Partial carpal arthrodesis
1. Principles
Partial carpal vs. pan-carpal arthrodesis
A partial carpal arthrodesis is preferred as it is safer and easier to accomplish than a pan-carpal arthrodesis.
Biomechanics
Maintenance of slight flexion of the limb and slight remaining varus deformity is an important principle in controlling the biomechanics of the postoperative construct.
2. Preparation and approach
This procedure is performed with the patient placed in lateral recumbency and through the approach for partial arthrodesis.
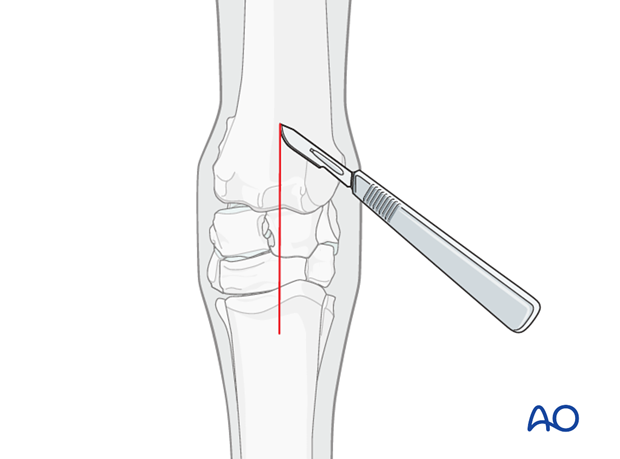
3. Correction of angulation
Principles
Traumatic injuries do not require an osteotomy, but deforming arthritic injuries may require a corrective osteotomy for realignment of the limb. For simple degenerative arthritis without limb deformity an osteotomy is not necessary.
If an osteotomy is needed, it is performed through the affected arthritic joint. For a partial carpal arthrodesis this is always the affected joint. For a pan-carpal arthrodesis the osteotomy is performed through the most deformed articulation.
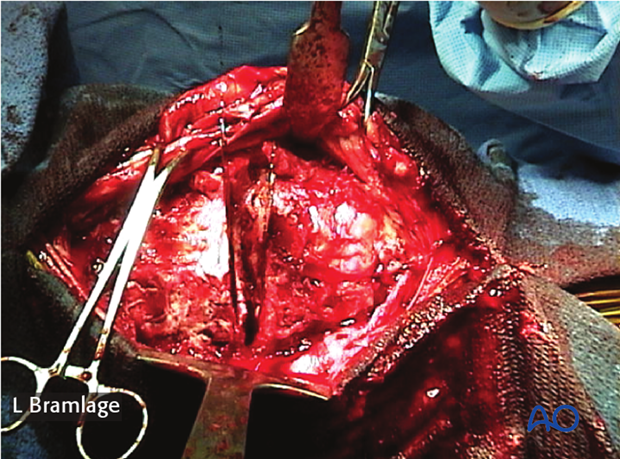
Osteotomy
The angulation of the osteotomy is estimated from the preoperative radiographs.
The postoperative goal after the osteotomy is to have the limb in slight flexion with slight remaining varus deviation to assure that the tension surface of the reconstruction is in the location where the plates will be placed.
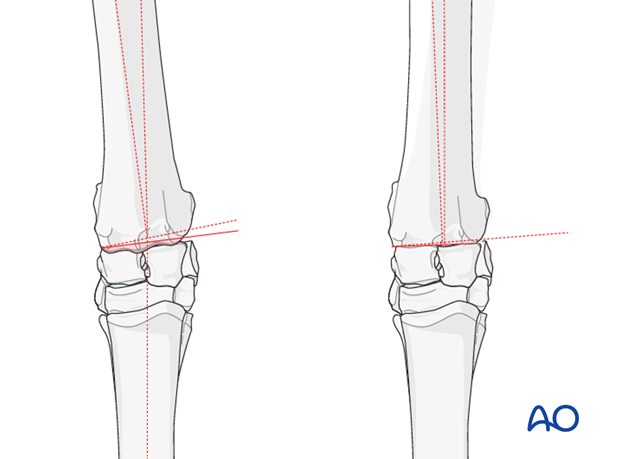
Therefore the plane of the osteotomy should diverge slightly from dorsal to palmar and should remove a wedge of bone smaller than the calculated amount as determined from the radiographs. If the osteotomy is done in the antebrachial carpal joint the surgeon must be aware that the accessory carpal bone is present in the posterior aspect of that joint and stop the osteotomy short of that bone.
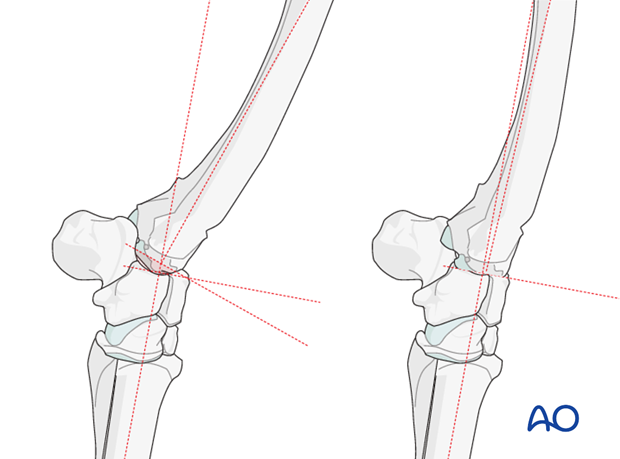
Once the osteotomy is created the wedge of bone to be discarded is removed using the bone saw and rongeurs. The limb is then corrected into the new alignment and a radiograph taken if needed.
4. Plate selection and preparation
Plate selection
For a partial carpal arthrodesis dynamic compression plates (DCP or LC-DCP) or locking plates can be used.
The first plate is normally a DCP or LC-DCP to take advantage of the ability to use the tension device and close the osteotomy. A locking plate with its increased strength and stability should be used for the second plate. If no osteotomy is needed the surgeon may choose to use two locking plates for the fixation.
Two screws through each plate are normally placed in the proximal row of carpal bones and 3-4 screws are placed across the distal row of carpal bones and the proximal metacarpus.

Plate contouring
The plates are contoured to the dorsal surface of the carpus.
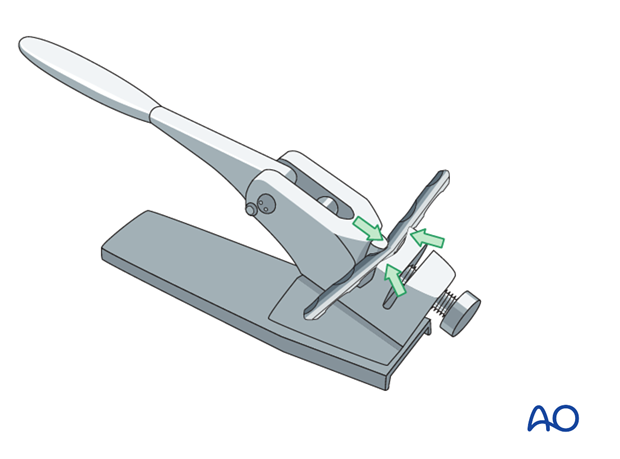
5. Surgical technique
Plate position
The plates are normally located dorsomedially and dorsolaterally over the intermediate and radial carpal bones of the proximal row. Occasionally, the plates will be placed over the intermediate and ulnar carpal bones if marked realignment of the limb is necessary.
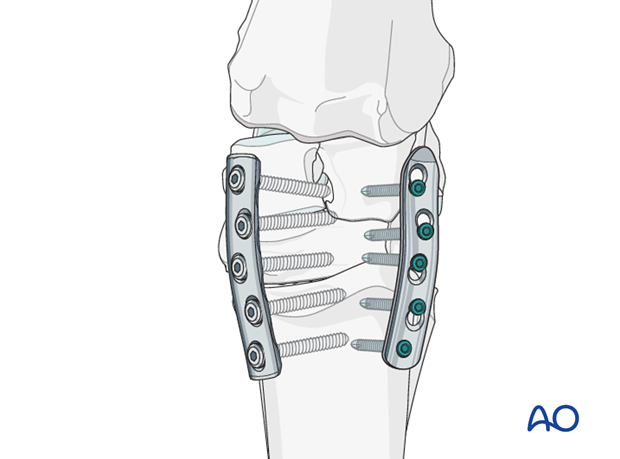
Application of the first plate
For a middle carpal joint arthrodesis, the medial plate is attached proximally into the radial carpal bone first and extended onto McIII.
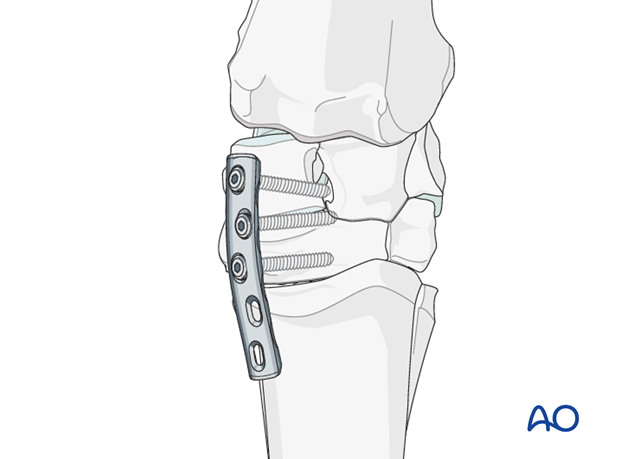
Once the plate is attached proximally the tension device is attached to the distal end of the plate and used for creating axial compression across the osteotomy site. Normally only the first plate requires the use of the tension device. The second implant can be placed in compression using the dynamic compression holes. If no osteotomy is present and significant reduction of a deformity is not necessary the dynamic compression capabilities of the implant may be sufficient to achieve compression across the joint to be fused.
The tension device is always placed distally with the screw attaching the tension device in McIII.
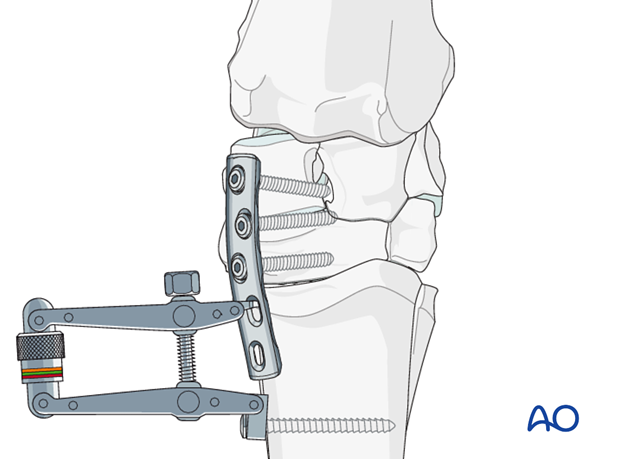
Once sufficient compression is achieved using the tension device in the first plate, the remaining screws are inserted into the third carpal bone and proximal McIII.
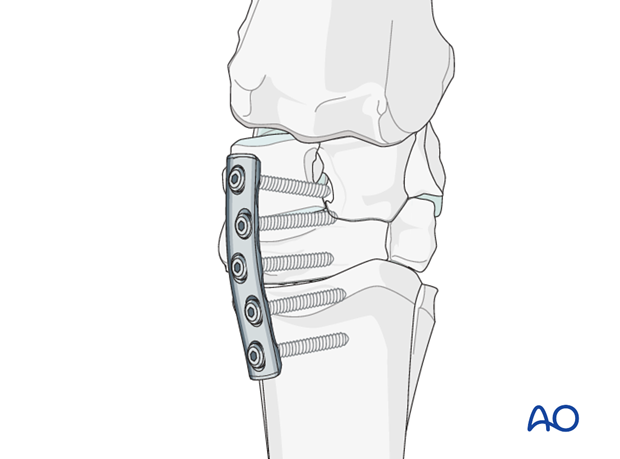
Application of the second plate
The tension device is removed and the second plate is attached using appropriate dynamic compression or locking plate principles.

Radiographic confirmation
Radiographs are taken after all screws are inserted to assure that all screws are in the proper location and the joint is been well reduced.
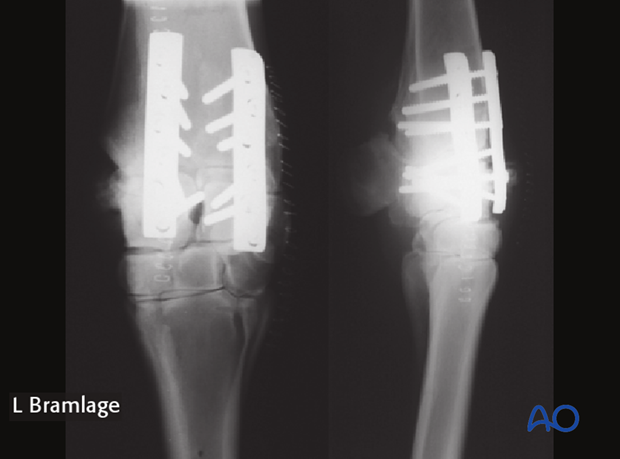
6. Closure
Antibiotic containing implants (PMMA beads or collagen sponges) are placed alongside both plates and the exposure closed using the annular ligament of the carpus, the subcutaneous tissue and the skin sequentially.
Suction drainage may be used in cases with considerable intraoperative manipulation or in cases of trauma induced carpal injury.
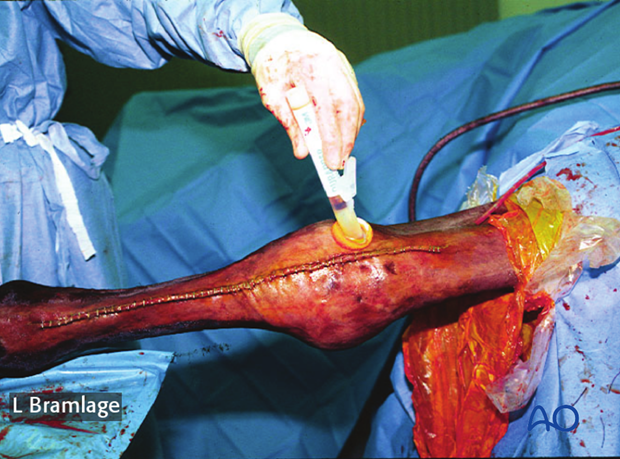
7. Aftercare
After closure a sterile dressing is placed on the wound and a cast is applied from the elbow to the distal aspect of the metacarpus just above the metacarpophalangeal joint. Allowing the metacarpophalangeal joint to maintain flexion and extension greatly increases the ability of the horse to move comfortably postoperatively.
The cast is maintained in place for 30 days with a cast change at 2 weeks postoperatively. The cast change can be performed standing or under general anesthesia depending on patient compliance.
After cast removal full limb bandages are maintained until swelling is eliminated.
Stall rest with no free-choice exercise is maintained for 60 days.
Follow up radiographs at 60 days will determine the next step in the reconvalescent period. Normally 30 days of gradually increasing exercise is recommended prior to resumption of free-choice exercise. Partial arthrodesis is for non-athletic purposes only.