Trochanteric femoral fracture
General considerations
Trochanteric fractures can occur because of a direct impact or avulsion type injuries. Rarely these fractures can involve a twisting mechanism with a spiral morphology. These fractures can also occur intraoperatively during femoral instrumentation. Critical to diagnosis is the assessment of the stability of the femoral stem and the hip joint.
These fractures are classified by UCPF as IV.3-A.
Fracture to the greater trochanter
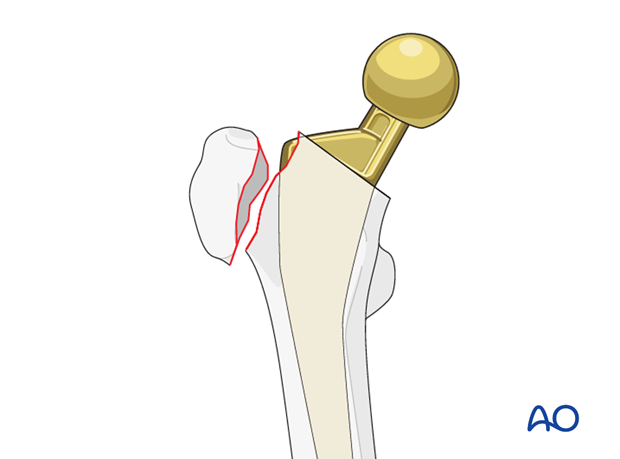
The type IV.3-A1 fracture involves the greater trochanter. The prosthetic stem remains stable.
Typically, a fracture of osteoporotic bone that can occur with simple trauma.
Intraoperative fracture of the greater trochanter more commonly occurs with a direct anterior approach to the hip.
Imaging
AP and lateral radiographs may be required to visualize these fractures. However, if a patient continues to have pain following a trauma with negative radiographs, then a CT scan may be required. Utility of MRI is limited due to inadequacy of metal suppression.
Look for asymmetric liner wear and associated osteolysis.
Fracture to the lesser trochanter
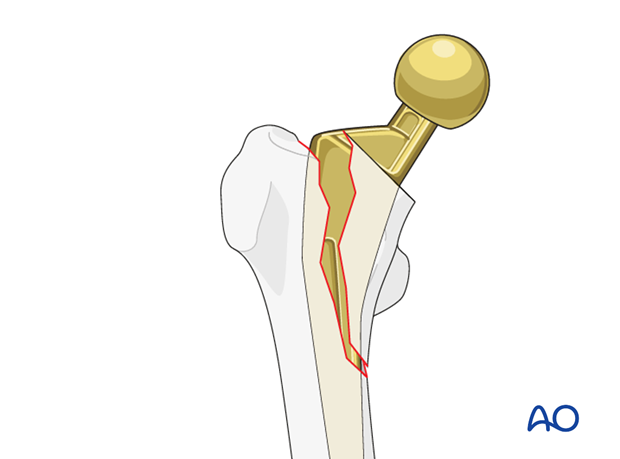
The type IV.3-A2 fracture involves the lesser trochanter. The prosthetic stem remains stable.
These fractures occur most commonly intraoperatively as the femoral stem is being implanted. Careful evaluation of the femoral neck during index surgery is critical to diagnosis. Heightened awareness during hip arthroplasty for femoral neck fractures is important. Lesser trochanter fractures occur more commonly with posterior approach arthroplasty. They can also occur remote to surgery, with a twisting mechanism.
Pathologic fracture must always be considered. Particularly for fractures involving the lesser trochanter.
Imaging
AP and lateral radiographs may be required to visualize these fractures. However, if a patient continues to have pain following a trauma with negative radiographs, then a CT scan may be required. Utility of MRI is limited due to inadequacy of metal suppression.
Look for asymmetric liner wear and associated osteolysis.













