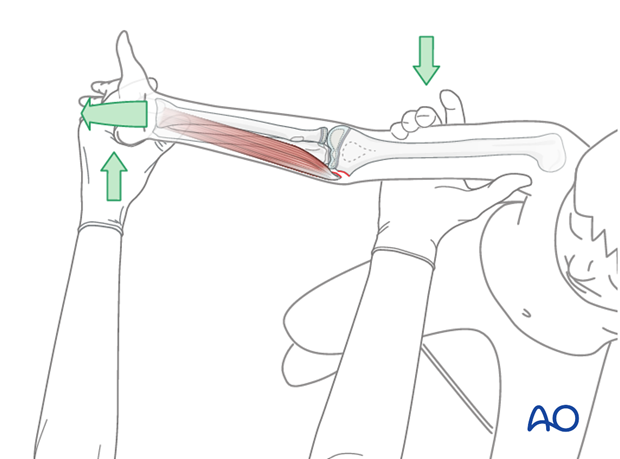
The fingers and wrist are fully extended, while the forearm is fully supinated.
This causes the flexor-pronator mass to pull the medial epicondyle away from the elbow joint.
The elbow joint itself is then reduced by longitudinal traction followed by flexion.
A complete and congruent reduction of the radiocapitellar and humeroulnar articulations, as well as the position of the medial epicondyle, are assessed using image intensification.
4. Splint application
With the elbow positioned in 90° of flexion, a posterior plaster backslab is applied.
The addition of medial and lateral slabs stiffens the splint and prevents it from flexing and extending.
The splint should be removed after 10–14 days to allow rehabilitation to commence.
Application of splint
A splint of fiberglass or plaster is applied on the posterior aspect of the arm and forearm. It should be wide enough to cover more than half the circumference of the arm and forearm.
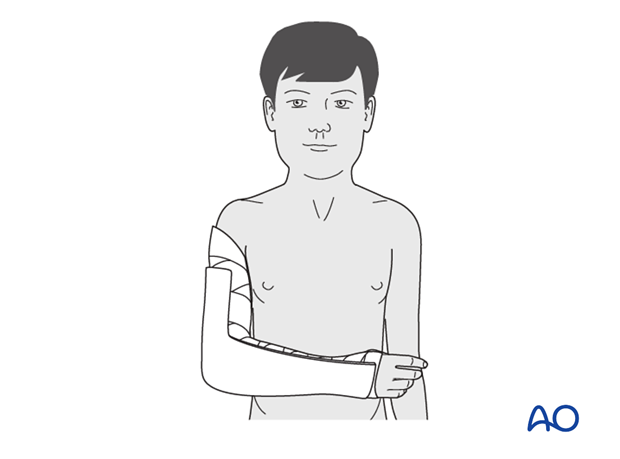
The splint is secured with a noncompressive bandage.
It is very important to ensure that this is not tight and can accommodate subsequent swelling.

Sling
The injured arm is supported with a sling.

Analgesia
Nonnarcotic analgesia may be required.
Caregivers should be taught to monitor for excessive pain or other signs of potentially dangerous swelling.
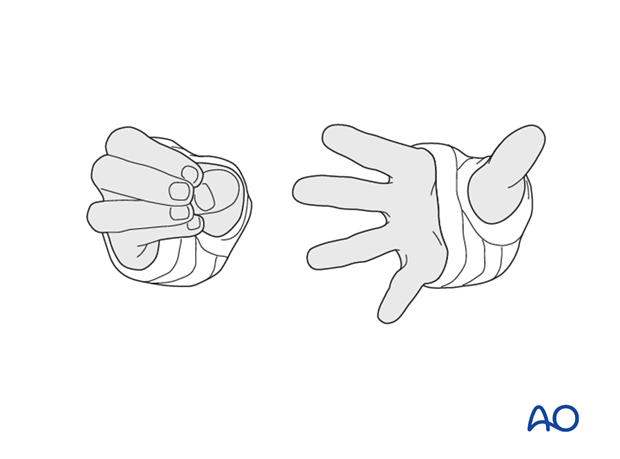
The ability to passively or actively fully extend the fingers without discomfort indicates normal perfusion and absence of neurological compression.
5. Aftercare
Compartment syndrome
Compartment syndrome is a possible early postoperative complication that may be difficult to diagnose in younger children.
The child should be examined frequently, to ensure finger range of motion is comfortable and adequate.
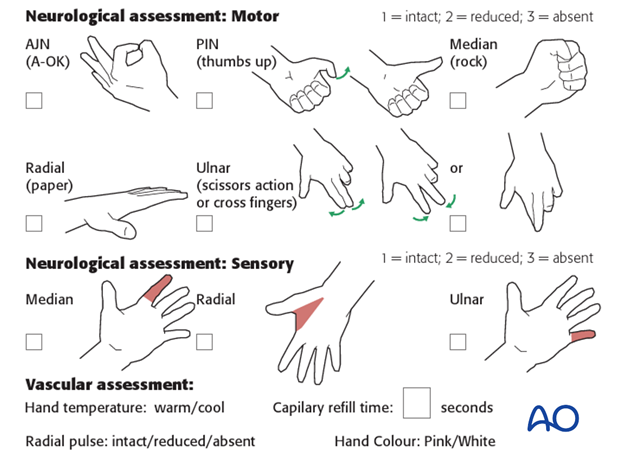
Neurological and vascular examination should also be performed.
Increasing pain, decreasing range of finger motion, or deteriorating neurovascular signs should prompt consideration of compartment syndrome.
Discharge care
When the child is discharged from the hospital, the parent/caregiver should be taught how to assess the limb.
They should also be advised to return if there is increased pain or decreased range of finger motion.
It is important to provide parents with the following additional information:
- The warning signs of compartment syndrome, circulatory problems and neurological deterioration
- Hospital telephone number
- Information brochure
For the first few days, the elbow and forearm can be elevated on a pillow, until swelling decreases and comfort returns.
Follow-up x-rays
Control x-rays may be taken at one week following injury to assess fracture position. Further x-rays may be necessary at three weeks to assess fracture healing.
Recovery of motion
As symptoms recover, the child should be encouraged to remove the sling and begin active movements of the elbow.
The majority of elbow motion is recovered rapidly, usually within two months of splint removal. The older child may take a little longer.
Once the child is comfortable, with a nearly complete range of motion, he/she may resume noncontact sports incrementally. Resumption of unrestricted physical activity is a matter of judgment for the treating surgeon.













