Plate fixation
1. Principles
Compression of the articular surface
The major principle involved in lag screw fixation of these fractures is compression of the articular surface. Lag screw fixation of the distal portion of the bone may help prevent proximal propagation of the fracture, but definitely does not prevent it. A plate that is securely attached along the rest of the bone effectively helps to prevent catastrophic failure.
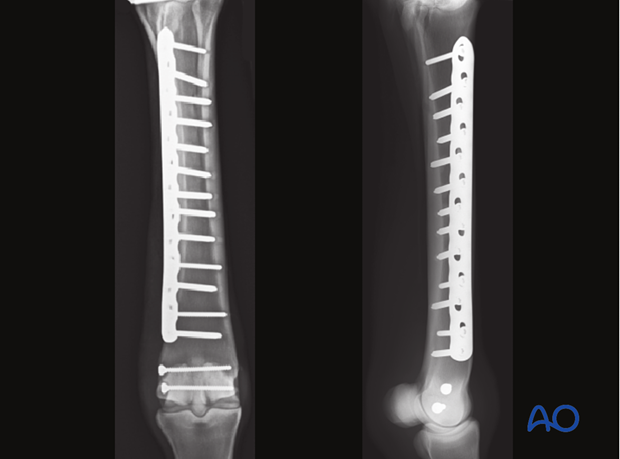
"Backward" fixation
Although the glide hole is typically drilled through the smaller fragment and the thread hole across the larger fragment, this particular fracture is often repaired in the opposite manner. The major reason is that it is much safer and easier to approach the leg from the lateral side than the medial side during implant removal, which is routinely performed in the standing position. Fortunately medial condylar fractures tend to be very close to the midline so there is little difference between the width of the two fragments. The bone in this location is so strong, that 25 mm of thread engaged with a 4.5 mm cortex screw is already exceeding the strength of the screw. Therefore, strong fixation can be achieved even though the repair is called “backwards”.
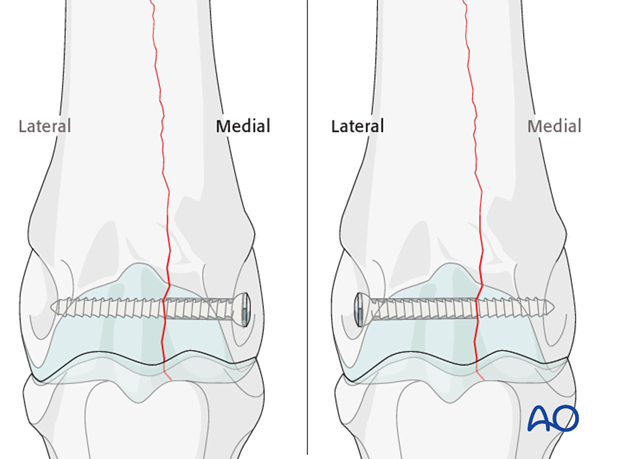
Positioning
Induction for general anesthesia should be carefully controlled using supporting ropes and/or sling technique. This is particularly important with metatarsal fractures.
The horse is placed in lateral recumbency. The affected limb should be uppermost. Horses that are supposed to return to race will need the plate removed and standing plate removal is much easier when the plate is on the lateral aspect of the bone.
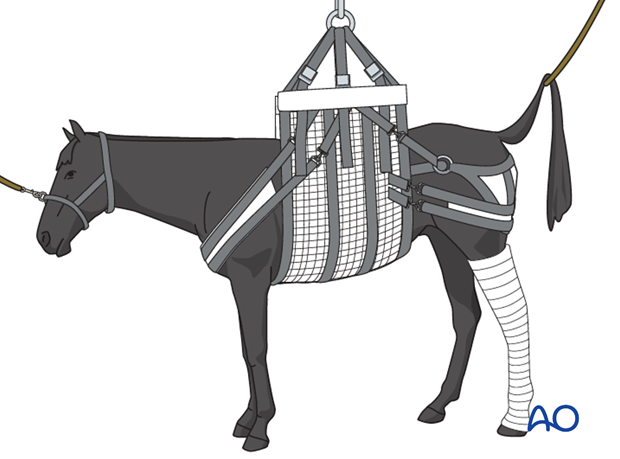
2. Insertion of interfragmentary screws
The distal two screws across the condyle are placed routinely through stab incisions under fluoroscopic or radiographic control. It is also desirable to examine the joint arthroscopically to confirm fracture reduction, evaluate joint surfaces and remove any loose fragments. For a detailed description see Medial incomplete condylar fractures - Lag screw fixation.
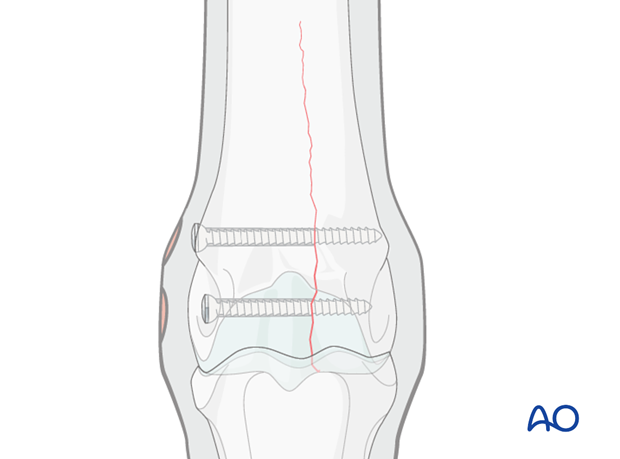
3. Approach
Dorsolateral approach
If the fracture is repaired through an open exposure, a dorsolateral approach is indicated.
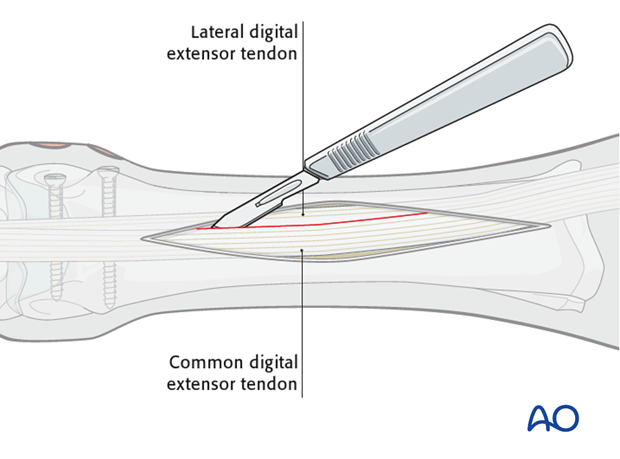
The dorsal fracture line is exposed with a periosteal elevator just enough to follow its proximal extent.
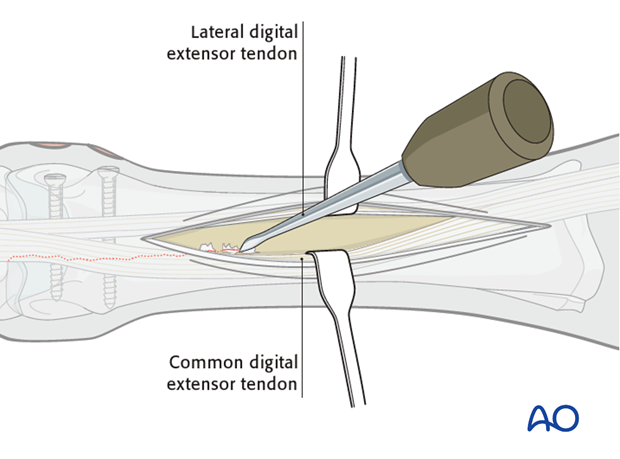
4. Plate preparation and application
Plate selection and preparation
A plate of appropriate dimensions is selected. In metacarpal fractures, a 10-11 hole broad 4.5 mm plate is usually used and in metatarsal fractures, a 12-13 hole plate is used in an average sized race horse. Although, traditional plates can be used successfully, locking compression plates (LCPs) are probably superior.
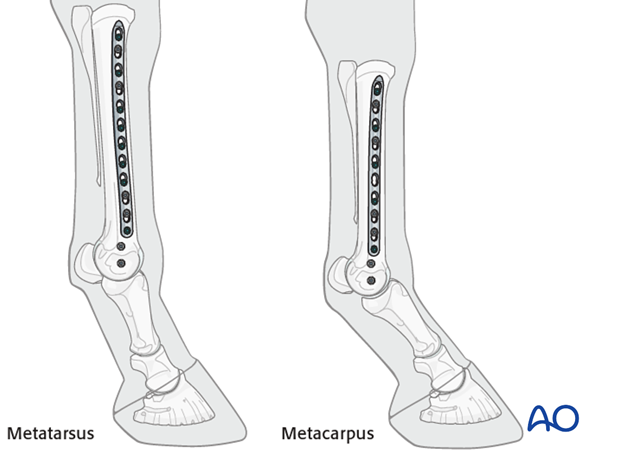
Using an aluminum template contoured to the dorsolateral surface of the bone the selected plate is prepared with a large bending press. If a traditional plate is used, the precision of the contouring is very important. The most common error is having the plate too far from the surface of the bone at its ends.
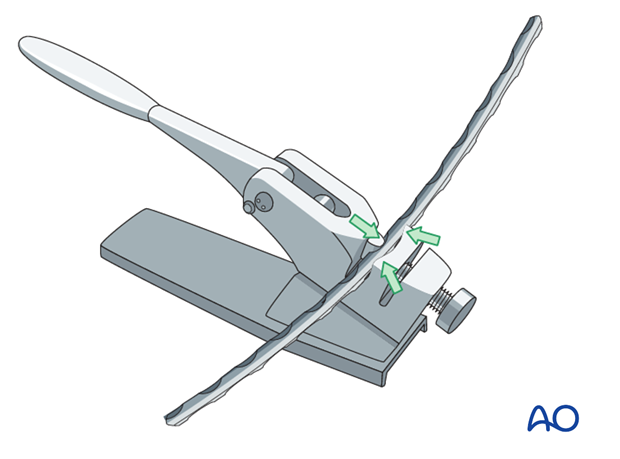
Insertion of a distal screw
The plate is held in position with fingers, a clamp or the push-pull device and one of the two most distal holes in the plate is used for placement of a 4.5 mm cortex screw in lag fashion. This presumes that the fracture plane is still visible at this level of the bone.
This distal screw may be inserted directly if exposure is adequate, but can also be inserted through stab incisions if the surgeon prefers not to retract the flap.
When this screw is tightened, the fracture is further compressed and the plate is pulled against the surface of the bone.
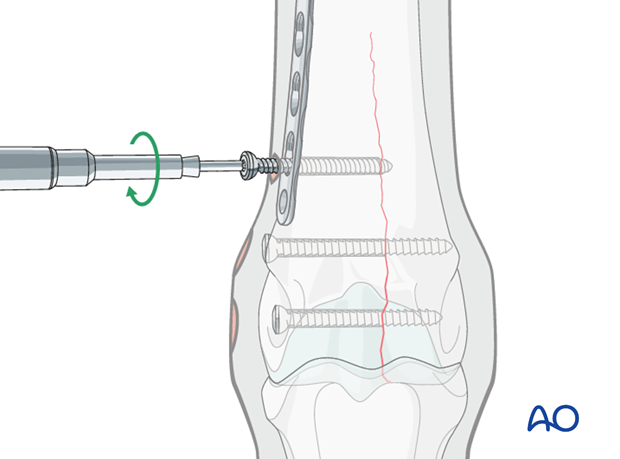
Pitfall: plate placement
Before drilling the second screw hole, the surgeon must be certain that the entire length of the plate is in the desired location. Once the second screw is placed, the longitudinal alignment of the plate cannot easily be changed. The only other option is twisting the plate and that takes additional time.
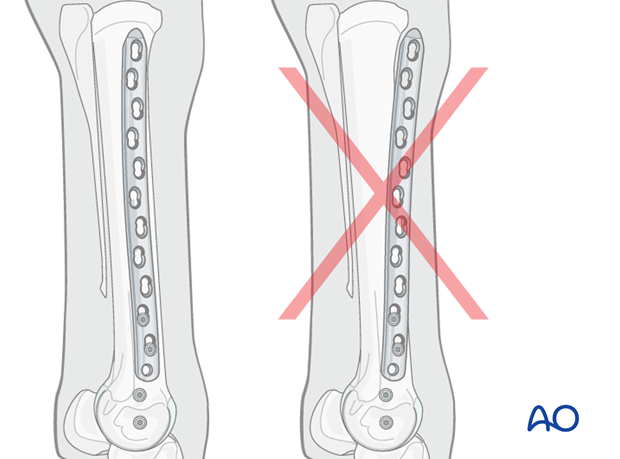
Insertion of cortex screws
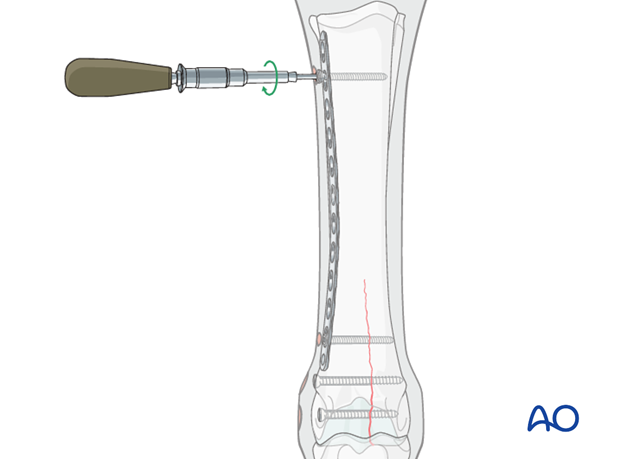
At least one additional cortex screw is placed through the proximal aspect of the plate to pull it down against the bone. Often, about 50% of the holes in the plate are filled with cortex screws, because they are less expensive than locking head screws. It is essential, that all cortex screws be placed and tightened before the first locking head screw is inserted.
4.5 mm cortex screws are easier to place through the plate holes and generally strong enough, but 5.5 mm cortex screws may be used, especially in larger horses.
Pitfall: drilling into the splint bone
Because the plate is positioned slightly dorsally on the lateral side, the drill path for all screws through the plate is towards the contralateral splint bone. A surgeon should be cautious to avoid unnecessary injury to that structure.
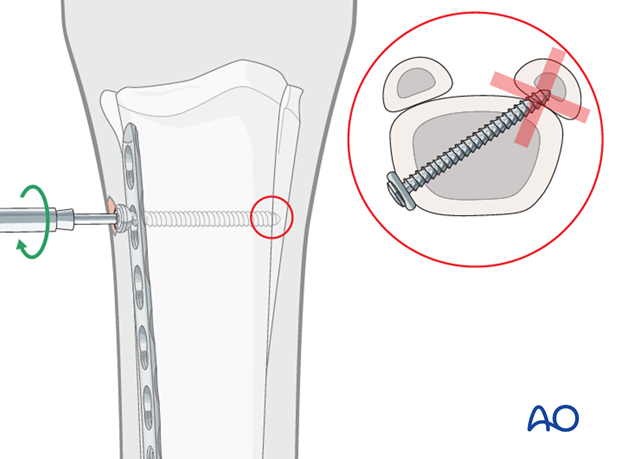
Insertion of locking head screws
The remaining screw holes are filled with appropriate length 5.0 mm locking head screws.
The guides must be carefully inserted so that the drill holes are perfectly perpendicularly aligned and the screws tightened properly into the plate.
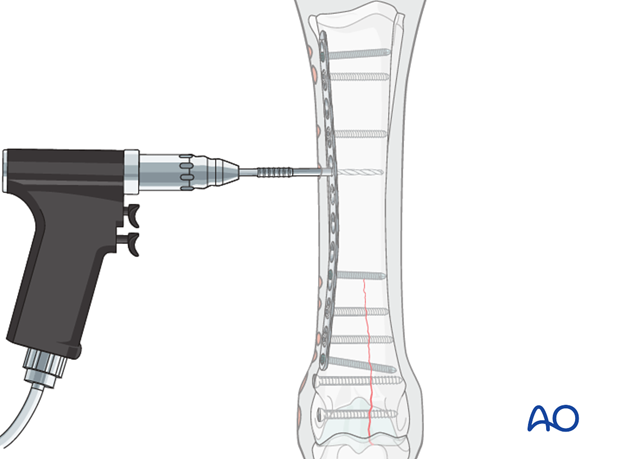
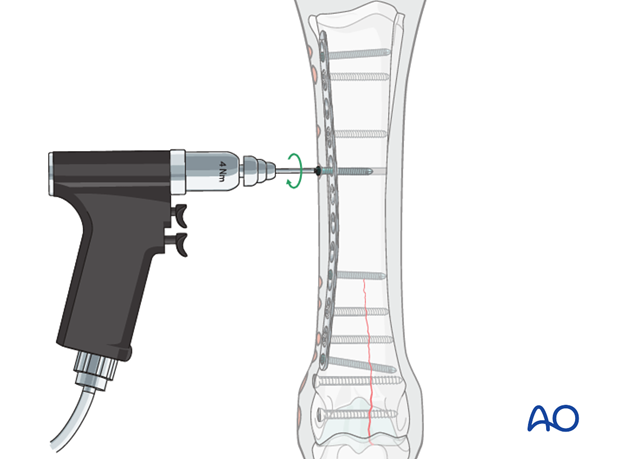
Locking head screws are inserted using the torque limiting adapter followed by complete tightening by hand. When using stainless steel implants in horses it is common to far exceed the 4Nm torque. The function of the plate is dependent on the screw head being tightly locked so be absolutely certain that it is as tight as possible. With stainless steel, the clinical experience has been that the screws can later be removed without difficulty.
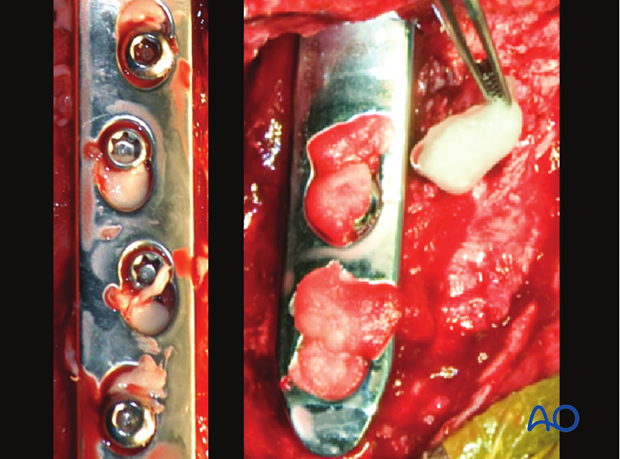
If desired, antibiotic impregnated polymethylmethacrylate (left) or pieces of a collagen sponge (right) can be placed in any voids in the plate.
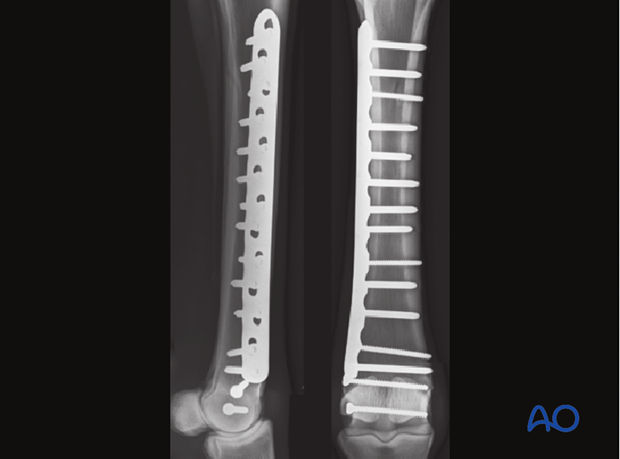
Radiographic confirmation
All screws are double-checked for complete tightness.
Wound closure is described in the approach section.
5. Alternative: minimally invasive plate fixation
Principles
Locking plate technology affords the opportunity to use minimally invasive plate fixation for these fractures. The advantages of so called “biological fixation” include minimal disruption of cellular elements at the fracture site, minimal interference with blood supply and no damage to the periosteum. It is possible that minimally invasive plate fixation could also lessen likelihood of implant infection and speed the surgical procedure.
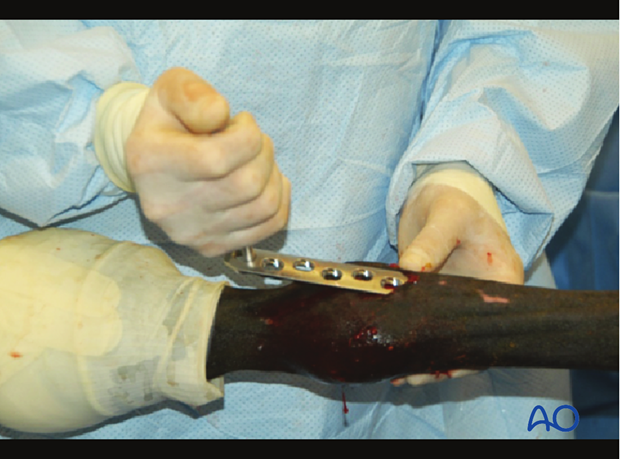
An old plate with a sharpened end attached to a handle or some similar device is necessary to create a subcutaneous, extraperiosteal tunnel in which the locking plate will be placed.

Plate preparation
The large bending press is used to roughly contour the selected plate to the dorsolateral aspect of the bone seen on the DMPLO radiograph. If a traditional (non-locking) plate is used, the precision of the contouring is very important.
The most common error made when contouring plates is having the plate too far from the surface of the bone at its ends.

Preparation of the periosteal tunnel
A 2 cm incision is made at one end of the proposed location of the plate and the plate passing device forced through the subcutaneous tissues along the bone in the correct location. The plate passer is superficial to the periosteum.
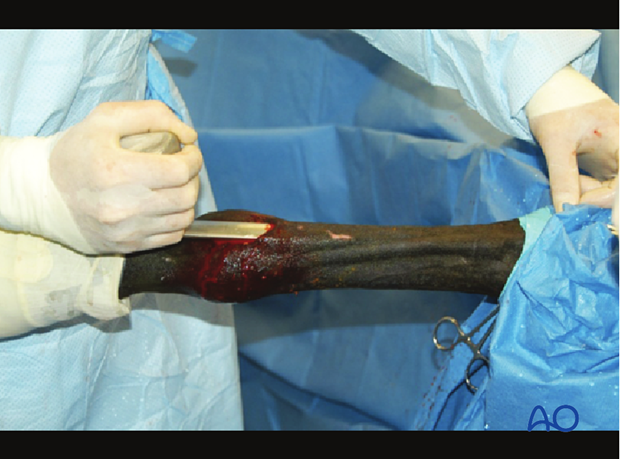
Plate insertion
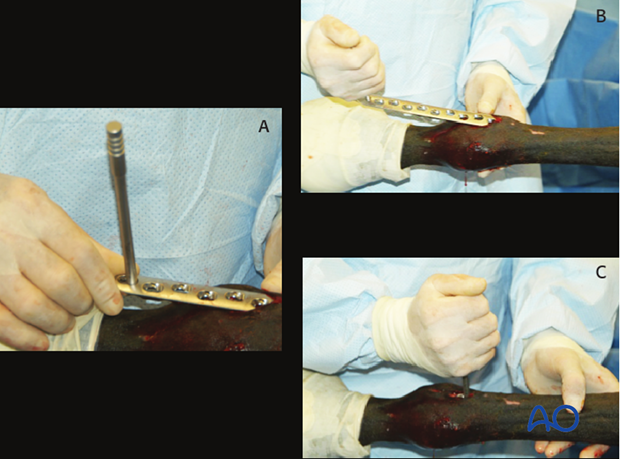
The plate holding device (A) is screwed into the locking plate and used as a handle to slide the plate into position (B,C).
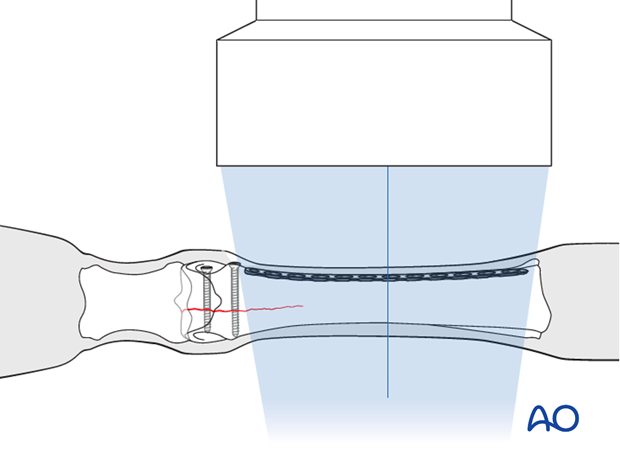
Intraoperative fluoroscopy or digital radiography is used to check the position of the plate relative to the bone and the previously placed distal screws. If the plate does not appear to match the bone surface adequately, it should be removed and re-contoured with the large bending press.
After reinsertion the position is checked again.
Screw insertion
As with an open exposure, approximately three cortex screws (one at the proximal and distal end of the plate and one in its center) are placed to pull the plate against the bone. The distal cortex screws in the plate can be placed in lag fashion if the fracture configuration allows it. The remainder of the technique is identical to that described above using locking head screws, except that one is working through small incisions over each hole in the plate. The stab incisions must be large enough to allow secure insertion of locking guides into the plate.
6. Recovery from anesthesia
These are very high risk cases for recovery, especially in horses with hind limb fractures. Ideally, special recovery systems should be used such as a sling…
…or a pool. If none of these are available a full-limb cast should be applied during recovery. Half-limb casts do not fully protect horses from catastrophic failure through the diaphysis.

7. Implant removal
Preparation
Plate removal is performed about 3 months postoperatively and should be done with the horse standing under sedation and local anesthesia.
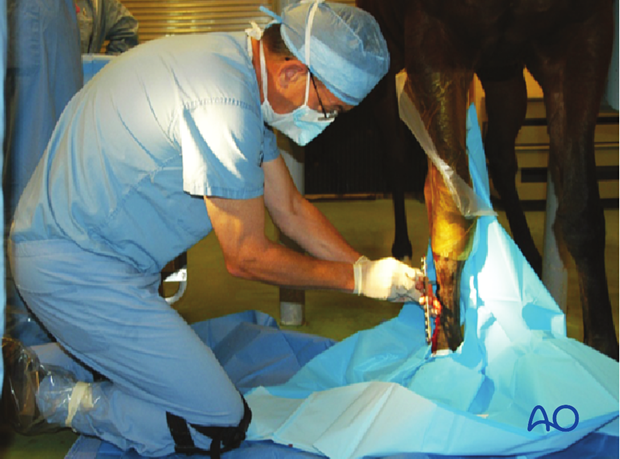
Plate removal
It is usually possible to feel some of the screw heads in the plate through the skin. An incision is made directly over the screw head and the screw is backed out until its head protrudes above skin level. Do NOT remove the screw completely.
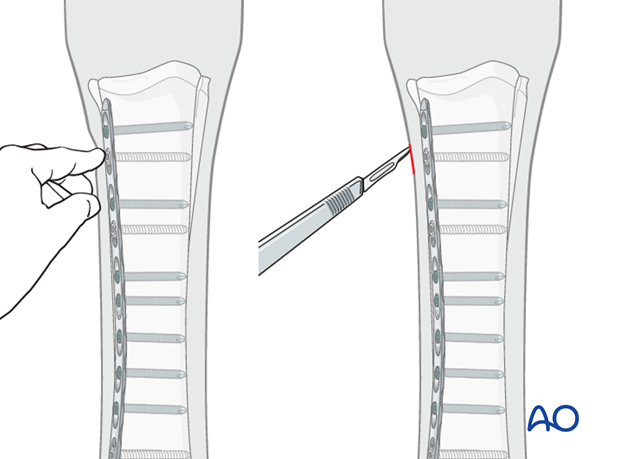
It is very helpful to have a sterile plate matching the one in the horse available. Once two screws in the implant have been identified the matching plate can be laid over the skin and used as a template to make individual stab incisions over each screw head.
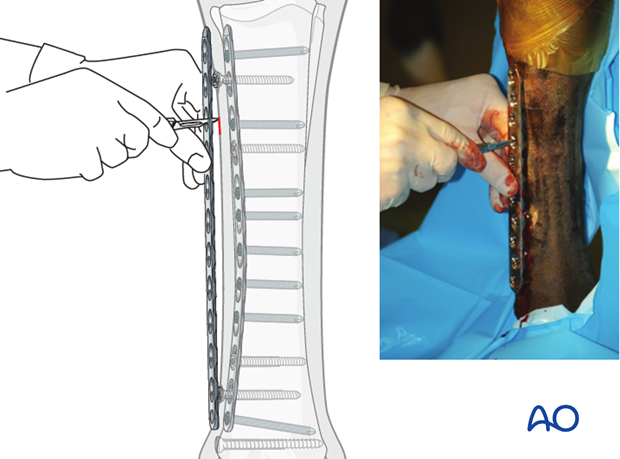
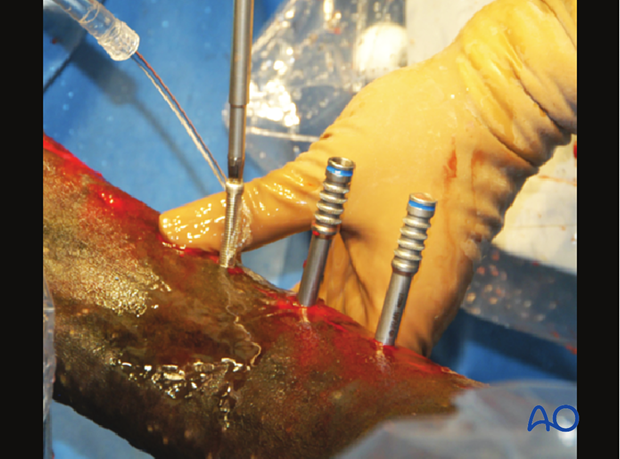
Individually remove all screws just to skin level. The surgeon should be sure to fully insert the screw driver into the screw head recess, especially in hexagonal heads to avoid stripping. Screw drivers containing the star drive configuration are less prone to stripping, which is a major advantage.
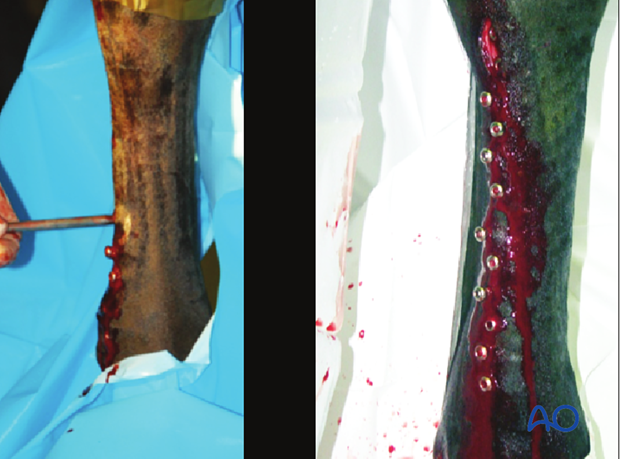
The exposed screw heads must be counted to be absolutely certain that the number matches the screws visible on the radiographs! All screws are then removed.
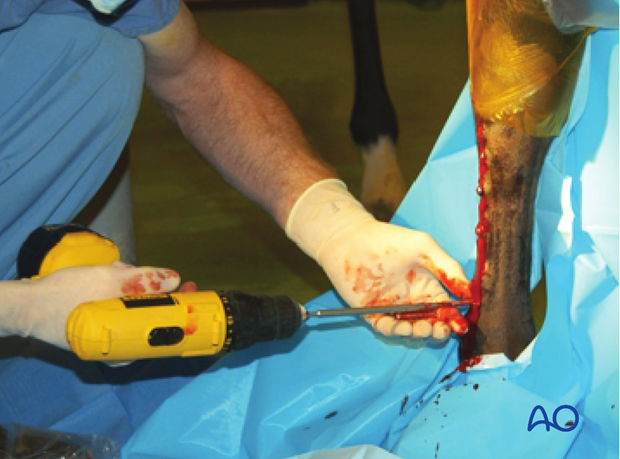
The plate is loosened by using a carpenter’s nail set on the edge of a screw hole and striking with a mallet.
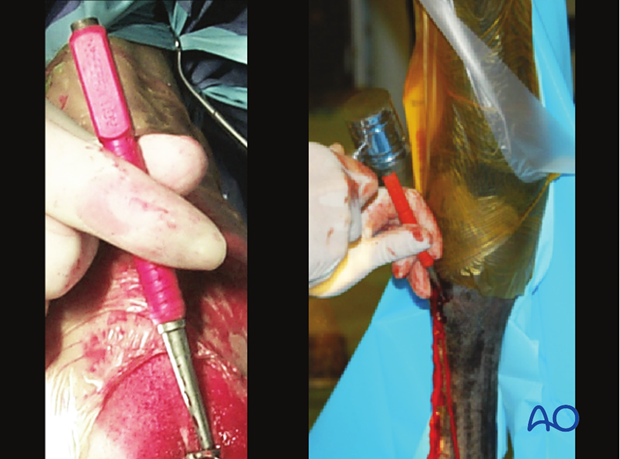
If necessary, the incision is enlarged at the proximal end of the plate. A 12 mm osteotome is used to pry the proximal end of the plate away from the bone. The plate is grasped with sterile locking pliers and pulled upward. If the plate is not easily removed, an osteotome is placed between the bone and the plate and with the help of the nail set and a mallet the plate is driven proximally. The osteotome placed between the plate and the bone acts as an inclined plane to ease removal.
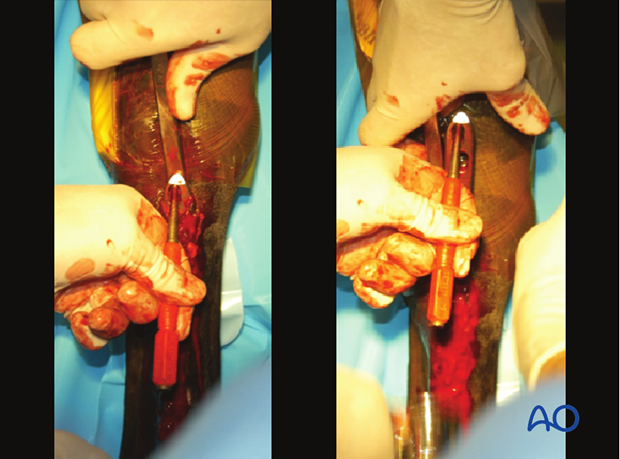
Closure
All incisions are closed with simple interrupted skin sutures and a padded bandage applied. The distal two screws that were inserted before plate application are left in place.
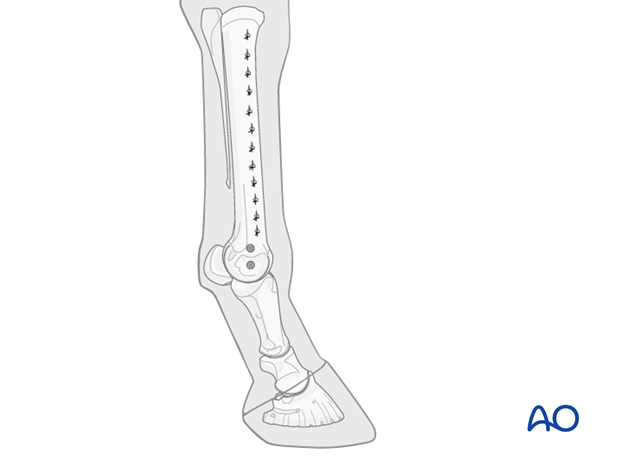
Radiographic confirmation
Documenting radiographs are obtained.
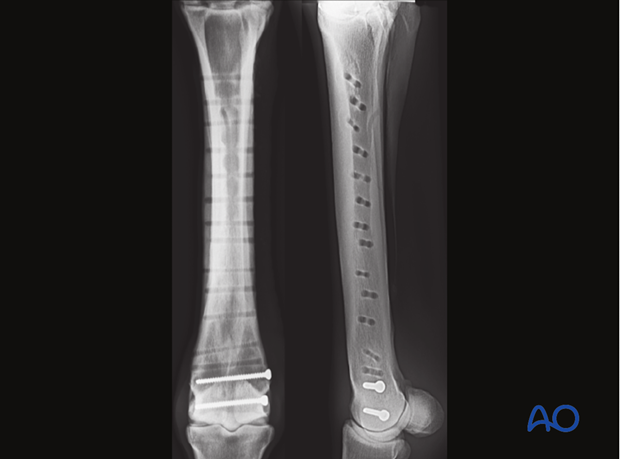
Aftercare
Horses receive stall rest and hand walking for 30 days followed by paddock exercise for at least another 30 days before returning to any type of training. A final set of radiographs is advised before work at high speed begins.

8. Aftertreatment
Horses are usually kept under stall rest and hand-grazing only for at least 60 days followed by hand walking or machine walking exercise for an additional 30 days before removing the plate. The two distal screws are usually left in the bone.

Prognosis
The prognosis for medial condylar fractures is generally very good if catastrophic complications can be avoided. Medial fractures tend to have less preexisting joint pathology than lateral condylar fractures.













