Resection
1. Principles
Use of a tourniquet
The use of a tourniquet is at the surgeon’s discretion. In most cases, it is better not to use a tourniquet. This allows ligation or cauterization of bleeding blood vessels prior to closing the surgery wound resulting in less postoperative hematoma formation, potentially complicated by subsequent mineralization of the hematoma.
Intraoperative imaging
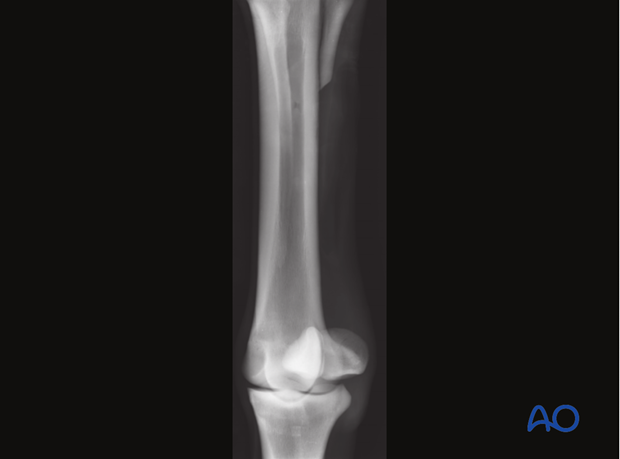
Intraoperative radiographic control is often necessary to confirm that all the fragments have completely been removed.
Anatomical considerations
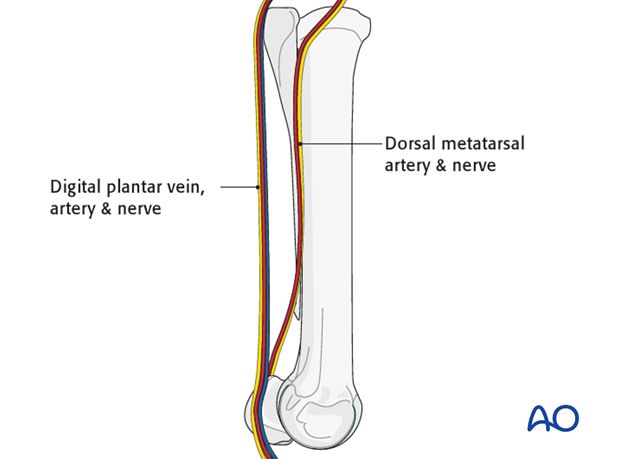
The dorsal metatarsal artery runs between the lateral splint bone and the third metatarsal bone. Care should be taken to avoid injury to the artery during surgery.
2. Removal of the distal fragment
Exposure
A straight longitudinal skin incision is made over the affected splint bone. The subcutaneous tissues and fascia are incised sharply down to the periosteum.
Further information on approaches to the split bone can be found here.
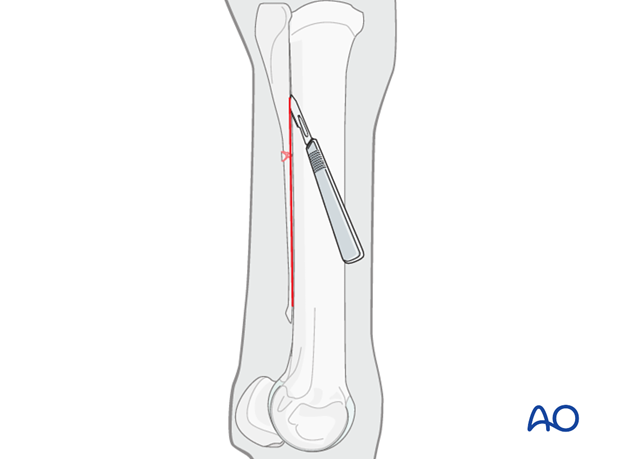
The distal fragment and the fracture callus are separated from the third metacarpal/metatarsal bone. Depending on the degree of ossification of the intermetacarpal/-tarsal ligament, a scalpel or an osteotome must be used.
Remember to avoid injury to the dorsal metatarsal artery.
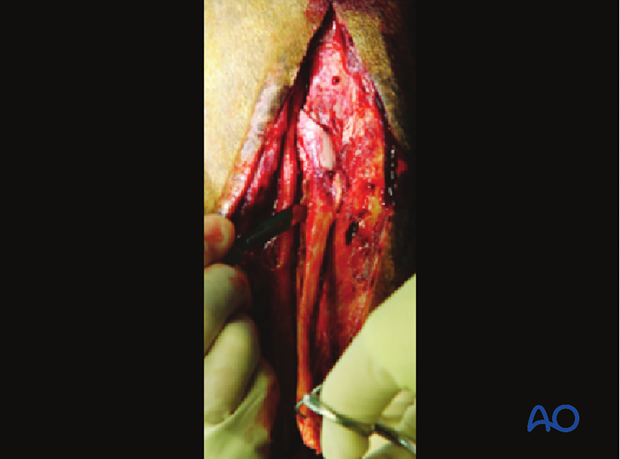
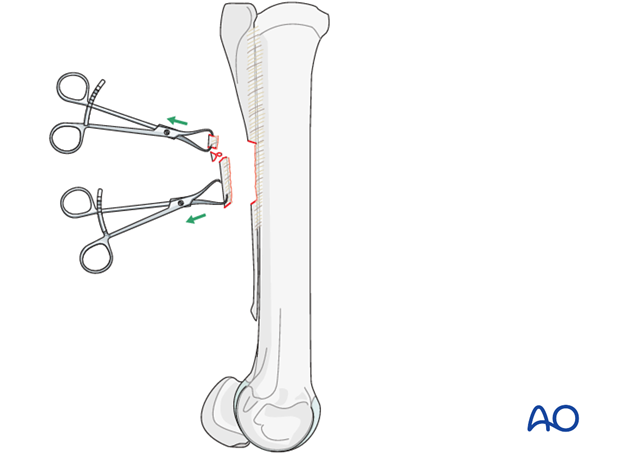
Transection of the splint bone
The splint bone is transected either obliquely or horizontal with an oscillating saw or osteotome approximately 1 cm proximal to the most proximal aspect of the fracture.
An oscillating saw is preferred to avoid microfissures, which can occur when an osteotome is used.
Avoid damage to the third metacarpal/metatarsal bone either with the osteotome or the oscillating saw.
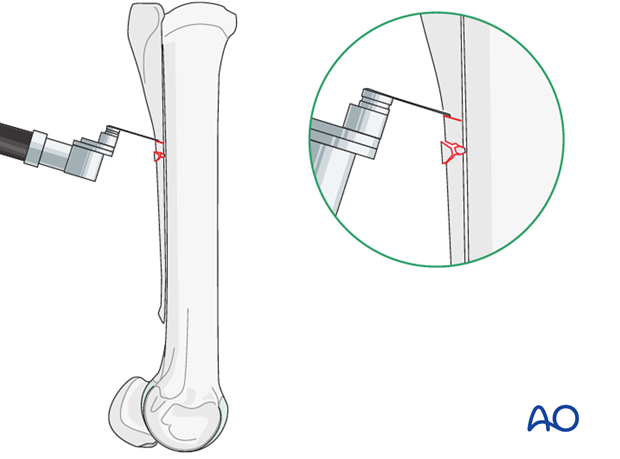
Use of an osteotome to amputate the most distal 1 cm of the proximal stump of the fractured splint bone.
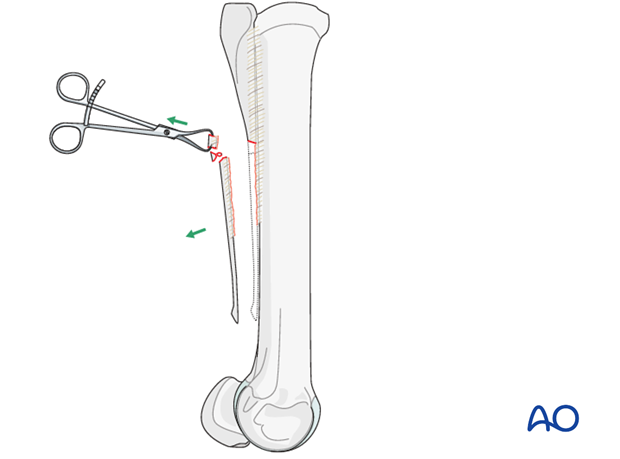
Removal of the fragments
The distal fragment together with its periosteum, any callus present, and the most distal aspect of the proximal fragment are removed.
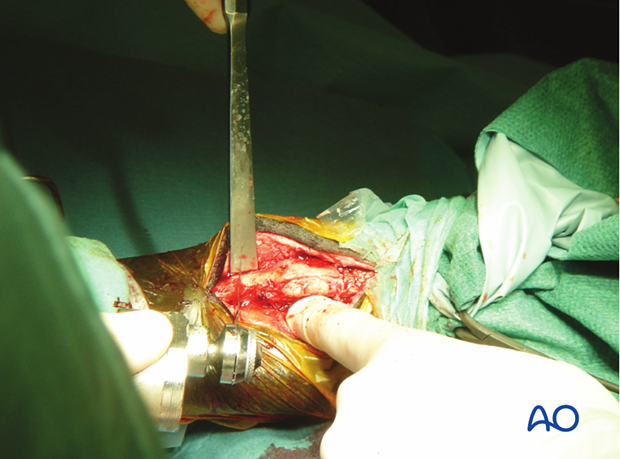
Intraoperative view of a fractured splint bone. The fracture site is identified by the arrow.
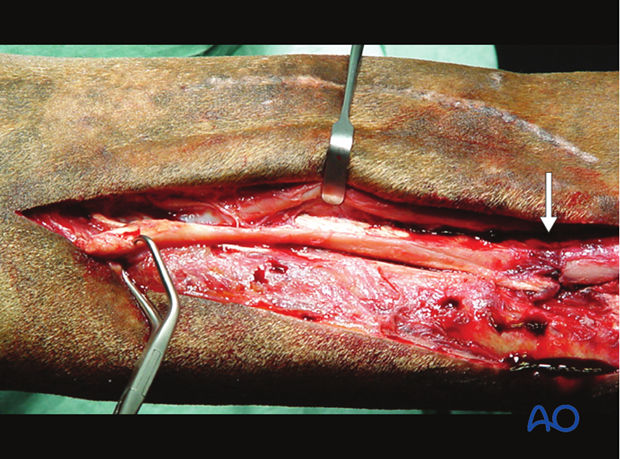
Lavage
The surgical site is extensively lavaged to remove any debris and bone fragments. Special attention is paid to hemostasis.
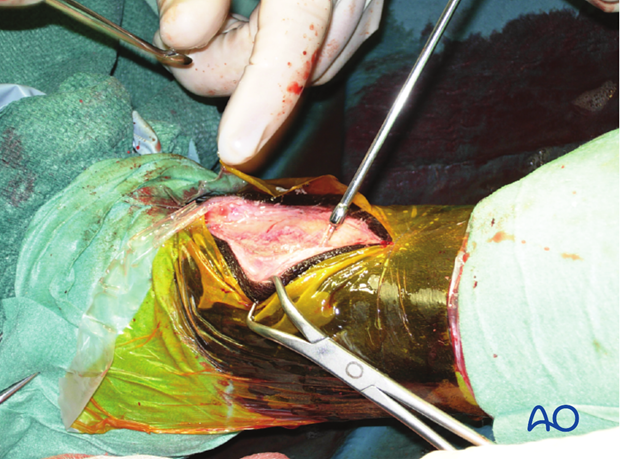
Closure
In open fractures, a drain is placed in the wound for 3-4 days. The exit wound of the drain normally heals on its own after drain removal. This treatment assures quick recovery of the horse and return to previous use.
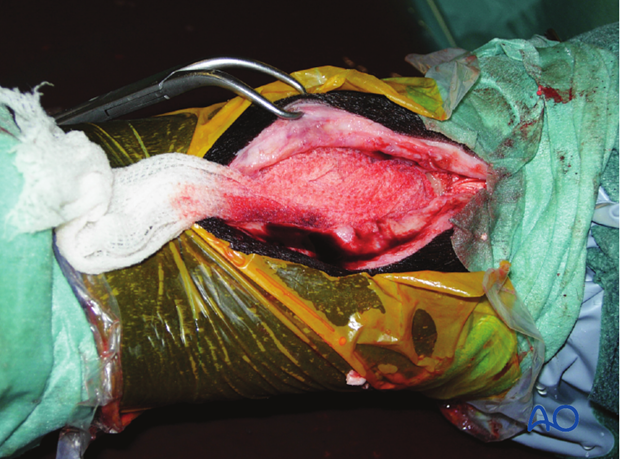
The surgery wound is closed in 2-3 layers applying routine technique. A pressure bandage is applied.
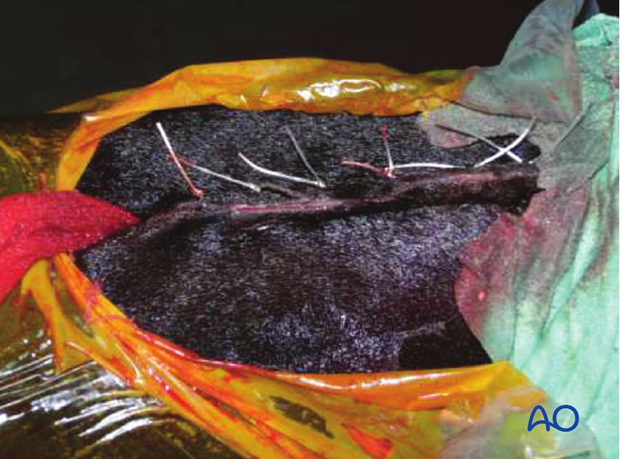
3. Alternative: Segmental ostectomy
Segmental ostectomy
In some cases, mostly very proximal mid-body splint bone fractures in mature horses, a segmental ostectomy can be performed (Jenson et al., 2004). The advantage of this technique is, that the incision can be kept shorter and a distal intact fragment remains in place.
If the distal fragment is not firmly attached to the third metacarpal/metatarsal bone, it should rather be removed, as it can irritate the suspensory ligament.
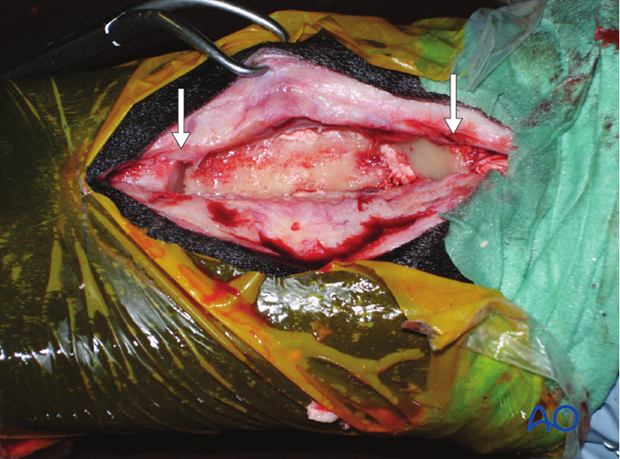
Intraoperative picture of a segmental splint bone removal. The proximal and distal osteotomy sites are marked with an arrow.
Complications
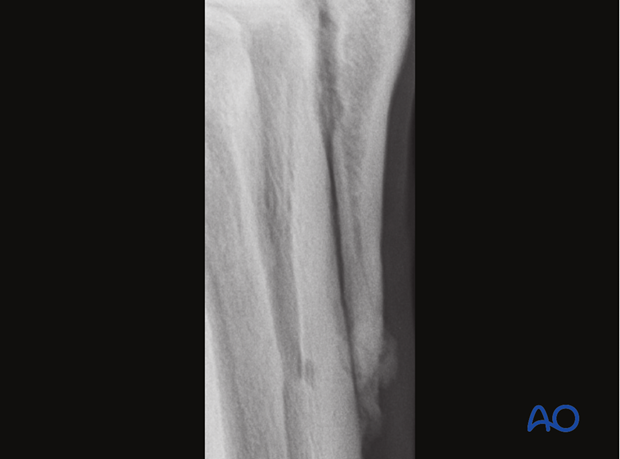
Complications of partial splint bone removal include new bone formation at the distal end of the proximal fragment, osteitis and wound infection.
In cases where new bone formation at the distal end of the proximal fragment results in chronic lameness, the callus together with the distal end of the remaining splint bone should be removed.
4. Aftertreatment
A bandage is applied and changed every 3 days for wound evaluation and wound care for two weeks.
Antibiotics are administered dependent upon the degree of infection.
The sutures are removed after 10 days.
The horse is kept in a stall for 4 weeks followed by hand-walking exercises for another 4 weeks before the horse can go back to its intended work.
Follow-up x-rays are taken 8 weeks after surgery to evaluate fracture healing resp. the remodeling process.
Possible complications
Splint bone fractures can be further complicated by the development of osteitis, osteomyelitis and/or bone sequestra.














