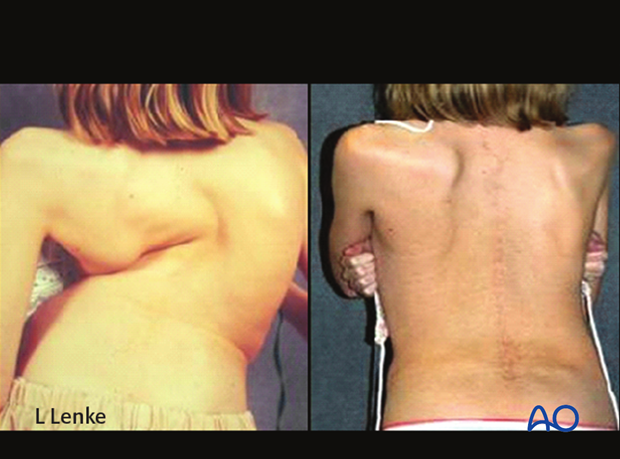
Management of large curves in the spine
1. Introduction
X-ray categorization of large curves
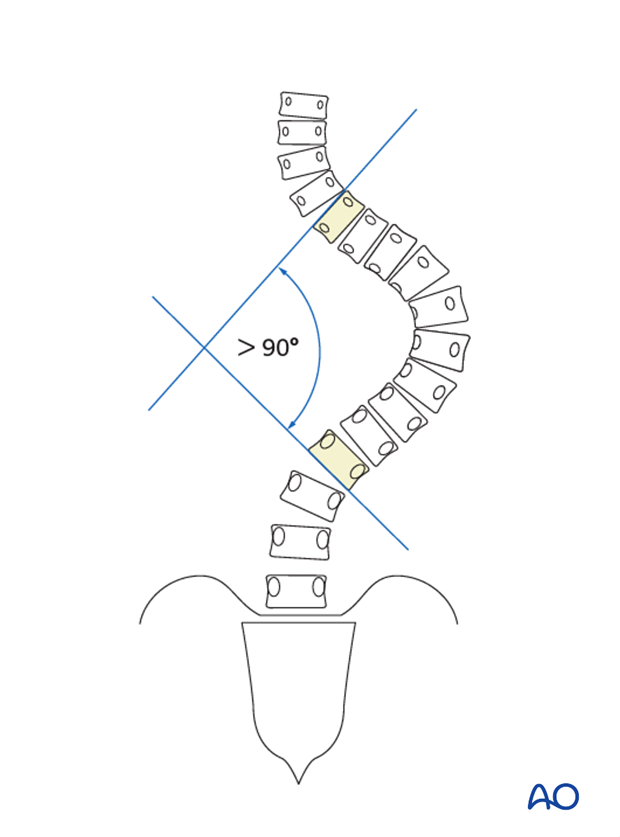
The definition of large curves is curves with a Cobb measurement larger than 90° and in addition to the curve size one must look at curve flexibility when assessing a large curve.
This author prefers to subdivide these curves into three categories:
- 90°–110° Cobb measurement; flexibility greater than 50%,
- 111°–130° Cobb measurement; flexibility between 30 and 50%.
- >131° Cobb measurement and less than 30% flexibility.
Additional patient assessment
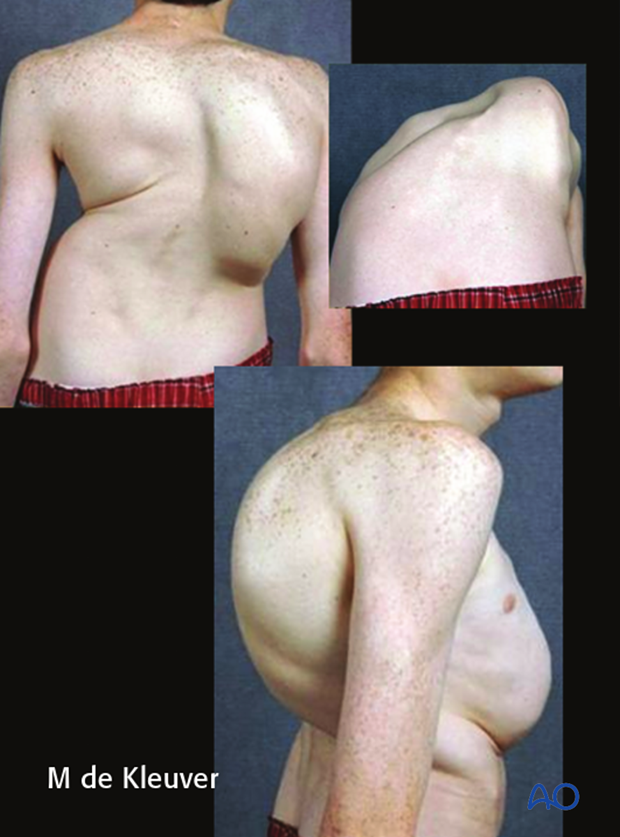
One must look carefully at the overall clinical appearance of patients with large curves to assess their preoperative shoulder balance, pelvic tilt, trunk shift, any coronal or sagittal imbalance or any waist line asymmetry. Although these are all part of the normal AIS patient assessment, because of the more severe curvatures and thus corresponding clinical deformity, the effect of surgical correction to optimize the postoperative clinical image is even more important.
It is also important to assess pulmonary function preoperatively as larger curves tend to produce greater pulmonary restrictive disease. This will directly impact the choice of surgical treatment and subsequent risk of pulmonary complications postoperatively.
2. Treatment options
The anterior only approach is almost always not advisable for large curves as the operative approach is quite difficult to gain access to the upper and lower end vertebrae. In addition the vertebrae at the ends and apex of the curve are often osteoporotic and do not hold screws very well. Thus the two main options for large curves are a combined anterior and posterior procedure or a posterior only procedure utilizing various forms of spinal osteotomies.
Anterior and posterior procedure
A combined anterior spinal fusion (ASF) followed by a posterior spinal fusion (PSF) with posterior instrumentation is still considered the primary means of correcting large AIS curves. The ASF procedure can be performed either thorascopically or via an open thoracotomy or thoracoabdominal approach. The goal of the ASF procedure is to release the anterior ligaments and remove the anterior disks. This provides increasing spinal flexibility as well as providing for a necessary anterior fusion via placement of bone graft into the dissected disc regions. The use of structural bone grafts or cages may be considered in the lumbar region. The PSF procedure then follows with further correction of the deformity with placement of posterior instrumentation performed along with a posterior fusion.
Posterior only procedure using spinal osteotomies
In the last decade it is becoming more accepted to approach large and stiff AIS curves through a posterior only approach utilizing various types of spinal osteotomies. Typically, these patients are treated with segmental pedicle screw fixation which provides the necessary instrumentation power to afford acceptable and safe curve correction. Spinal osteotomies are performed to release the large and stiff curve and can be performed through the posterior procedure. Thus, pedicle screw fixation provides the required instrumentation security while spinal osteotomies provides the required carpentry to release the large and stiff curvature.
3. Spinal osteotomies
There are three main choices for spinal osteotomies to release the spine during a posterior scoliosis procedure:
- Posterior column osteotomy (PCO).
- Pedicle subtraction osteotomy (PSO)
- Vertebral column resection (VCR)
4. Posterior column osteotomy (PCO)
PCO is also called SPO (Smith-Petersen osteotomy) or Ponte osteotomy.
The inferior aspect of the spinous process is removed followed by the removal of the inter spinous ligament utilizing a standard rongeur.
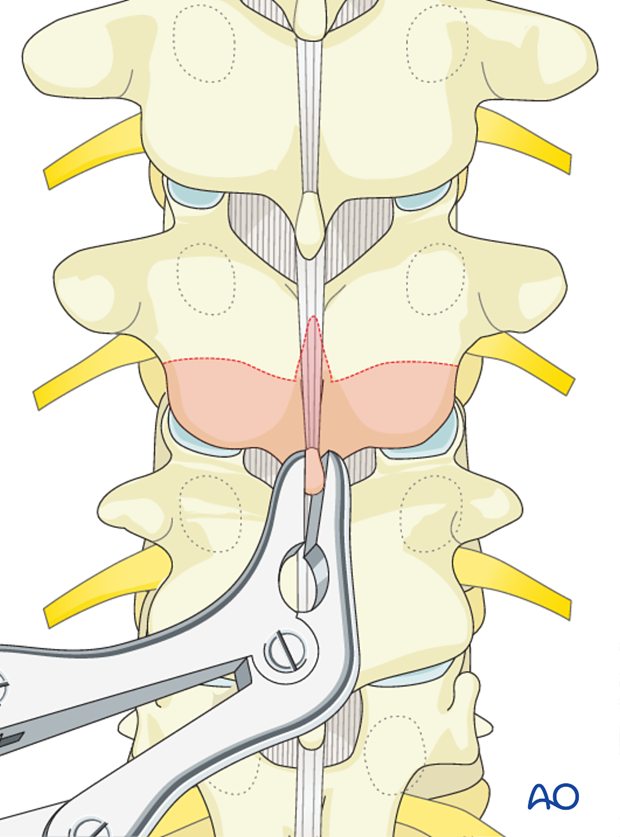
The ligamentum flavum is removed with a Kerrison rongeur, It is important not to penetrate deeply against the dura or tear the dura.
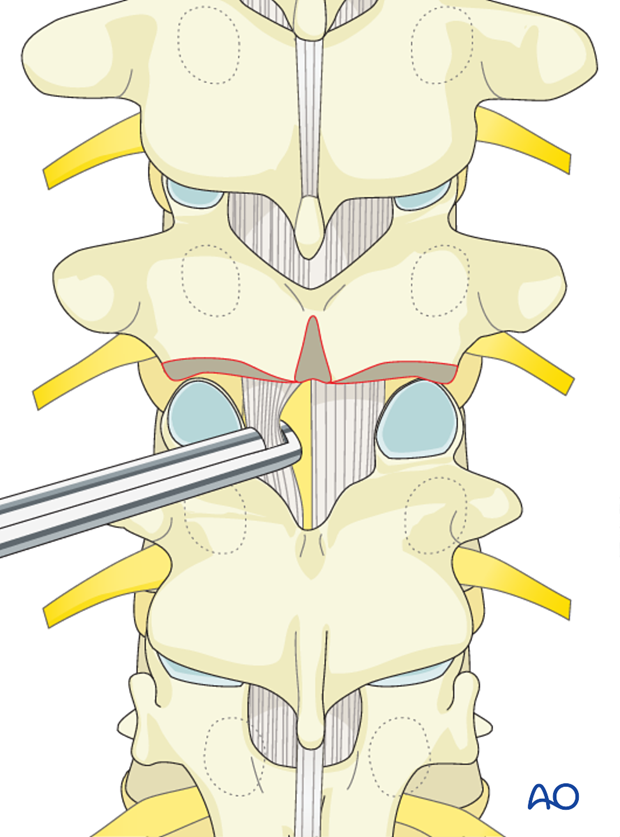
Then bilateral facet joints are removed either with a Kerrison rongeur or a high speed burr.
Care should be taken not to tear the dura particularly on the concavity of the curve where the neuro tissues lie, so as not to compromise the neurological function.

5. Pedicle subtraction osteotomy (PSO)
PCO's are performed at the upper and lower level of the planned PSO vertebra.
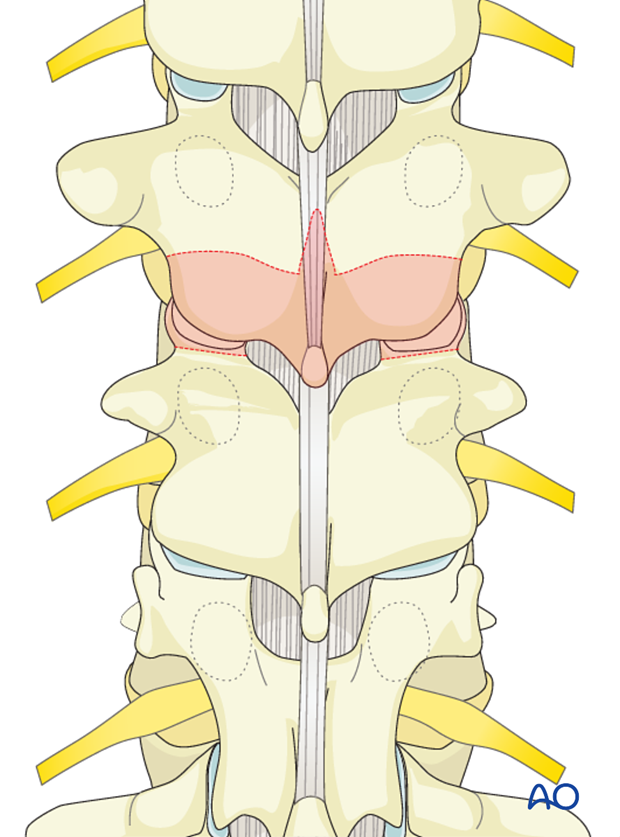
Utilizing a Kerrison rongeur, a laminectomy is performed from the mid-pars region of the vertebra cephalad to the PSO vertebra distal to the lower pars level of the PSO vertebra.
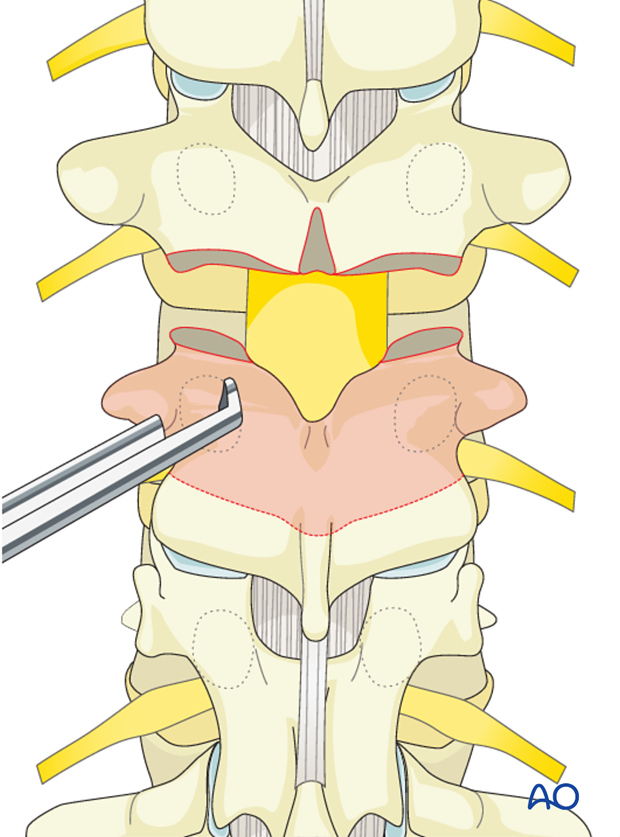
Both pedicles are surrounded and removed down to the base of the vertebral body, carefully protecting the exiting nerve roots which lie against the medial and inferior aspect of the pedicle.
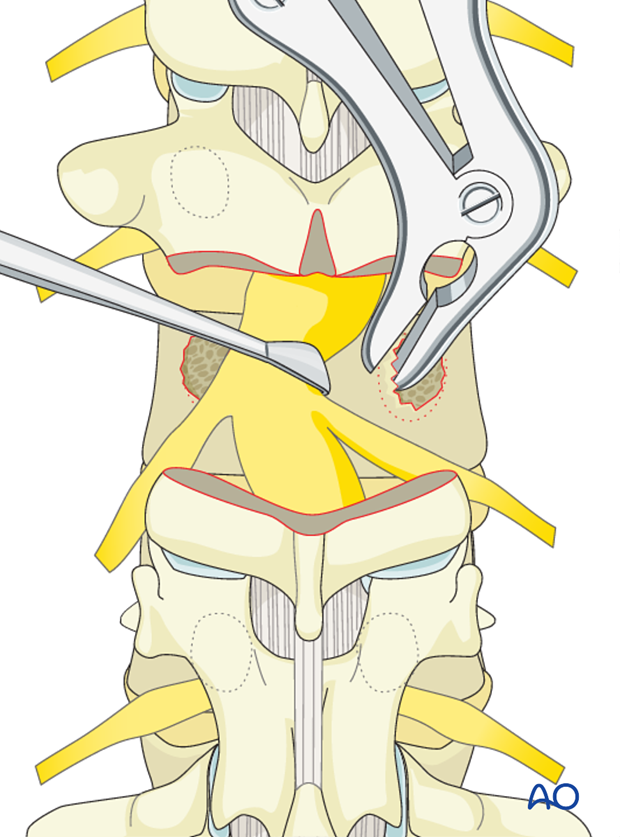
The vertebral body is then decancellated of the cancellous bone in order to thin out the vertebra and provide collapse and wedging of that segment. Any available bone graft is removed and saved for later use as fusion material.
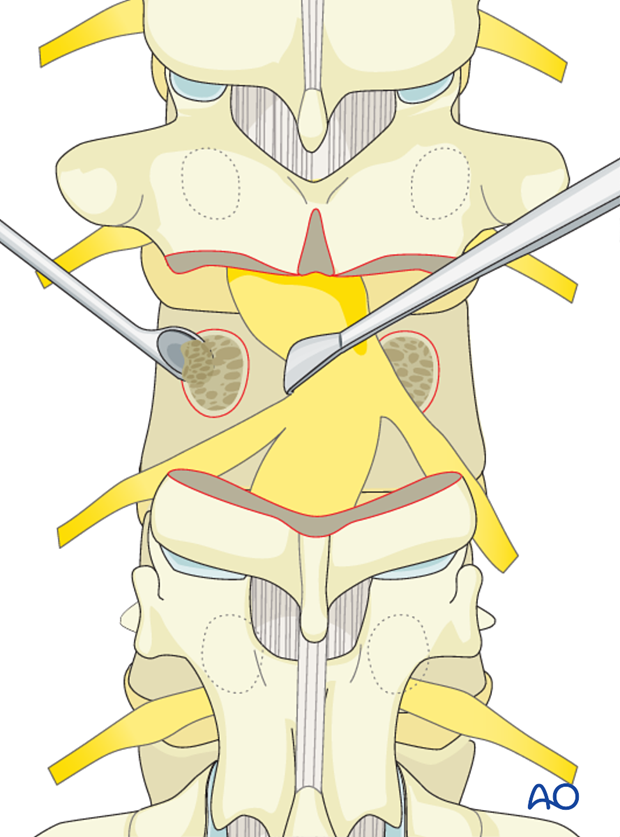
Both lateral portions of the PSO body are exposed subperiosteally and a wedge of the lateral vertebral body is removed from superficial to deep.
It is important to avoid injury to the segmental artery and vein which lies just lateral to the vertebral body.
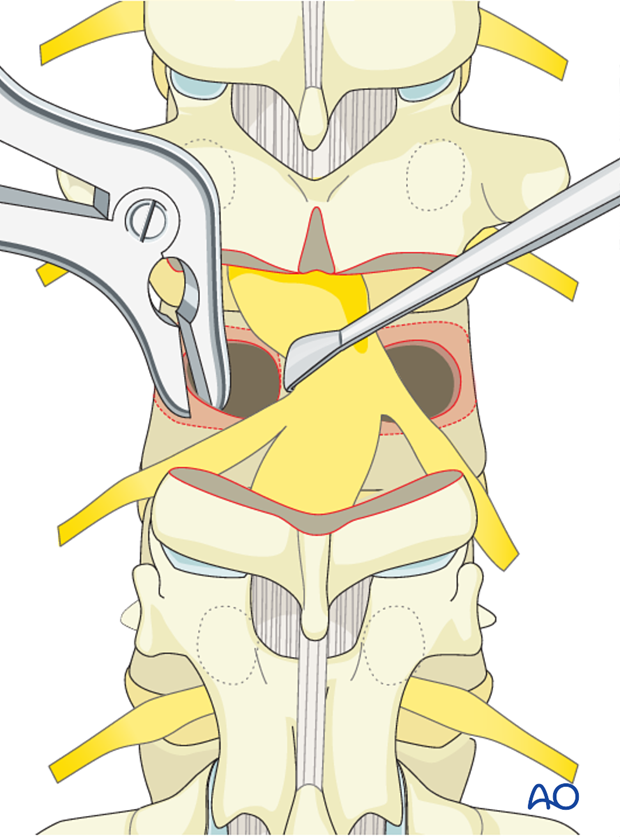
The posterior vertebral body wall is then carefully dissected from the ventral dural surface.
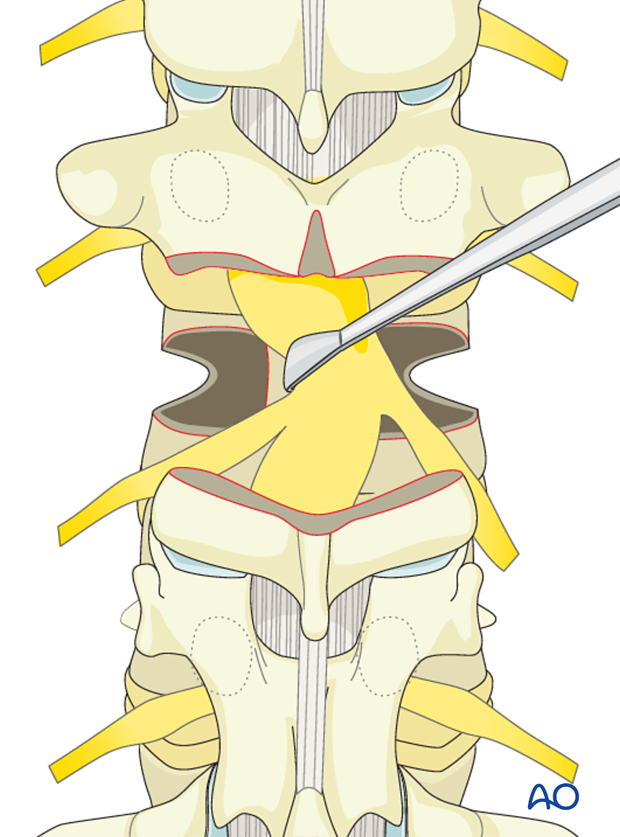
The posterior wall is impaled into the vertebral body thus freeing up the entire ventral dural surface. It is important not to place excessive stretch or tension on the dura during this procedure.
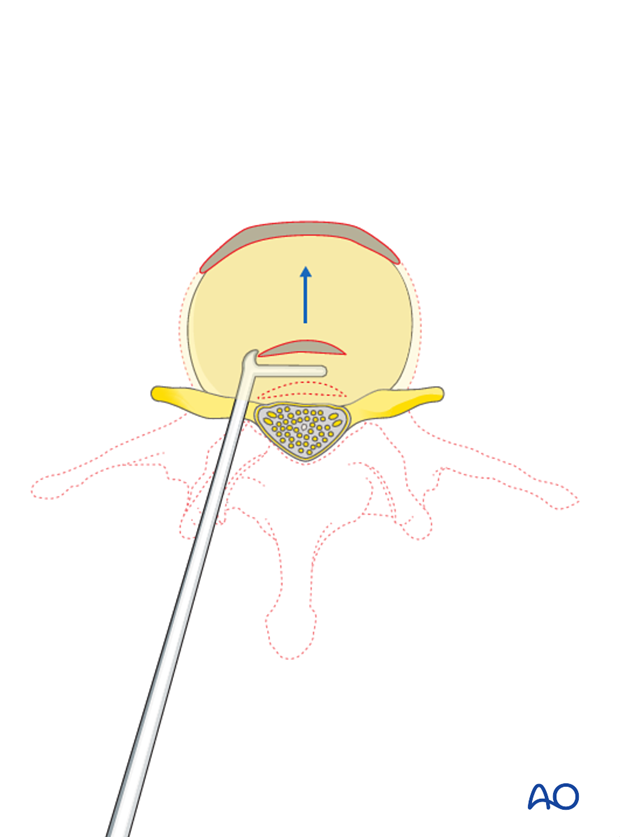
The PSO vertebra is then ready to collapse which provides the increased segmental and regional flexibility for improved correction of large scoliotic curves.
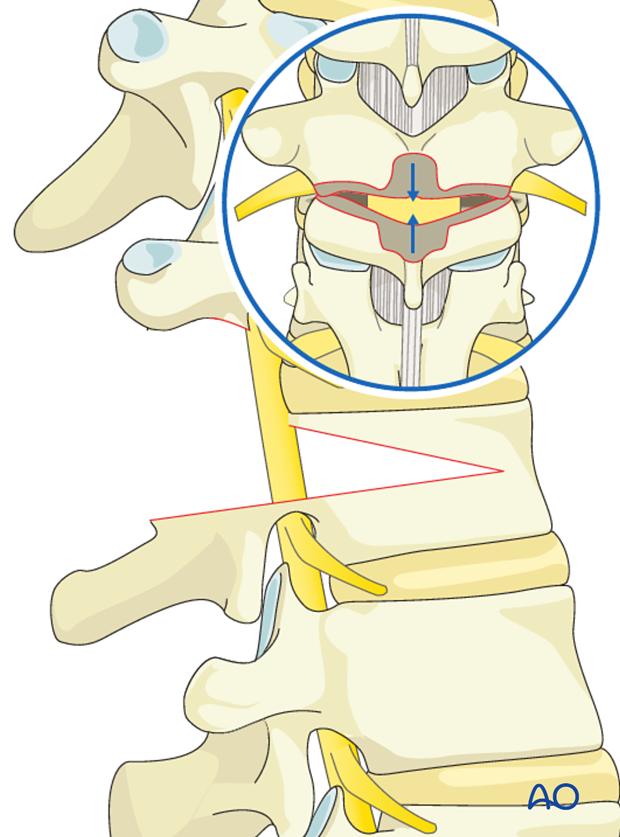
6. Vertebral column resection (VCR)
PCO's are performed above and below the planned VCR level.
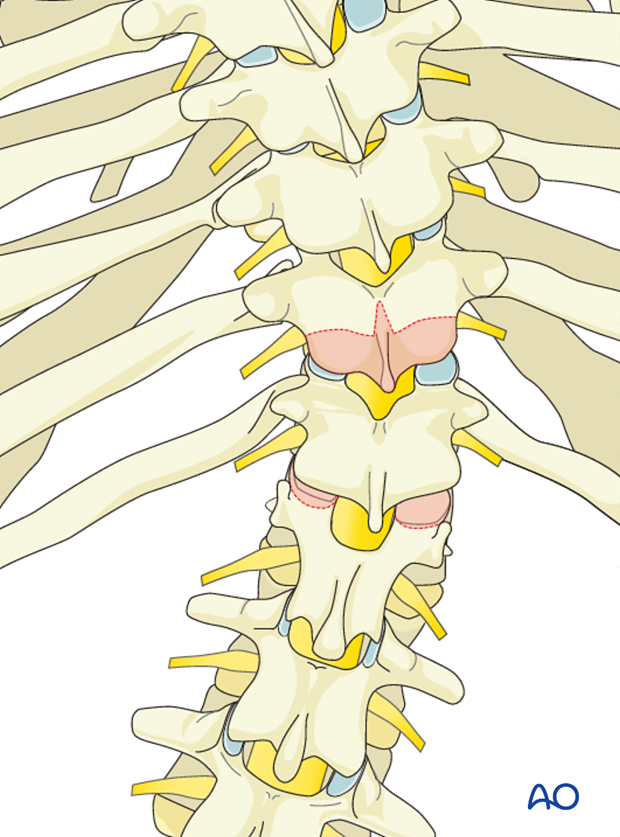
In the thoracic spine bilateral costotransversectomies are performed removing 4-5 cm of the adjacent ribs at the apical level to be resected while protecting the pleura from inadvertent penetration.
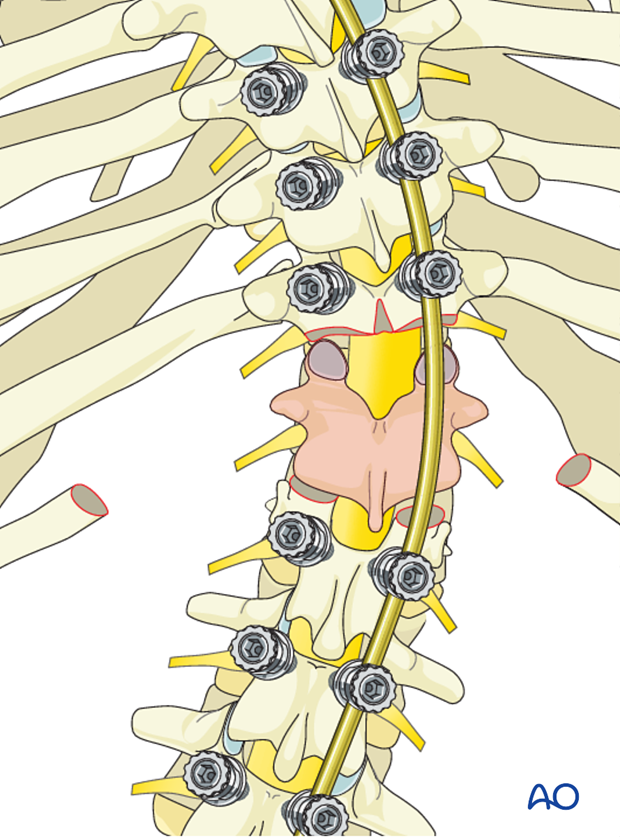
Segmental pedicle screws are placed at the predetermined levels and a temporary rod is placed on one side of the spine capturing three levels above and below the planned resection site.
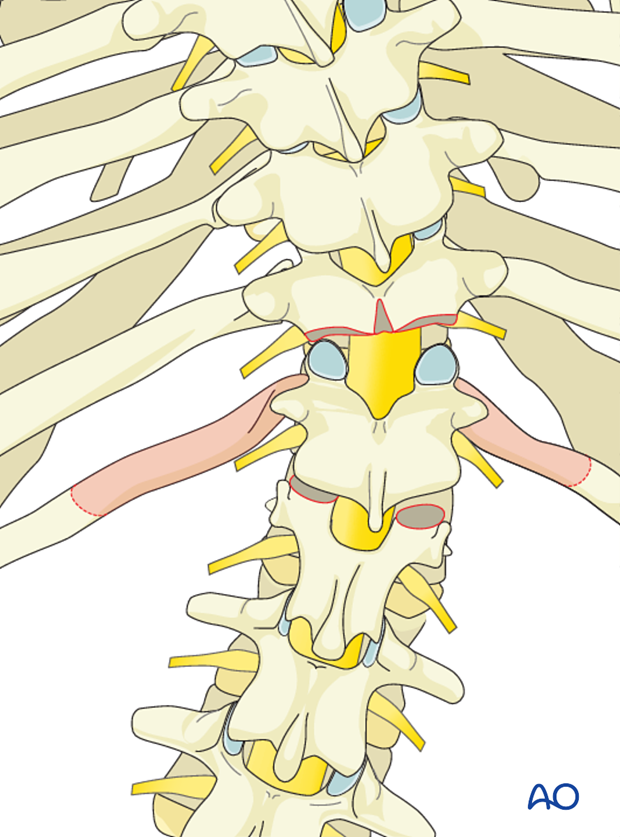
A laminectomy is performed of the entire lamina of the vertebra to be resected extending cephalad to the pars level of the supra adjacent vertebra.
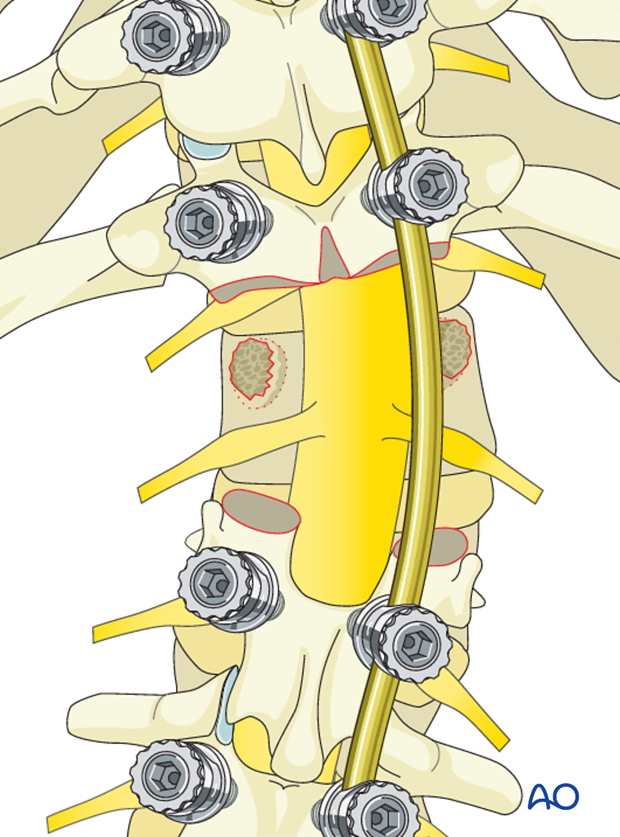
In the thoracic spine one may elect to sacrifice one or both exiting nerve roots to provide increased exposure for the removal of the vertebral body.
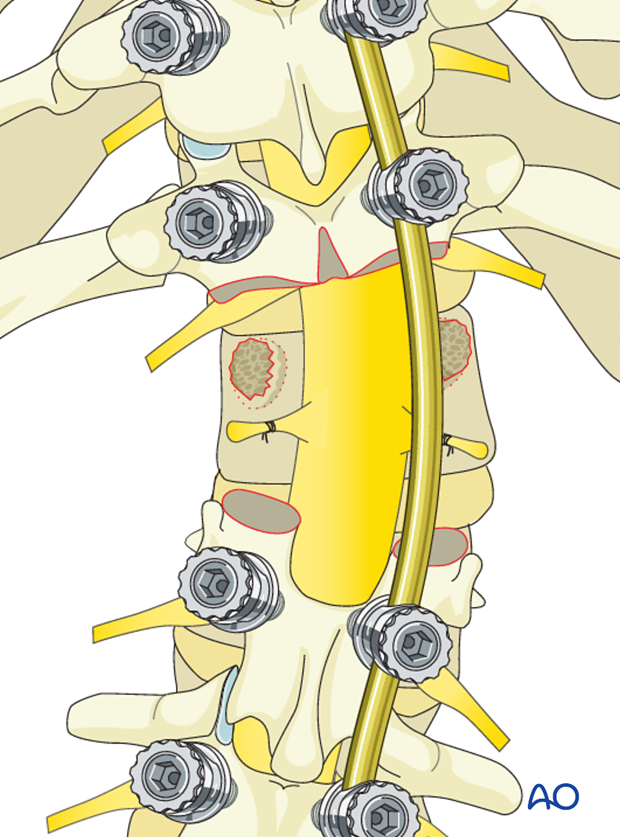
Both pedicles are surrounded and removed down to the base of the vertebral body carefully protecting the exiting nerve roots which lie against the medial and inferior aspect of the pedicle. One must be very careful removing the concave pedicle as the spinal cord rest directly against the structure. Careful dural protection along with minimal retraction is absolutely necessary. Often it is necessary to use a high speed burr to carefully remove the often cortical concave pedicle bone.
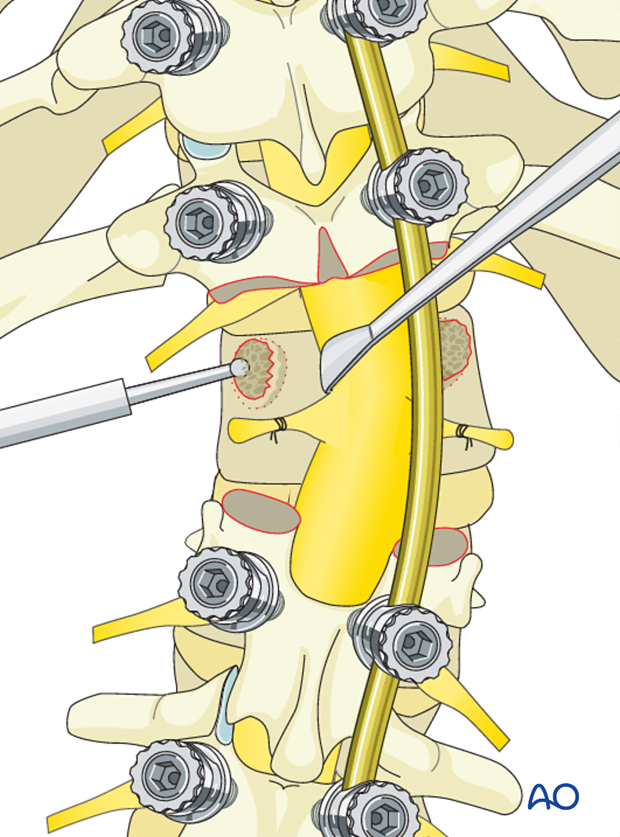
The vertebral body is then decancellated of the cancellous bone in order to thin out the vertebra. The majority of this decancellation is performed on the convex side of the curve. It is advisable to save as much bone as possible to use in the fusion.
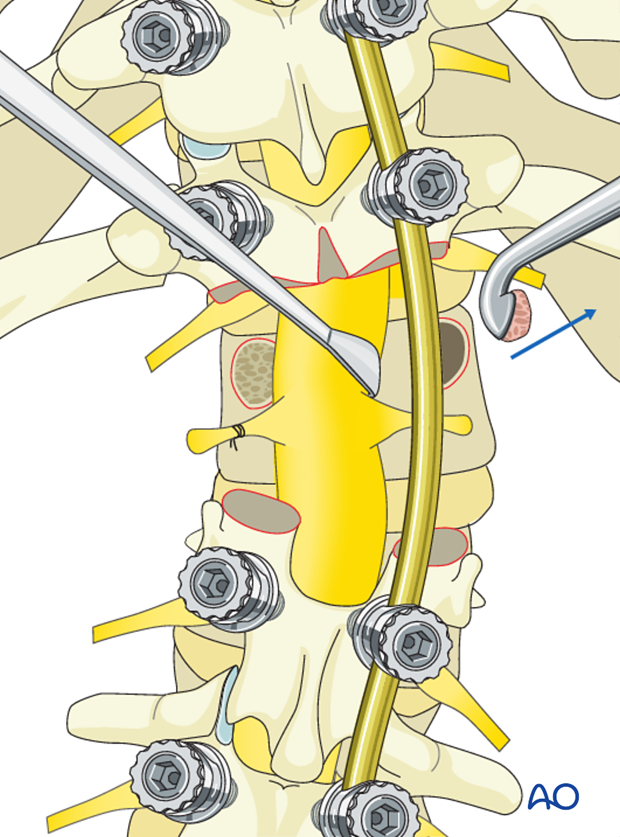
The lateral vertebral body walls are then subperiosteally exposed. It is important to place a protective instrument against the anterior lateral vertebral body to safely protect the adjacent viscera and vasculature from harm.
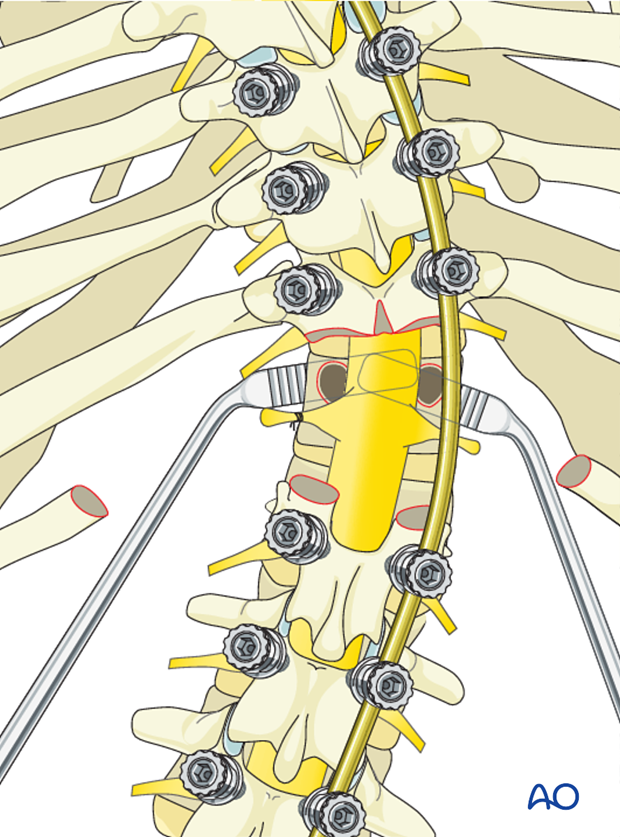
The lateral vertebral body walls are then removed allowing entrance into the remainder of the vertebral body.
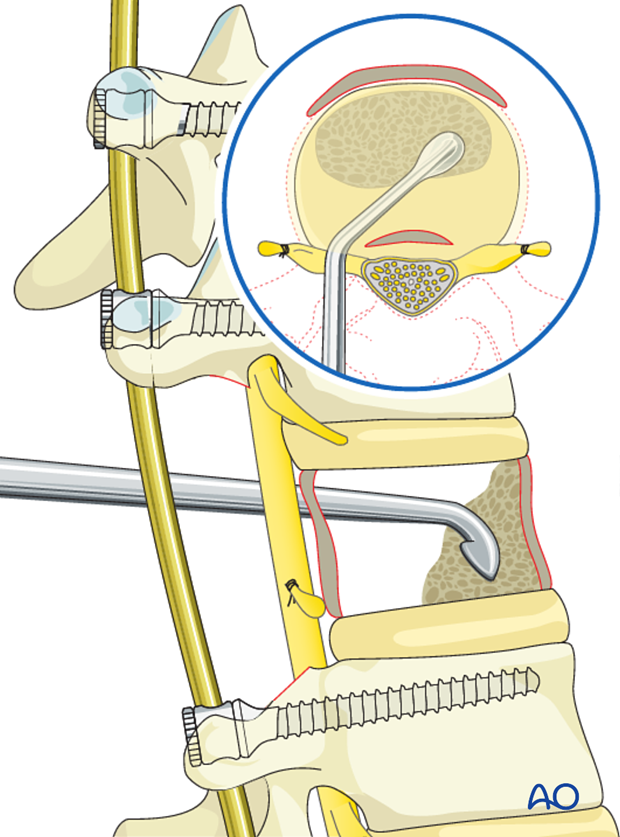
The remainder of the cancellous portion of the vertebra is completely removed to the endplates of the adjacent disks above and below. The bone removed is saved for fusion. Both the anterior and posterior walls of the vertebra are left intact.
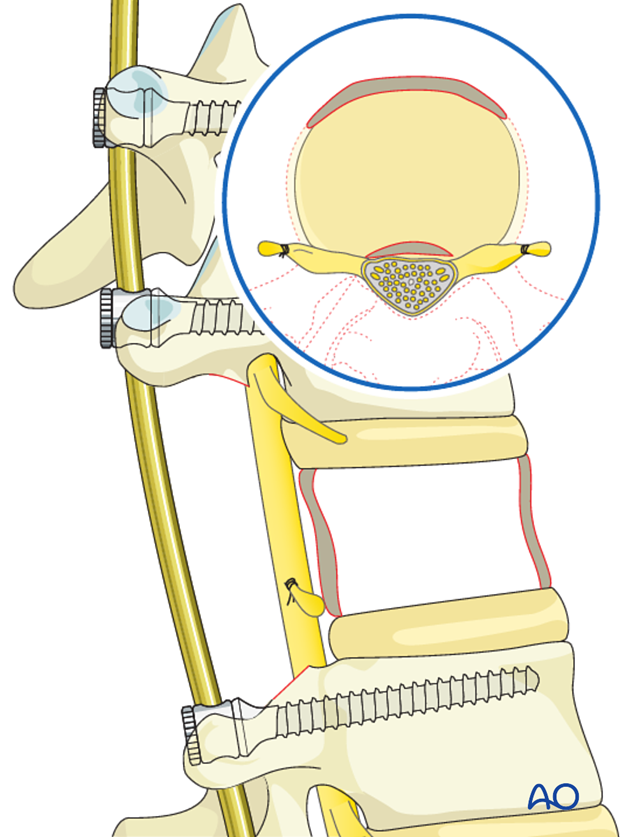
The discs cephalad and caudad to the resected vertebra are then removed.
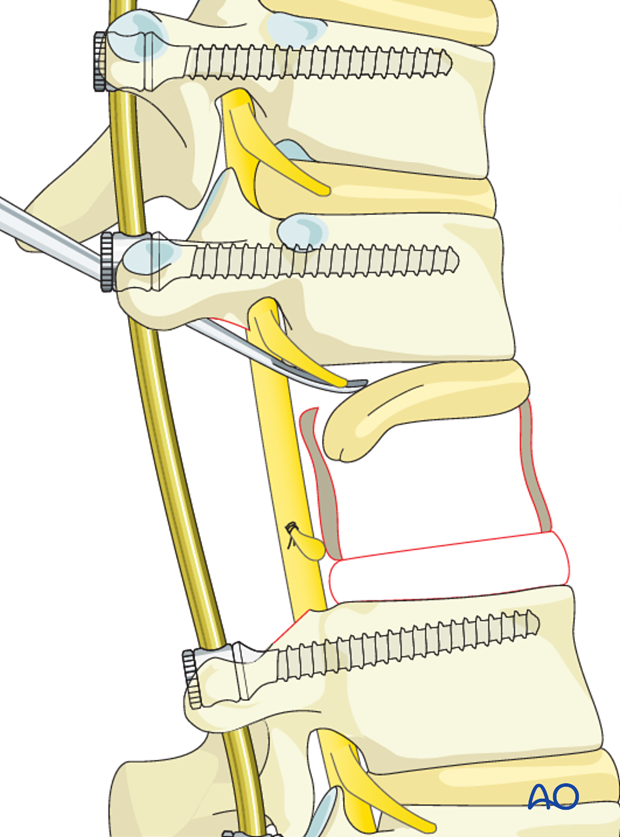
The posterior vertebral body wall is then carefully dissected from the ventral dural surface. The posterior wall is impaled into the vertebral body thus freeing up the entire ventral dural surface. It is important not to place excessive stretch or tension on the dura during this procedure.
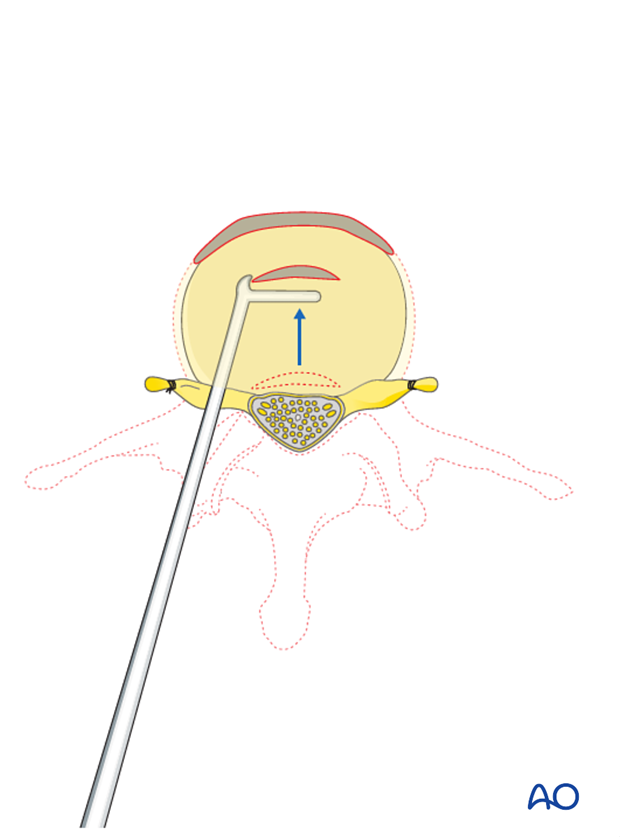
The deformity is then ready for correction by the temporary instrumentation, always beginning with spinal shortening by convex rod compression to avoid excessive stretch on spinal cord.
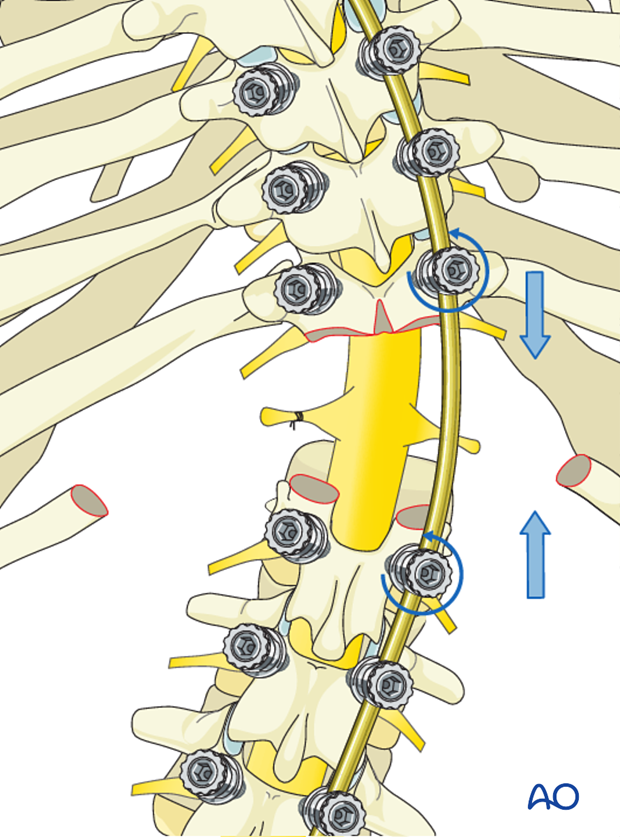
After the spine is shortened, correction via concave distraction and translation can safely occur.
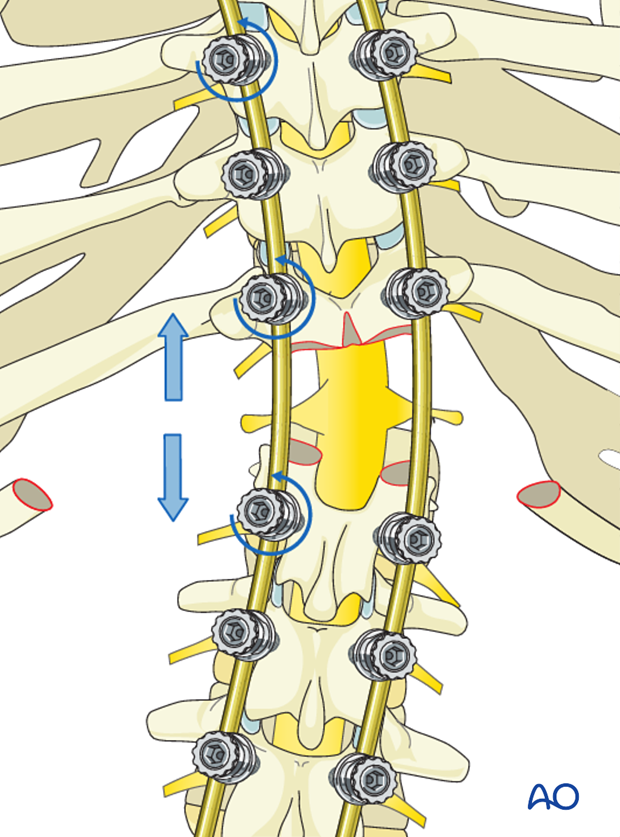
Prior to complete correction an appropriate sized metallic cage is placed into the anterior defect, filled with bone graft, supplying structural support to the anterior column of the spine. Final posterior rod correction is performed with the permanent rods locking in this anterior cage.
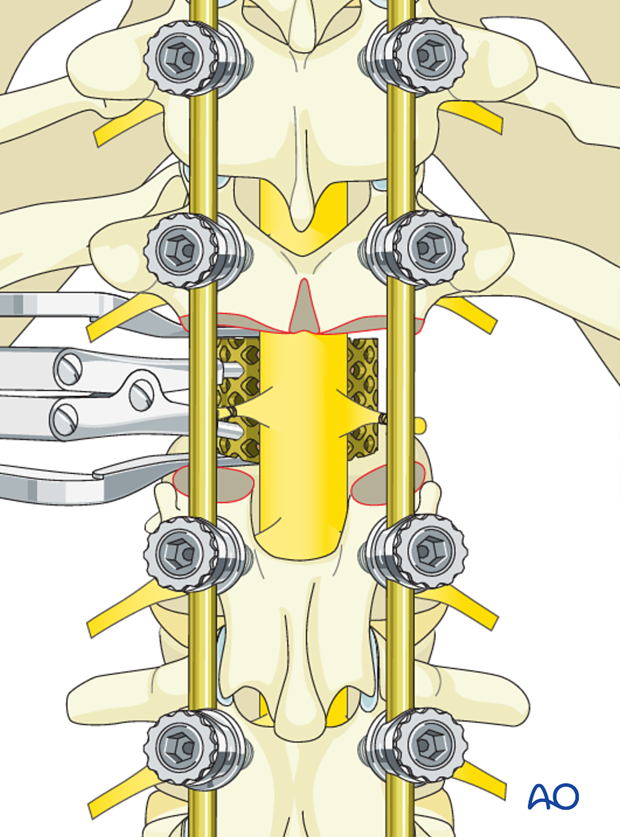
The dural sac is protected using some form of fibrin glue type of material.
Following decortication and posterior fusion, the rib pieces previously removed are split longitudinally and placed over the laminectomy defect in order to both provide dural protection and afford a posterior osseous fusion of the VCR site.
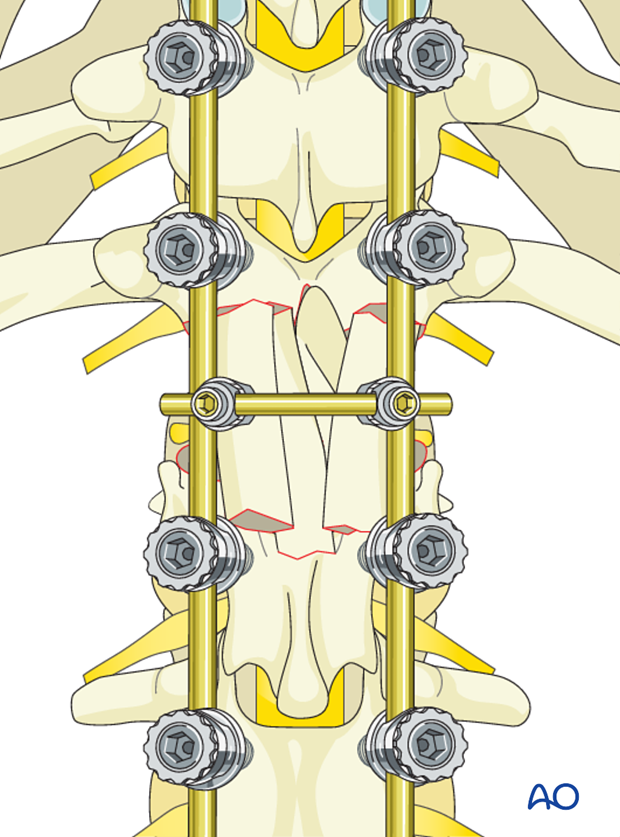
7. Case examples
Anterior posterior procedure
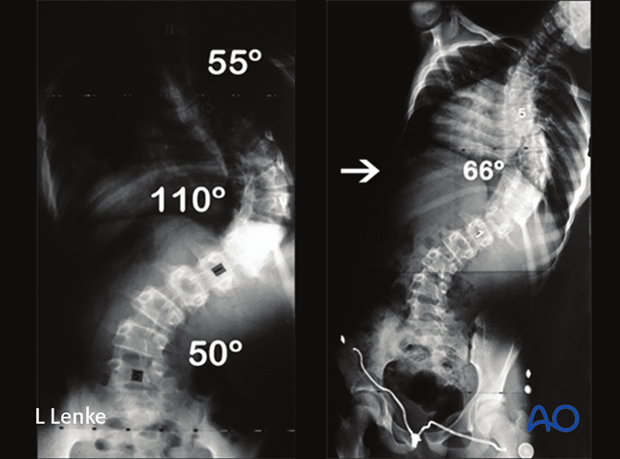
This is a teenage AIS patient with a 110° large MT curve, bending out to 66° preoperatively.
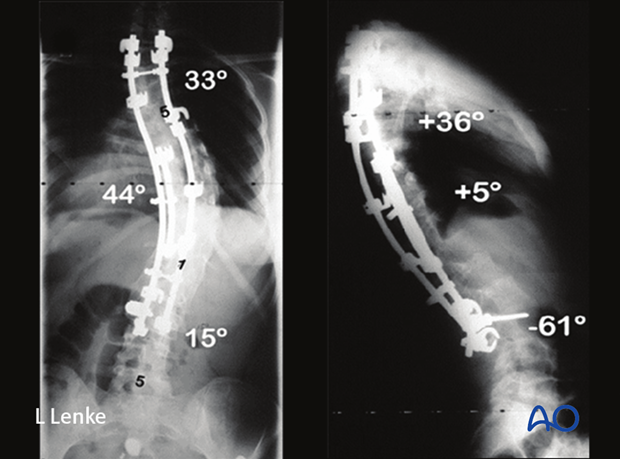
She underwent a same day ASF/PSF with hybrid instrumentation showing correction to 44° at 6 years postoperative.
Pre and post-operative clinical photos demonstrate the clinical correction as well as the anterior and posterior scars.
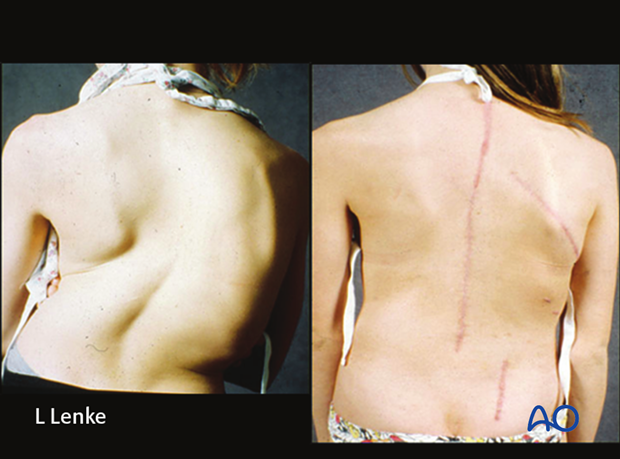
PCO
This is a 12 year old female with a 90° MT curve correcting to only 60° on side bending.
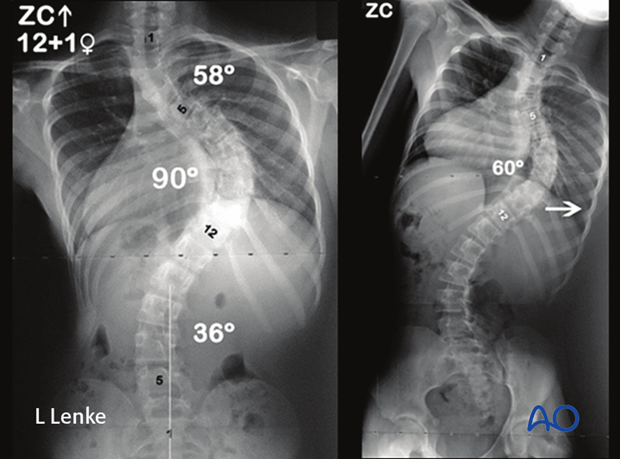
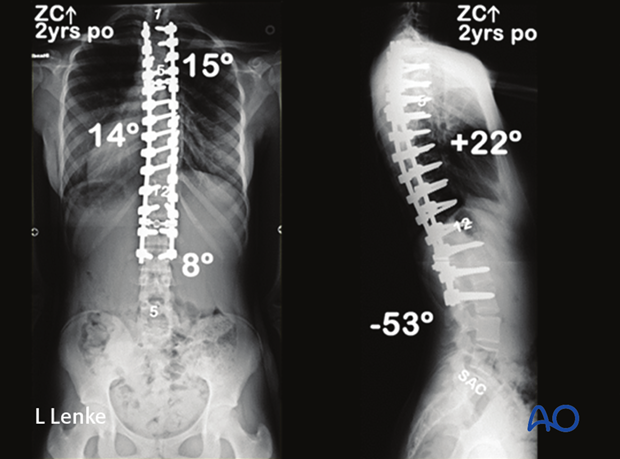
She underwent a PSF from the T2-L2 with 5 levels of PCO's at the apex for correction to 15° at 5 years postoperative.
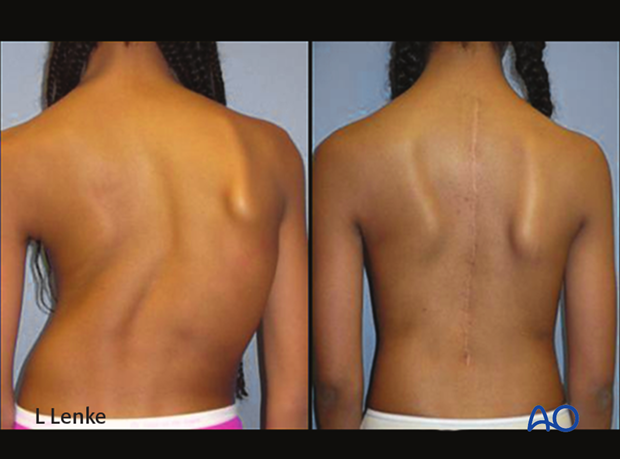
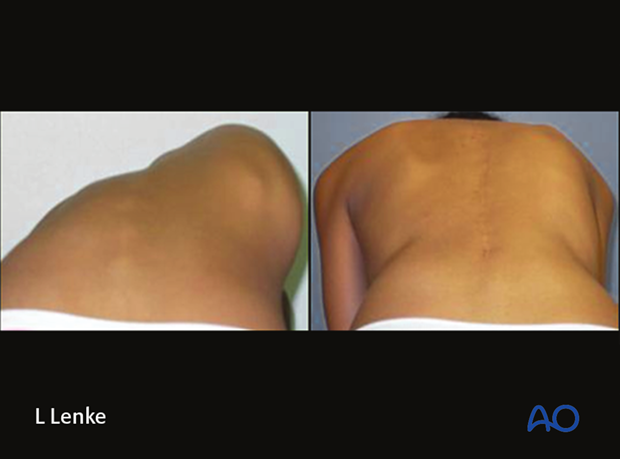
Pre and post-operative clinical photos illustrate her markedly improved clinical correction.
PSO
This case is a 12 years, 5 months female with 111° scoliosis correction only to 108° on side bending. There also is associated hyper kyphosis of 115°.
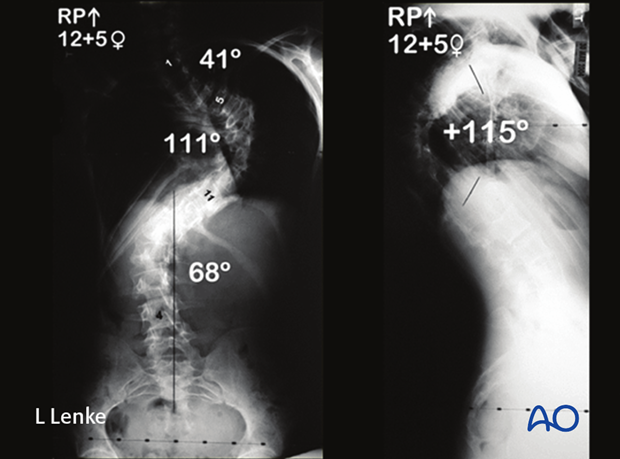
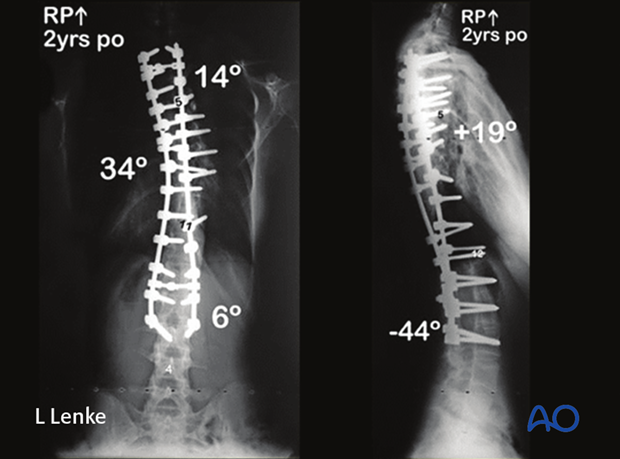
She underwent a PSF from T2–L3 with an apical PSO for correction of her idiopathic kyphoscoliotic deformity. Her marked correction is seen at her postoperative AP and lateral radiographs.
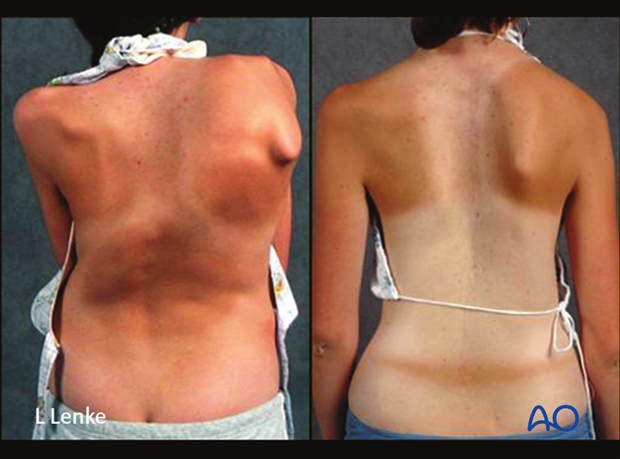
Her preoperative and postoperative clinical photographs demonstrate the marked correction of her trunk and rib cage following the surgery.
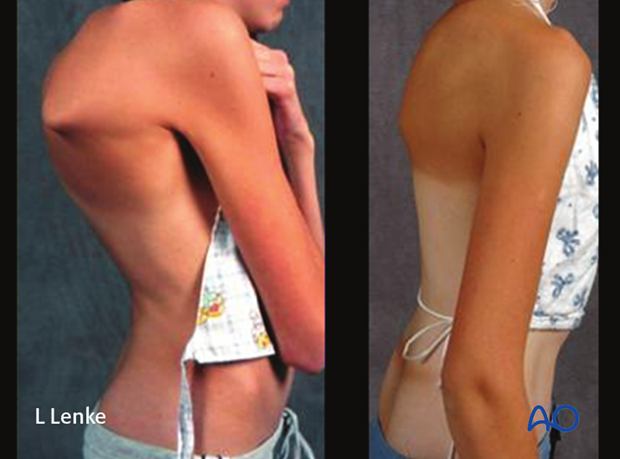
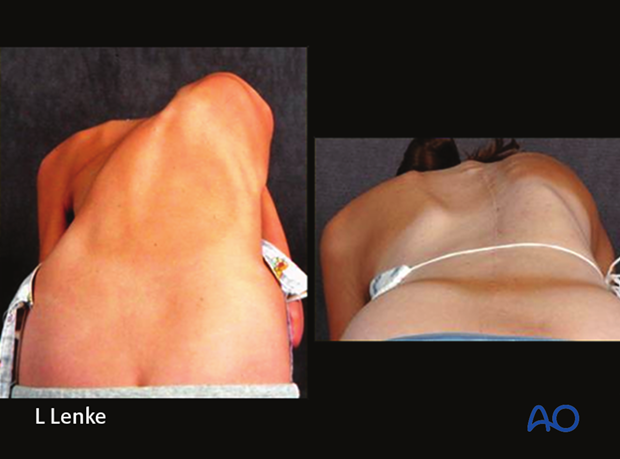
VCR
This 12 year, 6 month old female presented with a severe 159° MT scoliosis curve with correction only 135° on side bending.
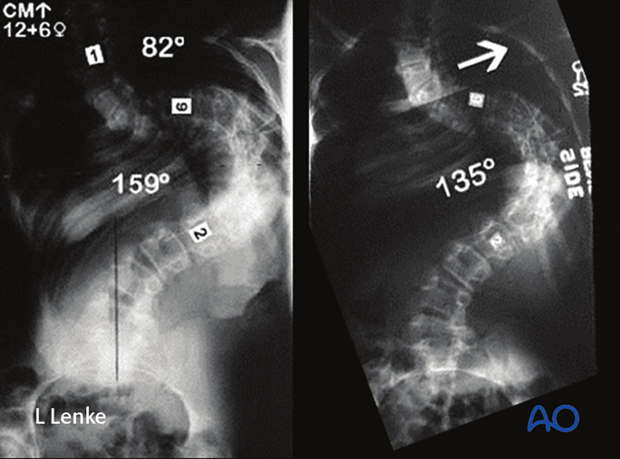
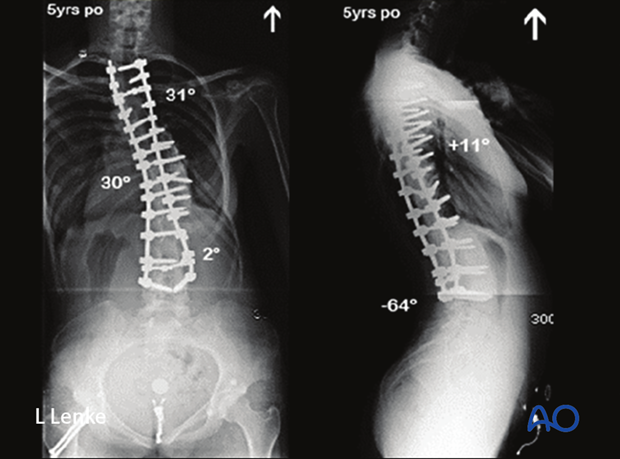
She underwent a 1 level VCR and PSF from T2–L4 for correction of her MT curve 30° at 5 years postoperative.
Pre and postoperative clinical photos illustrate the normalization of her severe truncal malalignment as well as a 6 inch gain in height after surgery.
Pre and postoperative clinical photos illustrate the normalization of her severe truncal malalignment as well as a 6 inch gain in height after surgery.