ORIF - Palmar plate
1. Preliminary remarks
Fracture assessment and decision making
These are metaphyseal fractures with no dorsal tilt.
In weak bone (osteoporosis), these fractures may be unstable in a cast and may shorten. If shortening of the radial metaphysis results in relative ulnar overlength, painful ulnar impaction may occur.
When the distal fragment is disimpacted, if there is a significant void created, a palmar locking plate is an effective means of stabilizing the fracture.
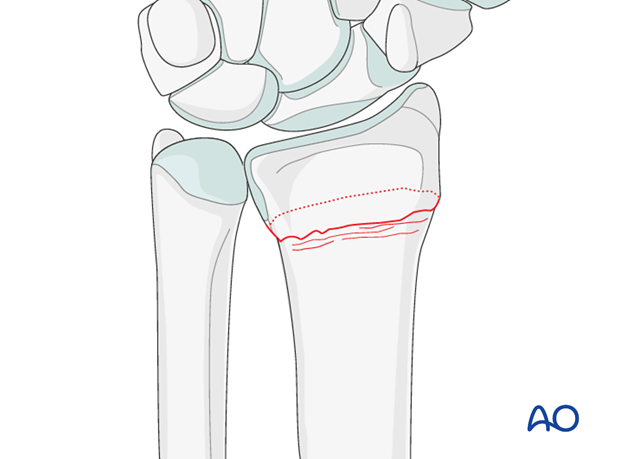
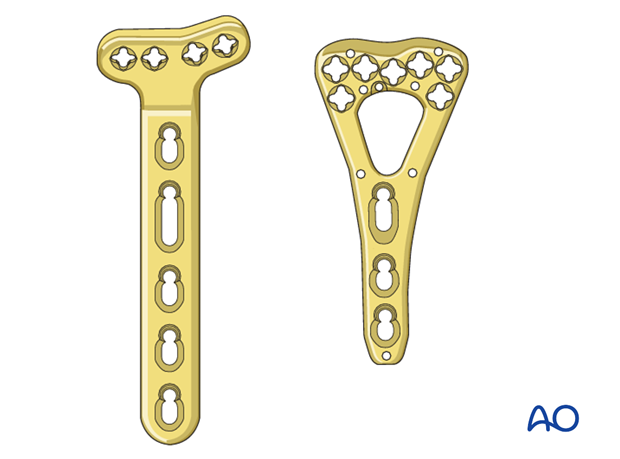
Palmar plate
Advances in plate design have provided angular stable fixation. This allows enhanced stability and ease of application, even in the presence of osteoporotic bone. Plates with variable angle locking screw options may be useful.
2. Patient preparation and approach
Patient preparation
This procedure is normally performed with the patient in a supine position for palmar approaches.
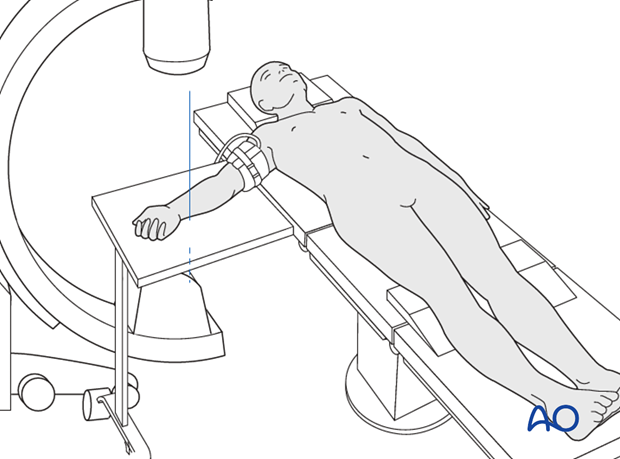
Approach
There are two palmar surgical approaches to the distal radius – a modified Henry approach to the radius and a more ulnar approach, designed to expose the median nerve as well as the distal radius.
A thorough knowledge of the anatomy around the wrist is essential. Read more about the anatomy of the distal forearm.
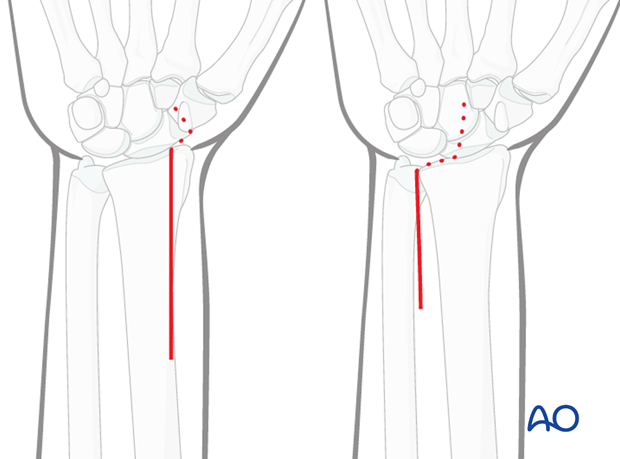
3. Open Reduction
Unlock impaction
Once the fracture is exposed, longitudinal traction is applied to try to disimpact the distal fragment.
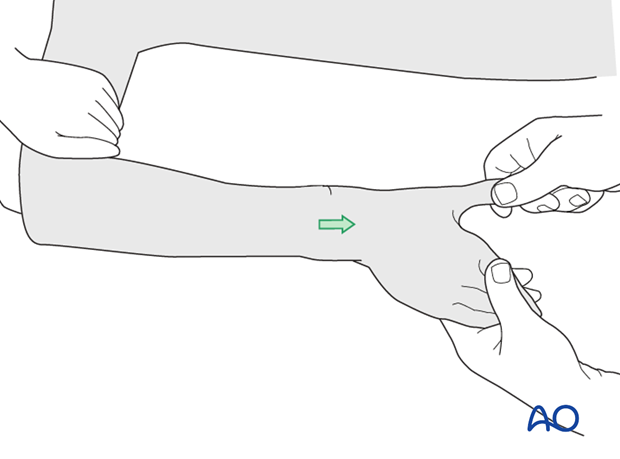
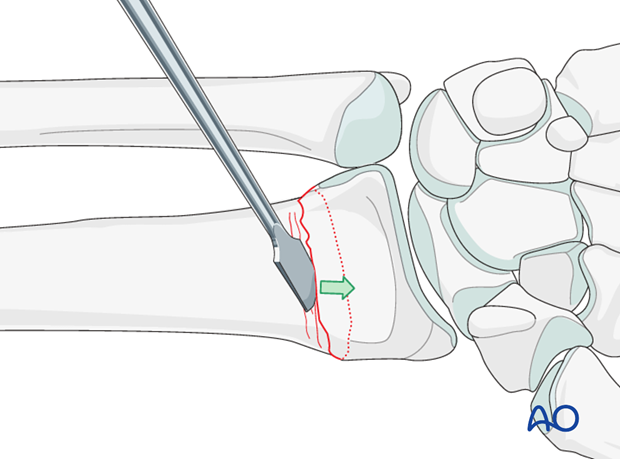
If the distal fragment is not easily disimpacted with traction alone, a periosteal elevator may be inserted into the fracture to help lever the distal fragment into position.
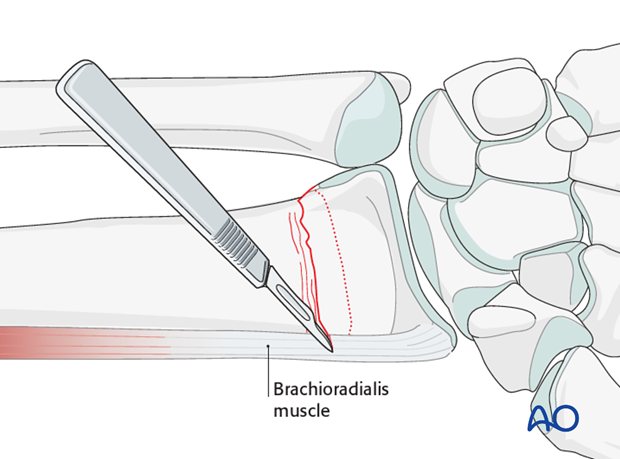
Pearl
Release the insertion of brachioradialis to make disimpaction easier.
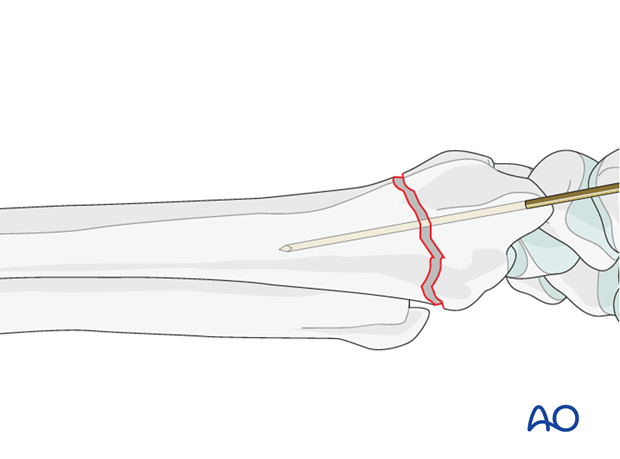
Provisional K-wire fixation
Insert a K-wire across the fracture, through the radial styloid, to provide provisional stabilization.
Confirm the reduction under image intensification.
4. Plate fixation
Plate insertion
Apply the plate to the bone. The distal end of the plate should end at the anatomic watershed zone of the distal radius.
Insert a screw through an oblong hole in the proximal radial fragment. Before fully tightening it, check the plate position using intraoperative imaging, adjusting the position of the plate as necessary.
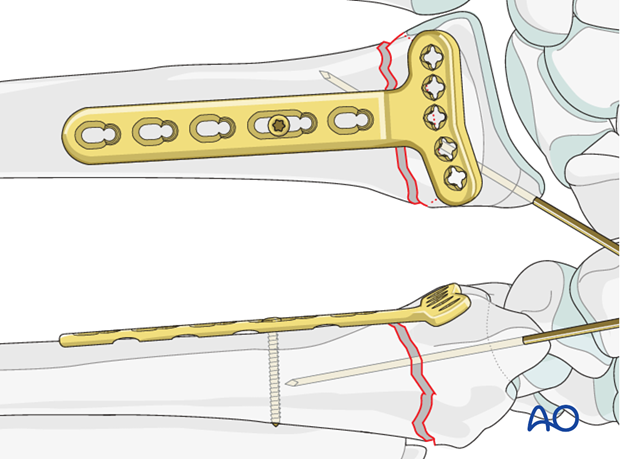
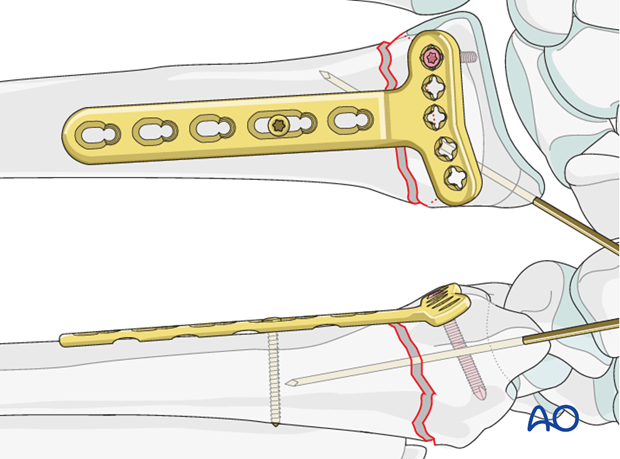
The initial distal screw should be placed through the ulnar sided screw holes.
The reason for this is that if the initial screw is placed on the radial side it will block accurate imaging of the ulnar screw placement.
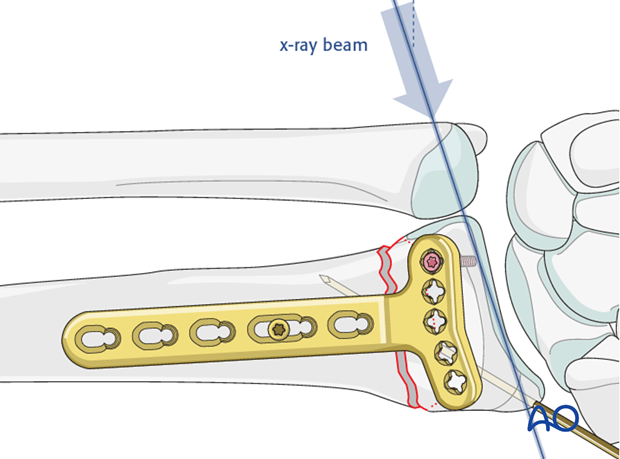
A sagittal image is obtained with the angle of the X-ray beam directed 20° obliquely to the radius to confirm that the screw is not penetrating the radial carpal joint.
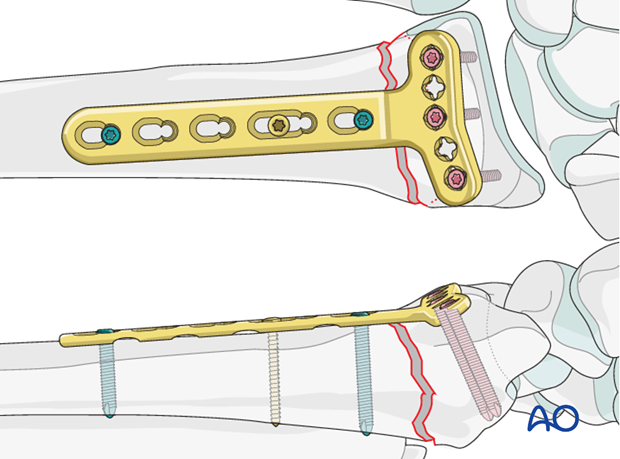
Insert remaining screws
Insert at least 3 distal locking head screws.
Insert at least two more proximal screws.
Remove the K-wire.
5. Aftercare
Functional exercises
Immediately postoperatively, the patient should be encouraged to elevate the limb and mobilize the digits, elbow and shoulder.
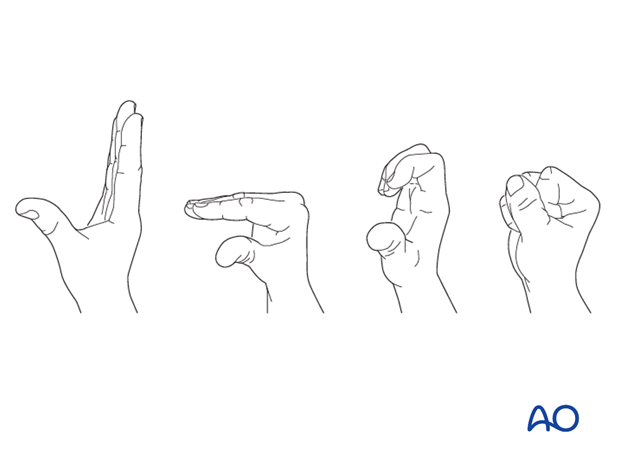
Some surgeons may prefer to immobilize the wrist for 7-10 days before starting active wrist and forearm motion. In those patients, the wrist will remain in the dressing applied at the time of surgery.

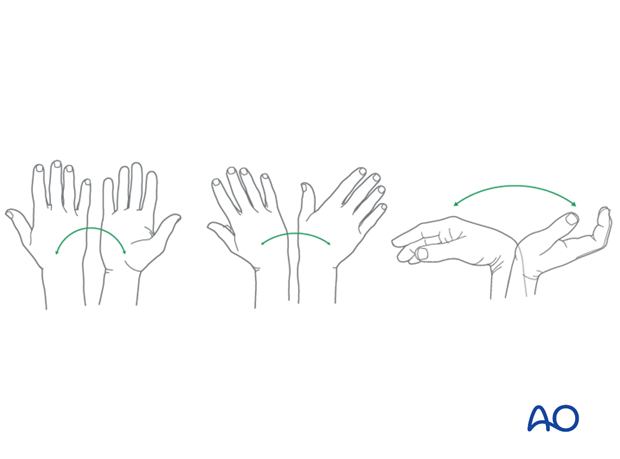
Wrist and forearm motion can be initiated when the patient is comfortable and there is no need for immobilization of the wrist after suture removal.
Resisted exercises can be started about 6 weeks after surgery depending on the radiographic appearance.
If necessary, functional exercises can be under the supervision of a hand therapist.
Follow up
See patient 7-10 days after surgery for a wound check and suture removal. X-rays are taken to check the reduction.
Implant removal
Implant removal is purely elective but may be needed in cases of soft-tissue irritation, especially tendon irritation to prevent late rupture. This is particularly a problem with dorsal or radial plates. These plates should be removed between nine and twelve months.













