Joint reconstruction with bone graft
1. Principles
Classification of avulsion fractures of the volar plate
Avulsion fractures of the volar plate are very common injuries, often resulting from sporting injuries and usually involving the middle and ring fingers. Several classification systems for them have been proposed. The Eaton classification is very useful for practical purposes. This classification is based on the premise that successful treatment must be based on the stability of the fracture, which in turn depends on:
- size of the fragment
- degree of impaction
- presence of one or both collateral ligament ruptures
- direction of the dislocation (hyperextension, lateral dislocation, flexion).
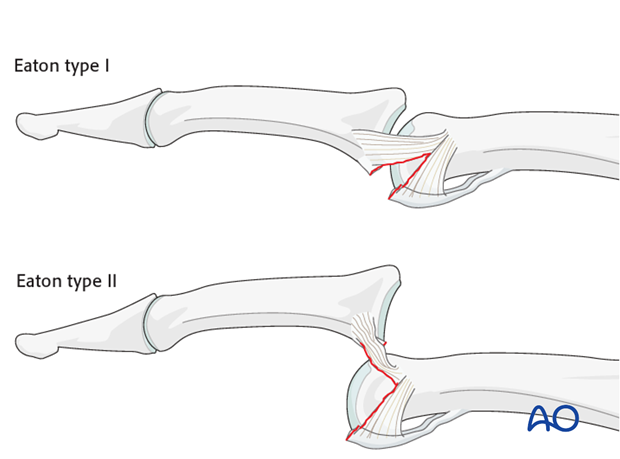
Eaton type I (hyperextension)
These are hyperextension injuries, with an avulsion of the volar plate and a longitudinal split in the collateral ligaments.
Eaton type II (dorsal dislocation)
Complete dorsal dislocation of the PIP joint and avulsion of the volar plate. The base of the middle phalanx rests dorsally on the condyles of the proximal phalanx, with no contact between the articular surfaces.
Eaton type III (fracture dislocation)
A fracture dislocation with a small fragment measuring less than 40% of the volar arc will remain stable when reduced.
If a larger part (>40%) of the volar articular segment is involved, ligamentous support will not suffice for a stable reduction.
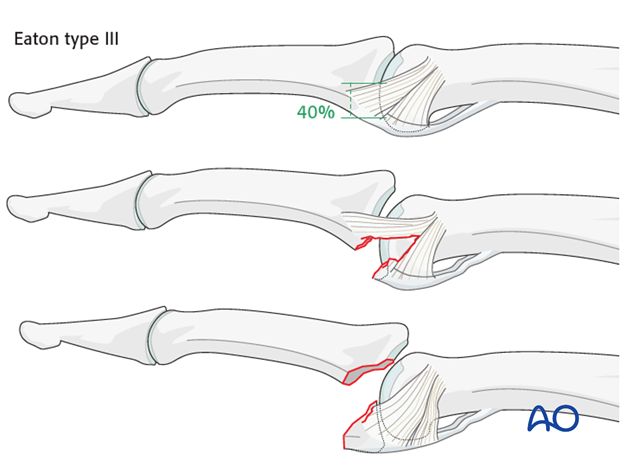
Stability of fracture dislocations (Eaton type III)
Stability of the reduction depends on the size of the avulsed fragment and the amount of ligament remaining attached to the middle phalanx.
If less than 40% of the articular segment is avulsed, the fracture is displaced dorsally, with the dorsal portion of the collateral ligament remaining attached to the middle phalanx. This helps to keep the reduction stable.
However, if more than 40% of the articular segment has avulsed, only very little or no ligament will remain attached to the base of the middle phalanx, rendering the reduction unstable.
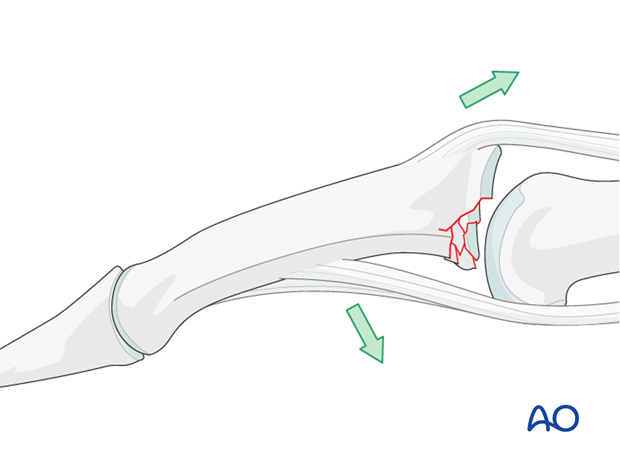
Mechanism of the injury
These injuries are commonly caused by sporting accidents.
Typically, hyperextension of the finger causes an avulsion fracture of the volar plate.
Often, in addition to hyperextension, pressure is applied to the fingertips, causing longitudinal compression forces on the middle phalanx towards the proximal phalanx and leading to an additional impaction fracture.

Deforming forces
The flexor digitorum superficialis (FDS) exerts a palmar pull on the middle phalanx around a pivotal point determined by the junction of intact cartilage and the fracture, which leads to subluxation and dorsal tilting, depending on the degree of the impaction.
Recognizing subluxation
Diagnosis is based on:
- the clinical history of the trauma and mechanism of the injury
- the clinical examination of the patient
- the x-rays
AP and lateral x-rays are necessary for diagnosis. Be careful to avoid interposition of other fingers in the x-rays.
An AP view will help to recognize impaction fractures.
Often, a subluxation is not apparent on the lateral view. Look for the characteristic “V” sign of diverging joint surfaces, which indicates this injury.
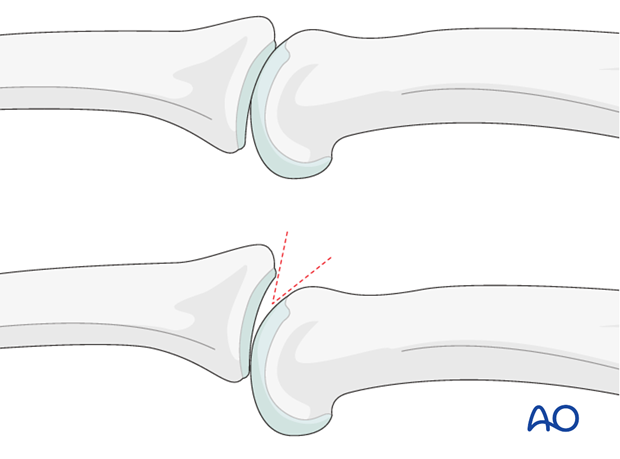
In the lateral view, the proximal and middle phalanges should be collinear. Any axial malalignment is a clear indication of subluxation.
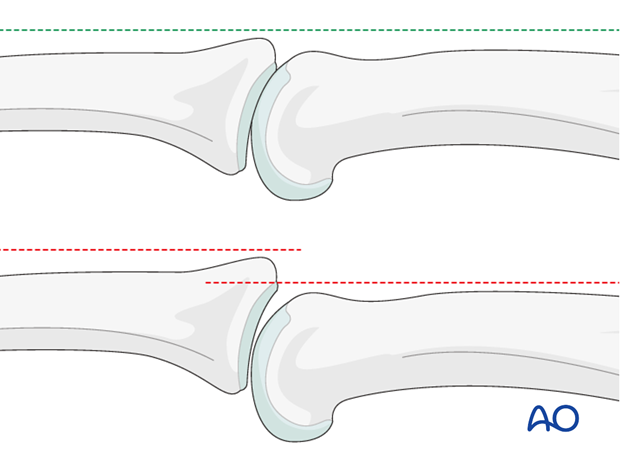
2. Indications
Check for impaction injuries
Impaction is possible either in the sagittal or the coronal plane. Check for both under true AP and lateral views.
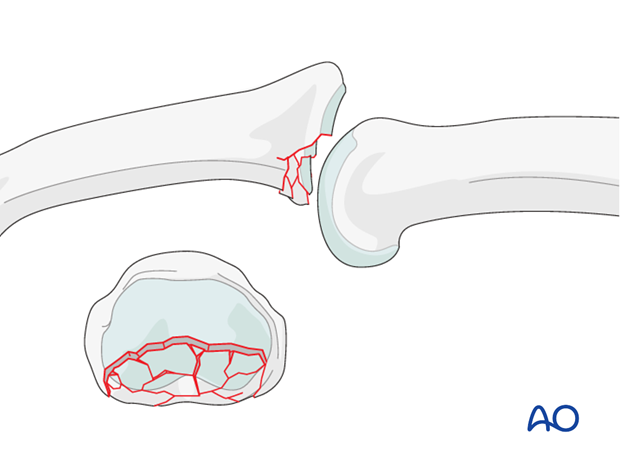
Impaction can occur in several areas, either involving the volar ring, up to 50% of the palmar joint aspect, or the central section of the joint. The latter injury is the ideal indication for the following procedure.
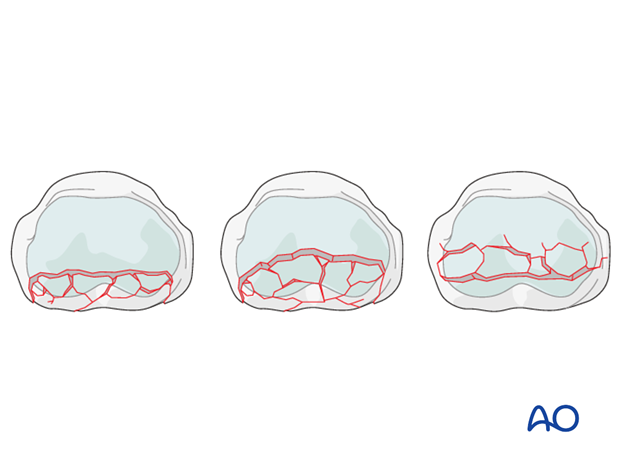
Extensive comminution and impaction - bone graft reconstruction
Extensive comminution with impaction of the subchondral metaphysis is a typical indication for bone graft reconstruction.
If more than 60% of the articular cartilage is comminuted and impacted, bone graft reconstruction of the articular surface remains the only therapeutic option.
3. Joint visualization
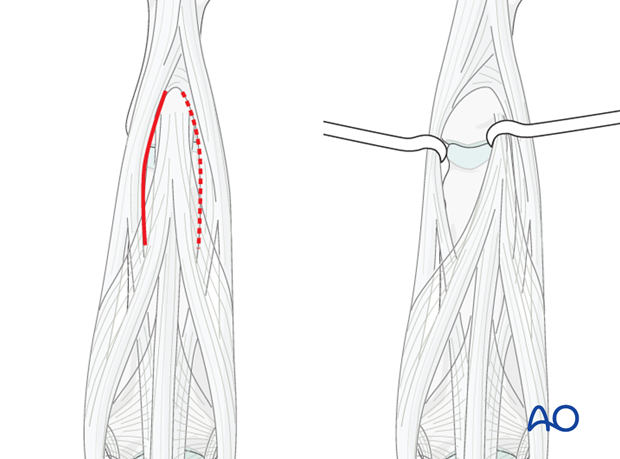
Visualize the joint
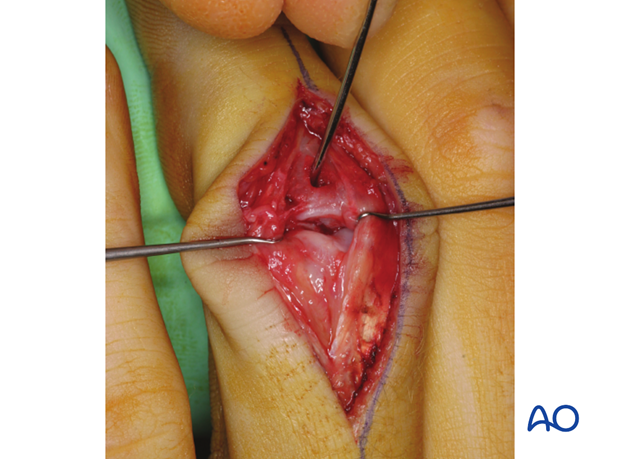
Often, a palmar approach, with shotgun extension, is used for these fractures. However, since that approach requires considerable additional dissection and trauma to the soft tissues, with consequent inflammatory reaction and fibrosis, a dorsal approach may be more biological. We recommend an incision between the lateral band and the central slip. Take special care to protect the insertion of the central slip, otherwise, a boutonnière deformity can develop.
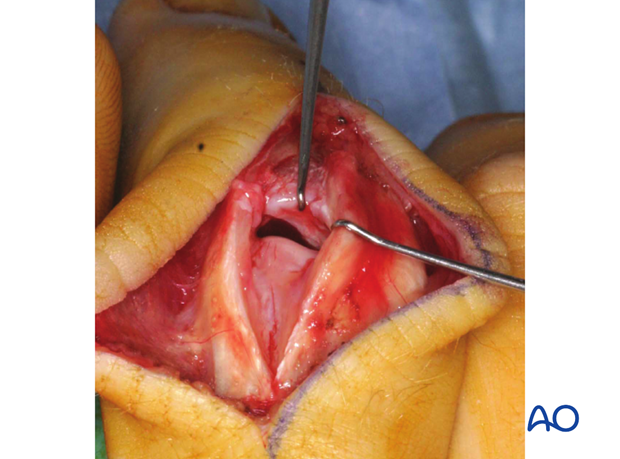
In order to gain a better view of the fracture, use a syringe to clear out blood clot with a jet of Ringer lactate.
Often the degree of comminution is not apparent from the x-rays, and can only be determined under direct vision.
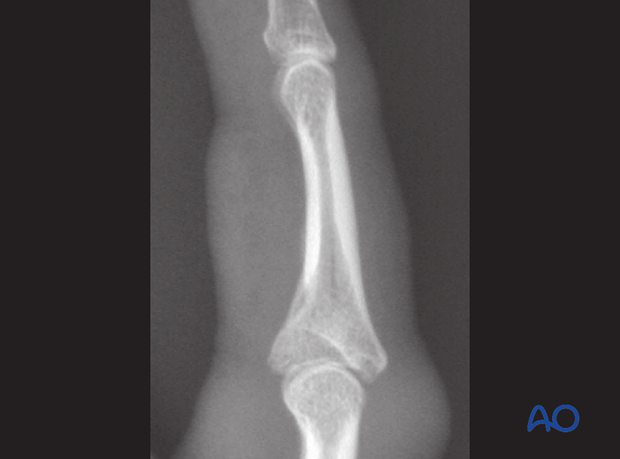
Evaluate the fracture
The image shows a fracture with a large area of the palmar articular surface comminuted and impacted. The only remaining articular cartilage is on the dorsal aspect. Bone grafting and reconstruction is the recommended option.
4. Reduce depressed fragments
Create access window
A window will aid with the reduction of the articular fragments. This window should be located in the basal metaphysis of the middle phalanx, well away from the joint surface, in the interval between the central slip insertion and the collateral ligament. Make sure that it is distal enough not to interfere with later screw placement.
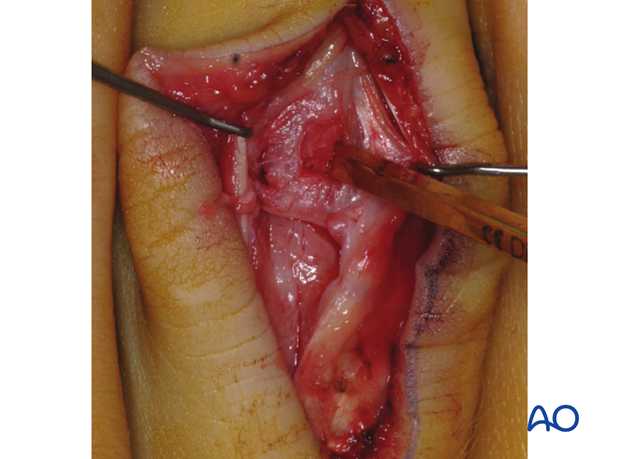
Use a small osteotome to cut a rectangular window into the cortical bone.
Remove the osteotomized bone and carefully preserve it for later replacement.
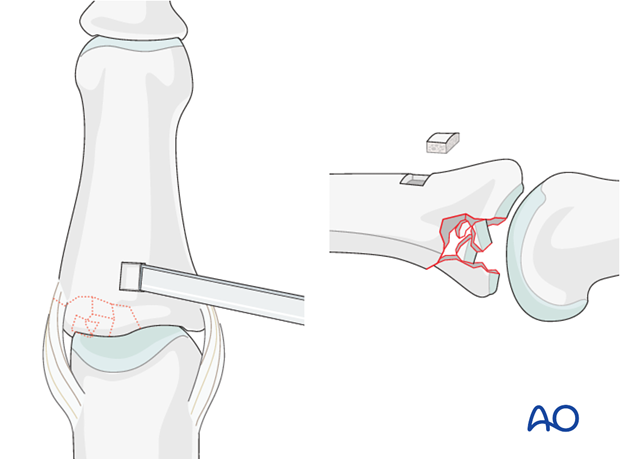
Reduction principles
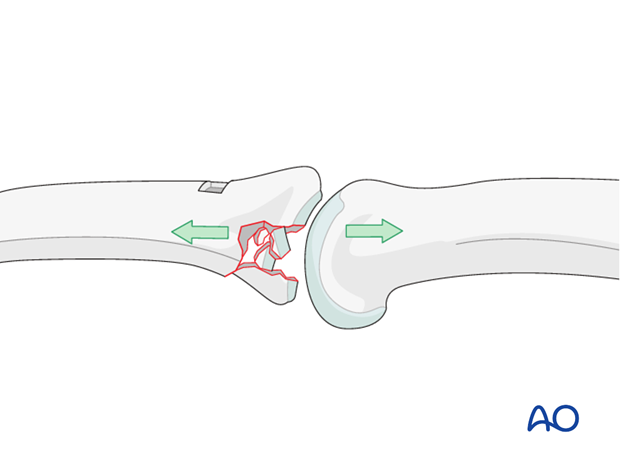
Compression fractures are not reducible by ligamentotaxis, as the centrally impacted fragments are devoid of soft-tissue attachments.
Direct reduction is thus necessary.
The key to fixing compression fractures is restoring the joint surface to as close to normal as possible (anatomically), and supporting the reduction with bone graft.
Reduce the depressed articular fragments
Use a stout hypodermic needle, a dental pick, or a small curette, introduced through the cortical window, to push the depressed fragments towards the head of the proximal phalanx, which is used as a template to ensure congruity of the reduced articular surface.
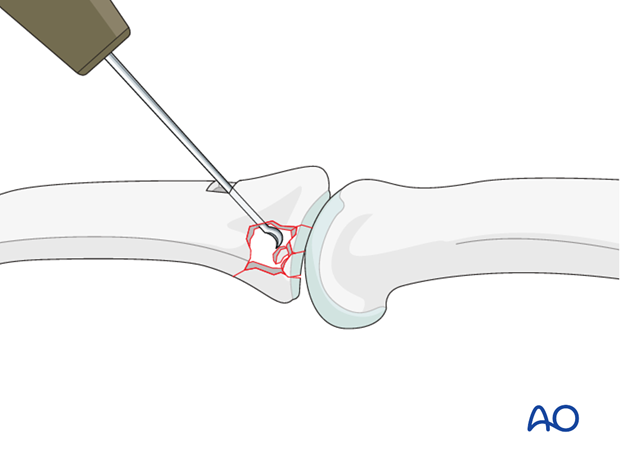
If a cartilage step-off > 1 mm remains, degenerative joint disease may follow.
Since the subchondral cancellous bone is impacted, a void will be created by the reduction.
This jeopardizes the fracture in two ways:
this is a very unstable situation in which the fragments may easily redisplace (collapse)
the healing process is very slow.
5. Bone graft
Harvest site
Cancellous autograft will be necessary to support the articular fragments and fill the impaction void. The graft will also accelerate the healing process.
Harvest the graft material from the distal radius. A good and safe place is proximal and slightly radial to Lister’s tubercle.
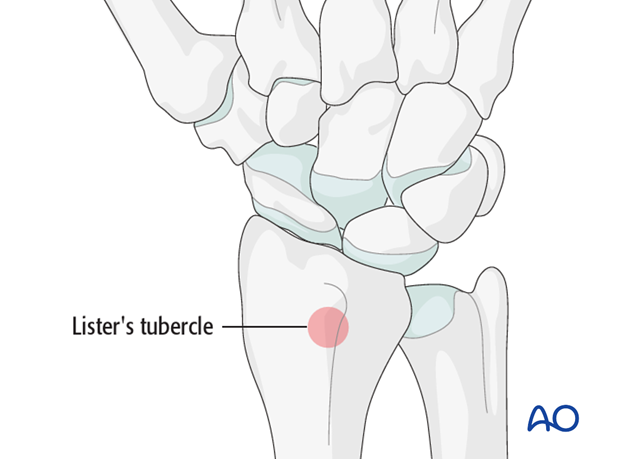
Harvesting
Make a 2 cm longitudinal incision proximal to Lister’s tubercle. Retract the tendons of the second compartment radially, and the extensor pollicis longus (EPL) in an ulnar direction.
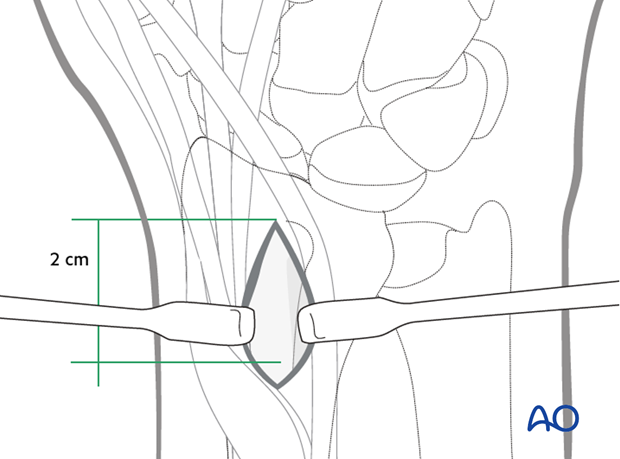
Use a chisel to cut three sides of a small square. Lift the dorsal radial cortex as a flap. After harvesting cancellous bone, replace the “lid”, and suture the periosteum and the skin incision.
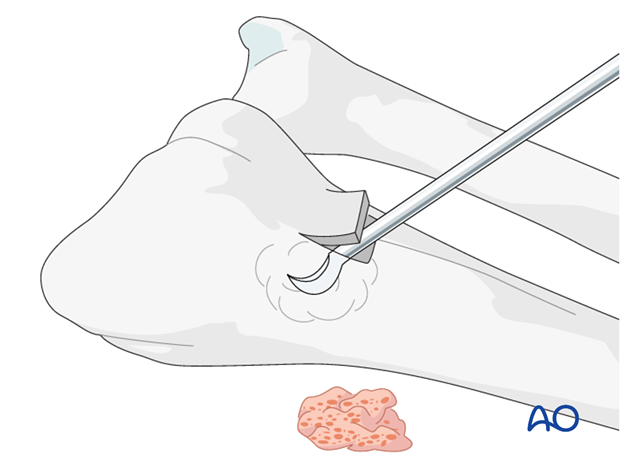
Use a pusher instrument to impact the bone graft and fill the whole fracture cavity.
Confirm reduction using image intensification.
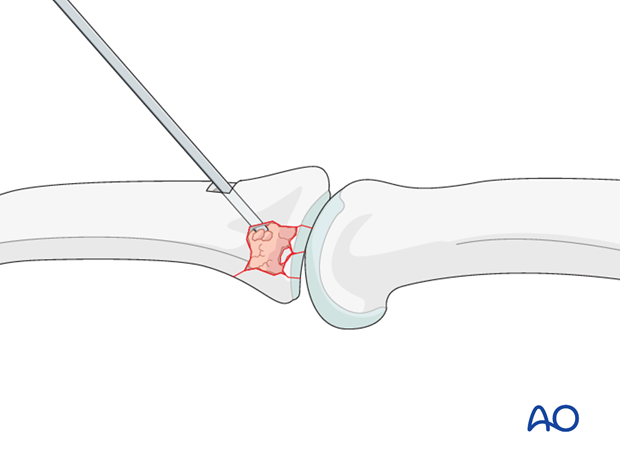
6. Screw fixation
Close access window
Replace the osteotomized piece of bone into the access window.
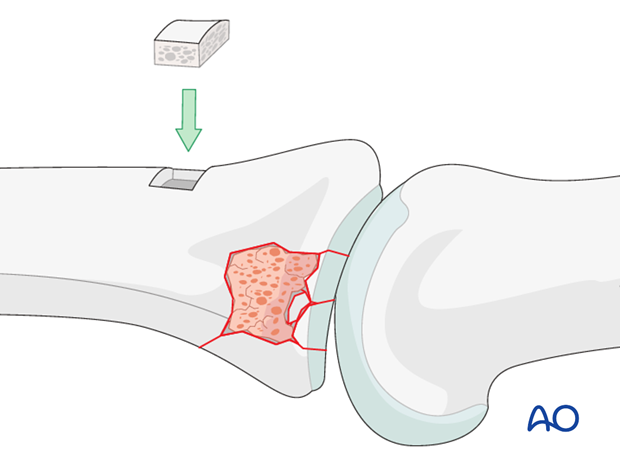
Screw planning
Depending on the quality of the bone stock, one or two position screws will serve to buttress the bone graft and the reconstruction.
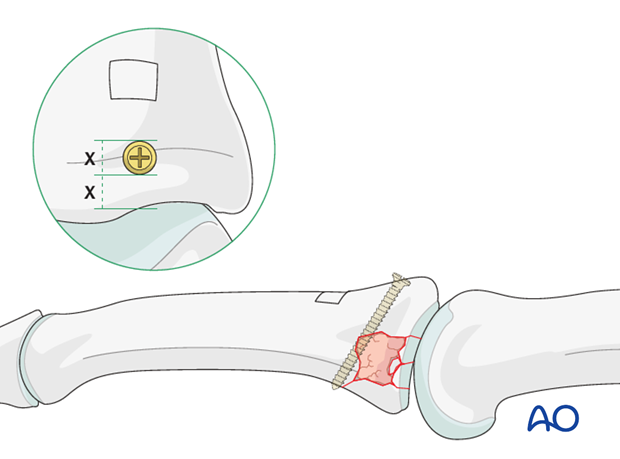
The screw must be inserted into uninjured palmar cortex, and must engage both cortices.
The screw does not need to be inserted parallel to the joint surface. It is more important that it will serve to stabilize the reconstruction, and that it has good purchase in both cortices.
The screw head must be of no greater diameter than a third of the distance between the articular cartilage and the access window. Usually a 1.0 mm or a 1.3 mm screw is used.
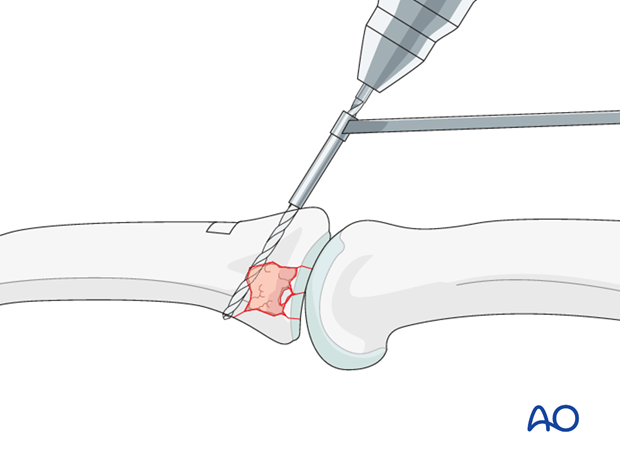
Drilling
Use a drill guide carefully to drill a hole through both cortices.
Accurately measure screw length with a depth gauge.
No countersinking is necessary.
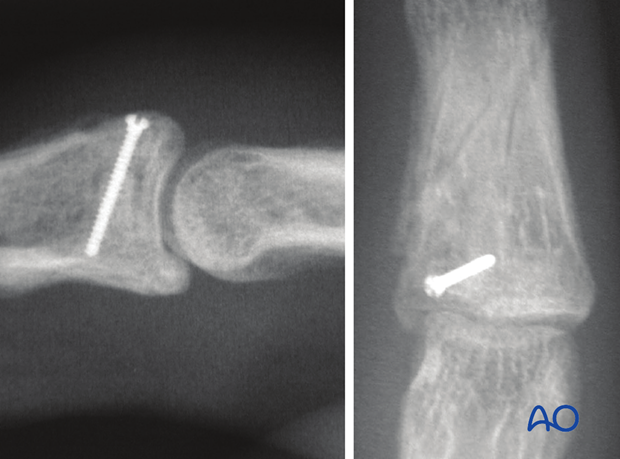
Screw insertion
Gently insert the screw.
If possible, a second screw may be inserted after the same fashion.
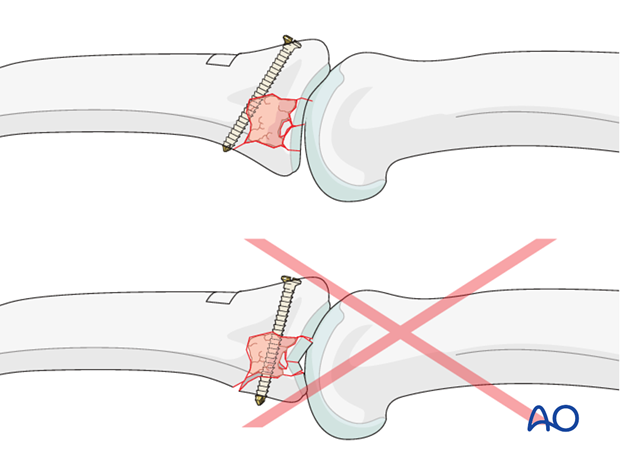
Pitfall: Screw exits in comminuted area
Be careful to insert the screw in such a way that it exits through uninjured cortical bone in the far cortex.
If it exits through the comminuted zone, the reconstruction is at risk of collapsing.
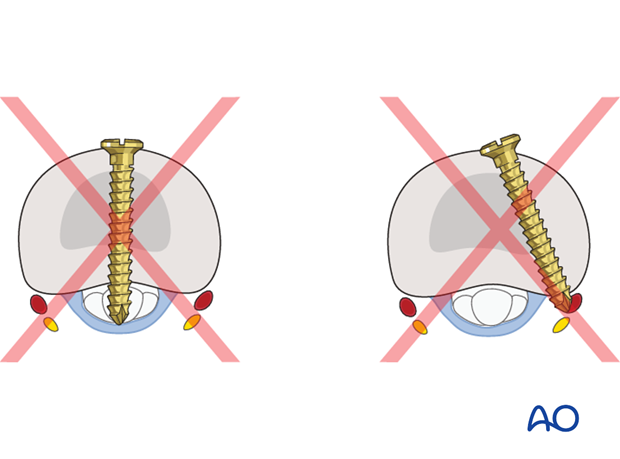
Pitfall: Tendon irritation
If too long a screw is inserted, injury to the neurovascular bundle, or flexor tendon irritation, may result.
7. Aftertreatment
DIP joint movement is encouraged immediately to avoid extensor tendon adhesion.
Functional exercises
Active and passive flexion of the PIP joint is initiated by using a dorsal extension block splint at 30 degrees.
After 4 weeks, the splint is removed, and unrestricted active extension is permitted.
Dynamic extension splinting
If after 5 weeks active extension is not full, dynamic extension splinting is recommended.
During the whole process, the hand therapist should closely monitor the rehabilitation.
The recovery process after such injuries is slow. Reassure the patient to expect 6-8 months for full recovery.