Nonoperative treatment
1. No immobilization and early motion
Indications
Consideration for nonoperative treatment would require articular displacement less than 2–5 mm, widening less than 5 mm, and valgus instability of less than 10° when examined, particularly in full extension.
However, even in situations where these criteria are satisfied, operative treatment may still be chosen in the setting of neurovascular injury, compartment syndrome, a multiply injured patient, associated injuries of the limb, etc.
If there is any question about medial/lateral instability, anterior/posterior stability, or rotatory instability, then further investigations such as MRI can be obtained.
Patient discomfort may preclude an accurate initial examination and may require a repeated examination, or adequate anesthesia.
2. Posterior plaster splint
Indications
This is only indicated as a means of temporary splinting in austere environments, or when prefabricated braces or immobilizers are unavailable.
3. Knee immobilizer and hinged fracture brace
Indications
These devices provide relative immobilization of the knee joint, allowing pain relief. Regardless of the device used, patients must be instructed to begin knee range of motion exercises as pain subsides, typically beginning within one to two weeks. During this time, ankle range of motion is to be encouraged, as are quadriceps setting exercises, and straight leg raising. These devices can be used for all fractures as a means of temporary splinting.
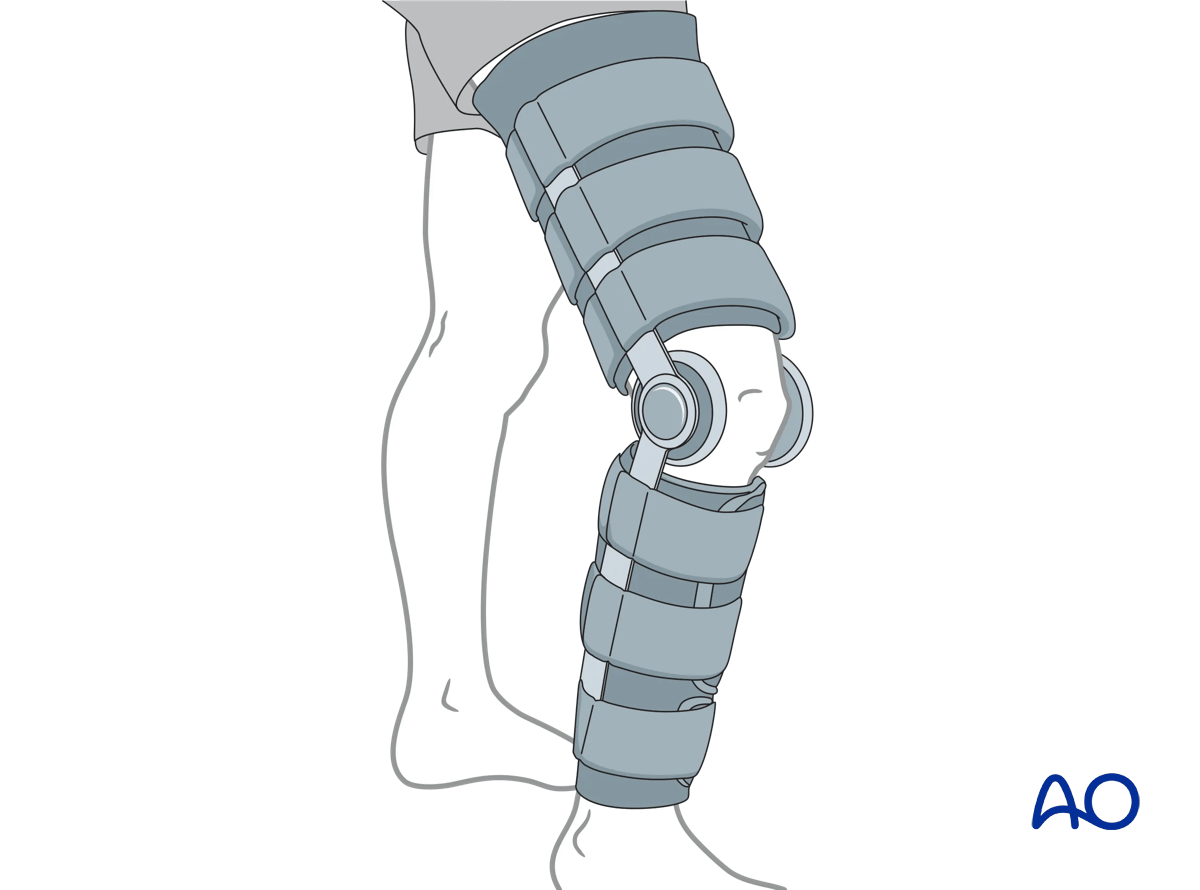
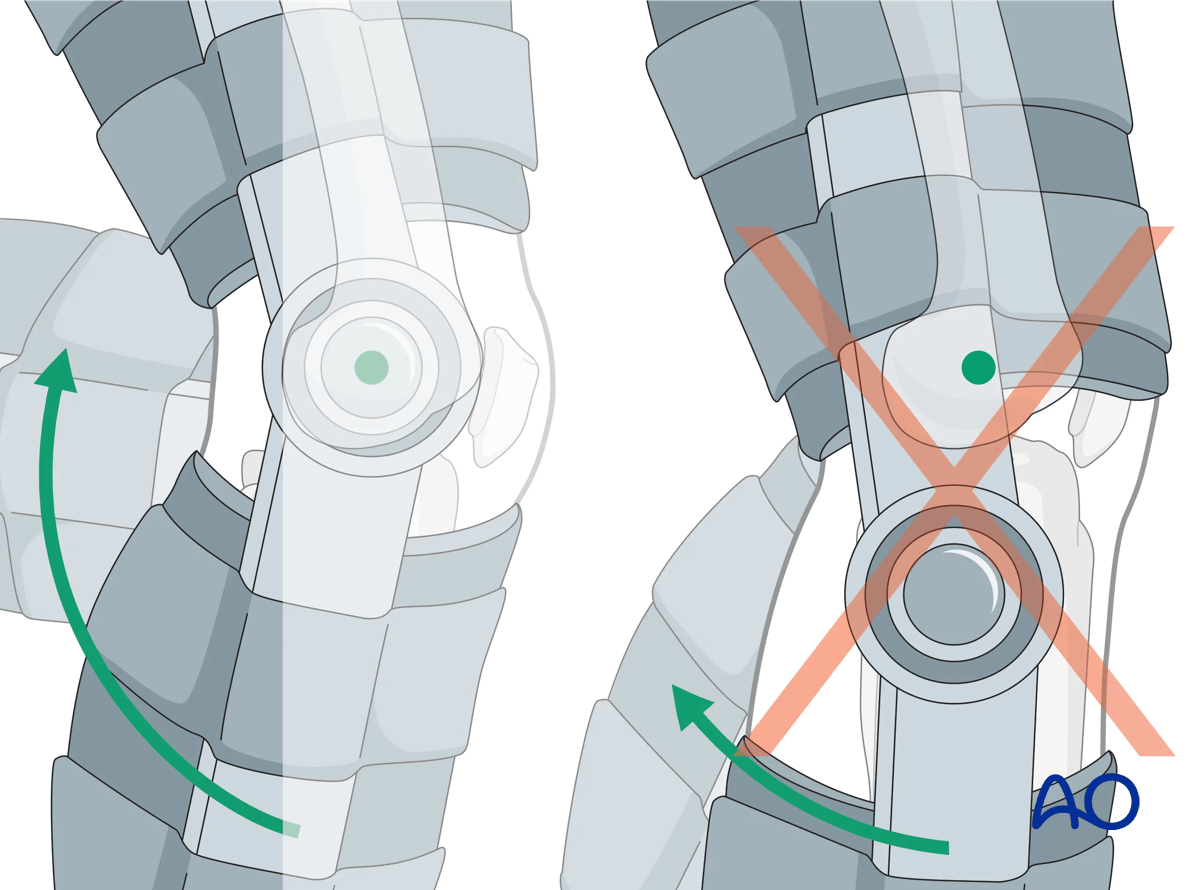
4. Aftercare
Patients should take off the immobilizer, or knee brace, for hygiene, quiet time, and range of motion.
DVT prophylaxis should be considered and addressed in both nonoperatively and operatively managed patients.
Aftercare and rehabilitation following nonoperative treatment should be individualized according to the patient, fracture, and local protocol specifics.
Pain and neurovascular status should continue to be monitored, particularly in the immediate post-injury time period. Active motion of the joint should begin within 7–14 days. Full weight bearing is often restricted for 6–8 weeks.
Early weekly radiographic follow-up is indicated to ensure there is no change in alignment, particularly with medial-sided fractures.