Screw fixation with bone graft of central impaction fracture
1. Principles
Mechanism of the injury
Digital hyperextension injuries are commonly caused by sporting accidents.
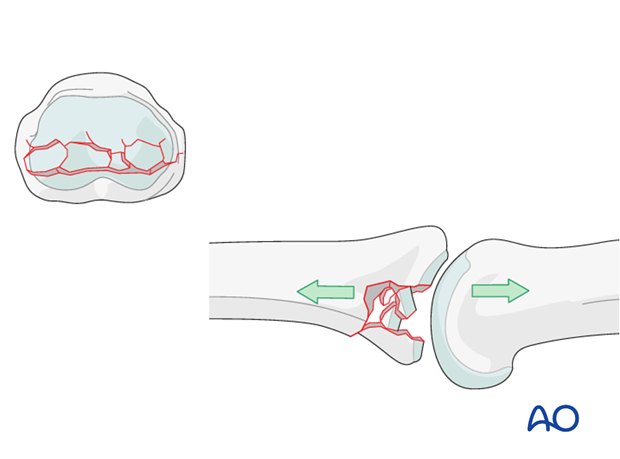
Typically, hyperextension of the proximal interphalangeal (PIP) joint causes an avulsion fracture of the volar plate. If there is significant axial load on the middle phalanx, the compression forces across the PIP joint lead to an impaction fracture in association with a palmar avulsion fracture.
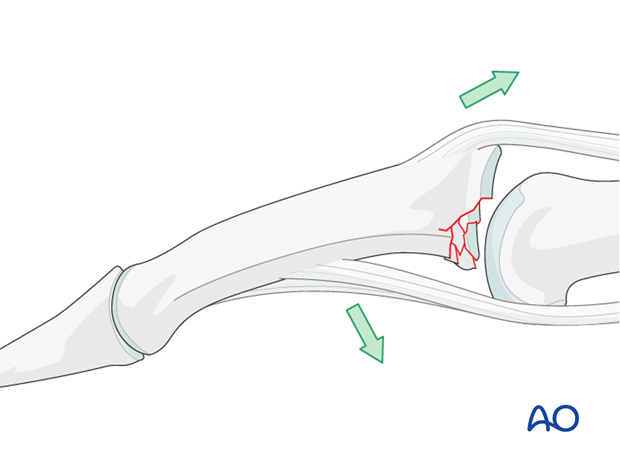
Deforming forces
In the presence of palmar instability of the PIP joint, muscle forces (flexor digitorum superficialis and the central extensor slip) lead to palmar tilting and dorsal subluxation, depending on the degree of the impaction.
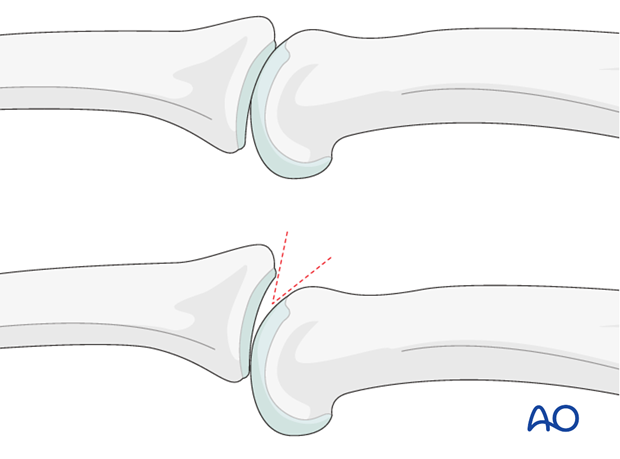
Recognizing subluxation
Diagnosis is based on
- the clinical history and mechanism of injury
- the clinical examination of the patient
- the x-rays
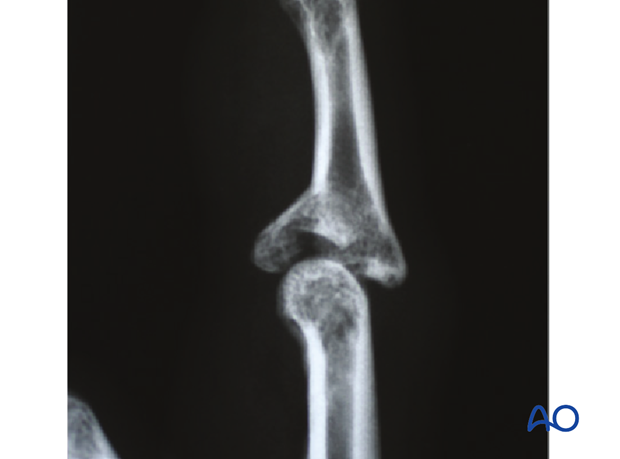
AP and true lateral x-rays are necessary for diagnosis. Be careful to avoid overlap of other fingers in the x-rays.
An AP view will help to detect impaction fractures.
Often, a subluxation is not easily recognized in the lateral view. Look for the characteristic “V” sign of diverging joint surfaces, which indicates this injury.
Check for impaction injuries
Impaction is possible both in the sagittal and the coronal planes. Check both true AP and lateral views.
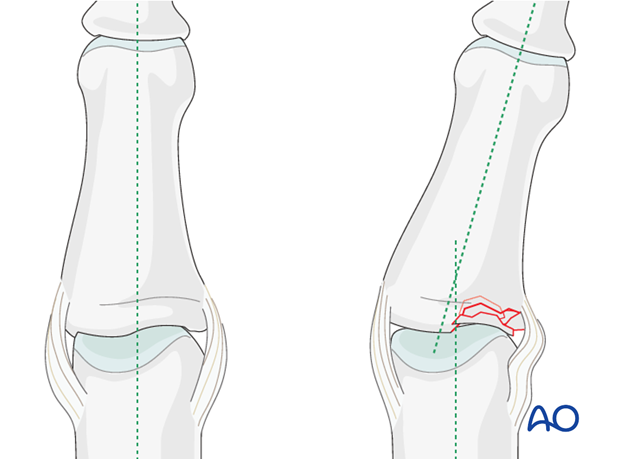
Malalignment in the coronal plane may be a sign of impaction.
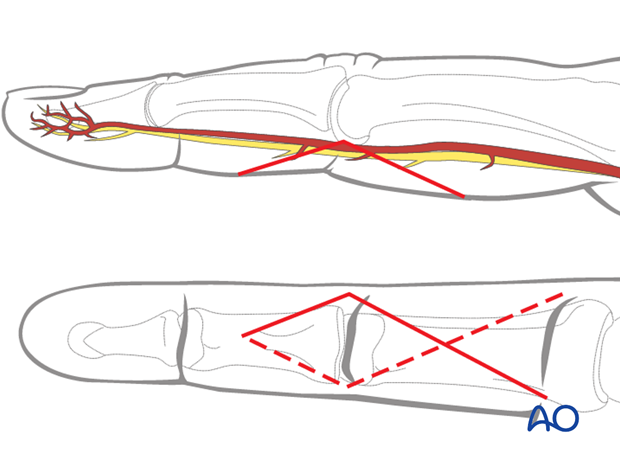
2. Approach
For this procedure a palmar approach to the PIP joint is normally used.
3. Reduction
Reduce the depressed articular fragments
Use a K-wire, a dental pick, or a small curette to push the depressed fragments towards the head of the proximal phalanx, which should be used as a template to ensure congruity of the articular surface of the middle phalanx to reduce the risk of later degenerative joint disease.
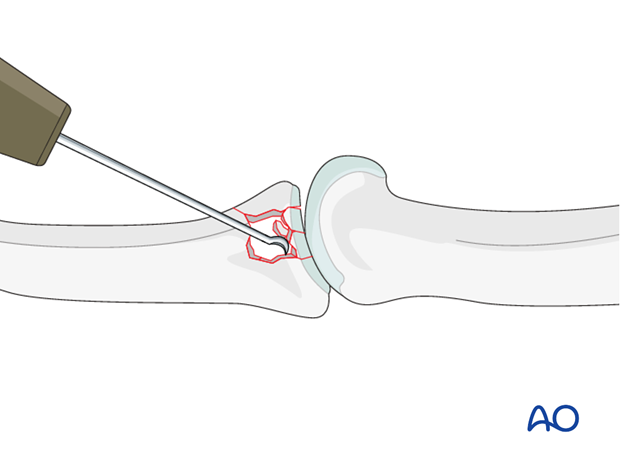
Since the subchondral cancellous bone is impacted, a void may remain following reduction of these articular fragments.
This jeopardizes fracture healing:
- This is a very unstable situation in which the fragments may collapse
- The healing process is very slow
Therefore bone grafting is recommended.

4. Bone graft
Harvest site
Harvest the graft material from the distal radius. A good and safe place is proximal and slightly radial to Lister’s tubercle.
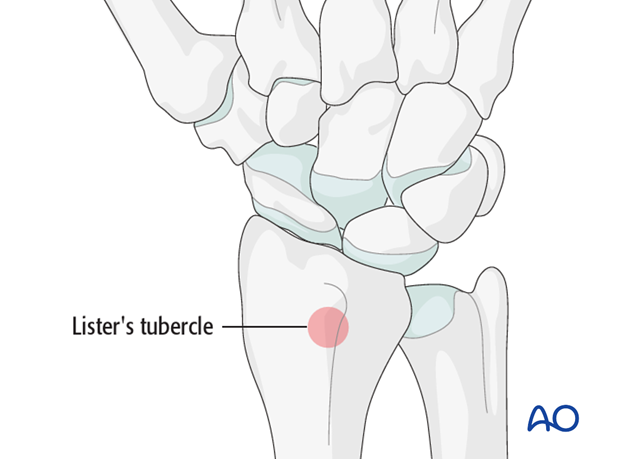
Harvesting
Make a 2 cm longitudinal incision proximal to Lister’s tubercle. Retract the tendons of the second compartment radially, and the extensor pollicis longus (EPL) in an ulnar direction.
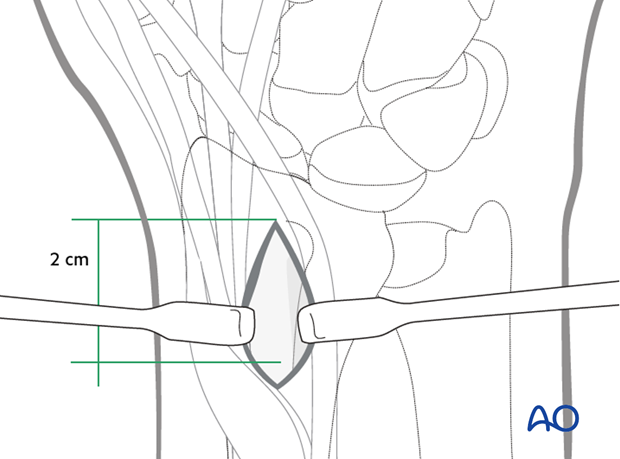
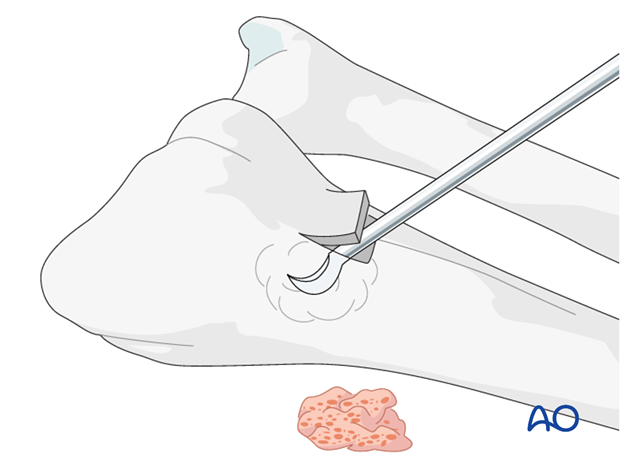
Use a chisel to cut three sides of a small square. Lift the dorsal radial cortex as a flap. After harvesting cancellous bone, replace the “lid”, and suture the periosteum and the skin incision.
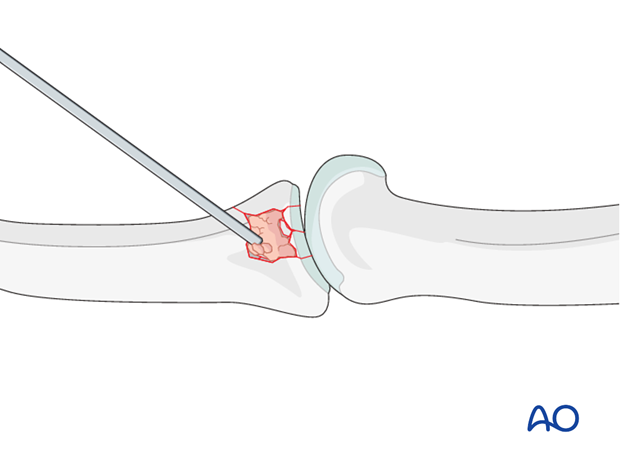
Use a pusher instrument to impact the bone graft and fill the whole fracture cavity.
Confirm reduction using image intensification.
5. Fixation
Drilling
Maintaining the reduction with slight pressure from a drill guide, drill a threaded hole using the corresponding drill.
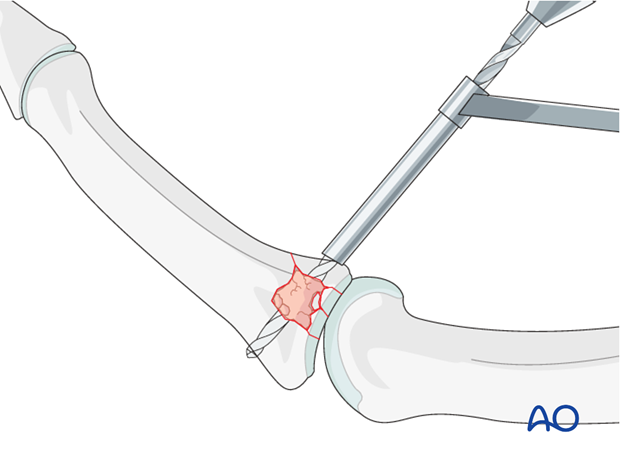
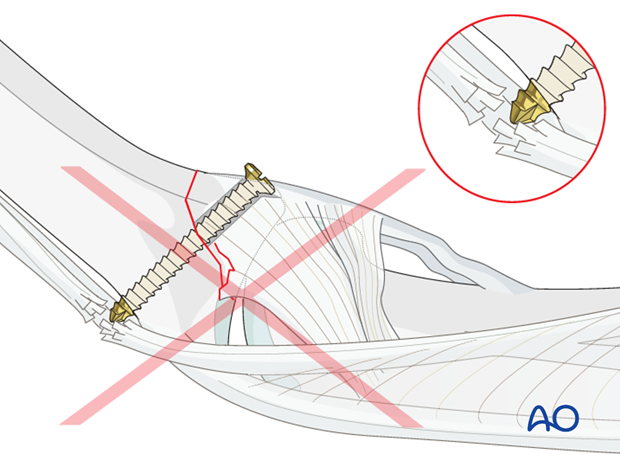
Pitfall: Too long a screw irritates extensor tendon
If too long a screw is chosen, the protruding end may damage the extensor tendon.
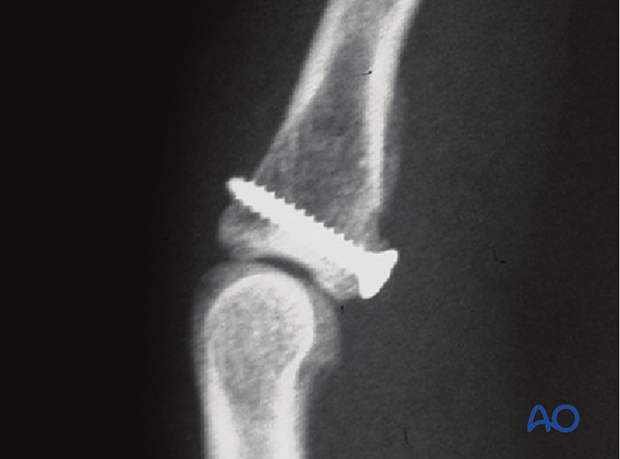
Screw insertion
Insert the screw and carefully tighten it just enough to hold the reduction. The screw should just penetrate the opposite cortex.
Check joint congruity using image intensification. Reduction must be anatomical.
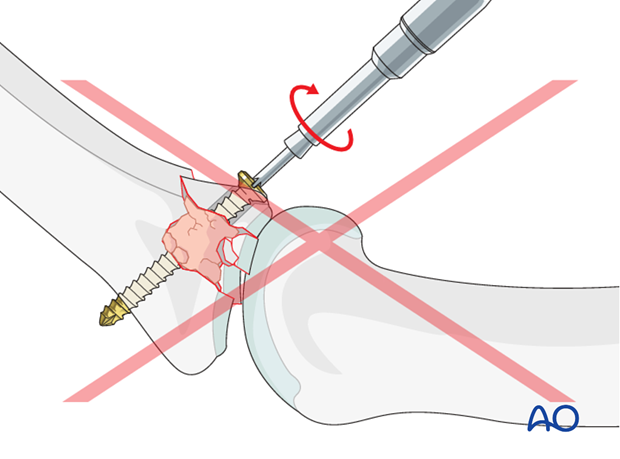
Pitfalls:
Using a lag screw
Using a lag screw would lead to collapse of the bone graft and redisplacement the articular fragments.
Overtightening the screw
Be careful not to overtighten the screw as this may result in comminution of the palmar marginal fragment.
6. Aftertreatment
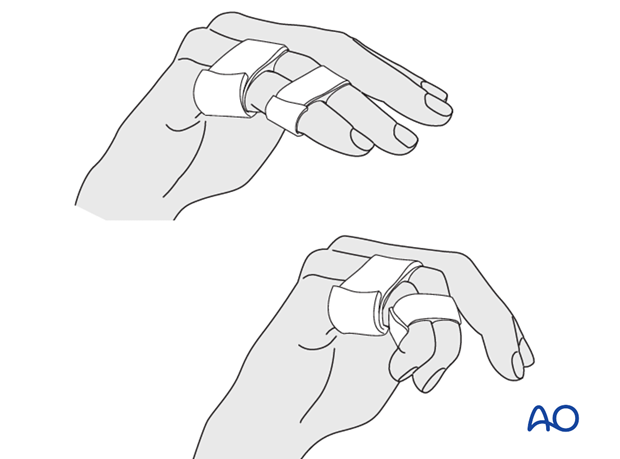
Postoperatively, protect the digit with buddy strapping to the adjacent digit to neutralize lateral forces on the finger.
A dorsal thermoplastic night splint, with the PIP joint in full extension, is used to avoid flexion contraction.
Follow up
Review the patient 5 days and 10 days after surgery.
Functional exercises
The patient can begin active motion (flexion and extension) immediately after surgery.
Heavy manual load, whether domestic, occupational, or sporting, should be avoided for 3 months following operation.
Implant removal
Rarely, the implants may need to be removed in cases of soft-tissue irritation.
In case of joint stiffness, or tendon adhesion’s restricting finger movement, tenolysis, or arthrolysis become necessary. In these circumstances, take the opportunity to remove the implants.