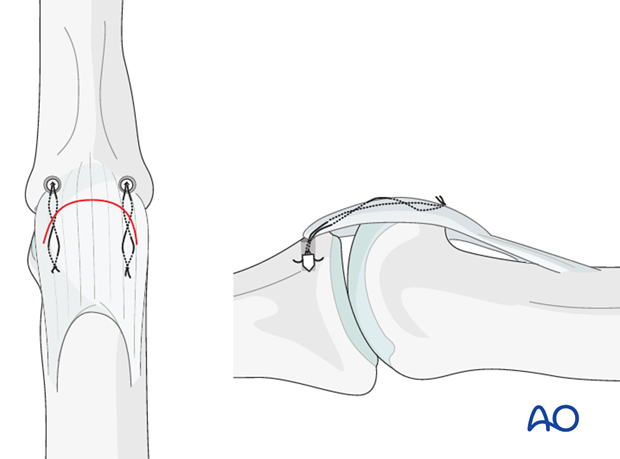
Palmar approach to the PIP joint
1. Indications
The palmar approach is indicated mainly for volar plate avulsion fractures of the base of the middle phalanx, for fracture dislocations of the proximal interphalangeal (PIP) joint, or for comminuted, impacted fractures of the base of the middle phalanx.
An exception to this rule is a dorsal central slip avulsion fracture of the base of the middle phalanx, with palmar dislocation, that can not be approached via a palmar exposure, and the dorsal route becomes the first choice.
The palmar approach is also indicated for volar plate arthroplasty.
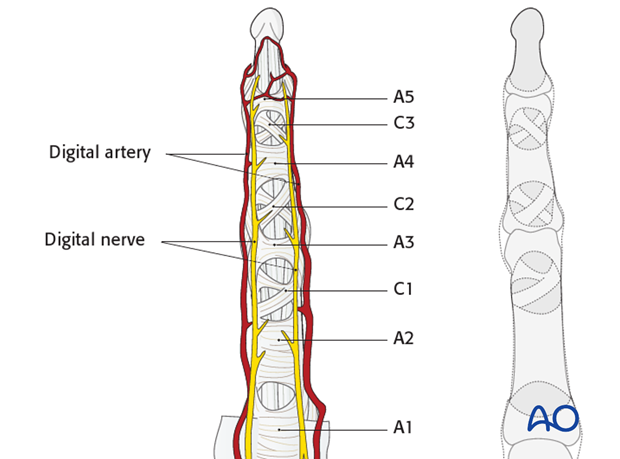
2. Surgical anatomy
When approaching the PIP joint, take care to preserve the digital arteries and nerve.
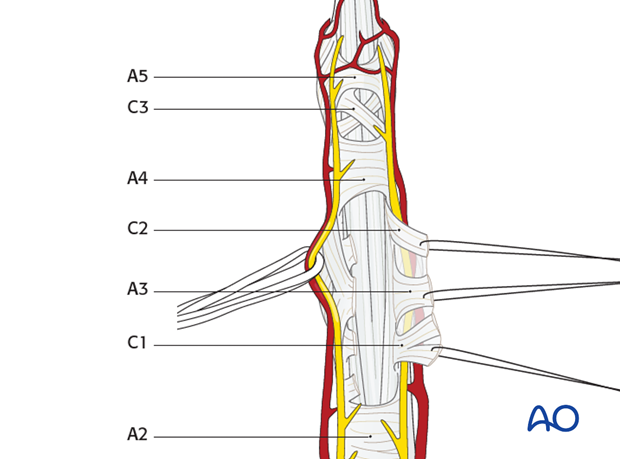
The flexor tendon pulleys are either transverse (A) or cruciform (C). They are numbered sequentially from proximal to distal, as illustrated.
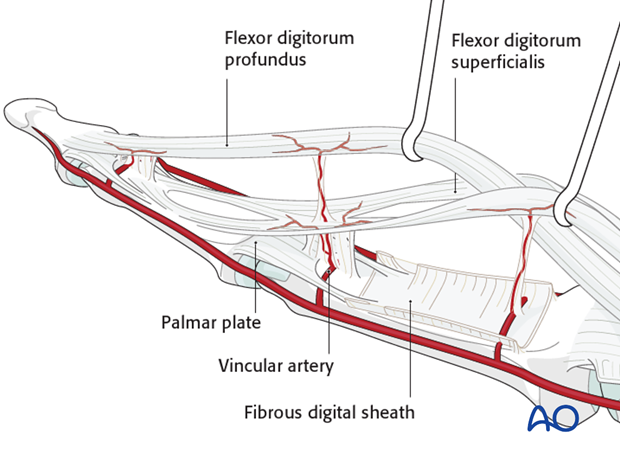
3. Vincular arteries
The vincular arteries are delicate, but essential to the vascularity of the flexor tendons. They must be preserved whenever possible, lest the vascularity of the tendon be compromised.
4. Skin incision
Make a carefully planned palmar, angled skin incision (Bruner zigzag), using the flexor skin creases as a guide, as illustrated.
The apex of the angle should be at the end of the intermediate flexor crease, level with the PIP joint.
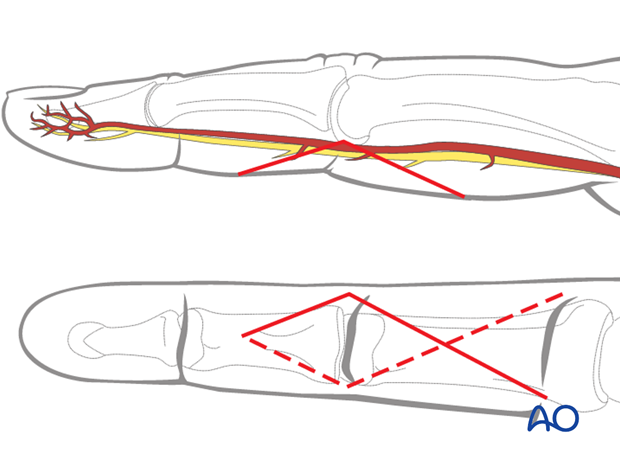
5. Elevate the flap
The angled skin flap is elevated by blunt dissection in the thin subcutaneous tissue, and the apex retracted using a fine stitch. Identify and gently mobilize the digital arteries and nerves.
The flexor sheath with the C1, C2, and A3 pulleys are now visible.
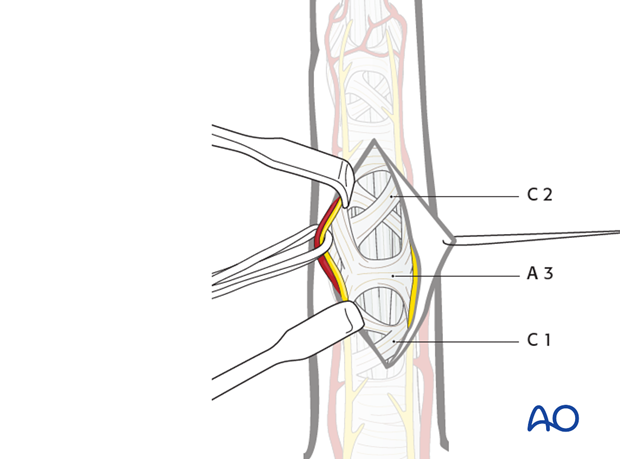
Division of the pulleys
Incise the C1, A3, and C2 pulleys laterally, near their bony attachments, leaving enough (at least 2 mm) for later reattachment, and elevate them with sutures.
Do not cut the A2 or A4 pulleys, as these are essential for the biomechanics of active flexion of the finger.
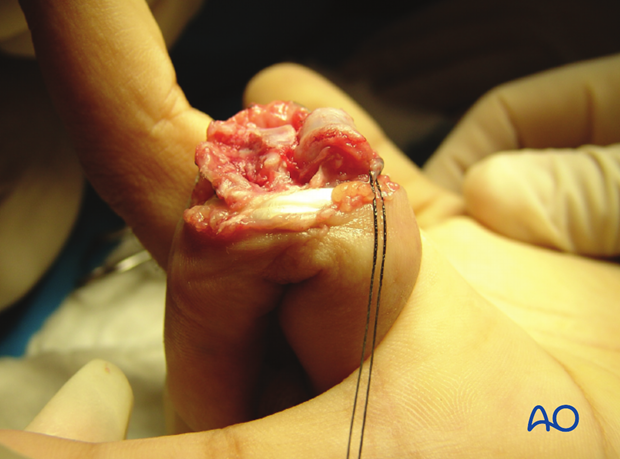
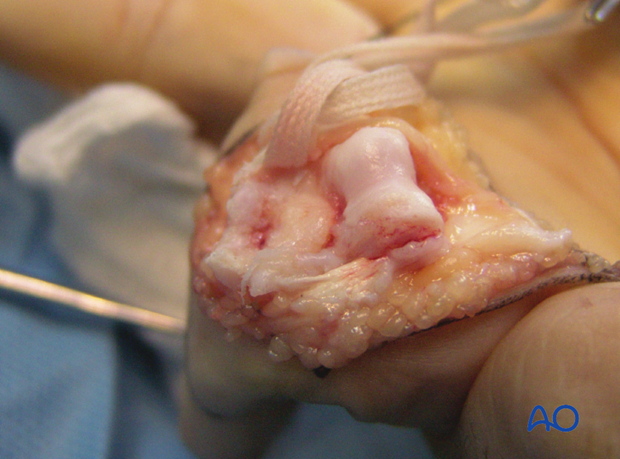
This clinical photo gives a good view of the flexor tendons after the pulleys have been divided.
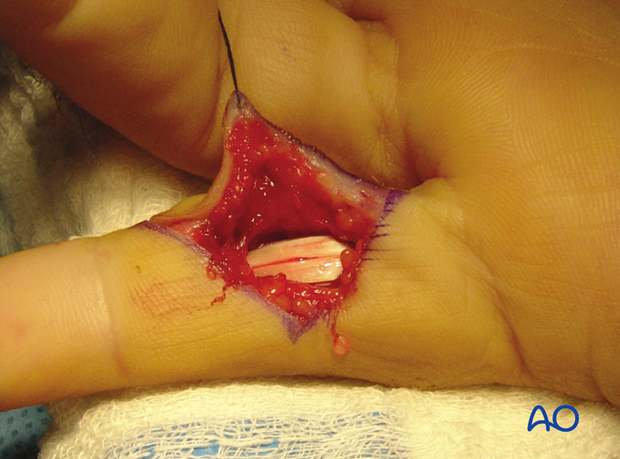
6. Exposure of the palmar capsule
Retract the flexor tendons, using a latex loop (such as a Penrose drain).
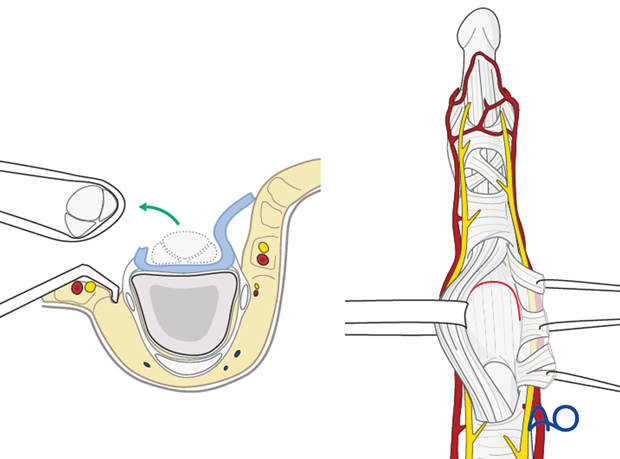
The palmar capsule is now visible.
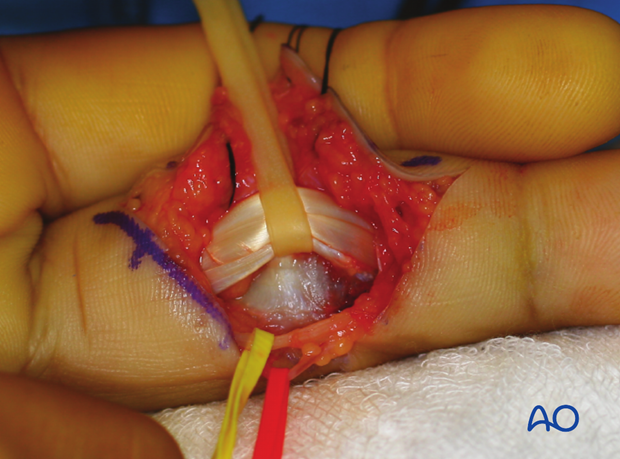
7. Exposure of the volar plate
Extension of the PIP joint now exposes the distal edge of the volar plate, which often bears a fracture fragment. The fracture fragment can be elevated together with the volar plate and retracted proximally.
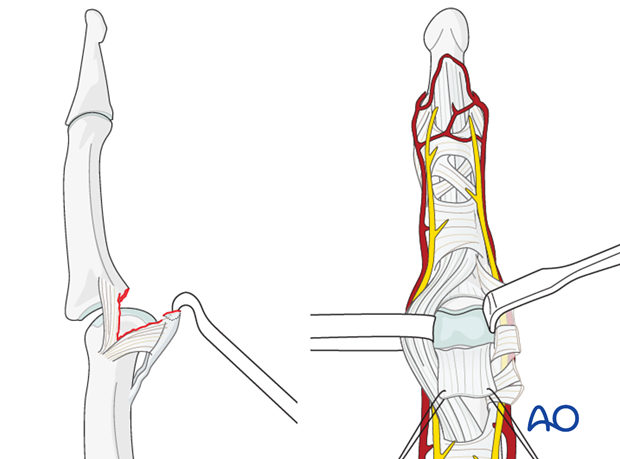
In the event that the volar plate is attached to small palmar fragments not suitable for fixation, and a volar plate arthroplasty is indicated, detach the volar plate distally using a transverse incision.
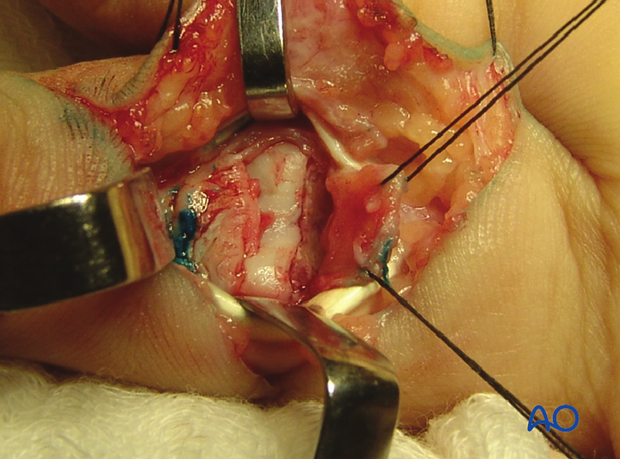
8. Indications for ‘shotgun’ hyperextension exposure
If there is comminution, or impaction of fragments, at the base of the middle phalanx that need to be reduced, both collateral ligaments need to be divided.
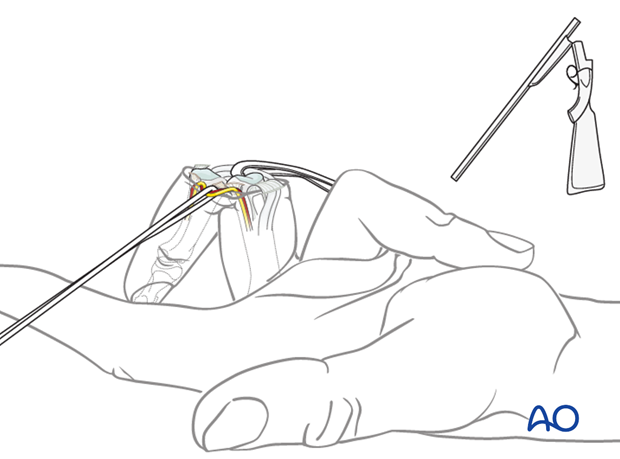
This will enable full opening of the PIP joint by hyperextension (Eaton), thereby exposing fully the base of the middle phalanx.
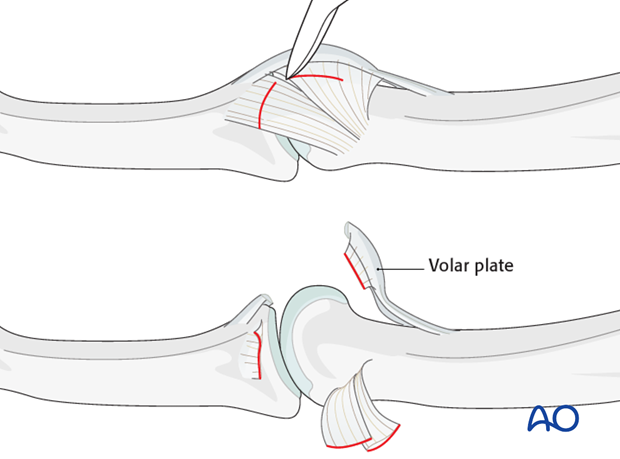
9. Detach the ligaments
The distal and palmar attachments of the collateral ligaments should be detached bilaterally, and retracted dorsally.
10. Hyperextend the finger
After detachment of the collateral ligaments, the finger can be fully hyperextended (as in breaking open a shotgun).
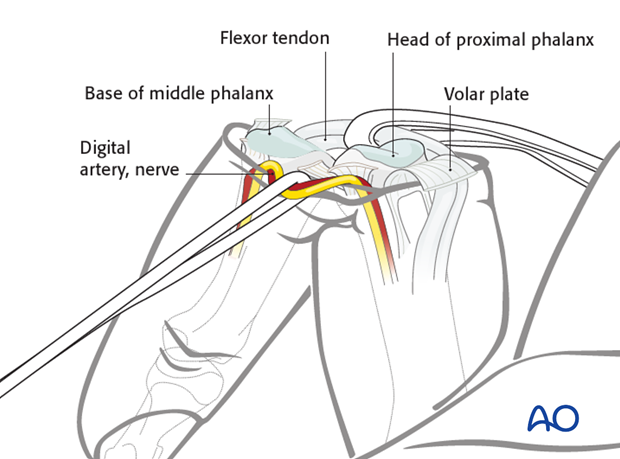
This will give a complete view of the whole joint surface of the middle phalanx and both condyles of the proximal phalanx.
11. Wound closure
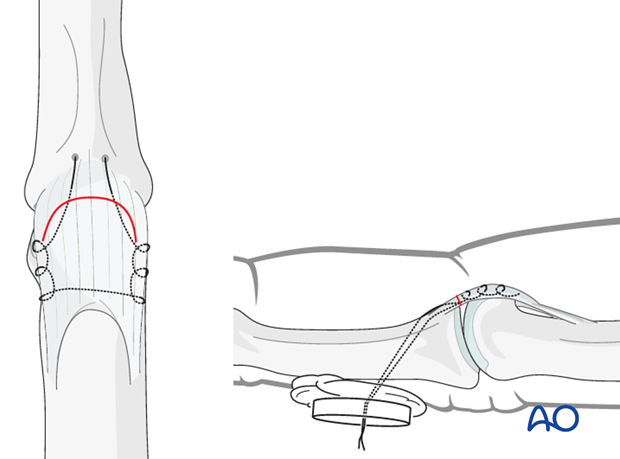
Volar plate
Reattach the volar plate and any small attached fracture fragment, using either a pullout suture, or at least two anchor sutures.
Pulleys
It is mandatory to repair the A3 pulley. If possible, also reattach the C1 and C2 pulleys.