Patient examination
1. Clinical examination
Inspect the soft tissues of the foot.
Deformity with soft tissue risk should be identified and promptly reduced.
Palpate the bony structures to identify points of maximum tenderness. Appreciate instability or crepitation from underlying fractures or dislocations.
Ensure soft tissue perfusion to the distal aspects of the digits.
If possible, assess motor function by requesting the patient to flex and extend toes actively.
Determine the presence of sensation at the distal aspects of the toes; a monofilament may be used.
Dimpling of the skin around a joint may signify a much more significant soft tissue injury or irreducible dislocation. This usually requires an urgent reduction maneuver, either closed or open.
Determine pre-existing conditions such as:
- Diabetic neuropathy
- Osteoarthritis
- Contractures
- Deformities (eg, hammertoe deformities)
- Vascular insufficiency
- History of prior surgical procedures or trauma
Comparing to the uninjured side may be helpful during the assessment.
2. Imaging
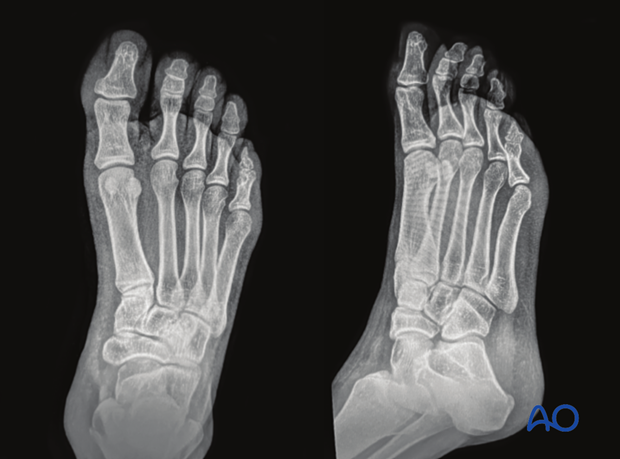
AP, lateral and oblique x-rays of the foot are frequently sufficient to identify the injury.
Advanced images such as CT-scan will clarify intraarticular fracture extensions and small fracture lines.
Images of the uninjured foot may help guide preoperative planning.
This image shows AP and oblique x-rays of a normal foot.