Reinnervation with cross facial nerve graft
1. Introduction
There are several options to power the facial nerve. The commonest options include:
- Cross face (contralateral VII)
- Masseteric nerve
- Hypoglossal (XII)
Selective reinnervation can be considered in which a local nerve is used for eye closure and the masseteric nerve is used to power smile.
General considerations regarding nerve repair techniques can be found here.
2. Cross face reinnervation
Approach and branches identification
A facelift, or parotidectomy type incision is performed on both the ipsilateral and the contralateral side and the distal branches identified as they exit the parotid gland. Existing lacerations may also be used if present.
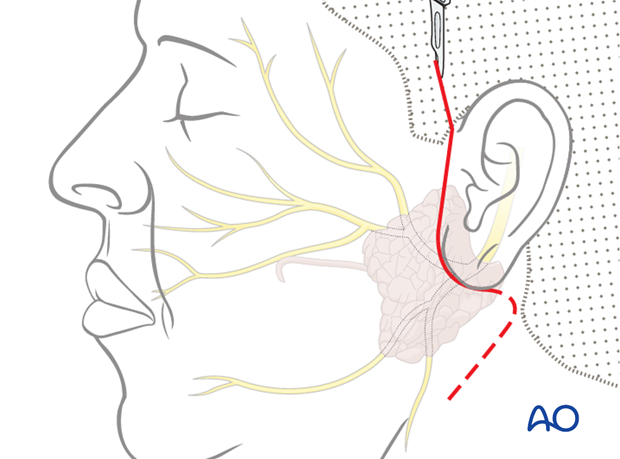
Preparation of contralateral nerves
On the contralateral side, intraoperative stimulation of the branches is used to identify which branches are responsible for eye-closure and which are responsible for smiling.
Multiple branches are identified and 50% of branches responsible for smiling (zygomaticus major) and 50% of the branches responsible for eye closure (orbicularis oculi) can be sacrificed without loss of function and used to power the paralyzed side through nerve graft.

Preparation of distal ipsilateral nerves
On the ipsilateral (paralyzed) side the distal branches of the facial nerve are exposed as they exit the parotid.
Intraoperative direct nerve stimulation may be possible up to 7 days from time of injury.
If not successful, the distal nerves are identified as they exit the parotid.
The distal nerves are dissected in retrograde fashion (from distal to proximal) through the parotid gland until the lacerated branches are identified.
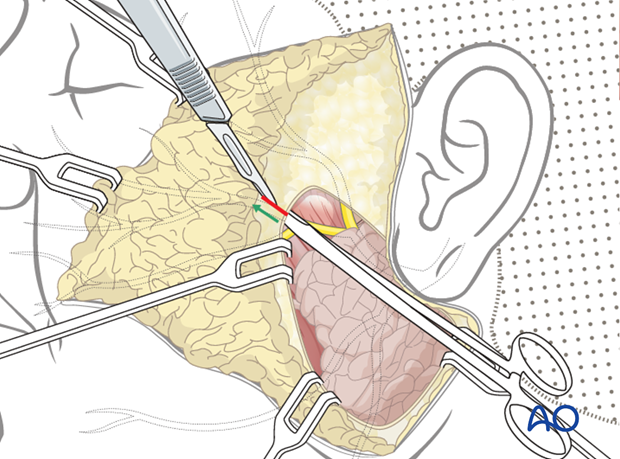
Nerve harvest
In order to get adequate length of graft to reach the opposite side of the face one would require harvesting the sural nerve. Both sural nerves may need to be harvested, one for eye closure and one for smiling.
The nerves are harvested.

Nerve graft insertion
The nerve graft is inserted through a subcutaneous tunnel.
For smile reanimation, the tunnel runs under the nose or on the upper lip.
For eye closure the tunnel crosses over the nasal bridge or above the eye brows.
The tunnel can be created either using tendon instruments, long blunt curved hemostatic forceps, or dissecting scissors.
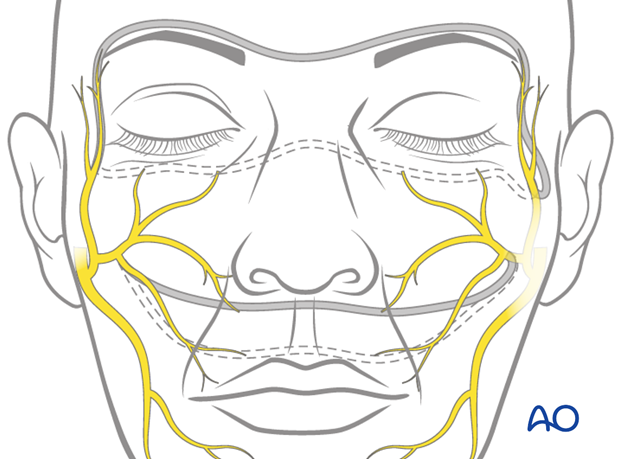
Nerve graft coaptation
Coaptation of nerve graft is performed to both the ipsilateral and contralateral facial nerves.
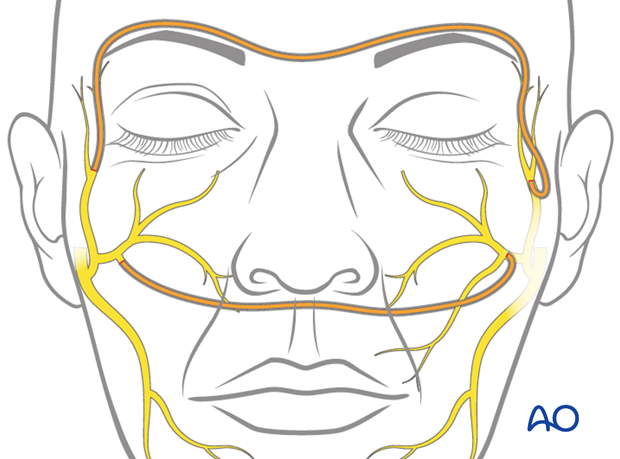
Static suspension may be used to augment reinnervation procedures, in order to improve facial symmetry at rest, especially during the period of facial nerve recovery.
Closure
The skin incisions are closed in layers.
3. Aftercare
Routine wound care is all that is necessary for the majority of the procedures.













