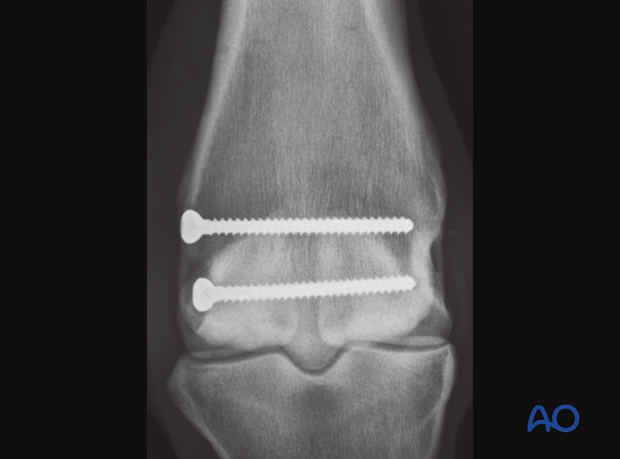
Screw fixation
1. Principles
Joint reconstruction
The overriding principle is perfect reconstruction of the metacarpo/metatarsophalangeal joint surface. This high-motion joint is of extreme importance in a race horse and even minor incongruities can be debilitating.
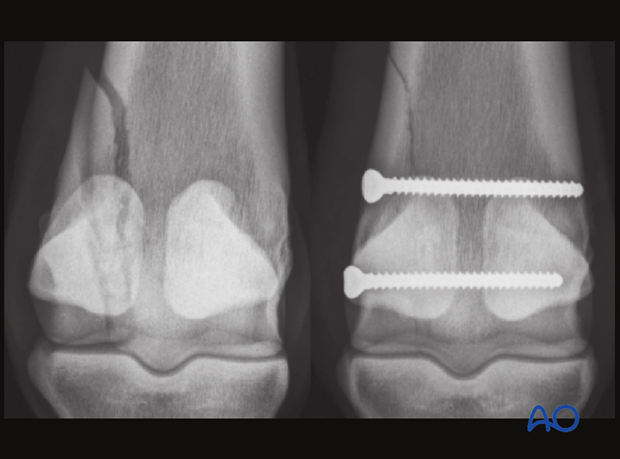
Further considerations
Other principles involved in the surgery are to remove unstable fragments and to appropriately treat accessible cartilage lesions.
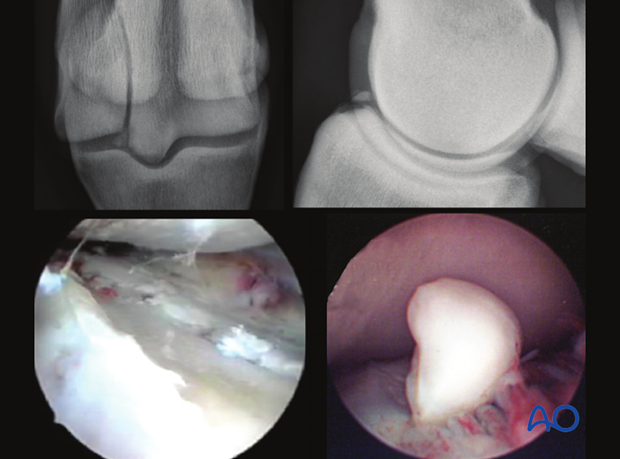
AO Teaching videos
Lateral condylar fracture of MCIII, fixation with 4.5mm cortex lag screws III
2. Patient positioning
This procedure is performed with the patient placed either in dorsal recumbency or lateral recumbency.

3. Preparation of the stab incision
Location of the insertion
The site of the first screw is the center of the epicondylar fossa. The location of the insertion in the fossa can be estimated by bisecting an imaginary line extending from the palmar/plantar wing of the proximal phalanx to the palpable dorsal edge of the lateral condyle.
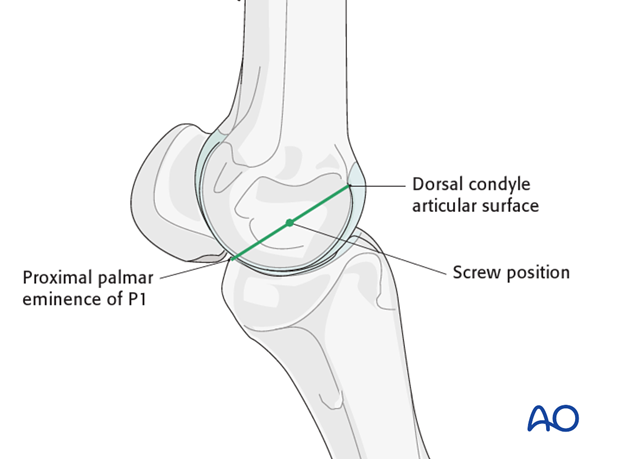
Needle placement
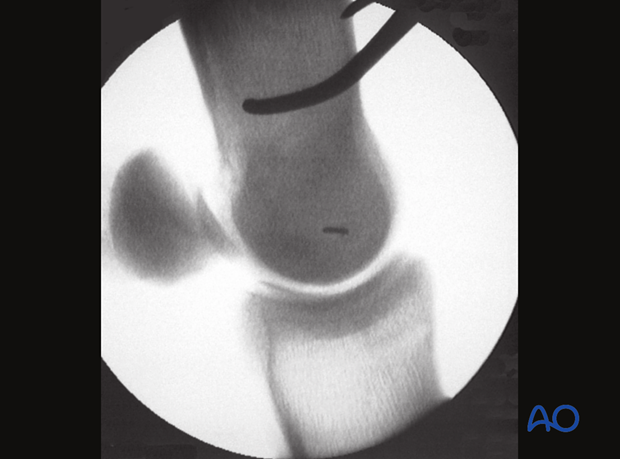
A needle should be placed at the selected site and with the help of a lateromedial radiographic/fluoroscopic view its correct location is verified. It is critical to remember that this view is the ONLY view that truly indicates the location for the incision/drill.
Note: The dorsopalmar/plantar view only provides information relative to the height of the needle but not whether is located in the center, at its edge or outside the fossa.
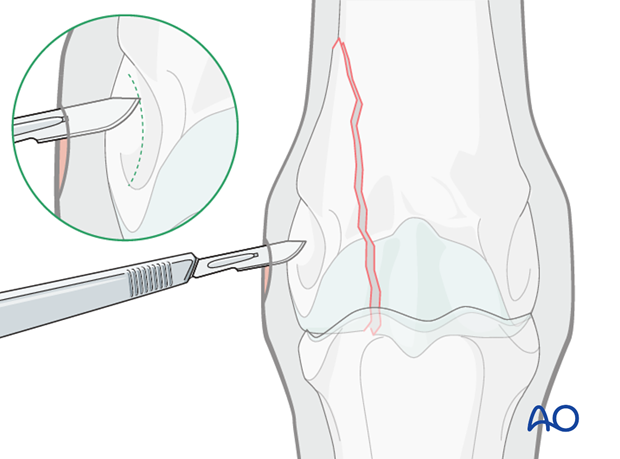
Incision
An incision is made with a #10 scalpel blade parallel to the fibers of the collateral ligament directly down to the bone surface. The epicondylar fossa is recognizable with the tip of the scalpel as it follows its contour.
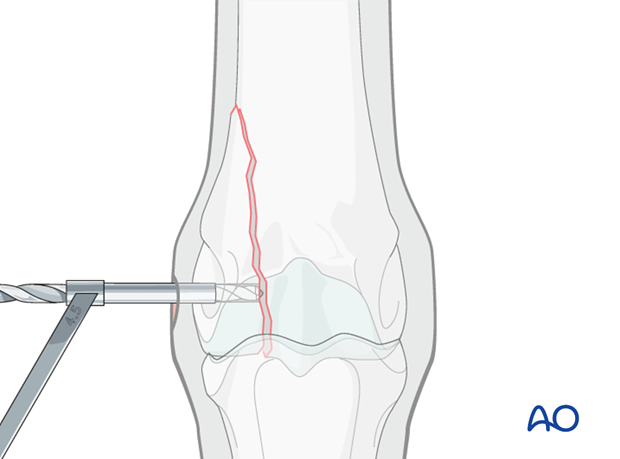
4. Creation of the glide hole
In most cases, 4.5 mm cortex screws are used.
The 4.5 mm glide hole is created without reduction of the fracture. This allows the surgeon to easily feel the drill bit entering the fracture plane, assuring that the glide hole is of the correct length.
Nonetheless, radiographic verification (DP view) of the glide hole position and length is strongly advised.
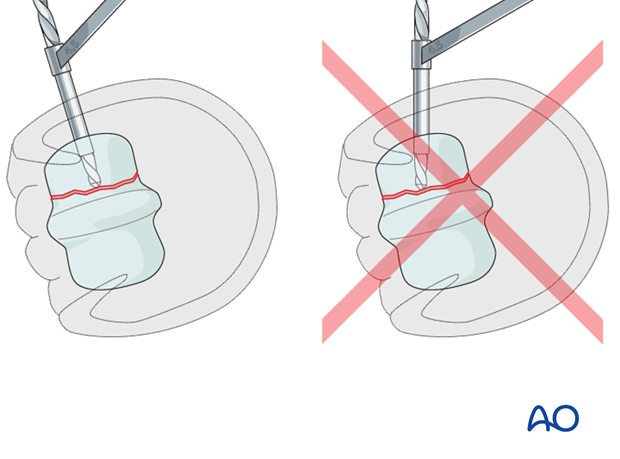
Pitfall: direction of the drill bit
The glide hole must be parallel to the distal joint surface and directed in a perfectly lateral to medial direction. It is critical for the surgeon to remember that a horse lying on its side tends to have its lower limb externally rotated. If the surgeon drills perpendicular to the floor, the drill bit will be directed in a palmar/plantar direction.
When the fracture plane is entered with the 4.5 mm drill bit, blood tinged synovial fluid may exit the hole.
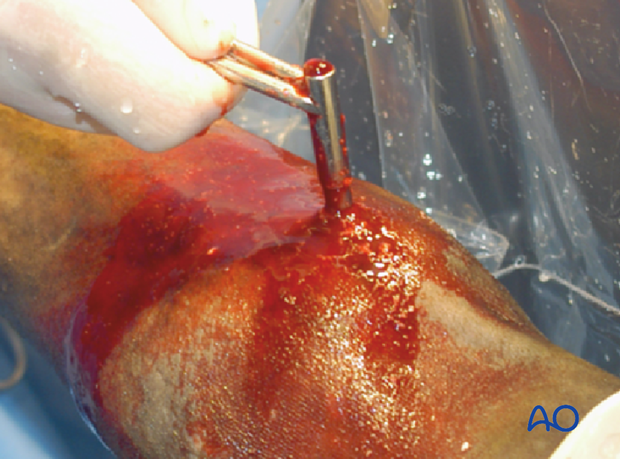
The 4.5 mm drill bit is removed, holding the drill guide in place. A 2.5 mm pin is placed through the guide into the glide hole. Maintaining a smooth pin in the hole while the drill guides are changed keeps the surgeon from temporarily “losing” the hole.
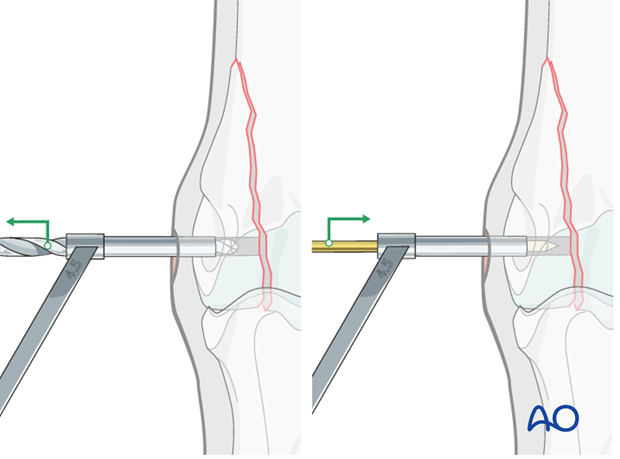
The 4.5 mm drill guide is removed and the 3.2 mm drill guide is slipped over the 2.5 mm pin into the glide hole. The pin is removed.
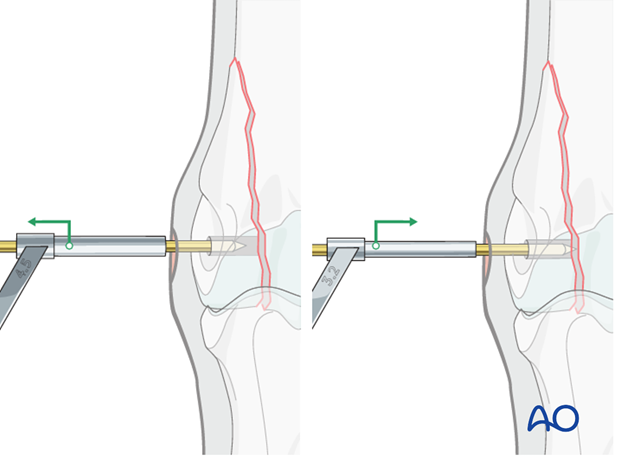
Radiographic confirmation
Ideally, one should check the direction of the glide hole by taking a lateromedial radiographic view with the 3.2 mm drill guide in place.
If the hole in the drill guide is clearly visible and the proximal sesamoid bones are superimposed, the surgeon can be very confident that the screw will be properly directed across the condyle.
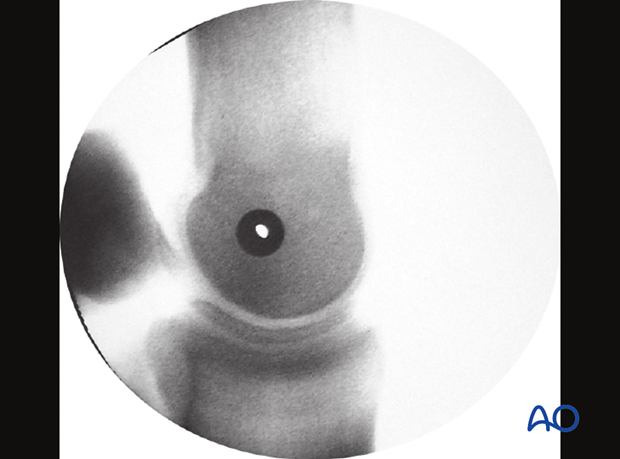
5. Reduction
Insertion of the arthroscope
The arthroscope is inserted into the proximal dorsolateral aspect of the joint using routine technique.
When assessing reduction, it is important to look over as much of the length of the fracture line as possible. This is made easier by placing the arthroscope proximally in the dorsal pouch.
The smooth pin can be re-inserted to provide leverage for manipulation of the fragment.
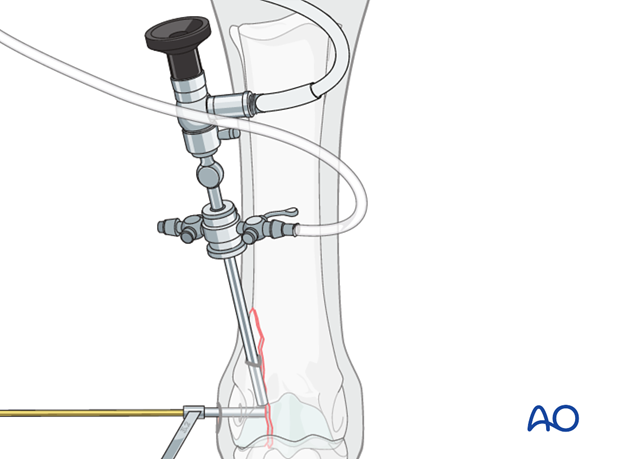
Using the 3.2 mm drill guide and pin to help manipulate the lateral fragment, the fracture is accurately reduced under arthroscopic observation. The metacarpo/metatarsophalangeal joint usually needs to be manipulated simultaneously to obtain perfect reduction.
Both flexion and extension as well as varus and valgus forces may be necessary.
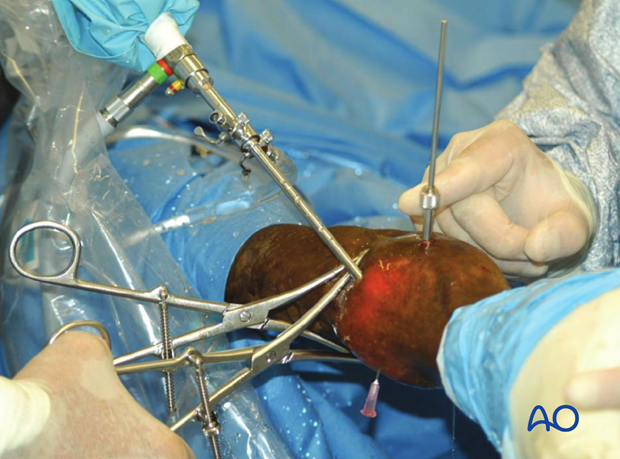
Maintaining reduction
When perfect reduction is achieved, the large pointed reduction forceps are applied to maintain position. Usually, it is easiest to place the points of the instrument at about the level of the physeal scar. The tips simply puncture the skin. The forceps should be positioned such that the arthroscope can still be manipulated.
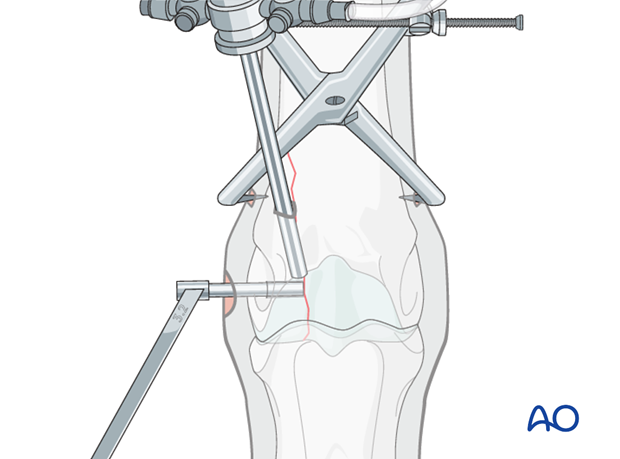
6. Screw fixation using lag technique
Preparation of the thread hole
After reduction is achieved, the 3.2 mm drill bit is used to prepare the thread hole across the remainder of the bone. The drill bit should be removed and cleaned frequently because this is very dense bone.
Extensive irrigation during drilling is always required.
Caution should be used when approaching the far cortex to minimize damage and debris as the drill bit exits the bone.
Note: It is essential to drill across the entire condyle and not to leave a blind hole.
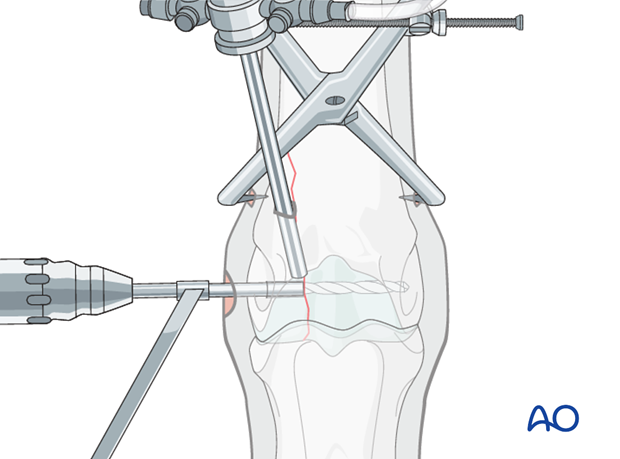
The 3.2 mm bit is removed and the 2.5 mm pin re-inserted through the drill sleeve. This pin is valuable to minimize any difficulties finding the screw hole through the stab incision.
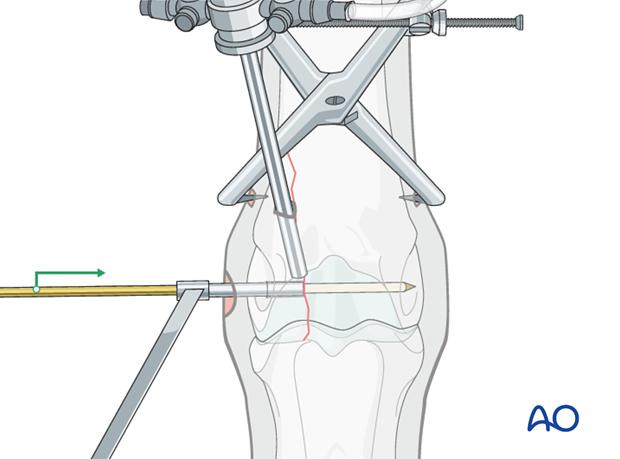
No countersink depression is prepared because the screw head comes to lie in the epicondylar fossa. Countersinking may add additional trauma to the collateral ligament.
Note, some surgeons nevertheless prefer to prepare a countersink depression.
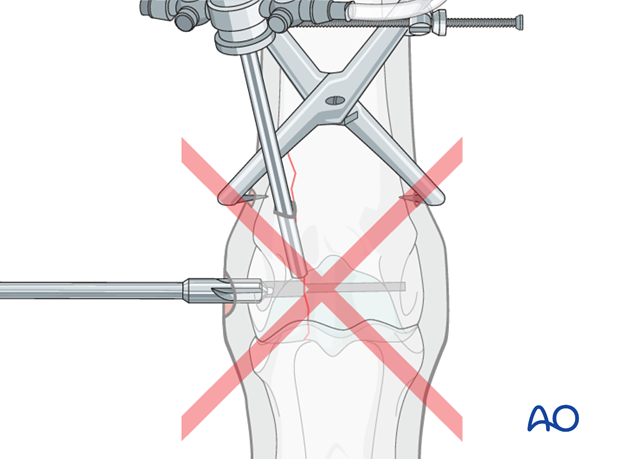
Tapping the hole
If no countersinking is done, the smooth pin is maintained in the glide hole and thread hole. The 4.5 mm drill guide is placed over the 2.5 mm pin (A). The pin is then removed (B) ...
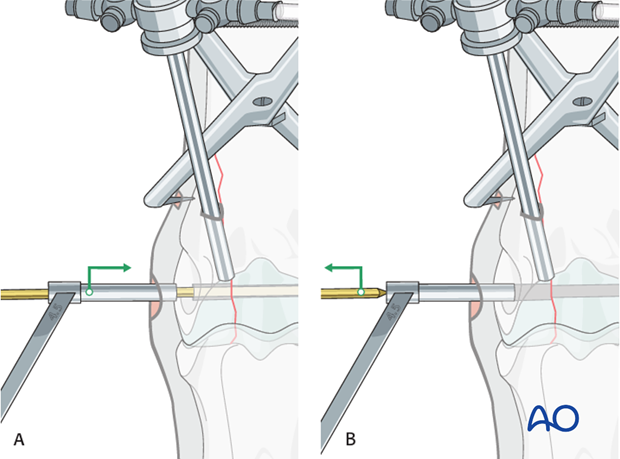
... and the 4.5 mm tap inserted through the guide (C).
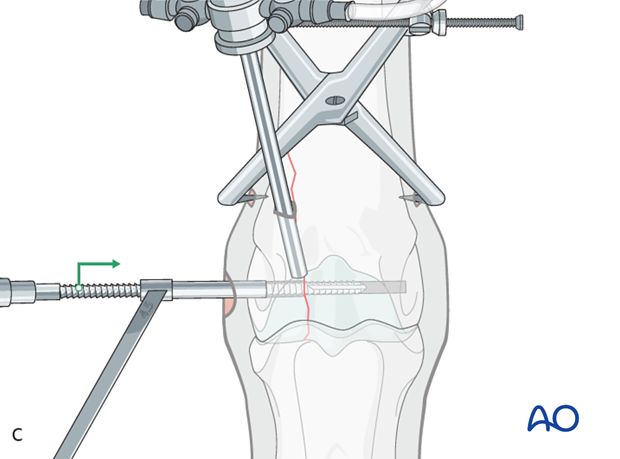
The hole is tapped routinely, keeping the very dense bone in mind.
It is critical to tap completely through the far cortex (red circle). The bone is so dense that even a single millimeter of untapped bone may prevent complete screw insertion and compression of the fracture plane.
A long tap is strongly preferred to avoid impinging of the end of the drill on the edge of the drill guide (yellow circle). This could result in stripping of the threads or breaking the tap.
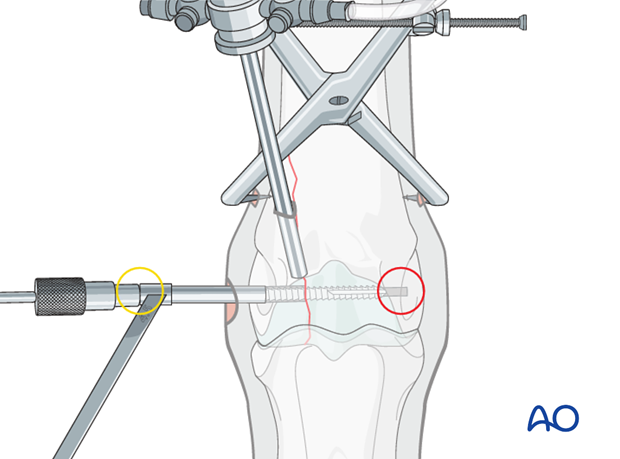
Screw insertion
Measurement of the hole is usually not necessary in this location. Most race horses accommodate a 52 mm cortex screw across the distal condyle.
The screw is inserted but not fully tightened. A fluoroscopic view may be taken to estimate if the screw length is correct.
Note, the provided image is a medial condylar fracture demonstrating the principle.
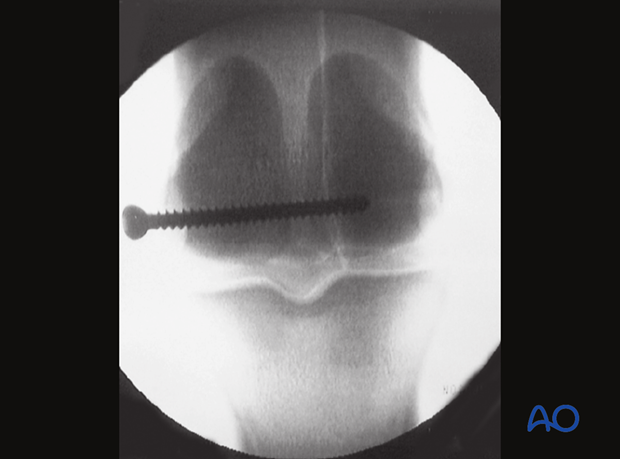
The arthroscope is positioned so that the fracture line can be seen while the screw is tightened. When the screw is tightened, blood/fibrin can usually be seen to be squeezed out of the fracture line, confirming compression by the lag screw.
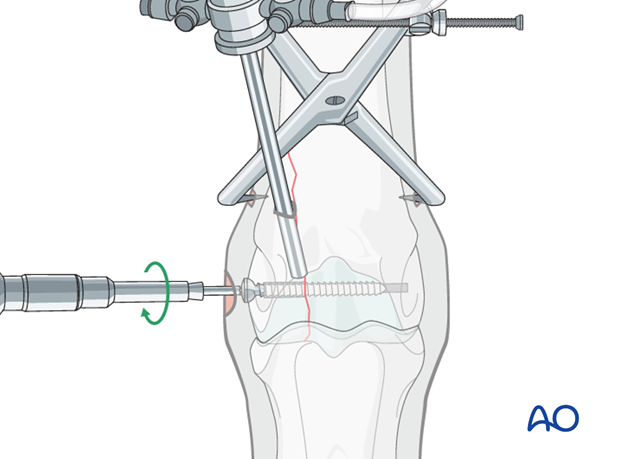
Placement of additional screws
A second screw is placed approximately 2 cm proximal to the first screw using routine lag technique.
Note: In this location countersinking is always used.
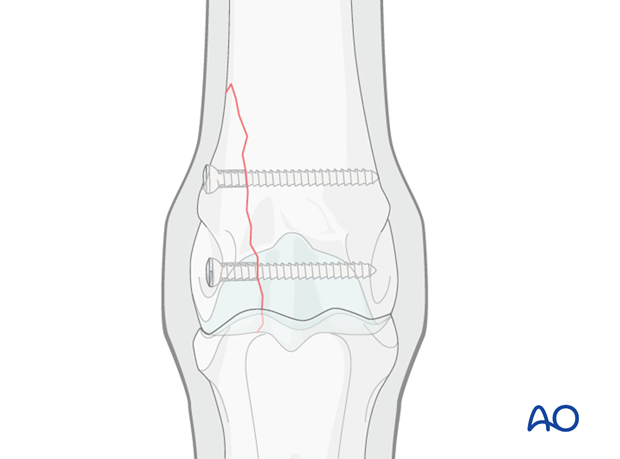
In the great majority of cases, only two screws are necessary. Caution is needed if placing a third screw because the lateral fracture fragment tapers and becomes narrow and thin proximally. The danger is placement of the screw in a fracture plane or splitting of this narrow portion of the fragment during tightening of the screw.
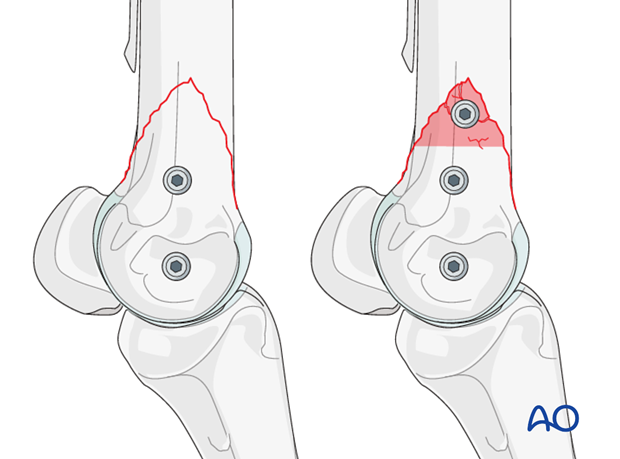
Arthroscopic confirmation
The palmar aspect of the joint should then be examined arthroscopically. Loose fragments along the distal palmar/plantar margin of the joint should be removed. The metacarpo/metatarsophalangeal joint must not be flexed too much or the area of injury on the distal palmar/plantar condyle will not be visible.
Full thickness cartilage defects on the proximal sesamoid bones also can be assessed and treated with microfracture if desired.
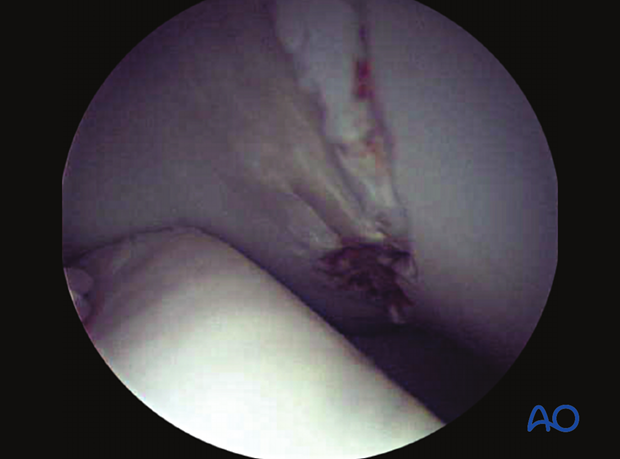
7. Recovery from anesthesia
Horses are usually placed in well-padded lower limb bandages for recovery from anesthesia.
Recovery of hind limb fractures
Hind-leg fractures should be recovered with more caution. If any special recovery system (pool, sling, deep mat/air mattress etc.) is available it should be employed. If none of these are available a full-limb cast should be applied during recovery. Half-limb casts do not fully protect horses from catastrophic failure through the diaphysis.
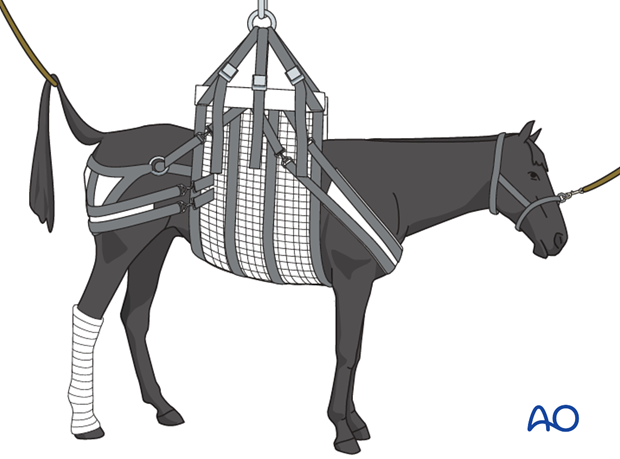
8. Aftertreatment
Horses are usually placed in stall rest and hand-grazing only for at least 60 days, followed by hand walking or machine walking exercise for an additional 60 days before allowing turnout in a very small paddock. Most horses get about a minimum of 6 months before returning to training.
Intra-articular medications depend on surgeons preference and the degree of articular damage seen during surgery.

Imaging
Follow up radiographs are usually taken in 90 days and again before returning to training.
Implant removal
Screw removal is generally recommended only if the screws extend up into the diaphysis.