ORIF - Dorsoradiopalmar triple plate
1. Preliminary remarks
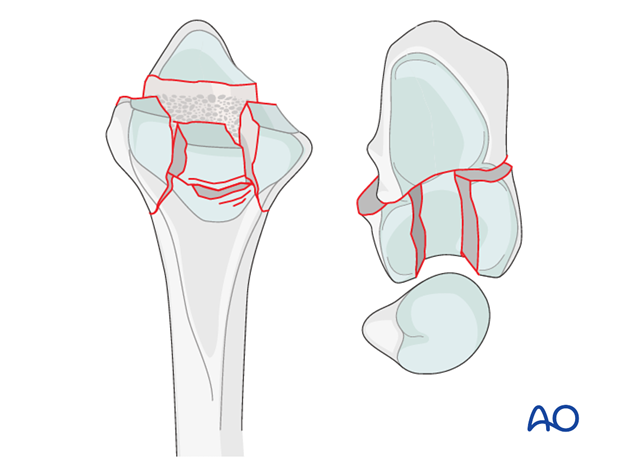
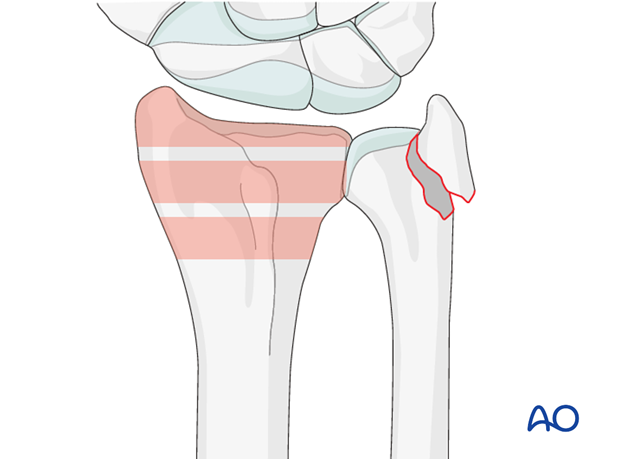
These are complete articular fractures of the distal radius.
As these are intraarticular fractures, where possible, they should be treated with anatomic reduction and absolute stability in order to minimize the risk of subsequent degenerative changes in the joint.
Anatomical reduction and stabilization of these articular fractures is also essential because of the functional implications of the involvement of the distal radioulnar joint.
These are among the most common fractures seen and treated in the older population, with underlying osteoporosis. When these fractures occur in younger individuals, they are more likely to be the result of high energy trauma, with associated soft-tissue, or skeletal injuries.
It is not possible to make an accurate assessment of the details of these injuries without a CT scan.
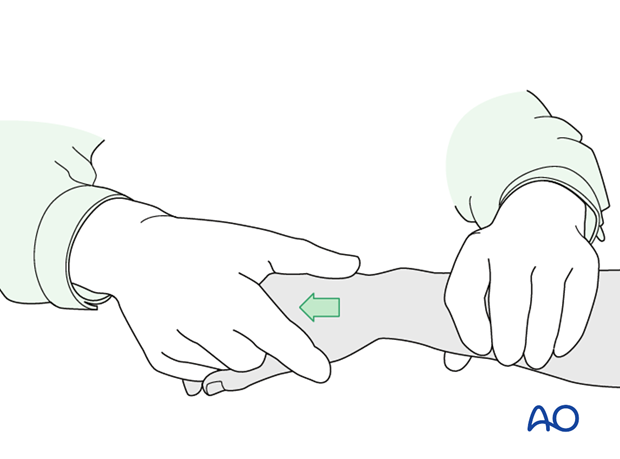
Provisional reduction in displaced fractures
Reduction is achieved by applying longitudinal traction either manually or using Chinese finger traps.
The reduction is maintained by a temporary splint.
If definitive surgery is planned, but cannot be performed within a reasonable time scale, a temporary external fixator may be helpful.
2. Associated injuries
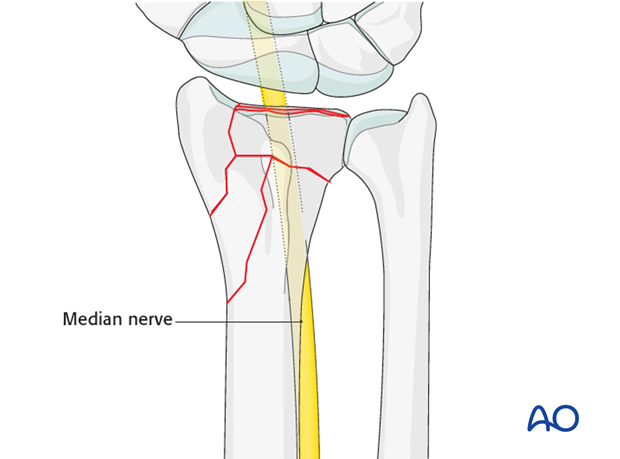
Median nerve decompression
If there is dense sensory loss, or other signs of median nerve compression, the median nerve should be decompressed.
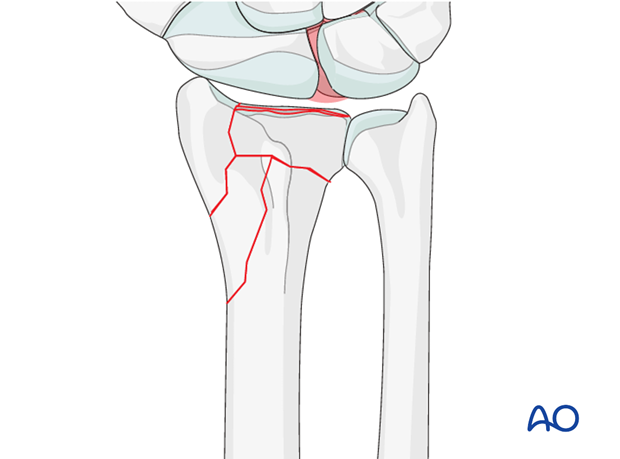
Associated carpal injuries
These injuries may be associated with shearing injuries of the articular cartilage, scaphoid fracture and rupture of the scapholunate ligament (SL). Every patient should be assessed for this injury. If present, see carpal bones of the Hand module.
DRUJ/ulnar injuries
These injuries may be accompanied by avulsion of the ulnar styloid and/or disruption of the DRUJ. If there is gross instability after the fixation of the radial fracture, it is recommended that the styloid and/or the triangular fibrocartilaginous disc (TFC) is reattached. This is not common in simple fractures, but may occur with some high energy injuries.
The uninjured side should be tested as a reference for the injured side.
It may not be possible to assess DRUJ stability until the fracture has been stabilized (as described below).
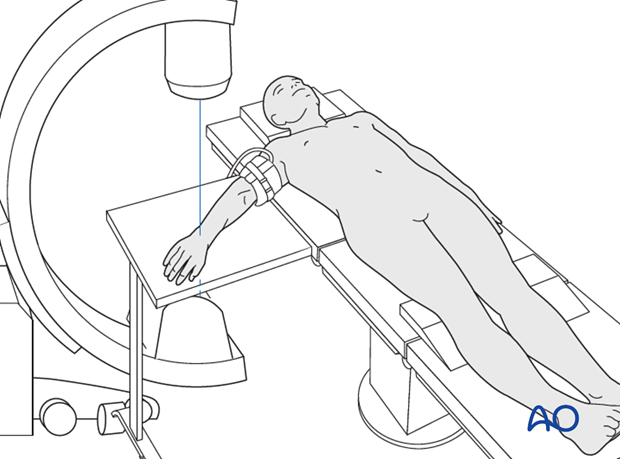
3. Patient preparation
The patient may be placed either in a supine position for palmar approaches or for dorsal approaches.
4. Operative rationale
The rationale for using both palmar and dorsal approaches includes: the hyperextended palmoulnar fragment (intermediate column) and the rotated radial styloid (radial column) requiring a palmar approach; and the displaced dorsoulnar fragment and the impacted central articular fragment (intermediate column) that require a dorsal approach and arthrotomy.
A thorough knowledge of the anatomy around the wrist is essential. Read more about the anatomy of the distal forearm.

5. Reduction and fixation of the palmoulnar and radial styloid fragments
Reduction of the palmoulnar fragment
If only the palmar lunate facet fragment needs to be stabilized, an ulnopalmar plate can be used. This is applied via an ulnar palmar approach.
After direct reduction of the palmoulnar fragment, an appropriate plate is inserted.
A screw is inserted through the oblong hole to allow longitudinal adjustment of plate position.
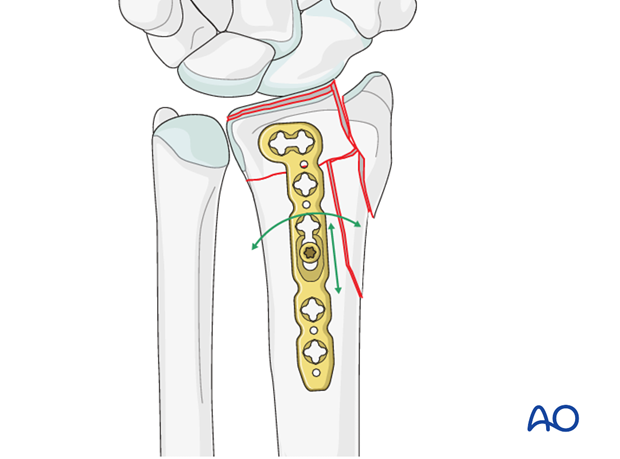
As an alternative, a palmar plate may be applied through a modified Henry approach.
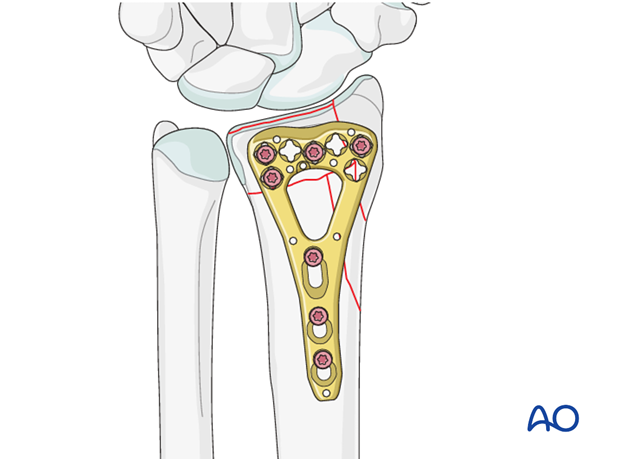
Preliminary fixation of the palmoulnar fragment
The palmoulnar fragment itself is now secured to the distal transverse limb of the plate with a short locking head screw.
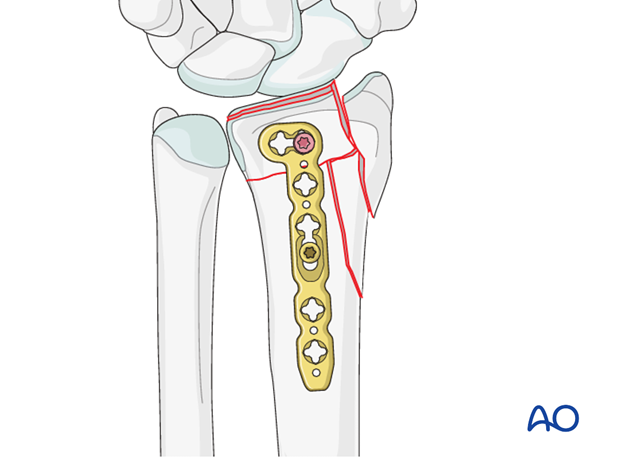
Buttressing of the radial column
A radial S-shaped plate of appropriate length is chosen to buttress the radial column, and is contoured further as necessary. This is applied through a dorsal approach.
The plate is positioned and fixed to the diaphysis using a standard cortical screw through the oblong hole. A pointed reduction forceps is then used to reduce the radial styloid fragment and to hold the plate in place.
At this stage, reduction and plate position are checked by image intensification.
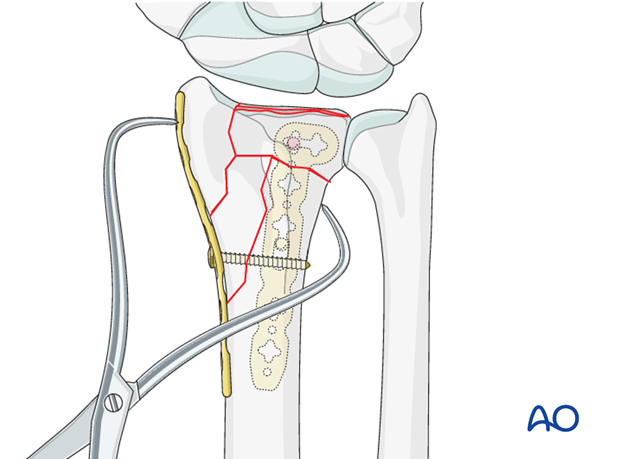
Definitive fixation
After confirming the correct position of the palmar plate, it is secured definitively with a second standard cortical screw through its most proximal hole.
After confirming the correct position of the radial plate, it is fixed definitively with a second screw through its most proximal hole. The radial styloid fragment is secured with a short locking head screw.
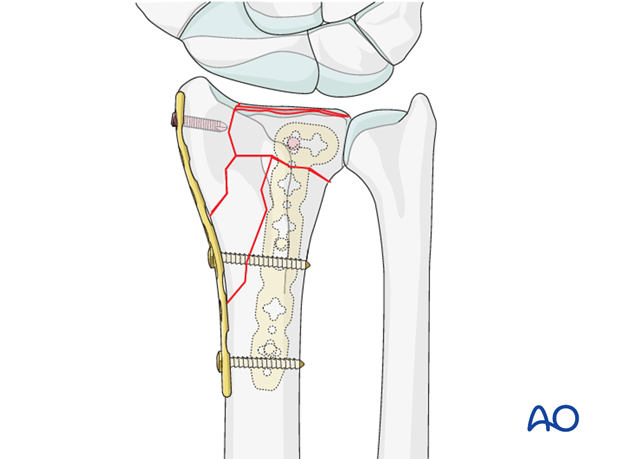
6. Reduction and fixation of the intermediate column
Reduction of the central articular fragment
After gentle retraction of the dorsoulnar fragment, the large articular fragment that is impacted into the metaphysis is identified.
The fragment is levered up and reduced onto the proximal carpal row.
In this illustration, the overlying ulna and the radial plate have been omitted in the interest of clarity.
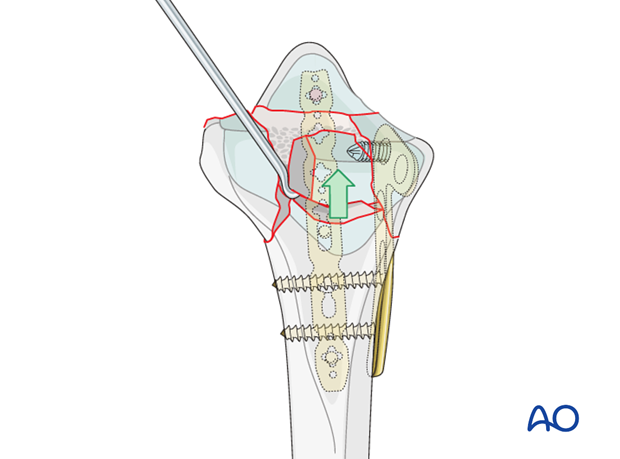
Reduction of the dorsoulnar fragment
The retracted dorsoulnar fragment is then replaced and preliminarily secured with a K-wire that additionally holds in place the reduced central articular fragment.
The radiocarpal joint surface is checked for residual gap, or step off.
Note
If a large metaphyseal defect is created by elevation of the central impacted fragment, and especially if a nonlocking plate is used, autogenous cancellous bone should be packed into the gap, prior to reduction of the dorsoulnar fragment.
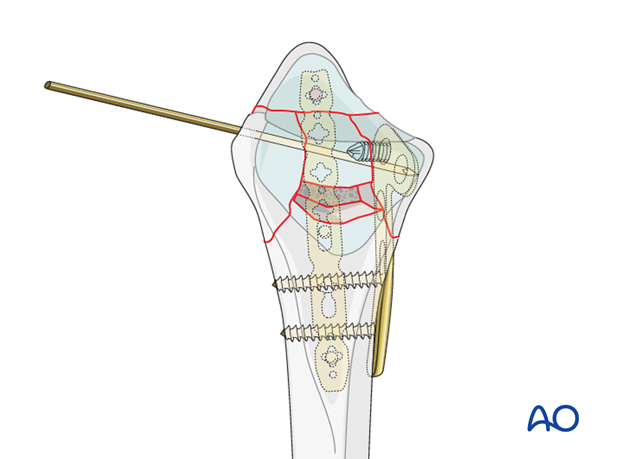
Plate selection and preparation
An appropriate plate is selected according to the fracture configuration. The choice of the plate (T-, or L-shaped) is determined by the fracture pattern. If necessary, the plate can be contoured.
A plate which allows variable angle locking screws may be very useful in this situation.
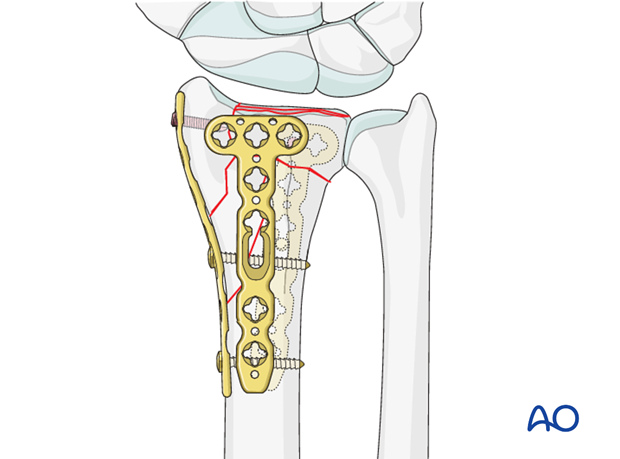
Plate application
Fix the plate provisionally with a standard cortical screw through the oblong hole.
Check the reduction and position of the implants using image intensification.
If necessary, adjust the reduction and plate position, then tighten the screw.
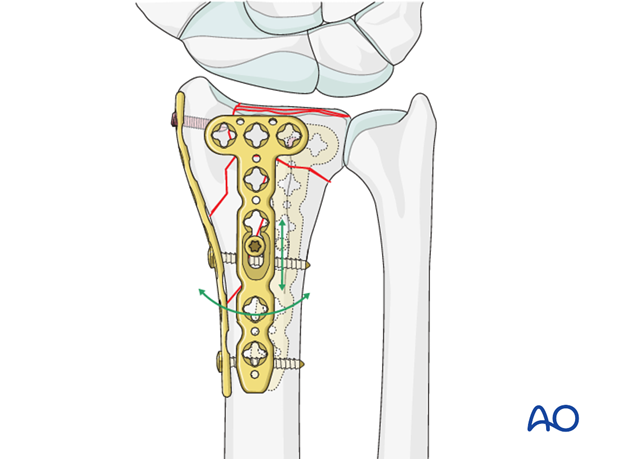
Image intensifier control
Reduction and plate position are checked at this stage using image intensification.
Provided the radiocarpal joint has been reconstructed and there is no major step off, a slight residual dorsal tilt of the radiocarpal joint line, in the lateral view, can be accepted.
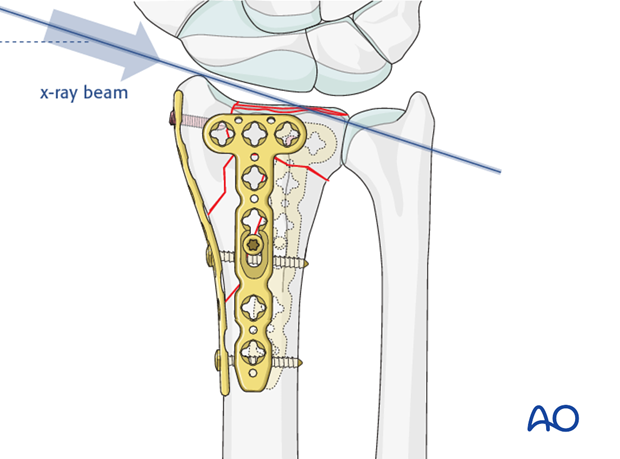
Definitive fixation of plate
After confirming the correct position of the plate using image intensification, it is fixed to the bone with a second standard cortical screw through its most proximal hole, and the screw through the oblong hole is then tightened fully.
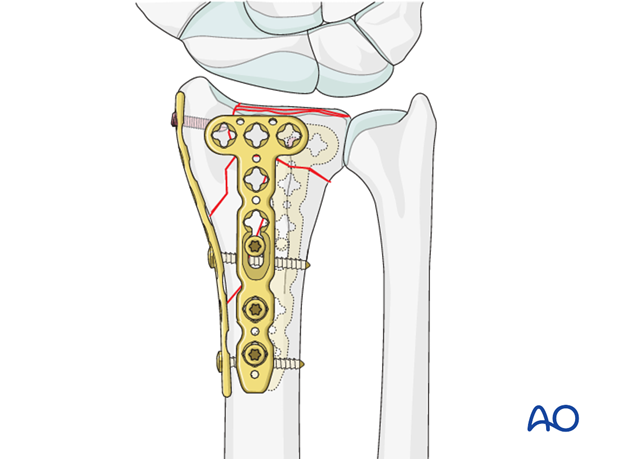
Locking head screws are then inserted distally to secure the dorsal fragments of the radiocarpal joint.
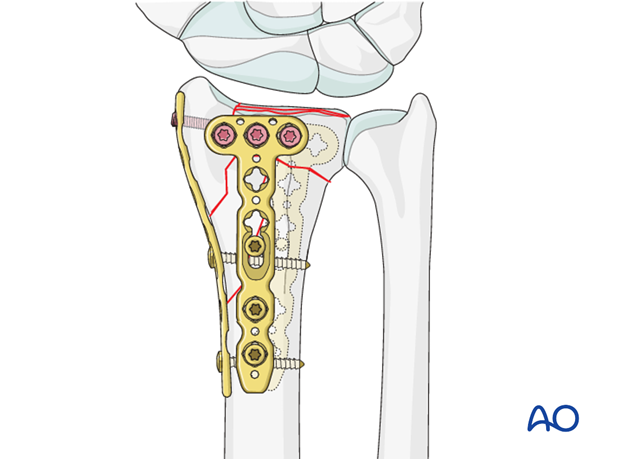
7. Assessment of Distal Radioulnar Joint (DRUJ)
Before starting the operation, the uninjured side should be tested as a reference for the injured side.
After fixation, the distal radioulnar joint should be assessed for forearm rotation, as well as for stability. The forearm should be rotated completely to make certain there is no anatomical block.
Method 1
The elbow is flexed 90° on the arm table and displacement in dorsal palmar direction is tested in a neutral rotation of the forearm with the wrist in neutral position.
This is repeated with the wrist in radial deviation, which stabilizes the DRUJ, if the ulnar collateral complex (TFCC) is not disrupted.
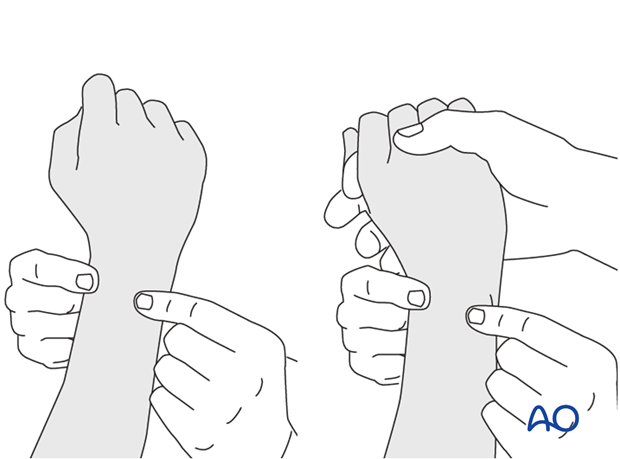
This is repeated with the wrist in full supination and full pronation.
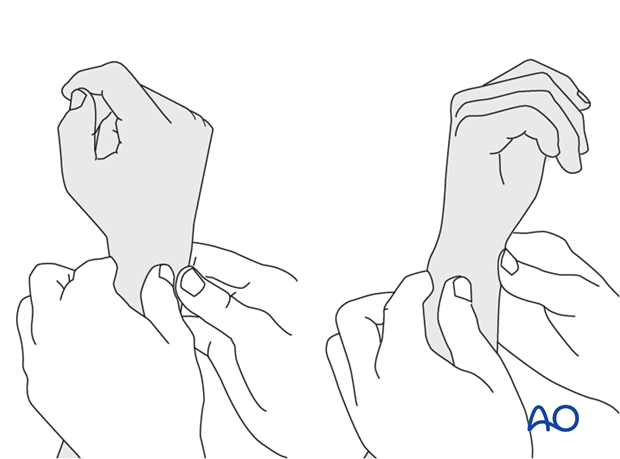
Method 2
To test the stability of the distal radioulnar joint, the ulna is compressed against the radius...
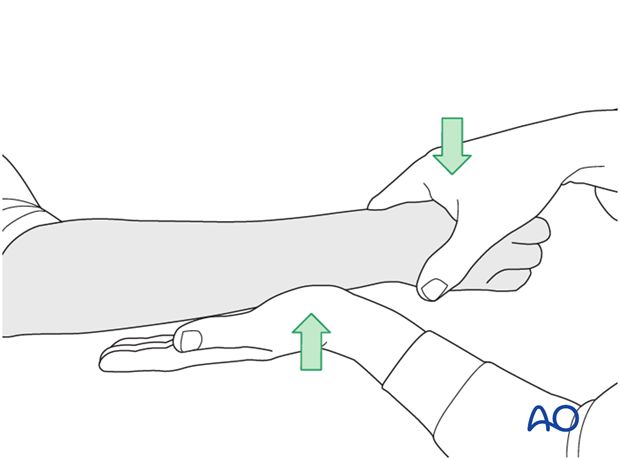
...while the forearm is passively put through full supination...
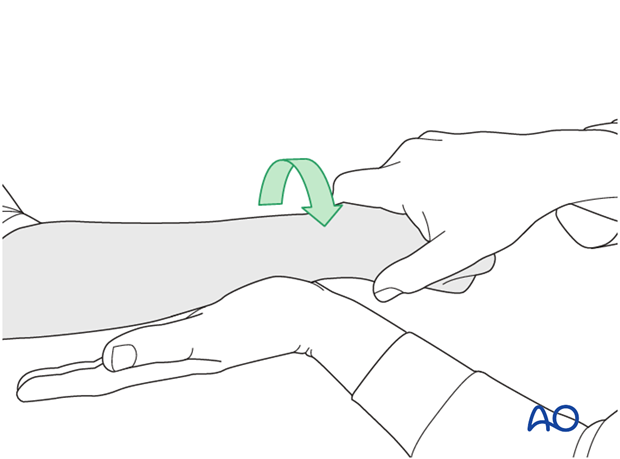
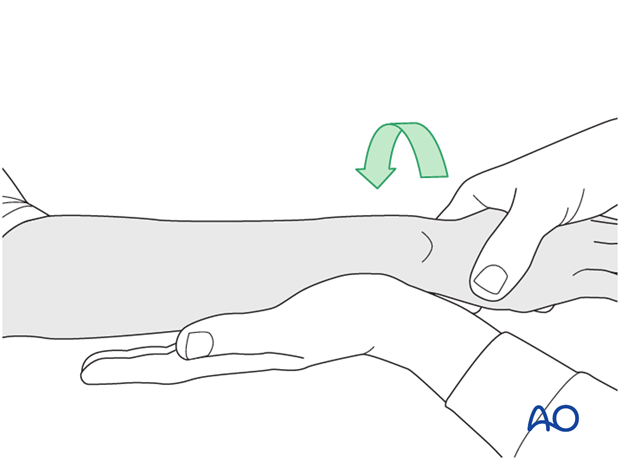
...and pronation.
If there is a palpable “clunk”, then instability of the distal radioulnar joint should be considered. This would be an indication for internal fixation of an ulnar styloid fracture at its base. If the fracture is at the tip of the ulnar styloid consider TFCC stabilization.
8. Aftercare
Functional exercises
Immediately postoperatively, the patient should be encouraged to elevate the limb and mobilize the digits, elbow and shoulder.
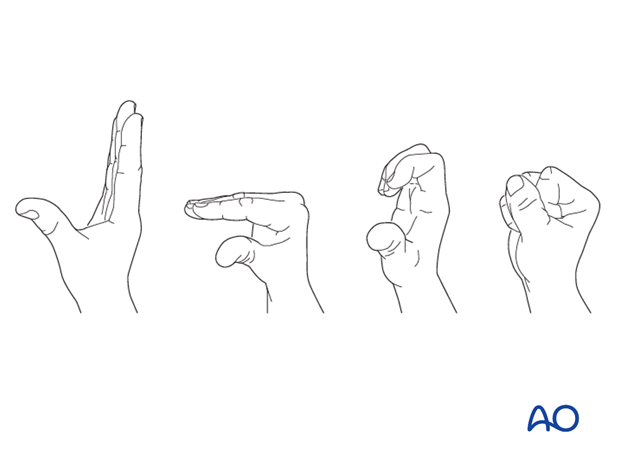
Some surgeons may prefer to immobilize the wrist for 7-10 days before starting active wrist and forearm motion. In those patients, the wrist will remain in the dressing applied at the time of surgery.

Wrist and forearm motion can be initiated when the patient is comfortable and there is no need for immobilization of the wrist after suture removal.
Resisted exercises can be started about 6 weeks after surgery depending on the radiographic appearance.
If necessary, functional exercises can be under the supervision of a hand therapist.
Follow up
See patient 7-10 days after surgery for a wound check and suture removal. X-rays are taken to check the reduction.
Implant removal
Implant removal is purely elective but may be needed in cases of soft-tissue irritation, especially tendon irritation to prevent late rupture. This is particularly a problem with dorsal or radial plates. These plates should be removed between nine and twelve months.













