Screw fixation under general anesthesia
1. Principles
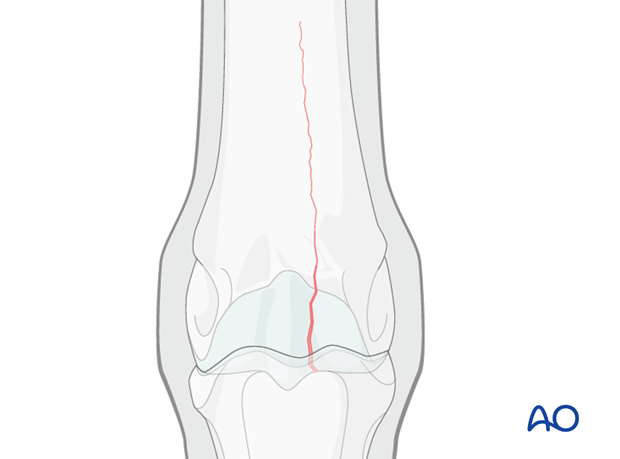
Compression of the articular surface
The major principle involved in lag screw fixation of these fractures is compression of the articular surface. The fixation of the distal portion of the bone may help prevent proximal propagation of the fracture, but definitely does not prevent it.
General anesthesia versus fixation in the standing horse
The decision to attempt lag screw fixation in the standing horse versus under general anesthesia will depend upon available recovery systems and the surgeon’s understanding of the risks involved. General anesthesia certainly allows superior aseptic technique, better radiographic control and more extensive arthroscopic evaluation of the joint. The significant advantage of attempting repair in the standing horse is minimizing the risk of catastrophic failure during anesthetic recovery.
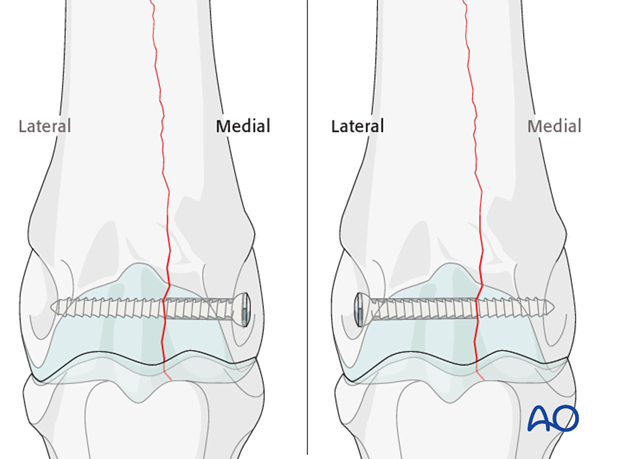
"Backward" fixation
Although the glide hole is typically drilled through the smaller fragment and the thread hole across the larger fragment, this particular fracture is often repaired in the opposite manner. The major reason is that it is much safer and easier to approach the leg from the lateral side than the medial side. Fortunately medial condylar fractures tend to be very close to the midline so there is little difference between the width of the two fragments. The bone in this location is so strong, that 25 mm of thread engaged with a 4.5 mm cortex screw is already exceeding the strength of the screw. Therefore, strong fixation can be achieved even though the repair is called “backwards”.
2. Approach
Positioning
Induction for general anesthesia should be carefully controlled using supporting head and tail ropes and/or a sling technique. This is particularly important with metatarsal fractures.
Most surgeons perform this repair with the horse in lateral recumbency. The affected limb can be up or down. If it is likely that diaphyseal screws will later be removed a lateral approach is preferred because the screws will be removed with the horse standing.
Stab incisions or open exposure
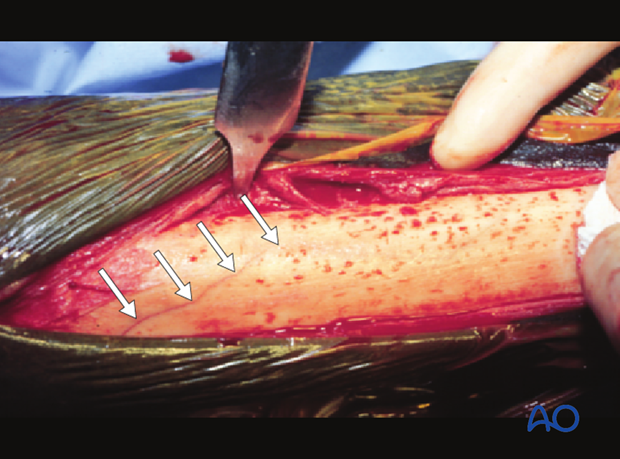
Screws can be placed through stab incisions or in combination with an open exposure of the fracture. This decision may be based on the quality of available imaging. For example, if intraoperative CT were available, open exposure to follow the fracture plane should be unnecessary. If the surgeon has any doubts about the configuration of the fracture, it is a simple matter to make an incision down to the dorsal surface of the third metacarpal/metatarsal bone to clearly see the fracture line.
Locating the site for screw insertion
The site of the first screw is the center of the epicondylar fossa. The location of the insertion in the fossa can be estimated by bisecting an imaginary line extending from the palmar/plantar wing of the proximal phalanx to the palpable dorsal edge of the condyle.
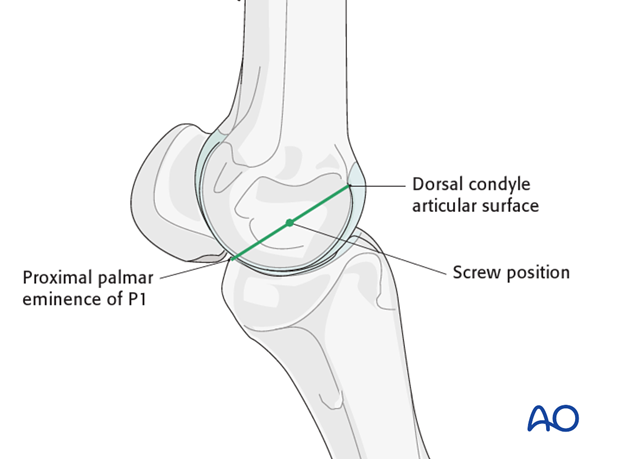
Needle placement
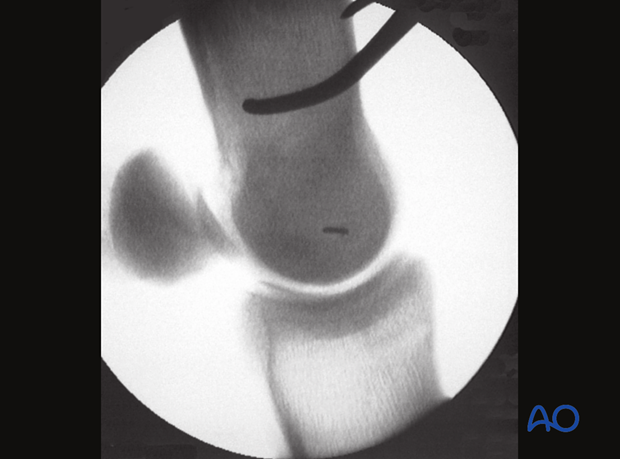
A needle should be placed at the selected site and with the help of a lateromedial radiographic/fluoroscopic view its correct location is verified. It is critical to remember that this view is the ONLY view that truly indicates the location for the incision/drill.
Note: The dorsopalmar/plantar view only provides information relative to the height of the needle but not whether is located in the center, at its edge or outside the fossa.
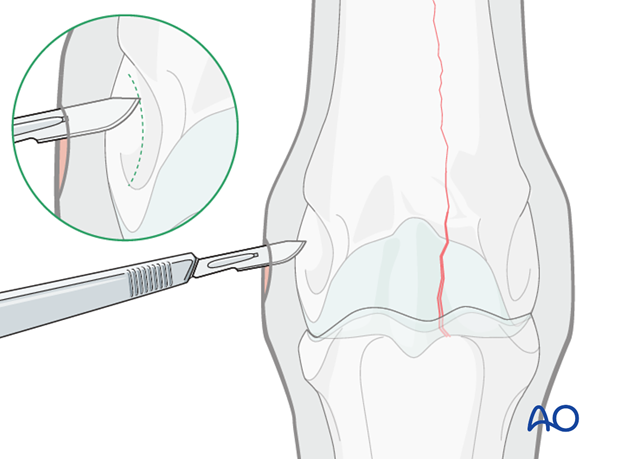
Incision
An incision is made with a #10 scalpel blade parallel to the fibers of the collateral ligament directly down to the bone surface. The epicondylar fossa is recognizable with the tip of the scalpel as it follows its contour.
3. Surgical technique
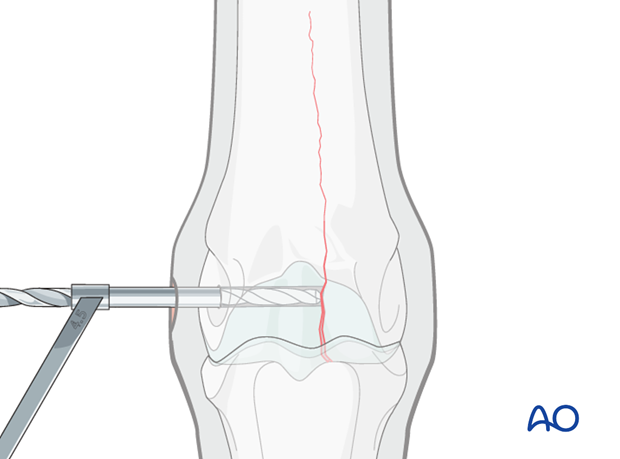
Preparation of the glide hole
In most cases, 4.5 mm cortex screws are used.
The glide hole must be drilled exactly to the fracture plane or just beyond it. It is absolutely essential in a non-displaced fracture, that the correct length and direction of the glide hole be verified with radiographs. Preoperative measurements on radiographs and careful measurements during drilling will help avoid any errors.
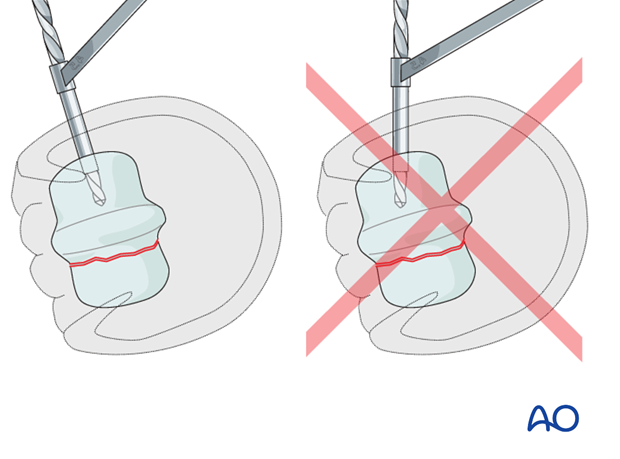
Pitfall: direction of the drill bit
The glide hole must be parallel to the distal joint surface and directed in a perfectly lateral to medial direction. It is critical for the surgeon to remember that a horse lying on its side tends to have its limb externally rotated. If the surgeon drills perpendicular to the floor, the drill bit will be directed in a palmar/plantar direction if the limb is uppermost. If the approach is medial (affected limb down) the tendency would be to drill too much towards the dorsal surface.
The 4.5 mm drill bit is removed, holding the drill guide in place. A 2.5 mm pin is placed through the drill guide into the glide hole.
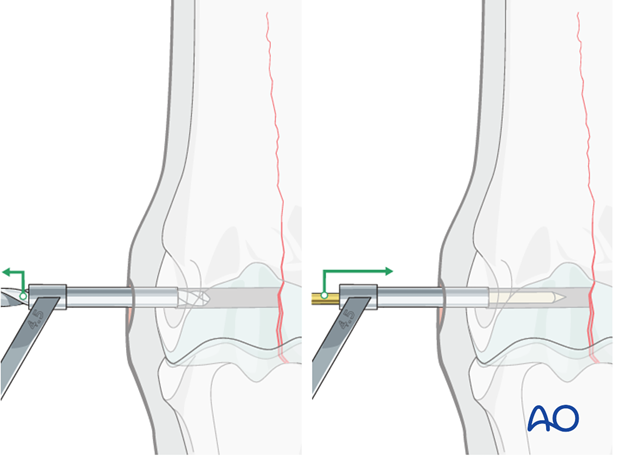
The 4.5 mm drill guide is removed and the 3.2 mm drill guide is slipped over the 2.5 mm pin into the glide hole.
The pin is removed.
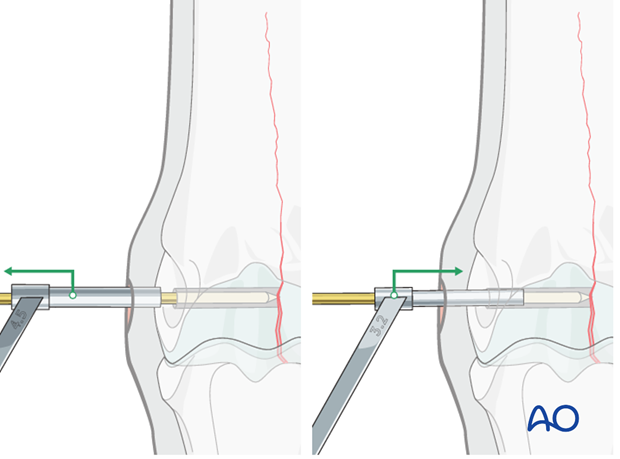
Ideally, one should check the positioning of the glide hole by taking a lateromedial radiographic view with the drill guide in place. If the hole in the drill guide is clearly visible and the proximal sesamoid bones are superimposed, the surgeon can be very confident that the screw will be properly directed across the condyle.
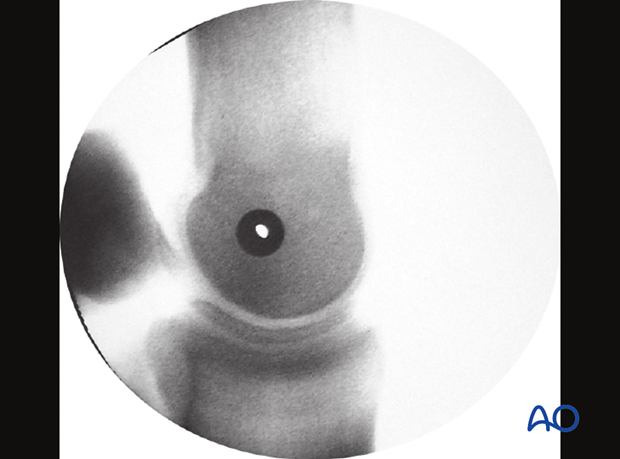
Preparation of the thread hole
The 3.2 mm drill bit is inserted into the corresponding drill guide and the thread hole is prepared across the remainder of the bone. The drill bit should be removed and cleaned frequently because this is very dense bone.
Caution should be used when approaching the far cortex to minimize damage and debris as the drill bit exits the bone.
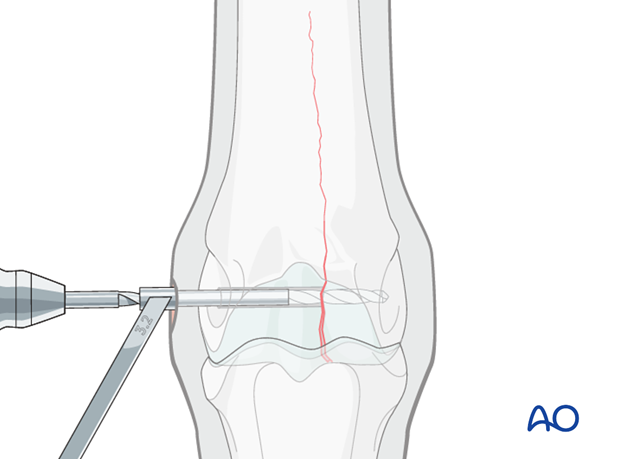
The 3.2 mm bit is removed and the 2.5 mm pin re-inserted. This pin is valuable to minimize any difficulties finding the hole through the stab incision.
Tapping the hole
No countersink depression is prepared because the screw head comes to lie in the epicondylar fossa. Countersinking may add additional trauma to the collateral ligament.
Note: Some surgeons nevertheless prefer to prepare a countersink depression.
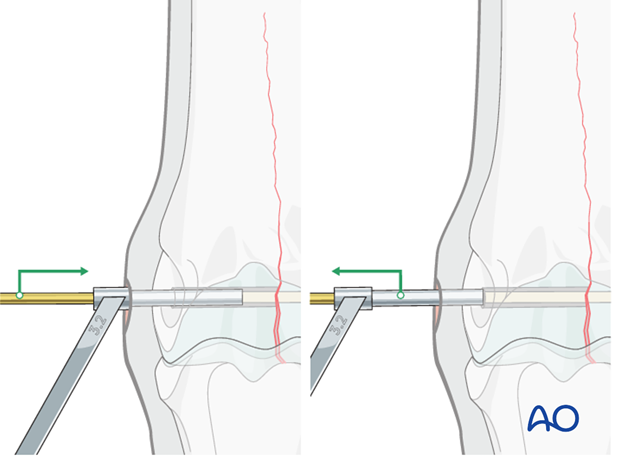
The 4.5 mm drill guide is subsequently placed over the 2.5 mm pin (A). The pin is removed (B)...
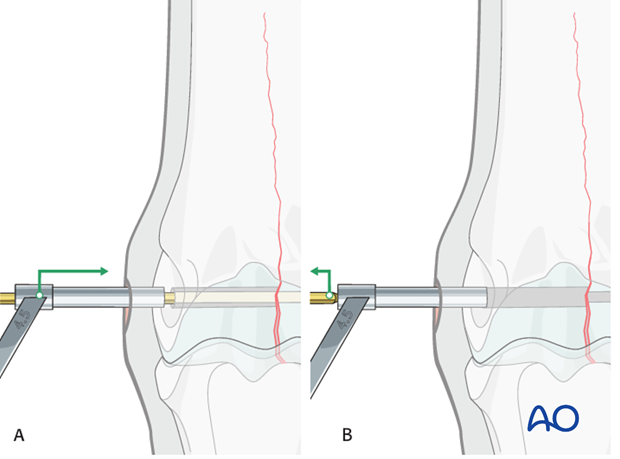
... and the 4.5 mm tap inserted through the guide (C).
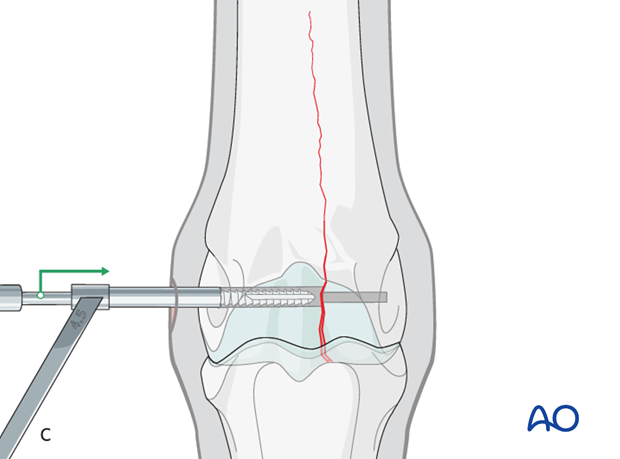
The hole is tapped routinely, keeping the very dense bone in mind. It is critical to tap completely through the far cortex (red circle). The bone is so dense that even a single millimeter of untapped bone may prevent complete insertion and tightening of the screw.
A long tap is strongly preferred to avoid impinging the end of the drill on the edge of the drill guide (yellow circle). This could result in stripping the threads in the hole or breaking the tap.
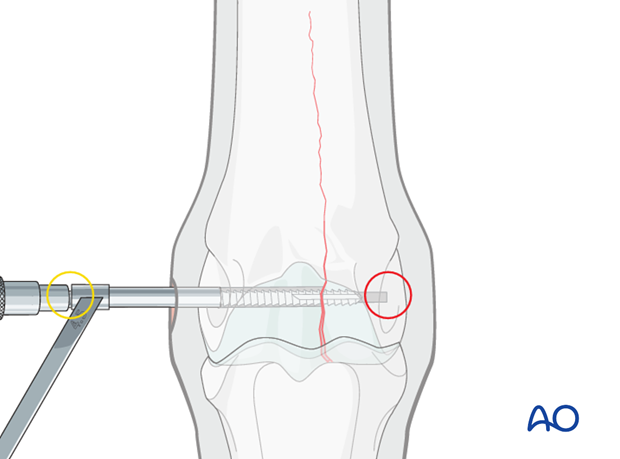
Screw insertion
In most horses, measurement of the hole is not performed in this location. Most race horses accommodate a 52 mm cortex screw distally.
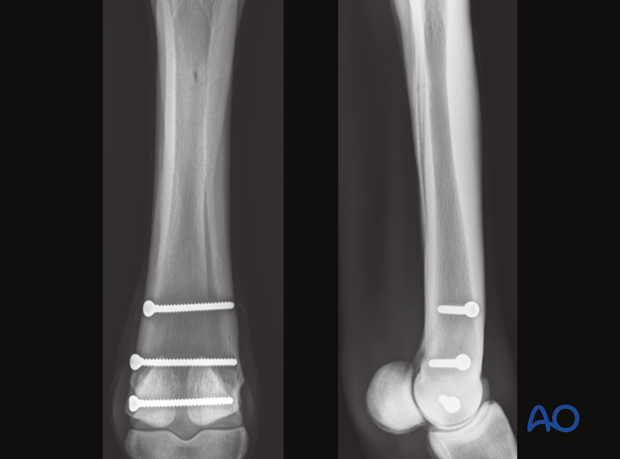
The screw is inserted and fully tightened.
Either a fluoroscopic or radiographic DP view is taken to verify correct the screw length.
Arthroscopic supervision of screw tightening is optional in these fractures as they are incomplete and correct articular alignment is guaranteed.
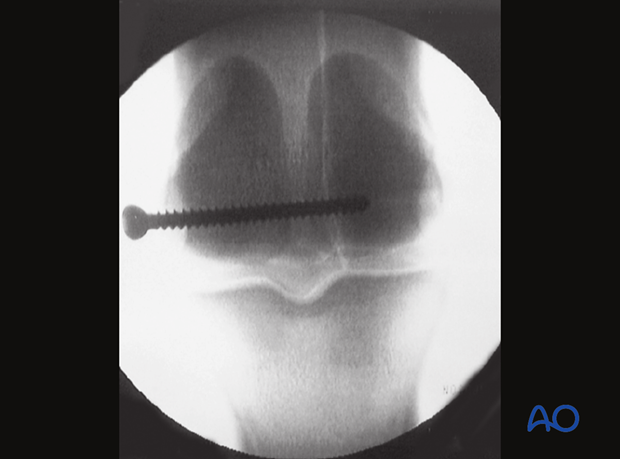
A second screw is placed approximately 2 cm proximal to the first screw.
Note: In this location a countersink depression is created to properly seat the screw head. Countersinking should only be deep enough to prevent screw bending. The goal is NOT to bury the screw head. That will make it more difficult to remove the screw and potentially weaken the bone.
It may be helpful to leave the power screw driver attachment in the head of the first screw to assist alignment.
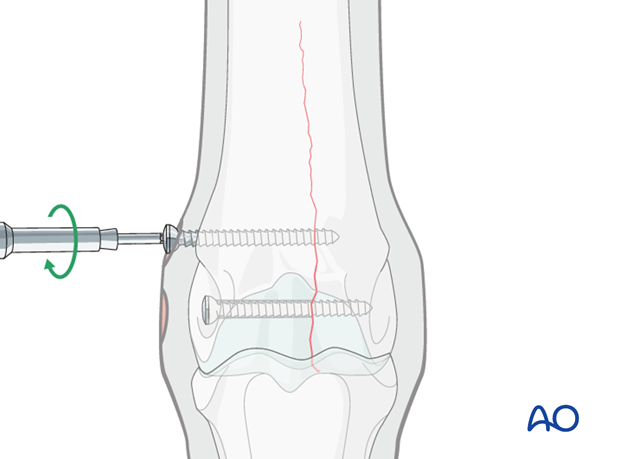
Additional screws are added according to the radiographically visible length of the fracture or what can be seen with the open exposure of the bone. A countersink depression is created for every screw head.
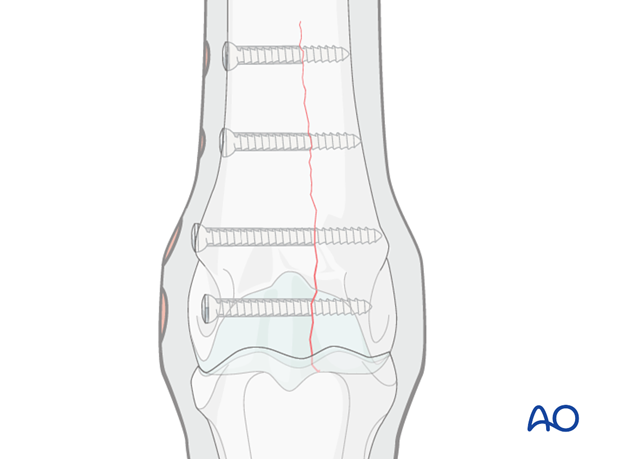
NEVER place a screw where you cannot clearly see the fracture line.
4. Recovery from anesthesia
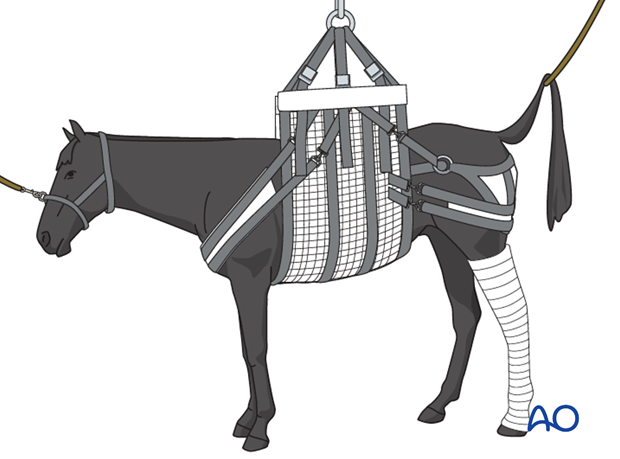
These are very high risk cases for recovery, especially in horses with hind limb fractures. Ideally, special recovery systems should be used such as a sling…
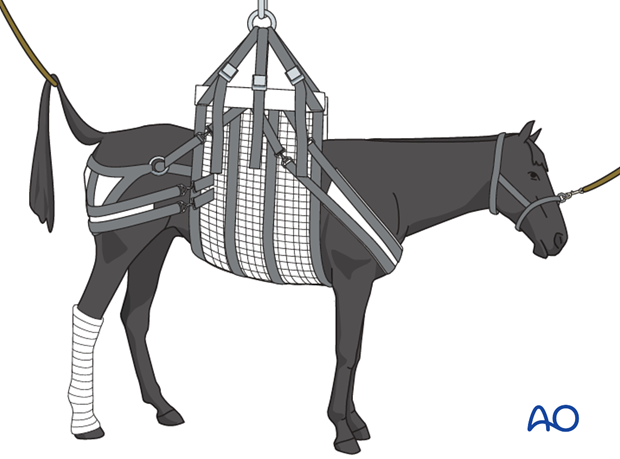
…or a pool. If none of these are available a full-limb cast should be applied during recovery. Half-limb casts do not fully protect horses from catastrophic failure through the diaphysis.

5. Aftertreatment
Horses are usually kept under stall rest and hand-grazing only for at least 60 days followed by hand walking or machine walking exercise for an additional 60 days before allowing turnout in a very small paddock. Most horses get about a minimum of 6 months before returning to training.
Intra-articular medications depend on surgeons preference and the degree of articular damage seen during surgery.

Imaging
Follow up radiographs are usually taken 90 days postoperatively and again before returning to training.
Implant removal
Screw removal is generally recommended only if the screws extend up into the diaphysis.
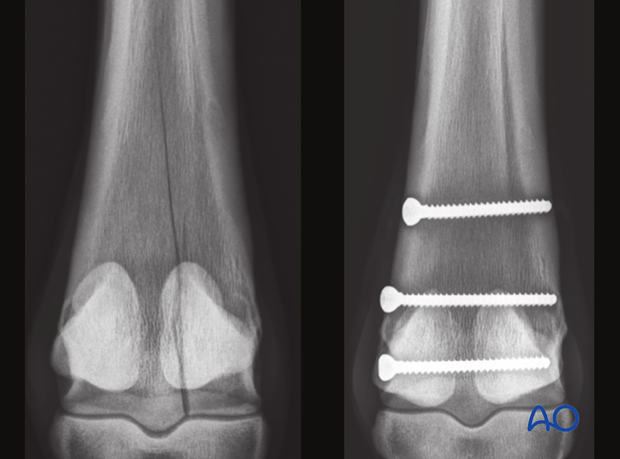
Prognosis
The prognosis for medial condylar fractures is generally very good if catastrophic complications can be avoided. Medial fractures tend to have less preexisting joint pathology than lateral condylar fractures.













