Extradural middle fossa repair using temporal fascia flap
1. General considerations
A lateral craniotomy after temporal skin incision offers the possibility of inspection of the whole lateral skull base including the upper portions of the petrous bone. Special care should be taken to perform the craniotomy as far basal as possible eventually after temporary removal of the zygomatic arch.
One has to consider that the reconstruction of the lateral skull base after trauma is only necessary in a small number of cases. Normally, after simple fracture even with rhinorrhea the problem can be solved by conservative management.
If it is necessary to perform that kind of procedure, the use of microsurgical techniques is highly recommended.
2. Approach
For this procedure a lateral skull bases approach is normally used.
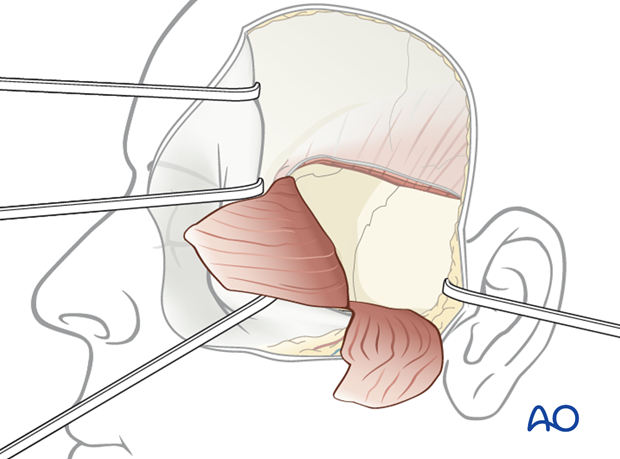
3. Extradural middle fossa repair using temporal fascia flap
After a classical subtemporal trepanation is performed, careful elevation of the temporal lobe according to the location of the skull base fracture is done.
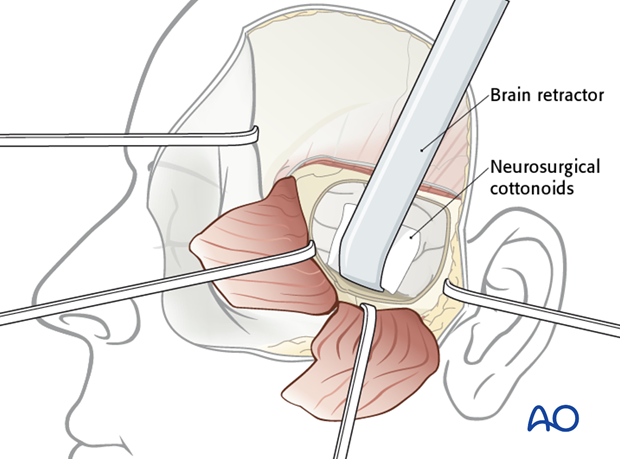
Localize the fracture segments and/or dural defect and remove any loose or displaced bony fragments.
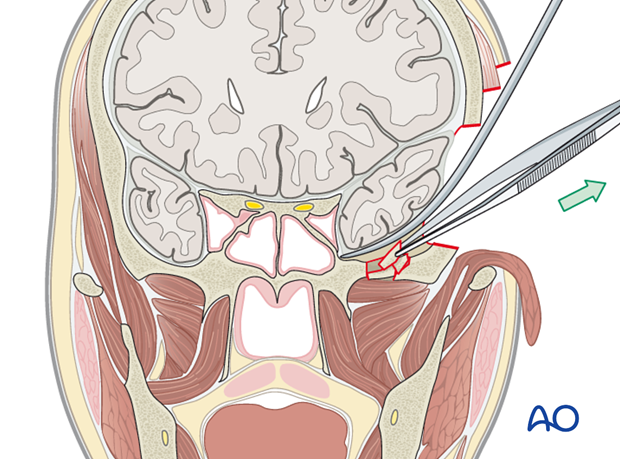
In some cases, it may be sufficient to smooth any sharp edges with a burr.
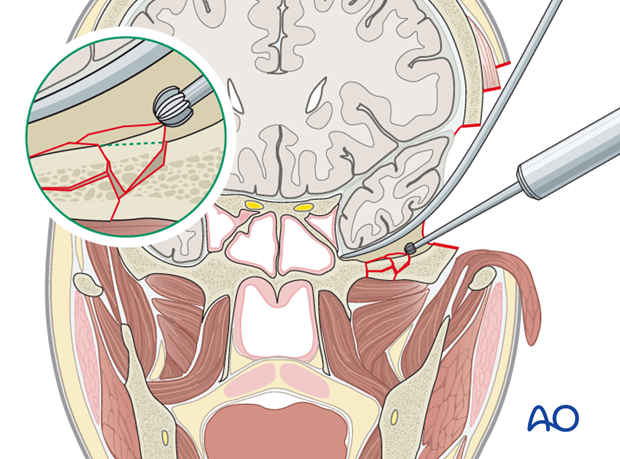
Dissect a pedicled temporal fascia flap from the underlying muscle.
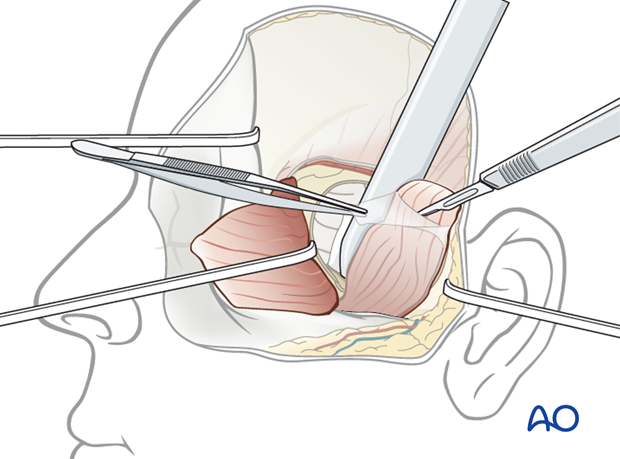
The pedicled temporal fascia flap is brought into the intracranial space in that way that the middle cranial fossa is covered.
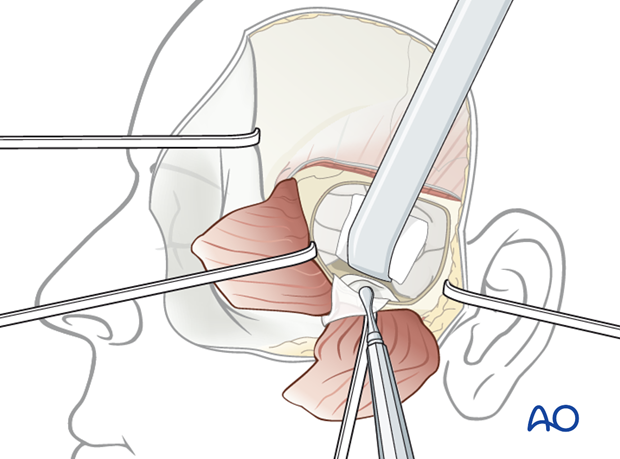
Depending on the size of the dural laceration, the temporal fascia flap should be sutured to the dura.
To achieve a water-tight closure, the use of sealant techniques is highly recommended.
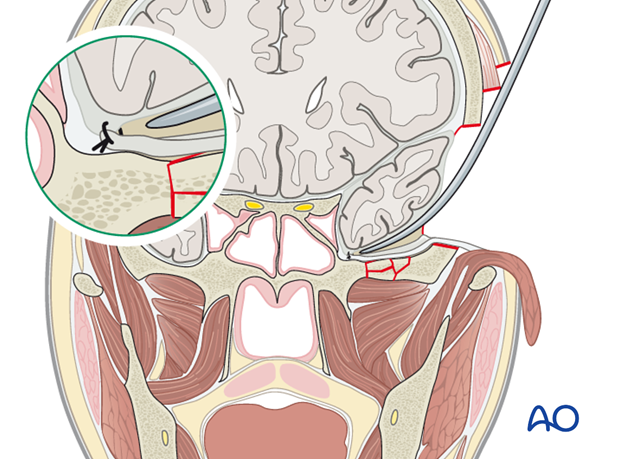
Fix the dura to the bone margins with 4-5 stitches.
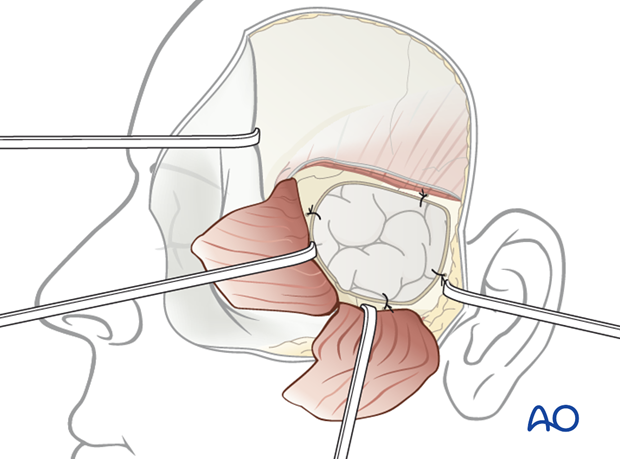
Replace the bone flap using internal fixation in a stable three point fixation technique.
Suspension sutures of the dura to the bone flap is highly recommended to avoid possible postoperative epidural hematoma.
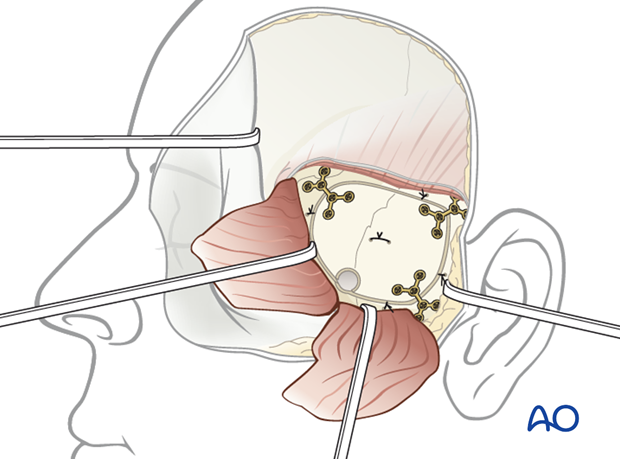
4. Aftercare following open management of skull base fractures
General postoperative care
- Intensive care 24 hours
- Hospitalization 5-8 days (to rule out reoccurrence of CSF leak)
- The use of broad-spectrum antibiotics during and after the procedure for the next 5-7 days is recommended.
- Radiologic control examinations are performed routinely the next day after leaving the intensive care unit.
- Patient follow-up after discharge. The patient is seen 4 weeks after, and if necessary, for the long-term follow-up a year postoperatively.













