Closed treatment, MMF
1. Treatment
This procedure is typically performed with the patient placed in a supine position.
Arch bars are applied to the teeth and MMF is secured. The patient is monitored for positional changes of the mandibular ramus using x-rays. After a period of at least 6 weeks, MMF is released and fracture stability determined by manipulation. The patient is placed on a soft diet and if the occlusion maintains for a two-week period after the MMF has been discontinued, the arch bars may be removed.
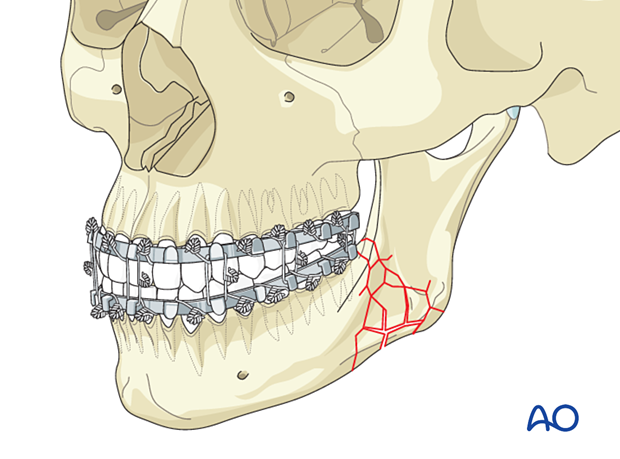
2. Case example
Images
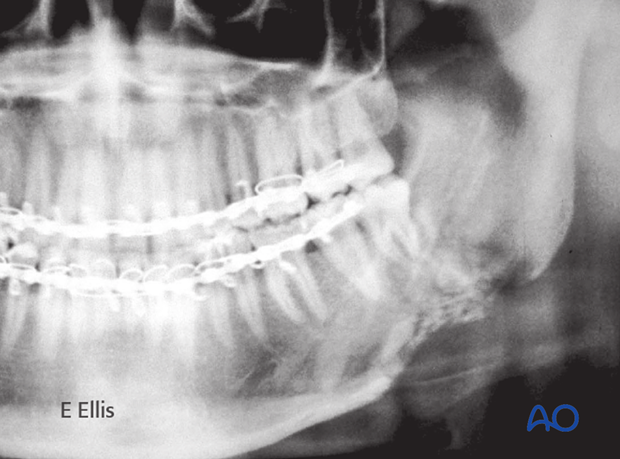
OPG shows a right comminuted mandibular fracture.
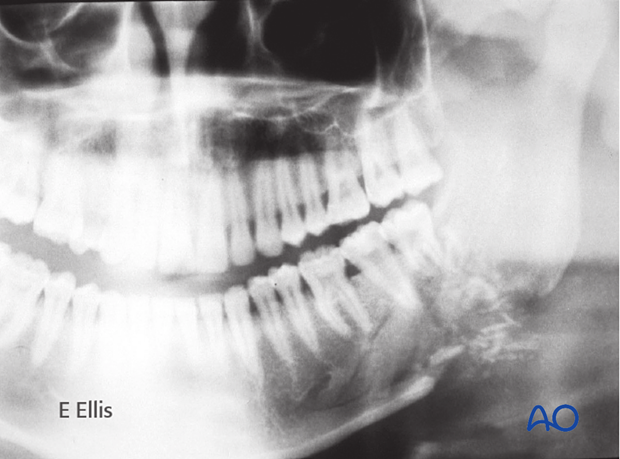
PA x-ray of the same case.
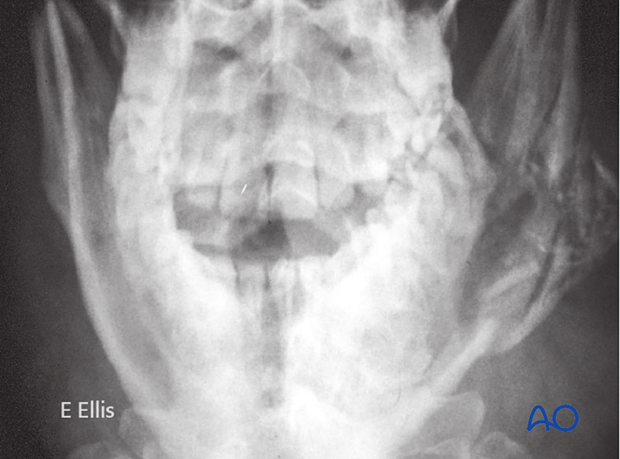
Principles
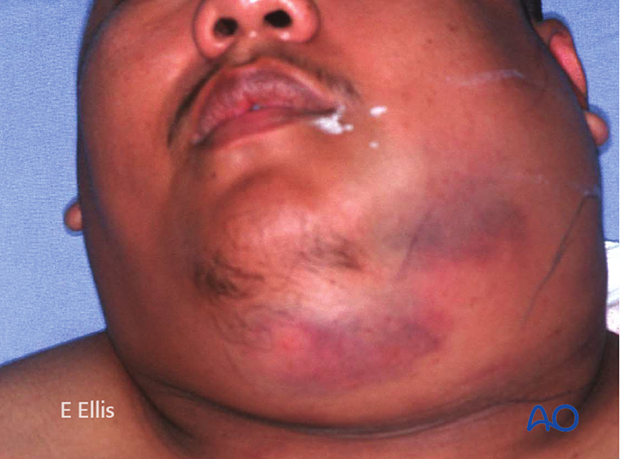
Massively swollen face with comminuted angle fracture. Open treatment would be extremely difficult no matter which surgical approach is selected.
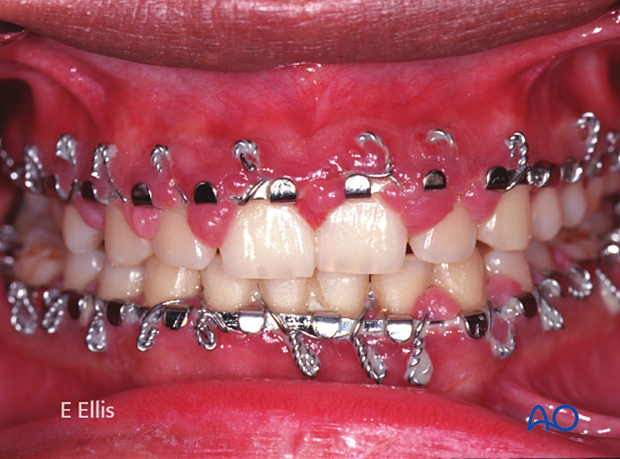
Because the occlusion could be readily reestablished, MMF was the selected treatment.
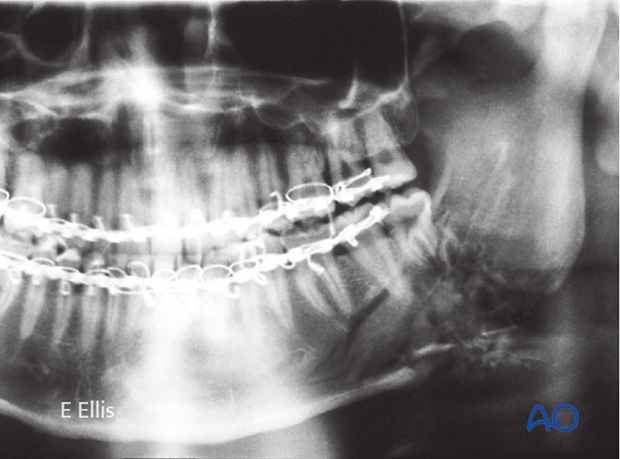
Postoperative x-rays
Postoperative x-rays following closed treatment and MMF show good alignment of bone fragments...
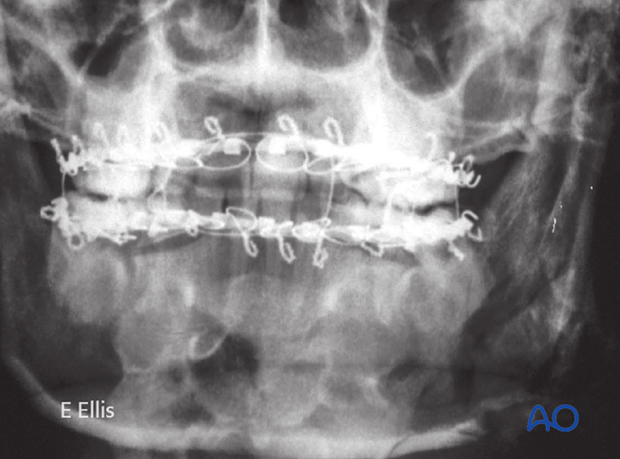
...and reestablishment of occlusion.
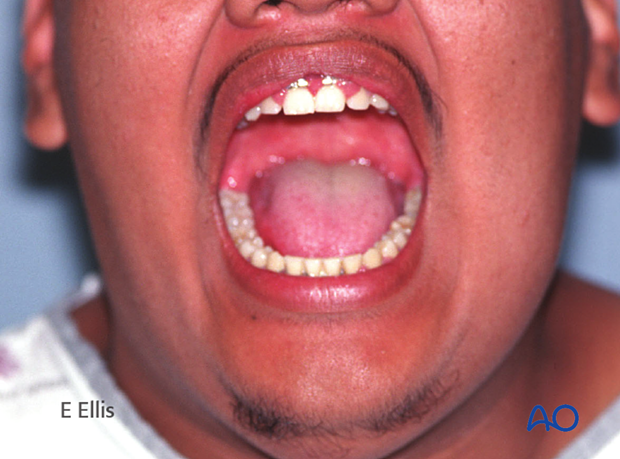
Outcome
Six weeks of MMF was indicated. Following rehabilitation of function, patient developed good mouth opening and occlusion and solidification of the fracture.
3. Aftercare following closed treatment of mandibular body, ramus, symphysis, and angle fractures
Release of MMF and elastics
The patient should be instructed how to release the MMF in case of an emergency. Some surgeons prefer to provide wire cutters to the patient for the period of MMF. During this period, wire fatigue and loosening can occur. The patient should report any loosening of the MMF to the surgeon immediately.
As an alternative, the MMF may be achieved by using elastics instead of wires. With an adequate number of elastics, the same level of reliability can be reached minimizing the risk of inability to release the MMF during an emergency situation.
X-Rays
Postoperative x-rays are taken within the first days after surgery. In an uneventful course, follow-up x-rays are taken prior to releasing the MMF.
Follow up
It will be necessary to see the patient approximately 1 week postoperatively to assess the stability of the occlusion and to check for infection of the surgical wound. The intermaxillary fixation wires or elastics must be assessed and proven to hold the patient tightly in occlusion. Patients also have to be periodically re-examined to rule out signs of infection. At each visit, the surgeon must evaluate the patient's ability to perform adequate oral cleaning. It may be necessary to provide additional instruction to assure appropriate hygiene and wound care.
Malocclusion
There should be no malocclusion detected as occlusion is determined and secured in the operating room.
Release of MMF
On releasing the MMF, physiotherapy can be prescribed. The mandible will be hypomobile after the period of MMF, and the muscles will be atrophic and “tight.” Opening and excursive exercises should be demonstrated and implemented. Goals should be set, and typically, 40 mm of maximum interincisal mouth opening should be attained by 4 weeks postoperatively. If the patient cannot fully open his or her mouth, additional passive physical therapy may be required.
Basic postoperative instructions
DietThe diet has to be in a liquid or semi-liquid form. For patients with a full complement of teeth, the diet must be more liquefied than when there are gaps with teeth missing. Because the diet will be no-chew, more fluids are required to assist in swallowing the food. A blender, or preferably, a juicer is useful. Anything can be made into a liquid or semi-liquid form with these tools. Liquid dietary supplements from the grocery store help maintain caloric intake. The patient should monitor their body weight on a weekly basis during the period of MMF to evaluate any dramatic changes.
Patients must be instructed in oral hygiene procedures. The presence of the arch-bars and MMF wires makes this a much more difficult procedure, and the inside of the teeth cannot be reached with a toothbrush. A soft toothbrush (dipping in warm water makes softer) should be used to clean the buccal/labial surfaces of the teeth, arch-bars and wires. Chlorhexidine oral rinses should be prescribed and used at least 3 times each day to help sanitize the mouth.
The patient should be warned to continue routine follow up with their dentist. Fractures near the dental roots can often result in delayed loss of tooth viability, requiring periapical films and additional dental procedures.













