ORIF - Lag screw with neutralization plate
1. Introduction
Goal of treatment
The goal of treatment for a simple two part fracture of the shaft of the clavicle requires anatomical reduction and absolute stability.
Note: This is the most common pattern. The deforming forces on the medial end is the pull of the muscles and the deforming force on the lateral side is the weight of the upper extremity.
Beware of the major neurovascular bundle (subclavian artery, vein, and brachial plexus) running directly beneath the midshaft of the clavicle.
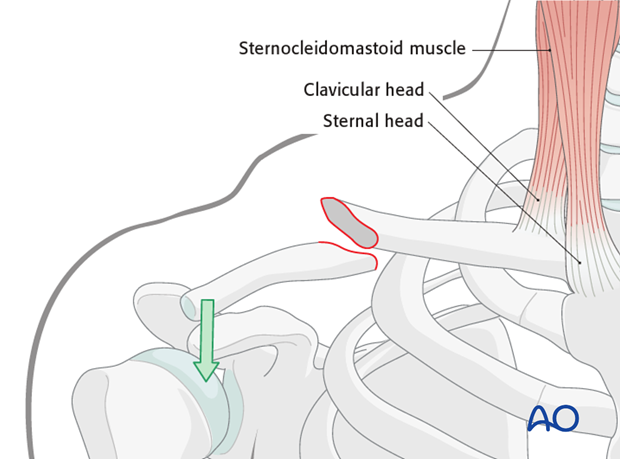
Other types of deformities may occur if the coracoclavicular ligaments are disrupted (eg, superior displacement of the lateral fragment).
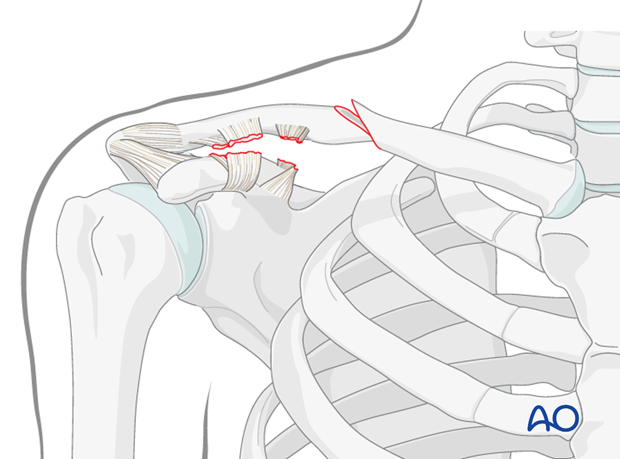
Lag Screw
The optimal inclination of the screw in relation to a simple fracture plane is 90°.
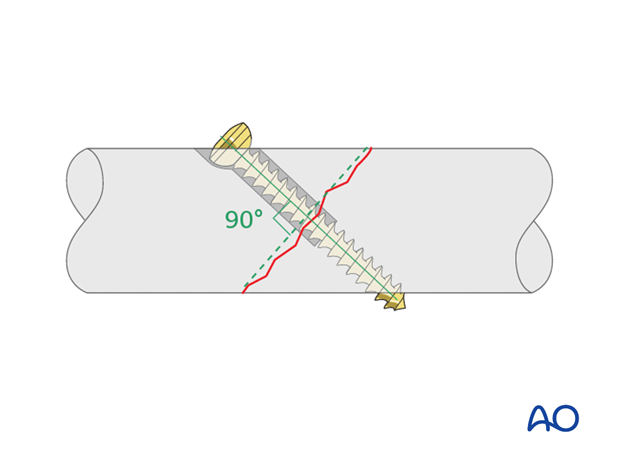
Neutralization plate
Lag screw fixation alone is typically insufficient to withstand the normal physiologic forces. A neutralization plate is required for additional stability to distribute the forces and allow early mobilization.
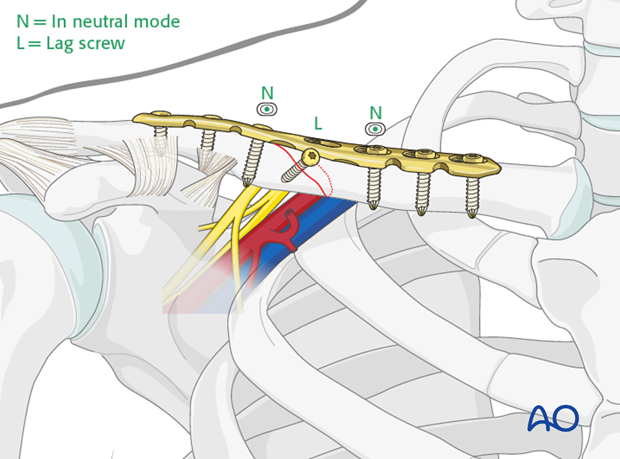
Plate alternatives
We will here show the procedure with a precontoured clavicular plate which has both a bend and a twist built into it.
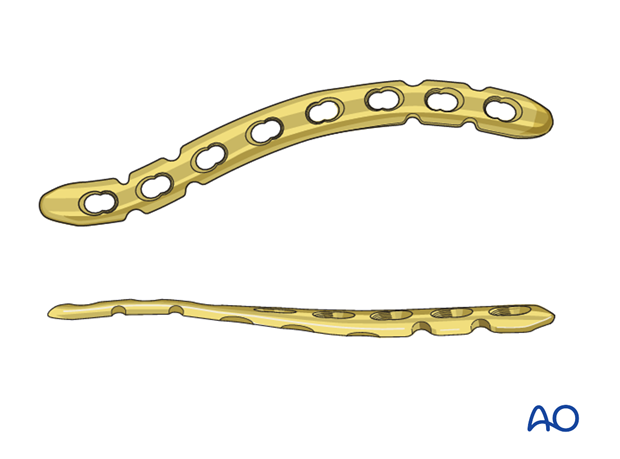
However, if a precontoured clavicular plate is not available, there are other options.
A straight plate may be used if it fits the clavicle (conventional or angle stable). If it does not, then it needs to be contoured.
This is best achieved with a slight twist at the midportion of the plate. This results in the lateral plate being applied superiorly and the medial portion anteriosuperiorly. A reconstruction plate which is easier contour may be used in smaller patients where the forces working on the plate are not as great.
Biomechanically, anterosuperior or anterior plates result in mechanically stronger fixation. The exact placement of the plate will depend on the fracture pattern and the position of the fracture.

2. Patient preparation and approach
Patient preparation
This procedure is normally performed with the patient either in a beach chair or a supine position.
Approach
For this procedure an anterior approach is normally used.
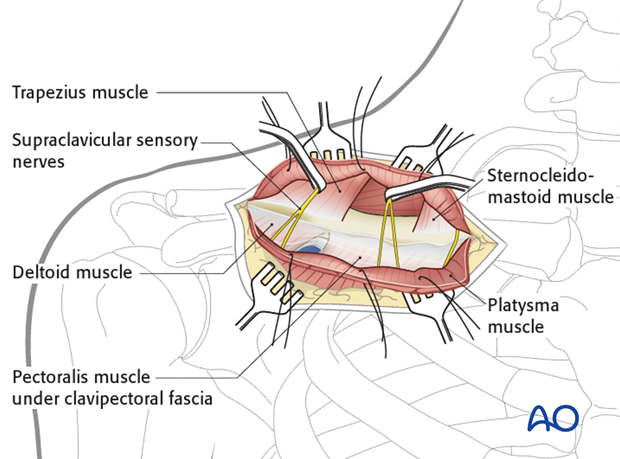
3. Reduction and fixation
Reduction
Using the fracture interdigitations as a gauge for the reduction, obtain control over the proximal and distal fragments using reduction clamps. Gentle traction using a lobster clamp on the lateral fragment or the free draped arm, and a derotation force, typically to the lateral fragment will assist to anatomically reduce the fracture.
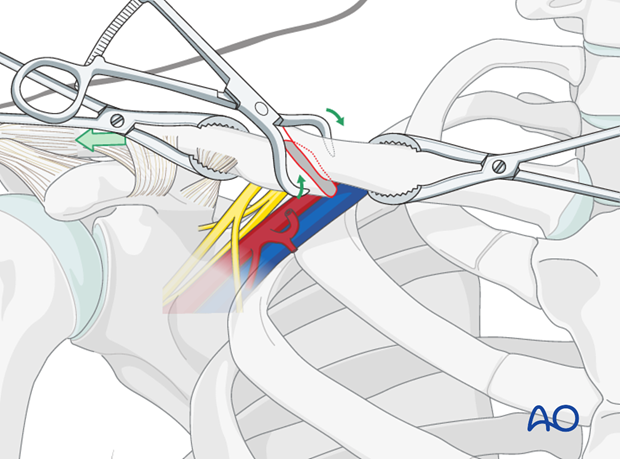
Lag screw insertion(s)
Provisional stability is maintained with a pointed clamp followed by the insertion of one or more lag screws (2.7 or 3.5).
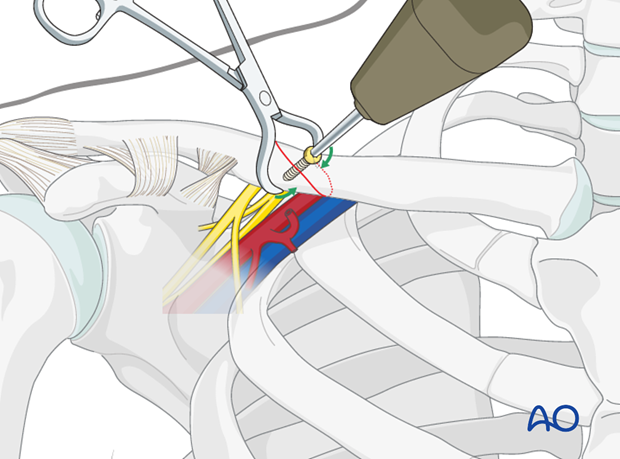
Plate application
The plate is secured with sufficient bicortical screws inserted in a neutral mode avoiding the previously inserted lag screw.
Typically, a minimum of three bicortical screws in each segment is sufficient.

Note: Occasionally when the fracture location is more lateral or more medial, the bone quality near the metaphysis may not offer sufficient screw purchase. In these instances, a plate offering additional screw fixation may be required (eg, longer plate, periarticular plate, locking screws).
4. Aftercare
The aftercare can be divided into 4 phases:
- Inflammatory phase (week 1–3)
- Early repair phase (week 4–6)
- Late repair and early tissue remodeling phase (week 7–12)
- Remodeling and reintegration phase (week 13 onwards)
Full details on each phase can be found here.













