Open reduction; plate fixation
1. General considerations
Introduction
Metaphyseal fractures can be managed with open reduction and plate fixation.
In fractures with insufficient distal metaphyseal length, it may be necessary to cross the growth plate.
Most pediatric metaphyseal fractures heal when fixed with relative stability.
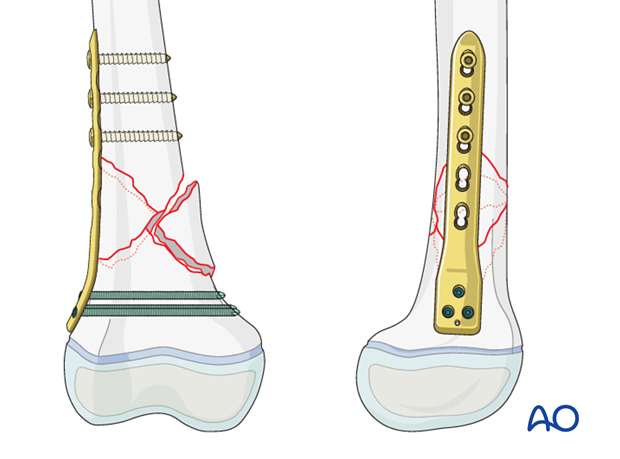
Size and type of implant
The size and type of implant is determined by the size and age of the patient as well as by the fracture pattern. The range of plate sizes in pediatric femur fractures is between 2.7 and 5.0 mm.
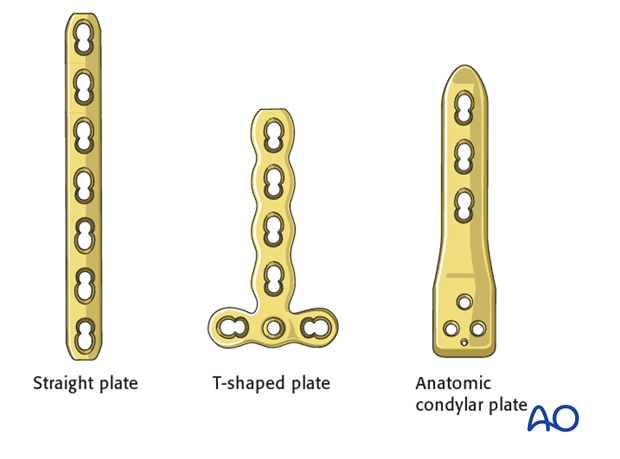
In more proximal metaphyseal fractures, a straight plate can be used.
In more distal metaphyseal fractures, a T-shaped plate can be used.
There are anatomic condylar plates specifically designed for pediatrics which are also an option.
Adult anatomic plates may be appropriate for patients with a closing growth plate or, in rare cases, where stable fracture fixation requires bridging (and potentially sacrificing) the growth plate.
2. Patient preparation and approach
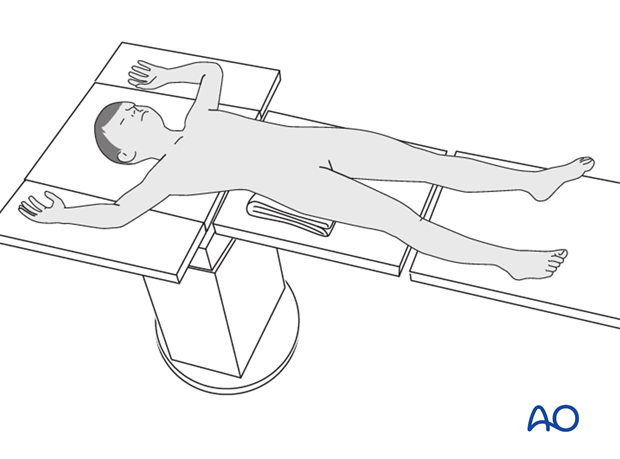
Patient positioning
Place the patient supine on a radiolucent table with a C-arm.
Approach
The majority of the fractures are approached using the distal component of a direct lateral incision.
Confirm the location of the growth plate with image intensification and protect it, taking care not to strip the adjacent periosteum.

3. Reduction
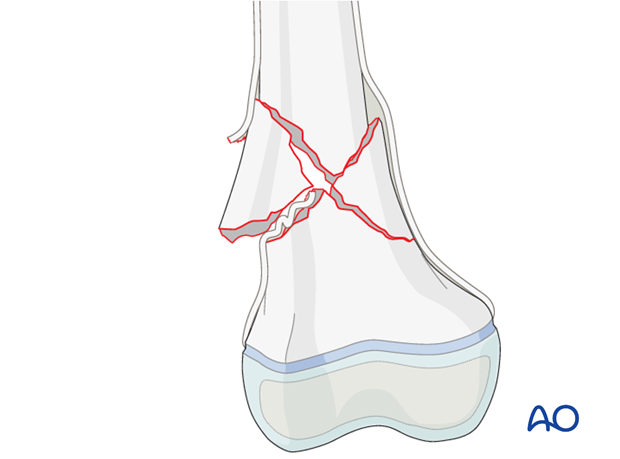
Removal of impediments
It may be necessary to remove interposed soft-tissue and periosteum prior to reduction of the fracture under direct vision, but not at the cost of devitalizing fragments.
Reduction aids
Open reduction is aided by:
- Bolsters placed posterior to the distal diaphyseal region to correct a hyperextension deformity of the distal femoral articular block
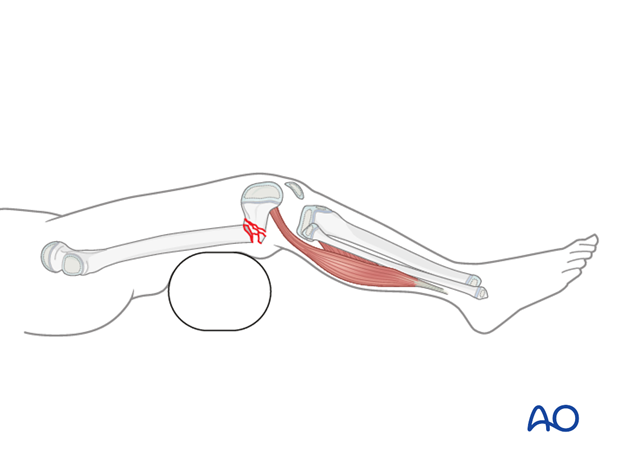
- Manual traction, to restore length of the limb
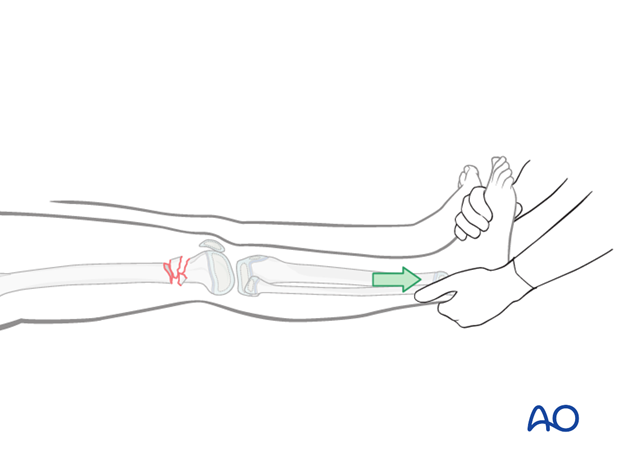
4. Plate fixation
Plate placement
Plate contouring is often required to match the overall anatomy of the femur but it is not necessary to anatomically reduce the individual fragments.
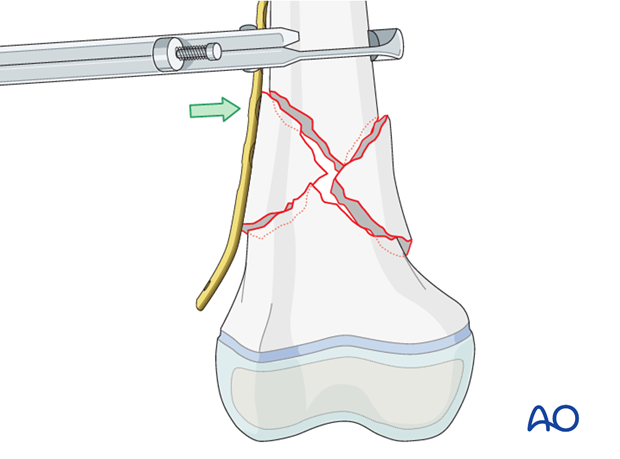
Secure the plate with bone holding forceps.
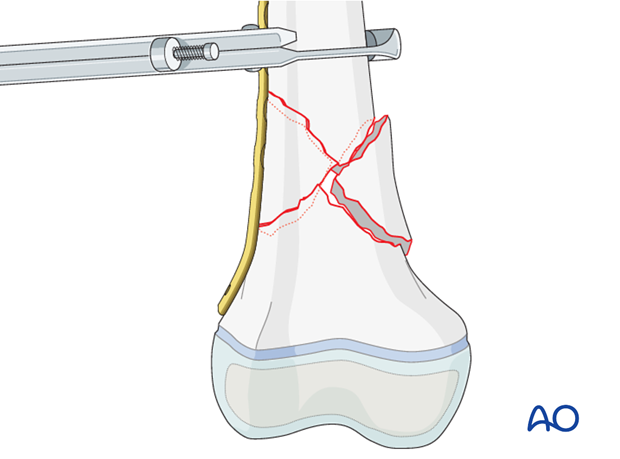
To control the position of the distal fragment, it may be necessary to introduce a temporary K-wire through the positioning hole in the most distal part of the plate.
In low fractures, take care that the K-wire does not cross the growth plate.
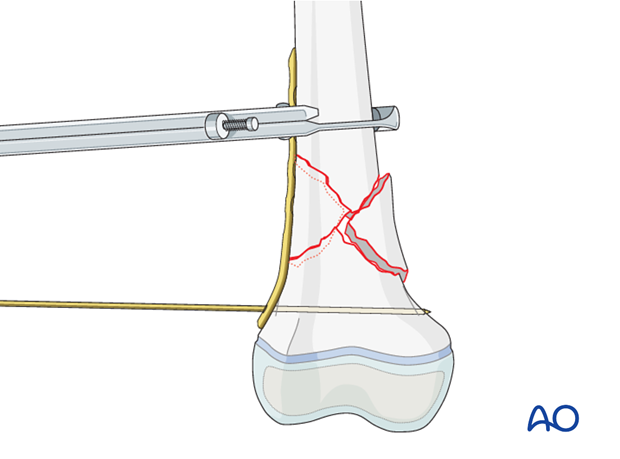
Insertion of screws
Prior to screw fixation make sure that both ends of the plate are well aligned and have good contact with the bone.
Check the femoral alignment with image intensification before screw placement.
Start with insertion of a screw on both ends of the plate, to provide initial stability, and then insert further screws.

Final construct with a straight LCP
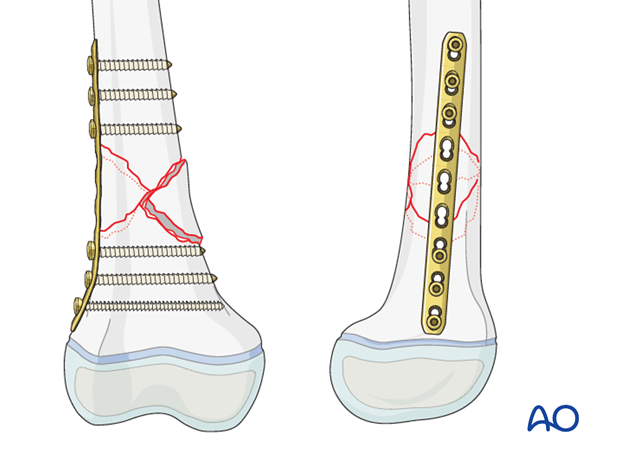
5. Final assessment
Check implant position and fracture reduction with image intensification.
Use clinical examination to check lower extremity alignment.

6. Aftercare
Immediate postoperative care
The patient should get out of bed and begin ambulation with crutches on the first postoperative day.
In most cases the postoperative protocol will be touch-weight bearing for the first 4 weeks.
Analgesia
Routine pain medication is prescribed for 3–5 days postoperatively.
Neurovascular examination
The patient should be examined frequently to exclude neurovascular compromise, particularly following displaced, high-energy fractures, when deterioration may be delayed.
Compartment syndrome, although rare, should be considered in the presence of severe swelling, increasing pain, and changes to neurovascular signs.
Discharge care
Discharge from hospital follows local practice and is usually possible after 1–3 days.
Mobilization
The patient should continue ambulation with crutches.
After ORIF, fractures are sufficiently stable for the knee to be immobilized in a removable brace and range-of-motion exercises can begin early in the postoperative phase.
For the more unstable or comminuted fractures, range-of-motion exercises will begin at a slower rate.
Follow-up
Clinical and radiological follow-up is usually undertaken 2 weeks postoperatively.
Follow-up for growth deformity
All patients with physeal fractures of the distal femur should have clinical and radiological examination 8–12 weeks postoperatively to assess for signs of physeal growth disturbance or resumption of growth.
Examination should be repeated at intervals until resumption of normal growth is documented. This can be seen as a horizontal growth line (Harris line) that is parallel to the entire physis on both AP and lateral views.
A growth line that converges towards the growth plate may be the earliest sign of growth arrest and should prompt investigation/treatment or referral as appropriate.
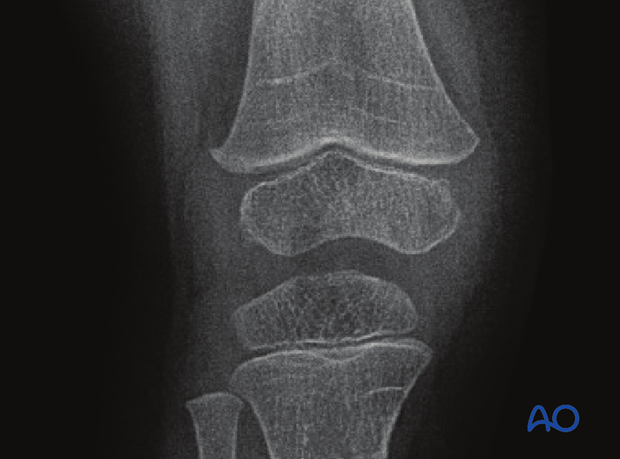
Clinical assessment of leg length and alignment is recommended at one-year.
Clinical assessment of leg length uses a tape measure from the ASIS to the medial malleolus.
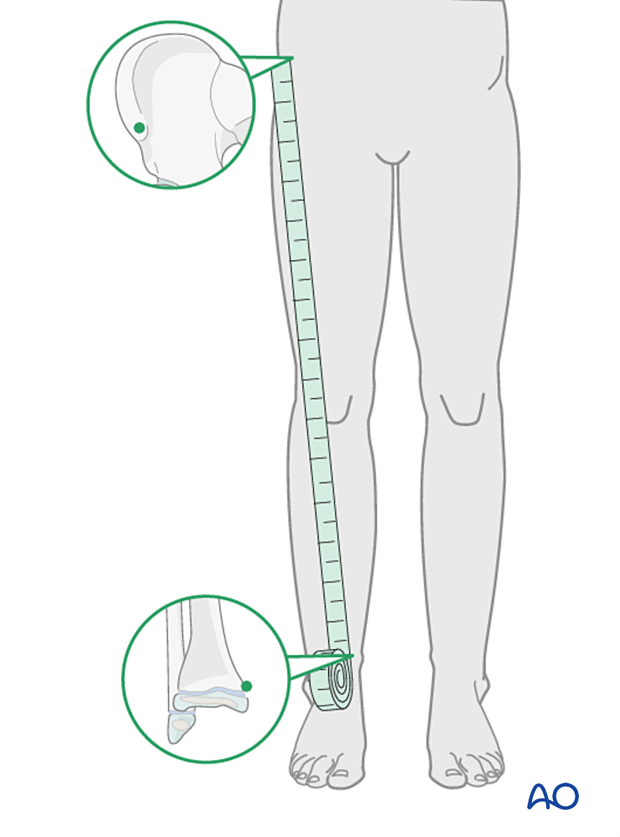
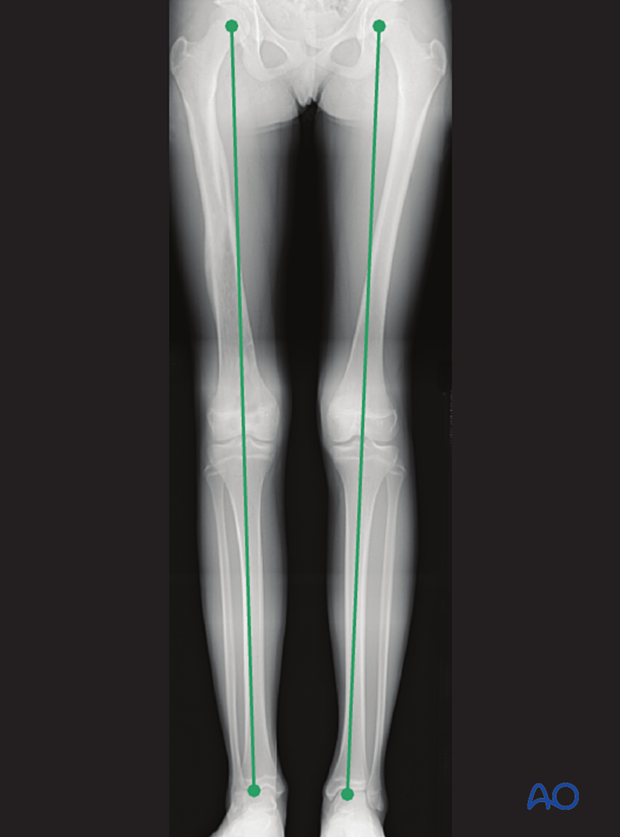
If there is any concern about leg length discrepancy or malalignment, long leg x-rays are recommended.
Leg length is measured from the femoral head to the ankle joint.
Implant removal
If symptoms develop, plate and screws can be removed once the fracture is completely healed, usually 6–12 months postoperatively.
If K-wires are used, they are typically removed after 4–6 weeks.













