Screw fixation with osteostixis
1. Positioning and approach
Positioning
This surgical procedure may be performed under general anesthesia or on a sedated standing horse under local anesthesia. There is a slight risk of injury during recovery following this procedure. General anesthesia provides a superior asepsis and is more comfortable for the surgeon.
Surgery in the standing horse eliminates the risk of injury during recovery and is quite easy to do.
Localize the fracture
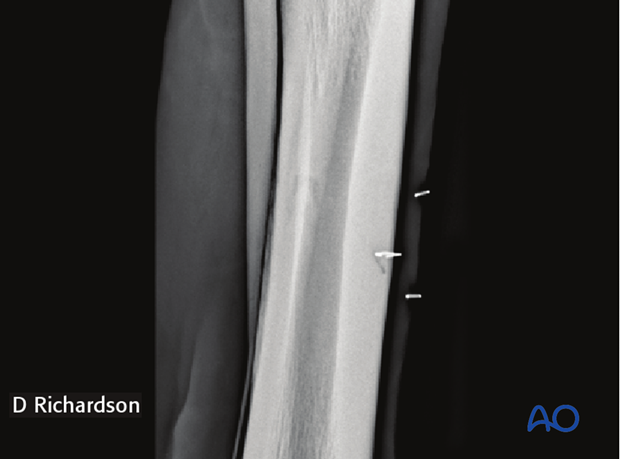
The incision is centered over the palpable swelling if it can be identified. If the fracture cannot be palpated, a small grid of sterile skin staples can be placed following aseptic preparation of the surgical site and a radiograph taken to identify the exact location for the incision.
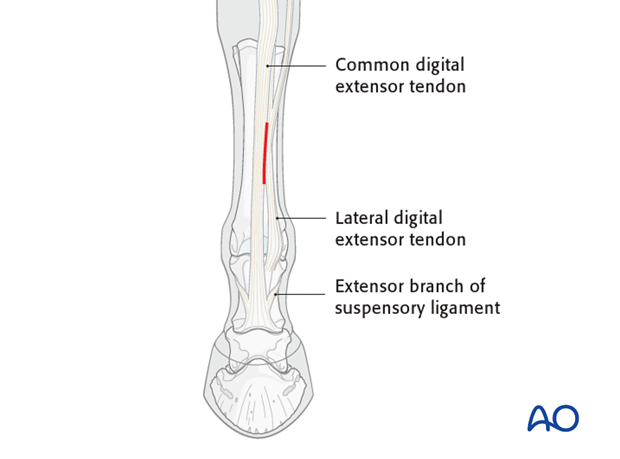
Skin incision
The incision is made directly down to the bone usually splitting the common digital extensor tendon from the lateral or simply splitting the edge of the combined tendon. If it is a more lateral fracture, the incision is made completely lateral to the tendons.
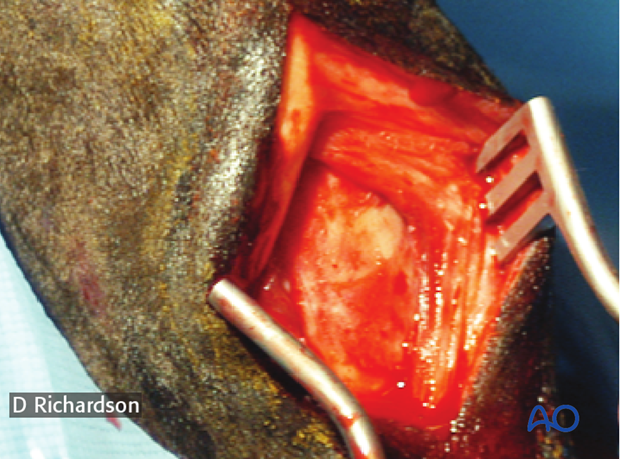
Exposure
The incision is approximately 4 cm in length and should go all the way down to the bone.
The scalpel can be turned over and the end of the handle used as a periosteal elevator. Alternatively the surgeon can use a standard elevator to expose the surface of the bone.
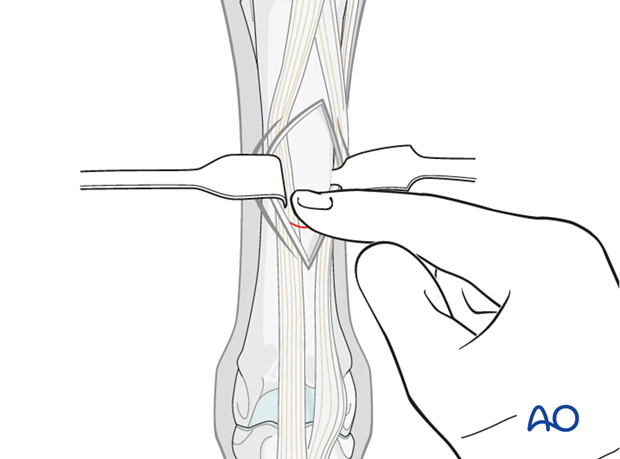
The actual fracture can only rarely be seen. Usually the surgeon can palpate the small callus on the surface of the bone.
Spreading of the edges of the incision with a sharp Weitlaner retractor is useful.
2. Principles
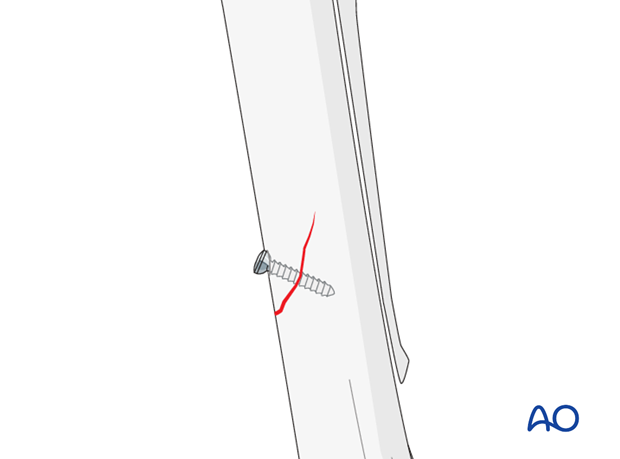
Many surgeons prefer to use a simple position screw for this fracture because it is not an unstable injury and the function of the screw is probably to cause a local response of the bone not to provide stability.
3. Preparation of screw insertion
Based on radiographs and palpation a 2.5 mm bit is used to drill across the dorsal cortex perpendicular to the estimated fracture plane.
If there is any question about the location of the fracture, an intraoperative radiograph either with the 2.5 mm drill bit in place or a 2 mm pin in the drill hole should be obtained.
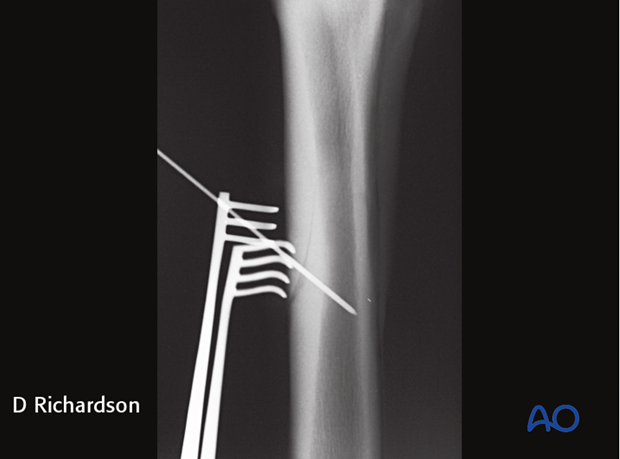
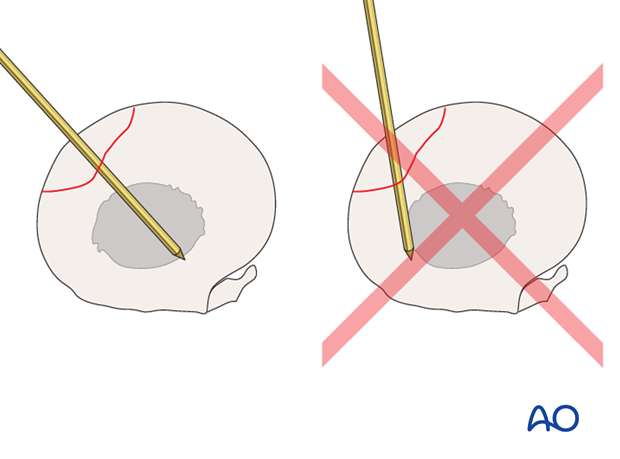
It is important to remember in these dorsolateral fractures to aim towards the middle of the medullary cavity, NOT directly towards the palmar cortex.
It is also important to only drill through the dorsal cortex.
If necessary, another hole is drilled in the correct location if the first hole was improperly positioned. The incorrectly positioned hole is not a problem and can be considered another osteostixis site.
The first drill hole in this case was too far proximal.
Measuring screw length
The hole can be measured, but does not need to be countersunk. It is easier to locate and remove the screw later if the head is not recessed.
Usually a 22 mm screw is adequate. The screw should not impinge on the palmar cortex.
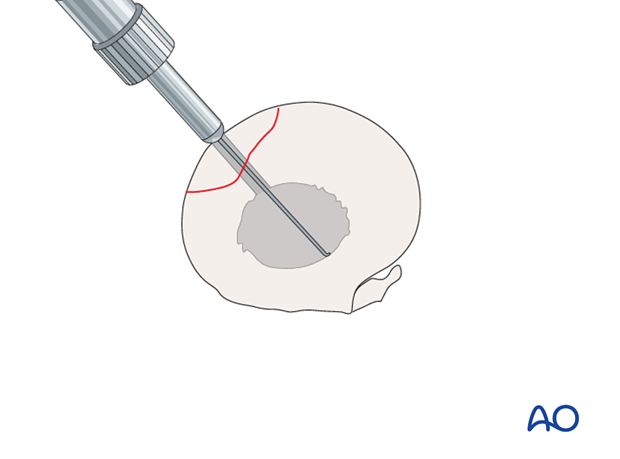
Cutting the threads
Threads should be cut in the hole with a 3.5 mm tap. This should be done by hand because power tapping may inadvertently result in striking the palmar cortex and breaking the tap.
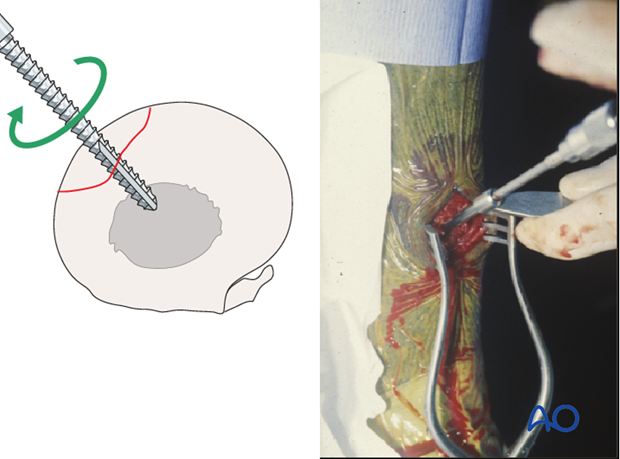
It is very important that the tap enters for a few mm into the medullary cavity to ensure that the hole is completely threaded. Even one mm of unthreaded hole in this very hard bone can result in the screw breaking during final tightening.
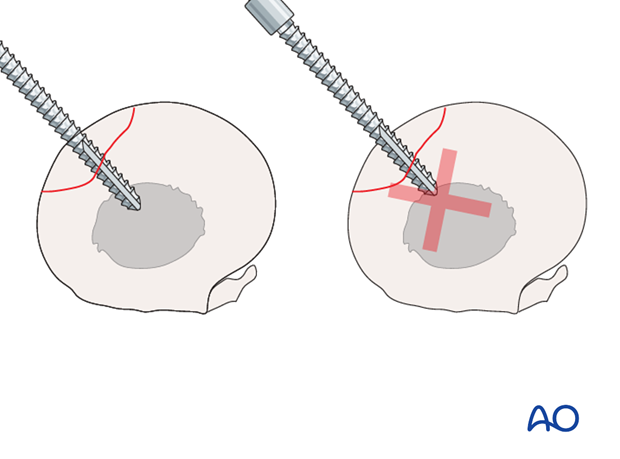
4. Screw Insertion
The screw is subsequently inserted and tightened. However the screw does NOT need to be excessively tight. Excessive tightening of a 3.5 mm screw will lead to bending because it is not countersunk or to stripping of the screw head.
Countersinking is not done because it makes it easier to remove the screw later.
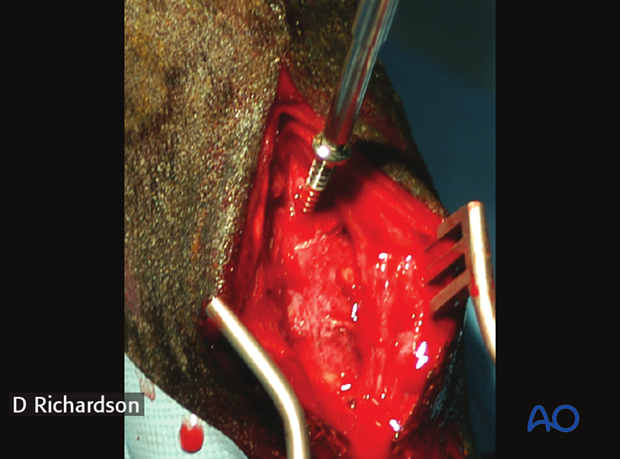
The screw head will protrude slightly from the surface because of the angle of insertion. Do NOT over-tighten it in an effort to get the screw head “flat” on the bone surface.
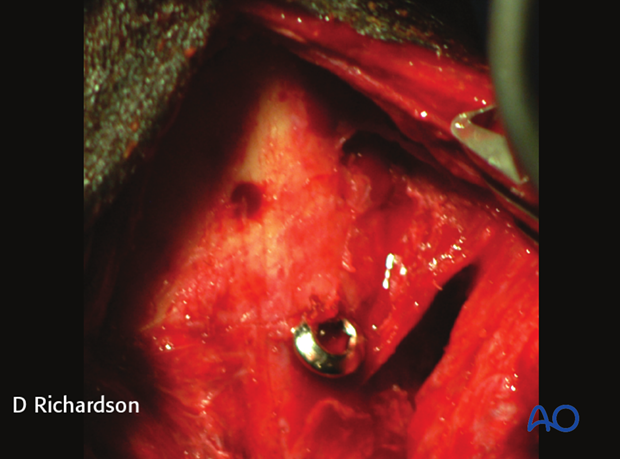
A postoperative radiograph is taken for documentation of screw and osteostixis positioning.
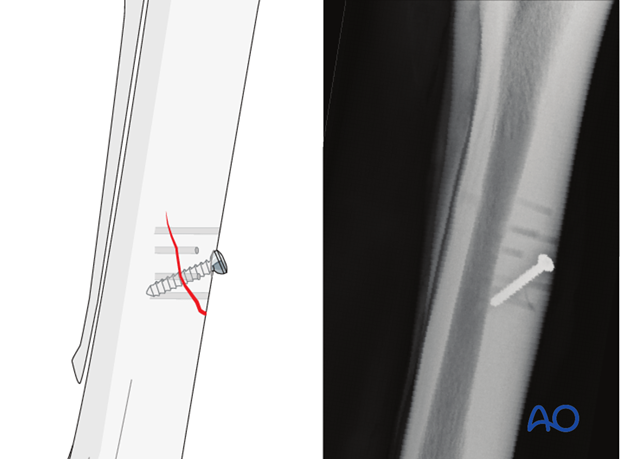
5. Complications
The most frequently encountered complications of this surgery are instrument breakage (left) and infection. The probability of either can be lessened by strict adherence to good technique.
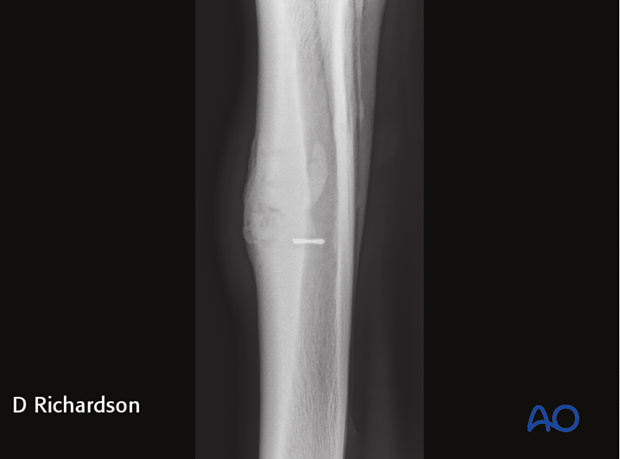
6. Alternative: Osteostixis alone
Osteostixis alone also has been used but many surgeons have found the results to be less consistent. It seems likely that the second procedure of screw removal “re-stimulates” the site.
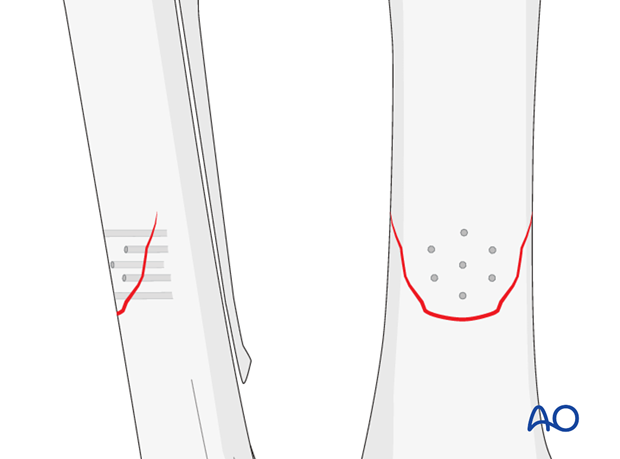
7. Aftercare
The horses can be bandaged routinely, but the owner/trainer should be advised that there will often be a large firm swelling at the surgical site.
Horses are stall rested with hand-grazing for two weeks followed by another two weeks of increasing hand-walking exercise. In four weeks the horse is allowed paddock exercise for another month.
After two months the horse is returned for screw removal.

Implant removal
More information about implant removal can be found here.