Metacarpals/-tarsals II and IV: Proximal fractures
Fracture characteristics
Proximal fractures of the metacarpals/-tarsals II and IV (splint bones) are usually the result of a kick from another horse and therefore are mostly open fractures.
They appear in various fracture configurations, from simple to segmental (left) to highly comminuted fractures.
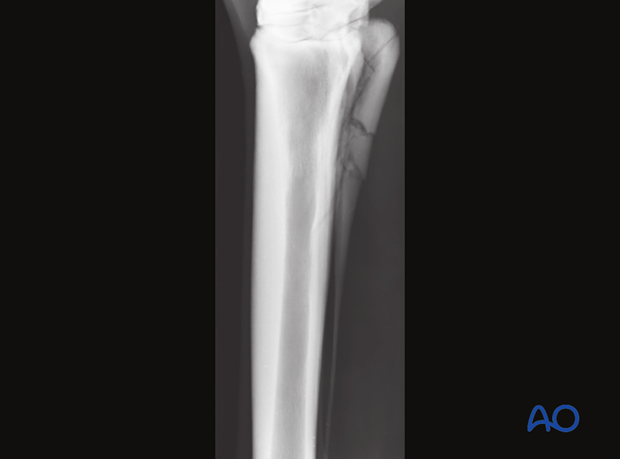
The third metacarpal/metatarsal bone and the region of the articulation with the carpal bones are carefully examined for associated fractures or fissures.
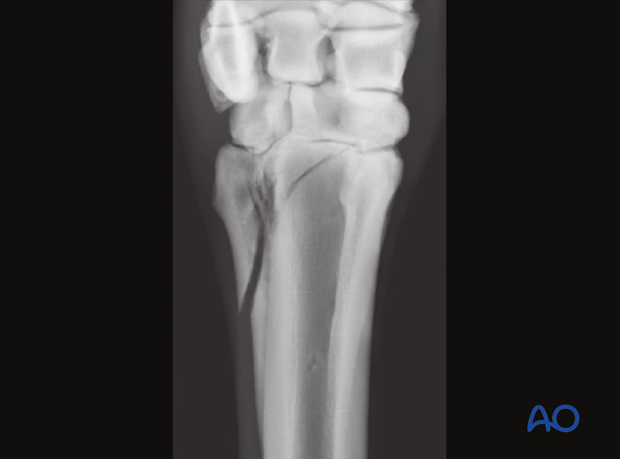
Anatomical considerations
The articulation between the splint bone and the carpal bone deserves special attention. The splint bones, especially the medial ones, are loaded axially. The attachment of the collateral ligaments exerts tension on the proximal aspect of the splint bones. Therefore, after removal of the distal aspect of a splint bone, the remaining proximal stump may dislocate, which can result in significant lameness and, eventually, degenerative joint disease.
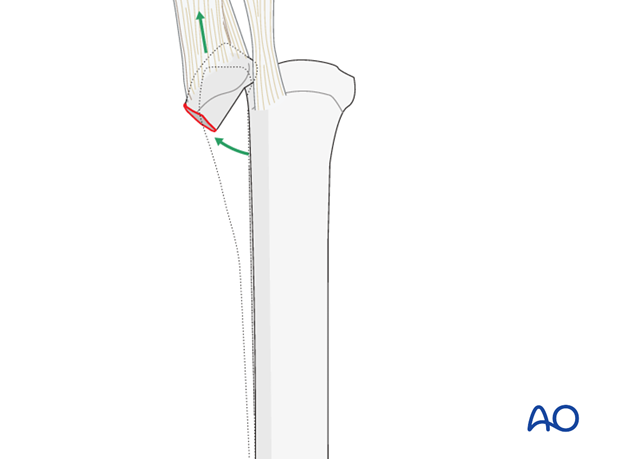
Fractures of the metacarpals/-tarsals II and IV - all fracture types
Fracture history
Fractures of the vestigial metacarpal and metatarsal bones, which are commonly referred to as splint bones, can occur anywhere along the bones and are very common in horses of all ages (Jackson et al., 2007). These bones are predisposed to injury because of their anatomic location, the nature of the horse and equine management practices. Kicks from other horses are probably the most important cause of splint bone fractures (Derungs et al., 2004), but fractures may also occur spontaneously, such as cyclic loading of the most distal aspect of the bone during exercise.

Fracture characteristics
Splint bone fractures can be open or closed, simple or comminuted, and localized in the proximal, middle or distal part of the bone.
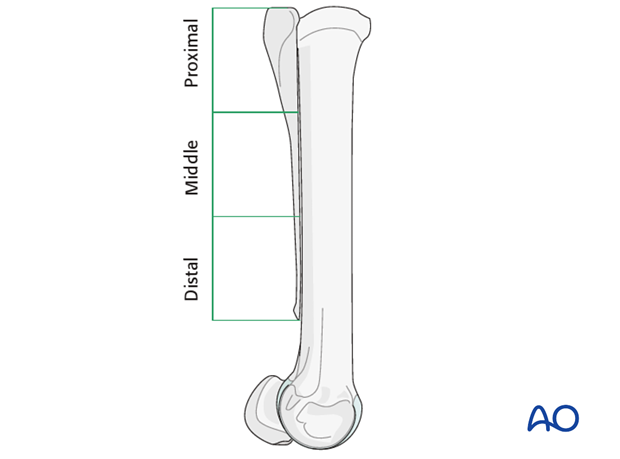
Physical exam
Once a splint bone fracture has been diagnosed, the structures close to the bone including the suspensory ligament, proximal sesamoid bones as well as the third metacarpal/metatarsal bone must be examined carefully. The lameness varies from moderate to severe; it is usually severe in horses with open proximal fractures and moderate in those with distal fractures. The interval between the injury and the time of presentation also profoundly affects the severity of lameness.

Open fractures
In addition to lameness, affected horses often also have an open wound near the splint bone. The degree of swelling, pain and heat is directly related to the extent of soft-tissue damage. The size of the wound caused by external trauma varies and is no indication of the severity of the fracture.
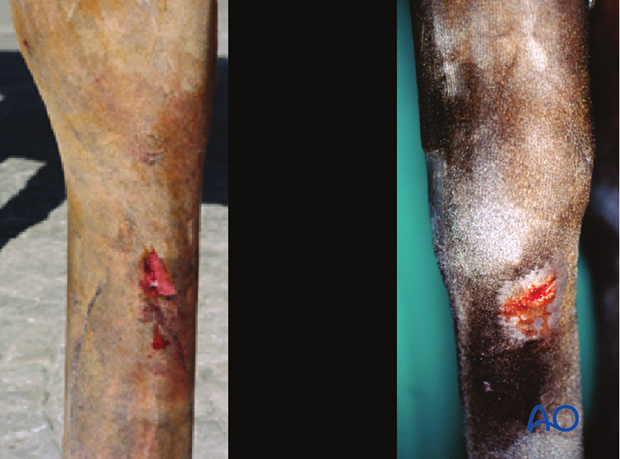
Imaging
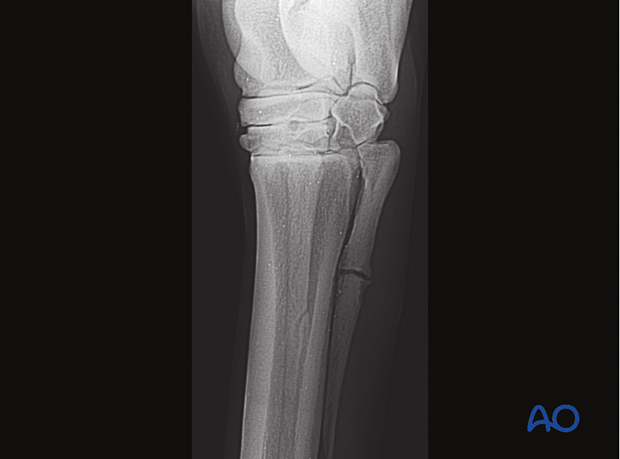
Radiographs are required to confirm the diagnosis and to rule out other complications. It is very important to take several views. The proximal articulation should always be included.
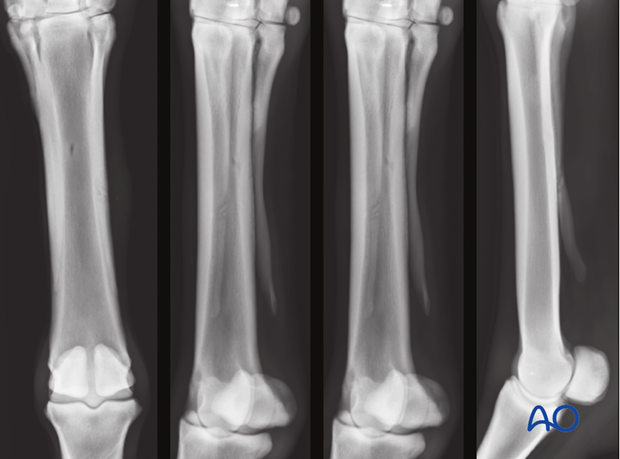
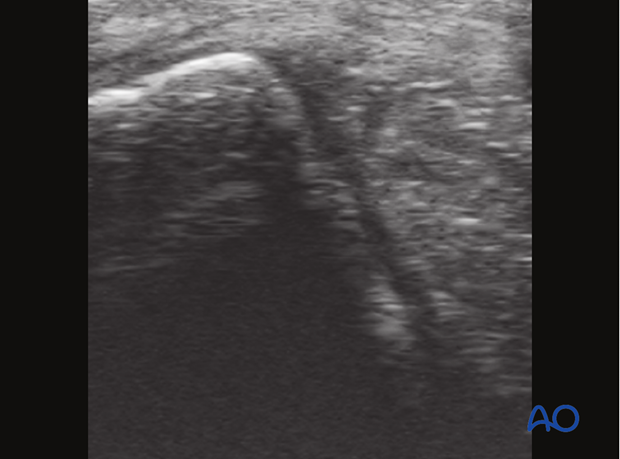
Ultrasonography is essential for the assessment of the suspensory ligament.
Computed tomography, if available, may be valuable for a definitive diagnosis in selected cases.
Complications
Complications, including nonunion (left), osteomyelitis and the formation of a sequestrum or excessive callus are common when the fracture is not treated properly. Involvement of the third metacarpal/metatarsal bone affects the prognosis negatively.
Prognosis
The prognosis of splint bone fractures depends primarily on the location, type and age of the fracture, but also on the involvement of tendons, soft tissues and the third metacarpal/metatarsal bone. If treated properly, the prognosis is good. It is critical that the clinician be alert and quickly identify fractures and infection, so that appropriate therapeutic measures can be implemented to improve the chances of the patient returning to its intended use.
Anatomical considerations
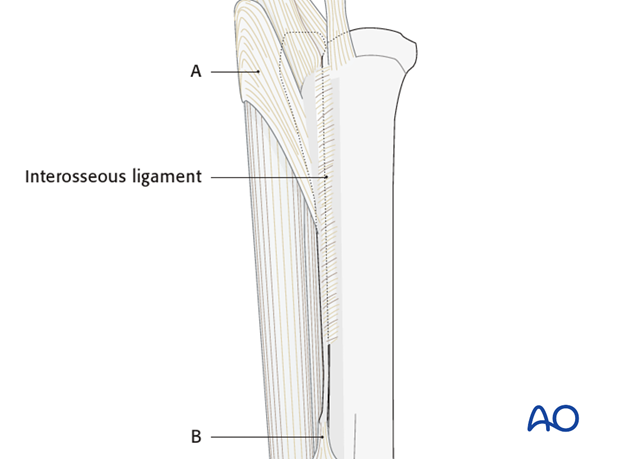
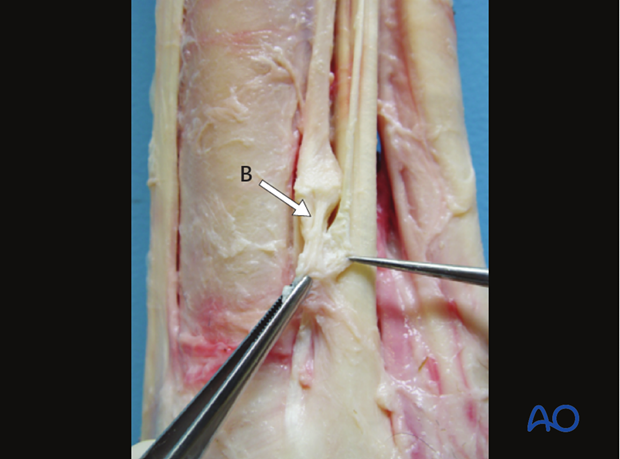
Strong collateral ligaments attach to the proximal part of the splint bones. The metacarpal/metatarsal interosseus ligament differs substantially among horses and may start to ossify at an early age. A firm fascia (A) covers the tendons in the proximal region of the metacarpus and is attached to the medial and lateral splint bone. A band-like structure (B) extends distally from the distal end of the splint bone toward the proximal sesamoid bone (Jackson et al., 2005).