Posterolateral (Boyd) approach to the pediatric proximal radius and ulna
1. Introduction
In proximal ulnar injuries associated with radial head dislocation or radial neck fractures, both bones can be addressed through a lateral extension of a posterior skin incision (Boyd).
This combined approach also provides the most convenient access for annular ligament reconstruction, a procedure which is rarely required in the acute setting.
2. Skin incision
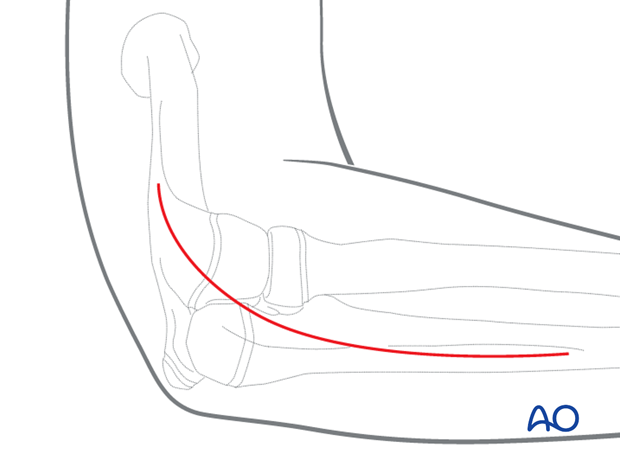
The Boyd approach can be performed through a posterolateral incision.
Start the incision laterally at the supracondylar ridge at the level of the superior border of the forearm and continue slightly more lateral crossing directly over the lateral epicondyle.
Extend the incision as far distally as desired as the direct (subcutaneous) approach to the ulnar shaft.
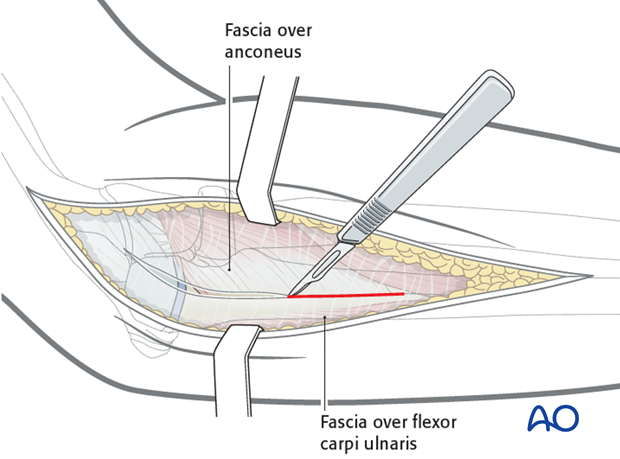
3. Superficial dissection
Incise the deep fascia in line with the incision to approach the lateral margin of the ulna between the anconeus insertion and the flexor carpi ulnaris.
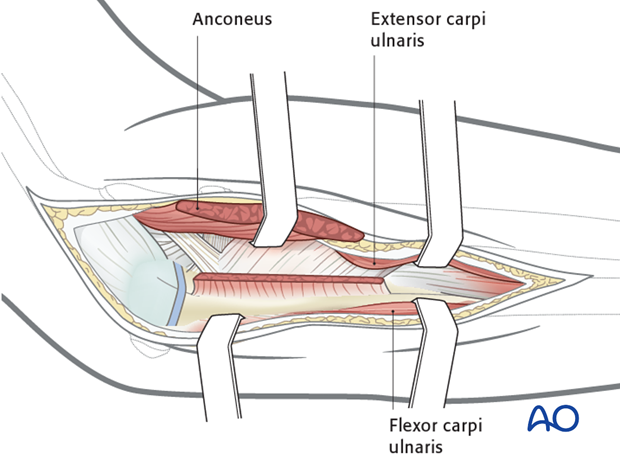
4. Exposure of posterior surface of the ulna
Expose the ulna behind the anconeus proximally and extensor carpi ulnaris more distally.
A plate applied to the posterior surface of the proximal ulna will lie on the apex of the ulnar diaphysis.
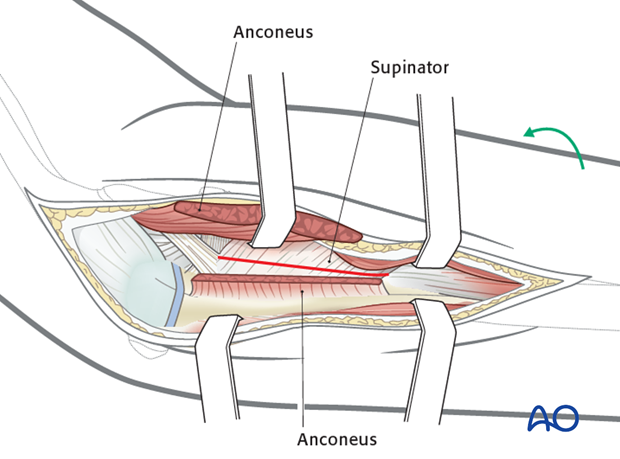
5. Exposure of radial head/neck
Reflect the anconeus anteriorly/laterally after incising its ulnar insertion.
Detach the supinator near its ulnar origin.
Hold the forearm in a pronated position to keep the posterior interosseous nerve away from the surgical field and limit distal dissection.
Elevate the anconeus and supinator muscles, carefully protecting the posterior interosseous nerve, which is within the substance of the supinator. Supinator may need to be separated from the oblique cord of the interosseous membrane.
By retracting these muscles, expose the posterior joint capsule over the radial head.
Pitfall: Do not place retractors around the radius as this may injure the PIN.
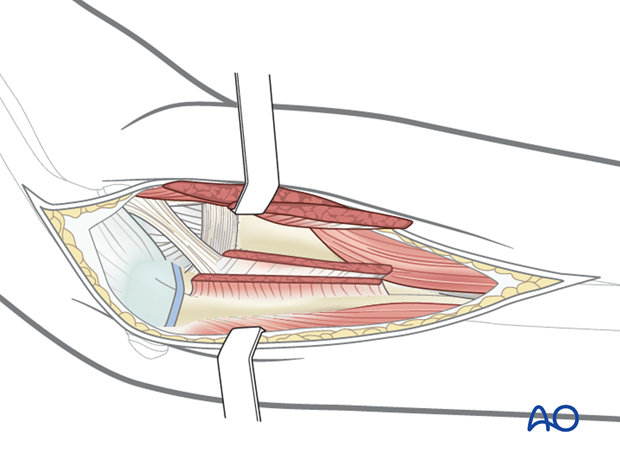
Now that the capsule is exposed, the radial head can easily be exposed.
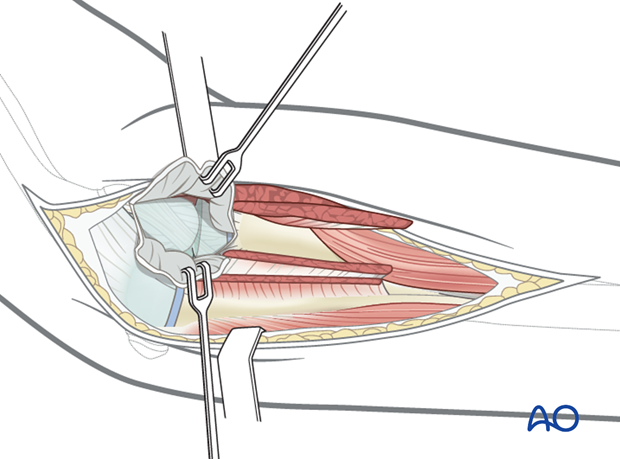
6. Wound closure
Close the capsule with resorbable sutures (3/0).
Reattach the muscles and fascia with resorbable sutures (2/0 or 3/0).
Close skin and subcutaneous tissue with fine resorbable sutures (this avoids distress to the child when removing nonabsorbable sutures).













