Double plating
1. Implants
The repair can be carried out with Dynamic Compression Plates (DCPs), Limited Contact Dynamic Compression Plates (LC-DCPs), or Locking Compression Plates (LCPs), among which the LCPs are presently the first choice.
Dependent upon the size of the animal and the fracture configuration, either 2 broad plates or one broad and one narrow plate may be applied.
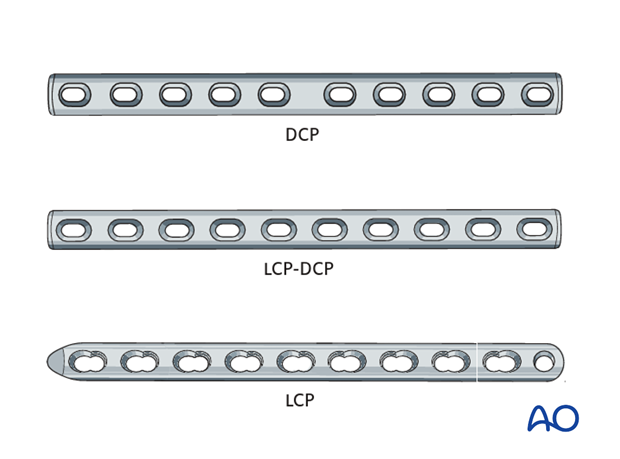
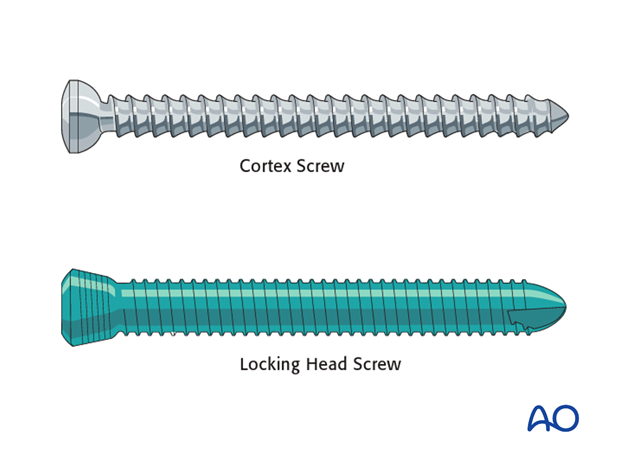
The plates are attached to the bone either with cortex- or locking head screws; the latter only in the LCPs.
Dependent upon the size and/or age of the animal either 3.5 mm (in ponies and small foals), 4.5 mm or 5.5mm cortex screws are used. Usually cancellous screws are avoided.
3.5 mm cortex screws can be used in lag fashion even in adult animals to initially repair the fracture. This is routinely followed by the application of larger plates.
2. Principles
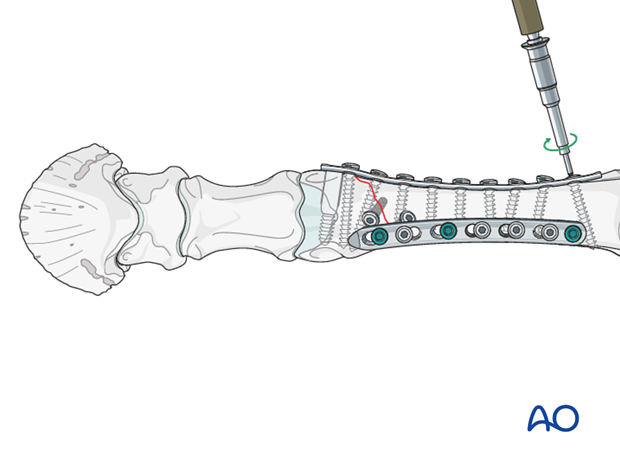
The fracture is anatomically reduced and repaired with one or two plates spanning the entire bone and applied at 90° relative to each other (left). In small ponies, some foals and selective cases of adult horses only one plate may be selected (right).
The major problem in these fractures is to achieve adequate purchase in the distal/proximal metaphyseal fragment to allow immediate weight bearing.
Special plates systems such as the DCS system are ideal for such situation because the barrel of the plate, with an outside diameter of 25 mm that is angled 95° relative to the plate is inserted into the metaphyseal fragment. Through the barrel a large screw with long shaft (8 mm diameter) and a threaded portion at the end (25mm long and 25mm diameter) is inserted through the barrel providing superior holding power within the small diaphyseal fragment.
Alternate possibilities are any of the human condylar plate, which either are stronger (left) or allow the placement of multiple screws in a widened area of one plate end.
Occasionally even an adjacent row of bones may be used to achieve additional purchase. The distal row of carpal/tarsal bones lend themselves for this techniques because they form non-moving joints with the proximal McIII/MtIII respectively.
It is very important to insert some interfragmentary screws to assure the not only the plate(s) bridge the fracture.
Care must be taken in foals to avoid bridging the distal physis of the bone.
3. Preparation and approach
This procedure is performed with the patient in dorsal recumbency or in lateral recumbency, through an open approach.
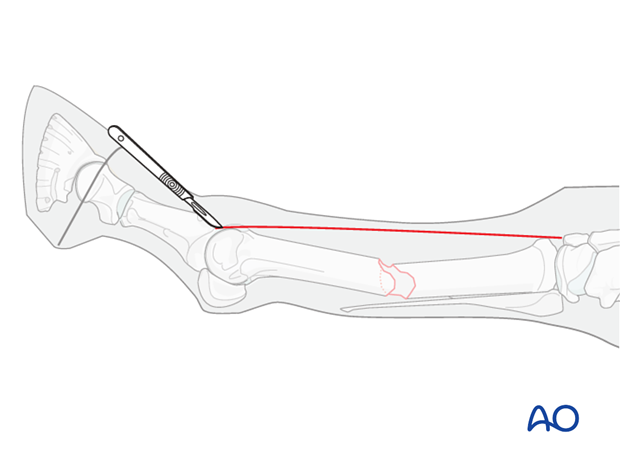
4. Fixation of a distal metaphyseal fracture
The skin is incised along the entire fractured bone to allow covering of the most distal aspect of the proximal fragment with the plate and avoiding joint penetration.
The periosteum is usually ruptured in the fracture region. Care should be taken to avoid additional extensive trauma to the periosteum, such as complete stripping of the periosteum around the circumference of the fractured bone.
Note: Locking Compression Plates can be applied over the periosteum. Alternately, only the area that will be located under the plate(s) can be stripped off the periosteum.
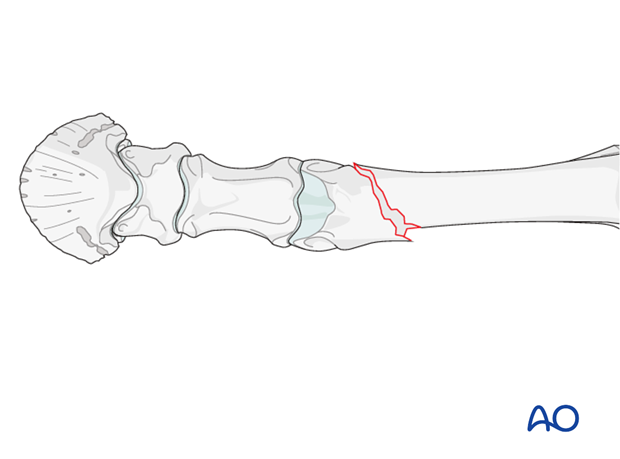
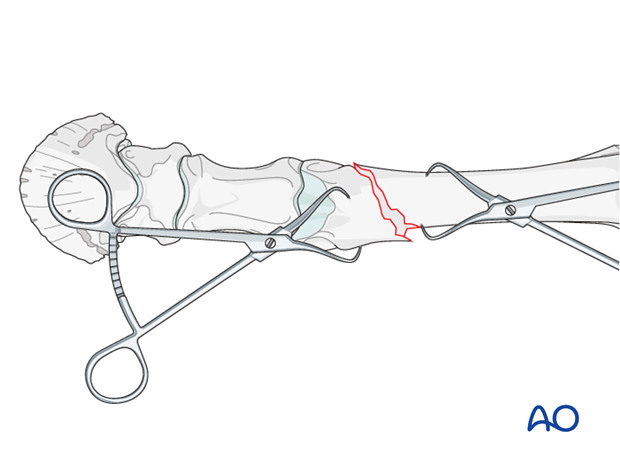
The fracture is anatomically reduced using traction, tenting and rotating movements, followed by the application of one or two pointed reduction forceps.
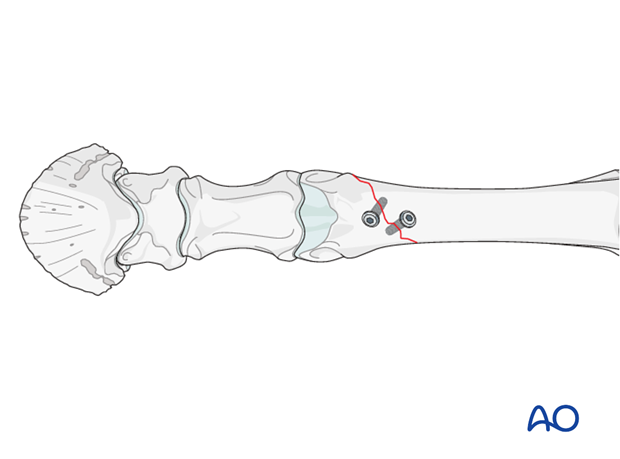
Ideally two 3.5 mm interfragmentary cortex screws are inserted to fix the fracture, ideally through places distant from the future plate location.
If necessary the screw heads can be countersunk such that they are flush with bone surface, which allows the placement of a plate directly over them.
The reduction forceps are subsequently removed.
The special DCS drill guide is placed with the hole at the level of the physeal scar (widest aspect of the distal McIII).
Care is taken not to tilt the drill guide forward to make contact with the bone. This would result in an altered angle of the drill hole relative to the plate barrel and would demand extensive additional plate bending resulting in inadequately contpured plate and significant prolongation of surgery time.
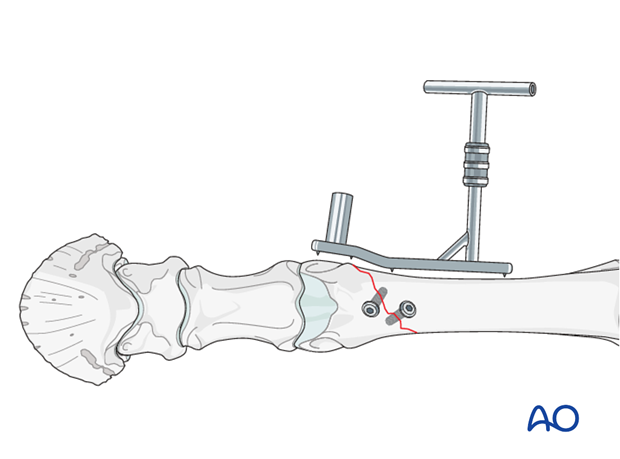
Because the equine bone is very dense it is necessary to pre-drill the hole for the guide pin with a 2.5 mm drill.
The drill hoe should not exit the bone on the distant side.
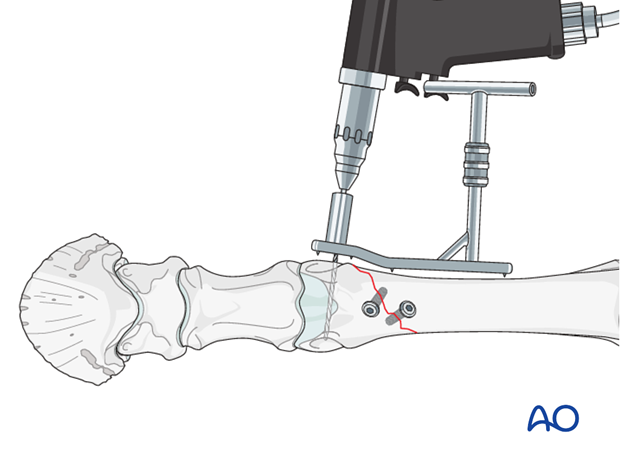
The drill bit is exchanged with the 2.5 mm guide pin, which is inserted to a length ca. 3 mm shorter than the bone width at this point.
The measuring device is placed over the guide pin and the portion of the pin located within the bone is determined.
It is advisable to measure the bone width on the radiograph and frequently compare it with the distance the guide pin is inserted into the bone.
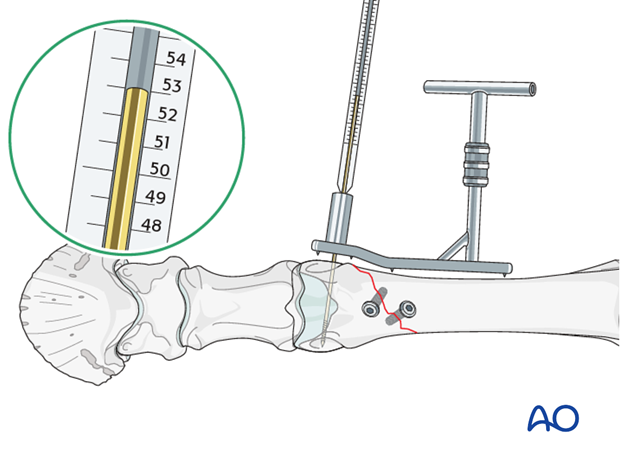
The DCS triple reamer is now assembled, adjusted to a length of 50 mm and fixed in that position.
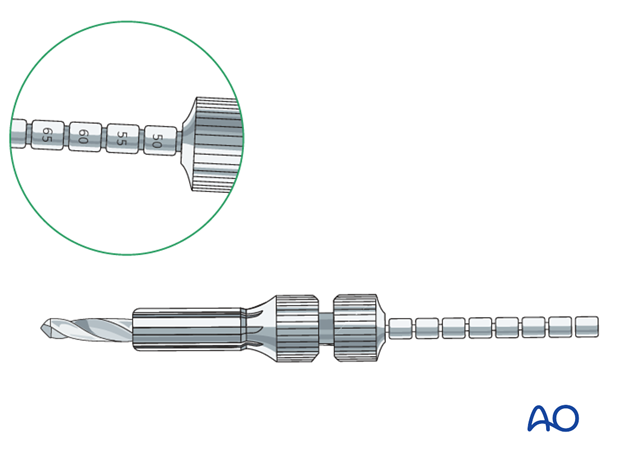
The triple Reamer is placed over the guide pin and subsequently the hole for the screw shaft (8 mm diameter), the hole of the barrel (25 mm diameter and 25 mm long) as well as the bevelled part where the barrel connects to the plate are drilled. It is advisable to frequently clean the triple reamer and continuously flush to lubricate the triple reamer.
Once the triple reamer has reached the bone surface the holes are prepared.
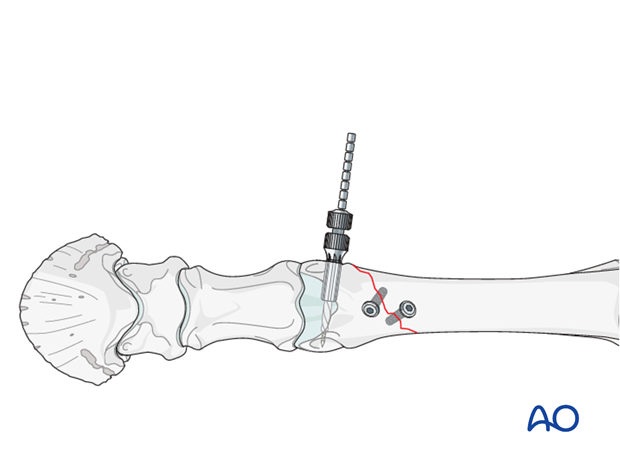
The triple reamer is removed and the DCS tap connected to the “T”-handle. The tap guide is placed sideways over the tap and fastened. The tap is subsequently paced over the guide pin and slit distally into the hole created for the plate barrel. Tapping is conducted judiciously and stopped once the resistance increases and the tap guide shows the “0”- mark at the level of the bone surface.
Note: Ideally tapping should be stopped approximately 5 mm short of the drill hole end, but because the smallest screw is 50 mm and the plate barrel together with thread length measures also 50 mm, there is no place for additional security millimeters.
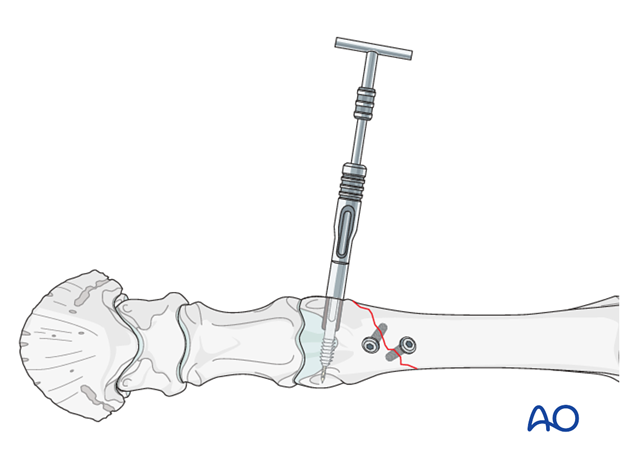
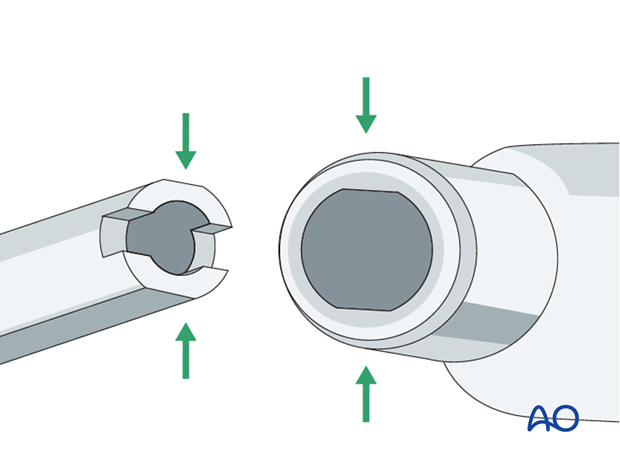
The shaft of the DCS screw has two opposing flat surfaces that fit perfectly into the barrel, which has the complementary cross-section. This configuration prevents rotation of the screw within the barrel once introduced into the prepared screw hole. The flat surfaces are oriented parallel to the long axis of the plate.
The Tap is removed and preselected and contoured DCS plate is placed over the applicator followed by connecting the DCS- screw and the insertion guide to the applicator. The screw is now inserted into the prepared screw hole and tightened such that the bar of the “T”-handle is parallel to the long axis of the plate, which assures that the plate barrel can be placed over the screw shaft in the correct position along the long axis of the bone.
Note: Minor adjustments in plate orientation can still be made once the plate barrel is placed over the DCS screw shaft. This will be coupled with minor screw rotation as well.
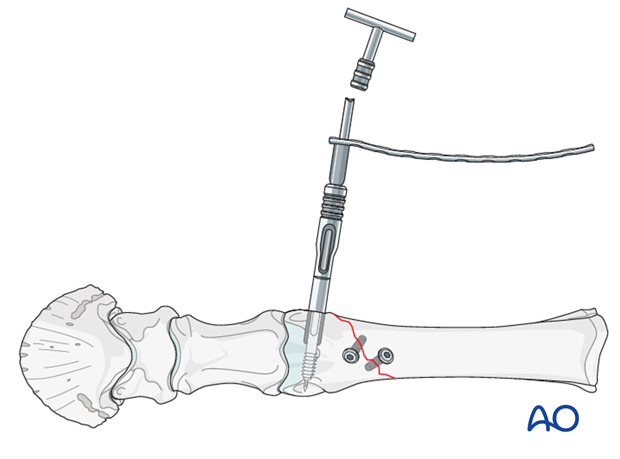
Once the plate barrel is placed over the screw shaft the impactor is applied the the plate and the help of a mallet the barrel is inserted to its end-position at the level of the DSC screw threads.
Note: In an ideal situation the should be some space between the barrel tip and the DCS screw threads. Because of the reasons explained above this is not possible in the distal McIII/MtIII.
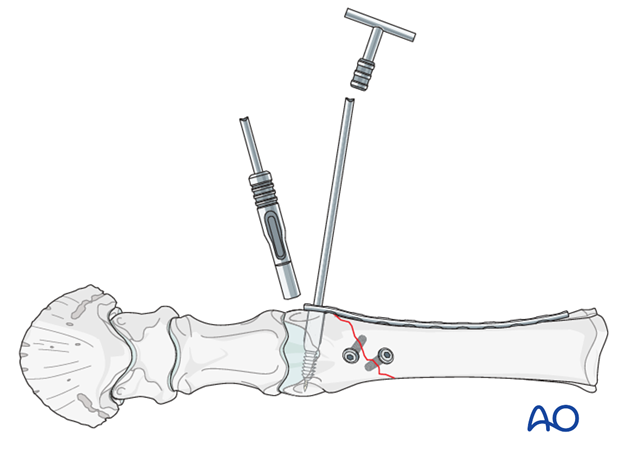
Next cortex screws are inserted through the second empty plate hole from the bottom and top respectively, and tightened, followed by insertion and tightening of the connecting screw into the back end of the DCS screw shaft. The latter unites the DCS screw and –plate into one implant.
If possible, 1 or 2 additional cortex screws are inserted in lag fashion through empty plate holes across the fracture.
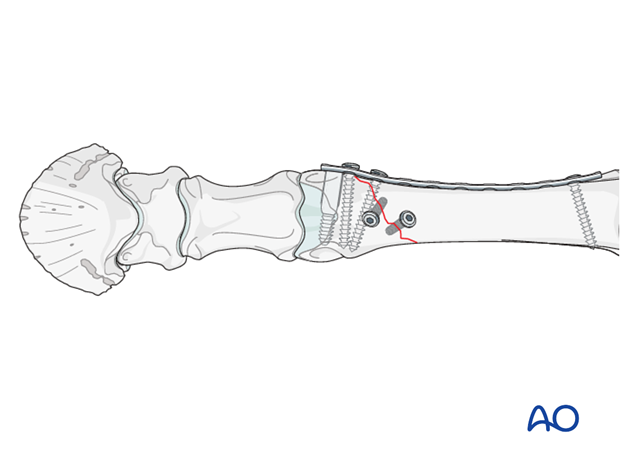
A plate slightly shorter than the DCS plate is now contoured to the dorsal aspect of the bone and applied with cortex screws through the second empty plate hole from the bottom and top as well as plate hole in the center of the plate.
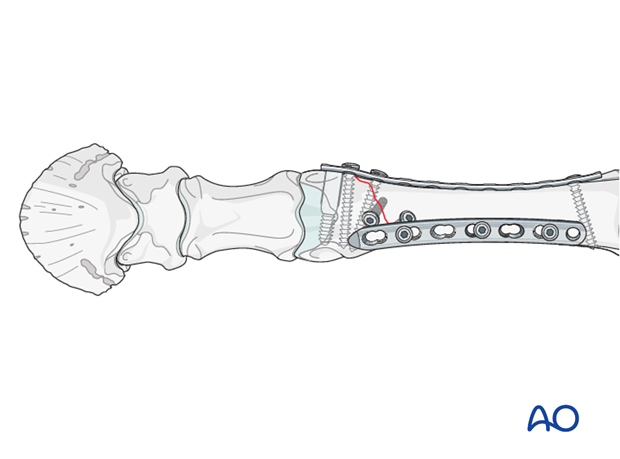
If locking compression implants are used (as shown here), locking head screws are now inserted through the empty holes at both ends of the two plates, as well near the fracture.
Note: The locking head screws need to be inserted perpendicular to the long axis of the plate. Therefore some adjustments in plate hole selection may be necessary.
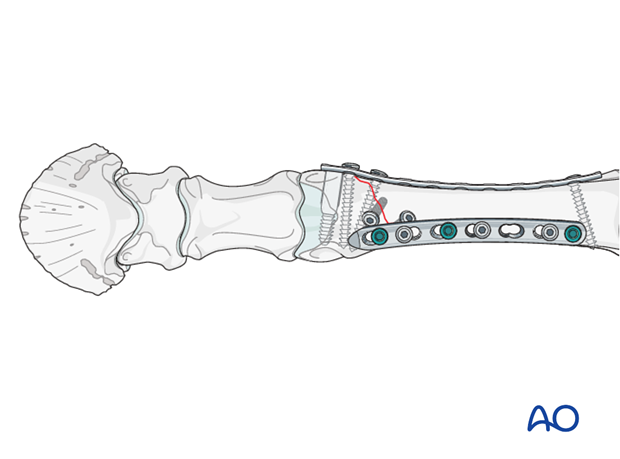
All remaining empty plate hole are subsequently filled with cortex screws and fully tightened.
Note: DCS implants can only be applied to the distal McIII/MtIII if the plate can be applied to the lateral or medial aspect of the bone. In all other location in these bones no 50 mm screws can be applied in the distal or proximal aspect because the bone is not thick enough. Therefore, two regular or special human plates, such as the condylar plate must be used in these locations.
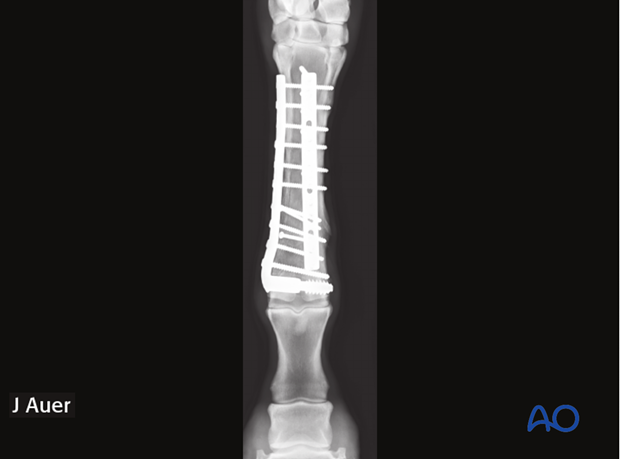
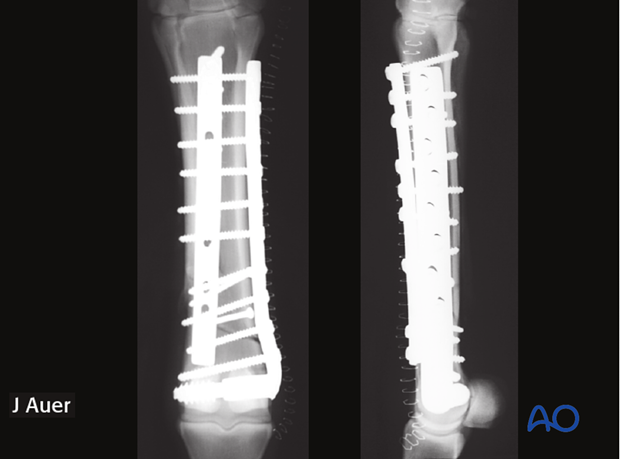
Immediate postoperative radiographs of a distal metaphyseal fracture treated with laterally applied DCS implant system and a slightly staggered dorsal DCP.
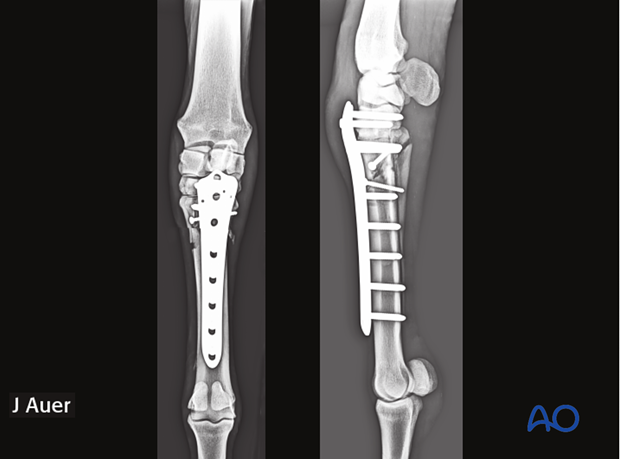
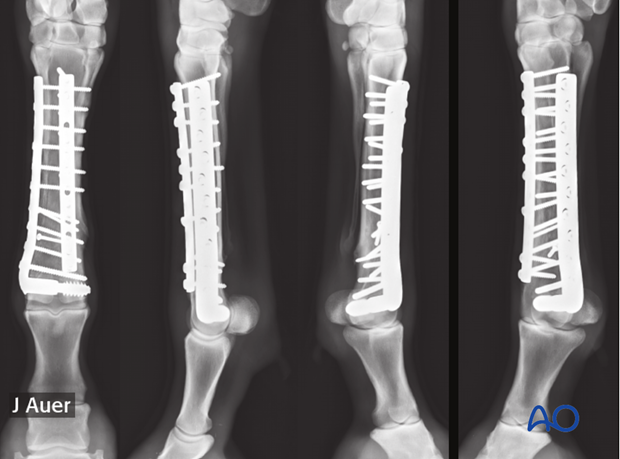
Followup radiographs of the same case as above 6 month postoperaively. The fracture is completely healed.
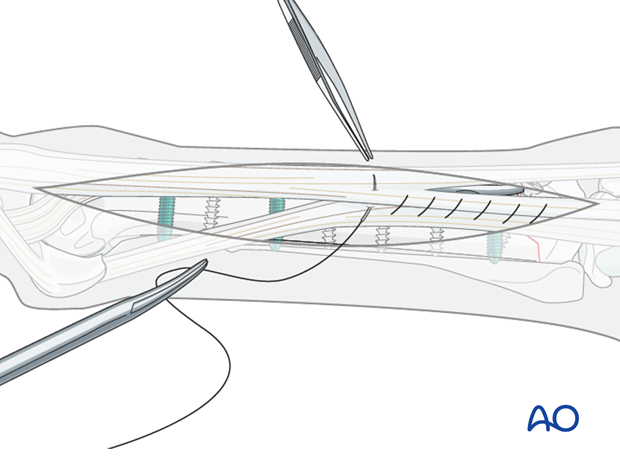
5. Skin closure
The longitudinally split common/long digital extensor tendon is sutured with a simple continuous suture pattern of a 2-O
monofilament synthetic absorbable suture material.
The subcutaneous tissues are subsequently closed in identical fashion as the tendon and the skin is closed with skin staples or simple interrupted monofilament nylon sutures.
6. Regional intravenous perfusion
At the end of the procedure it is advisable to perform regional intravenous perfusion with broad spectrum antibiotic of the surgeon’s choice.
A tourniquet is applied at the distal third of the radius/tibia followed by insertion of an indwelling catheter into the corresponding vein distal to the tourniquet (Cephalic vein in the forelimb, saphenous vein in the hind limb).
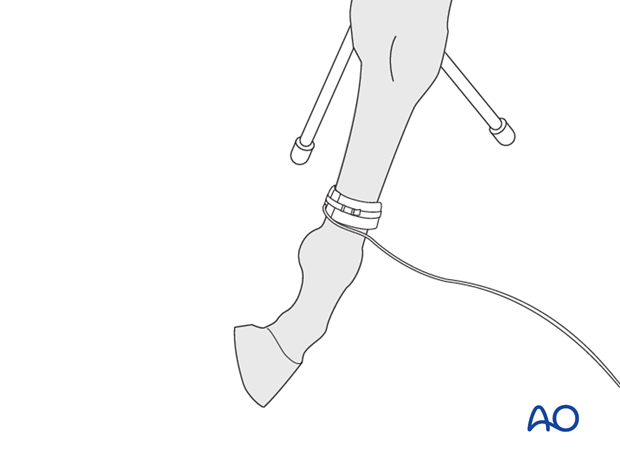
About 40 ml of blood is withdrawn from the vein followed by by slow injection of the same amount if antibiotic.
The antibiotic is maintained in the fracture region for 20 to thirty minutes.
7. Recovery from anesthesia
The animal is covered with a tight full-limb bandage and splint. Application of a full limb cast for recovery from anesthesia is an alternate option especially in proximal metaphyseal fractures.
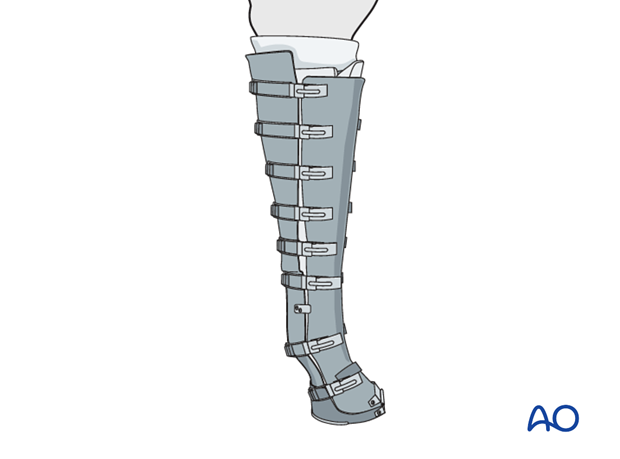
8. Aftercare
The patient is kept in a box stall for one month. The splint bandage is changed at 4-day intervals.
At the end of the first month, provided the patient uses the limb properly and and complication arose, the splint can be removed and a half limb bandage applied to the limb. At that time, some daily hand walking is allowed for one additional month.

Follow up radiographs are taken 2 months postoperatively. The remaining postoperative period is managed dependent upon the result of the follow up radiographs.
The management of the remaining reconvalescent period depends upon the progression of fracture healing assessed using the 2 month follow up radiographs.
Barring any complications the patient can be turned out into a small paddock and assume light exercise at 3 months postoperatively.

Implant removal
More information about implant removal can be found here.













