Anterior (Henry) approach to the pediatric radius
1. Introduction
The anterior (Henry) approach offers good exposure of the whole length of the radius. The length of the incision depends on the extent of exposure needed. If it is necessary to cross the elbow crease, then a Z-incision is recommended.
The landmarks for the skin incision are:
Proximal
- The biceps tendon, which crosses the front of the elbow joint, medial to the brachioradialis.
- The “mobile wad”, formed from the brachioradialis and the extensors carpi radialis brevis and longus
Distal
- The radial styloid process.
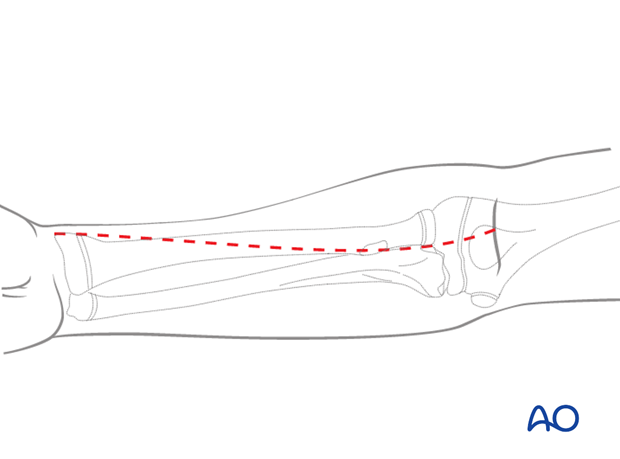
This illustration shows the extent of the incisions for the anterior approaches to the radial shaft:
- Proximal third
- Middle third
- Distal third
Note: The posterolateral (Thompson) approach also offers good access to either the middle or distal third of the radial shaft.
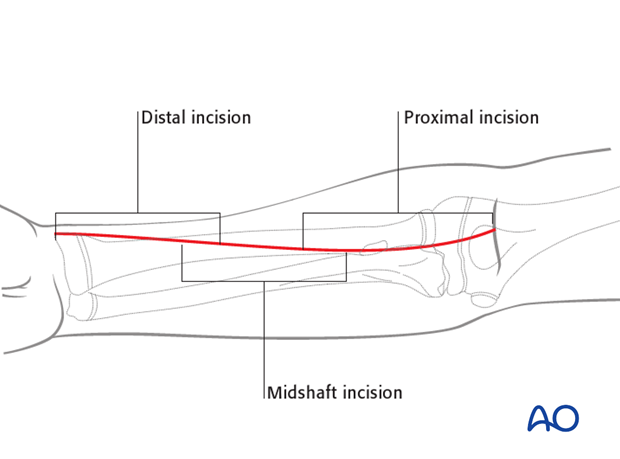
2. Superficial dissection
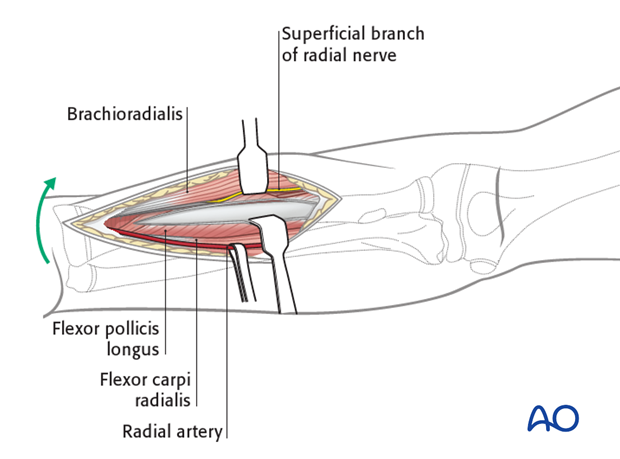
The superficial muscular dissection is similar for all three parts of the Henry approach, illustrated here for the proximal third.
Develop the interval between the brachioradialis (mobile wad) and flexor carpi radialis.
The radial artery lies deep to the brachioradialis in the middle part of the forearm and between the tendons of brachioradialis and flexor carpi radialis distally.
It can be identified by its two venae comitantes, which run alongside it.
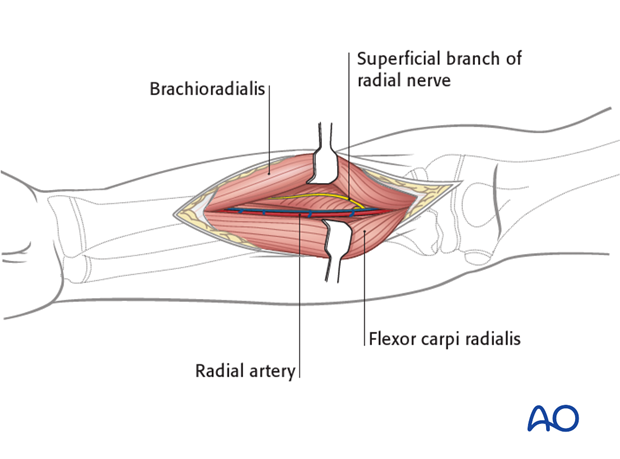
Proximally, identify the arterial branches arising from the lateral side of the radial artery by slipping a finger underneath them, lateral to the artery.
These are predominantly the recurrent branches and those to the mobile wad. Ligate them to retract the artery medially.
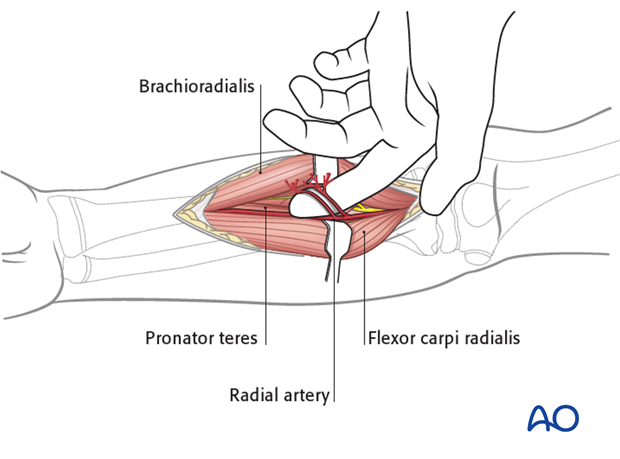
Laterally retract the superficial radial nerve, which runs under the brachioradialis on the lateral aspect of the radial artery.
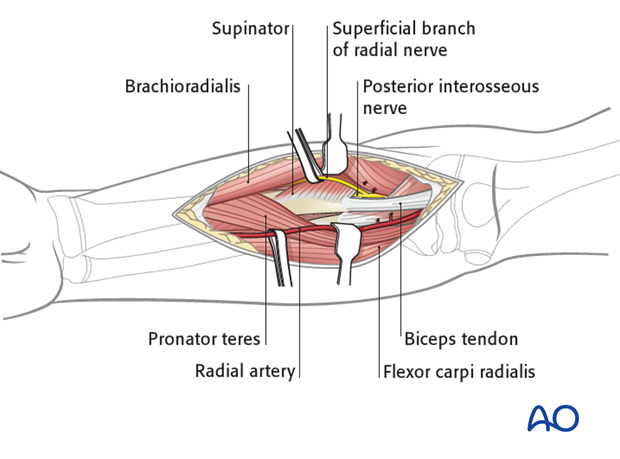
3. Deep dissection - proximal third
The supinator muscle covers the lateral aspect of the proximal radius.
The posterior interosseous nerve (also known as deep branch of the radial nerve) lies within the substance of the supinator muscle.
Supinate the forearm fully to displace the posterior interosseous nerve away from the surgical field.
Incise the supinator muscle along its most medial edge, and gently elevate it from the bone surface only to the extent that is necessary for the required exposure.
The lateral edge of the biceps tendon and its bursa are a useful anatomical guide to finding the medial edge of the supinator at the most proximal end of the dissection.
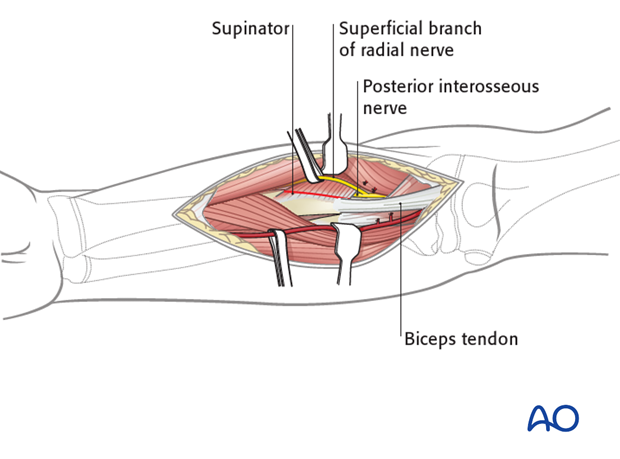
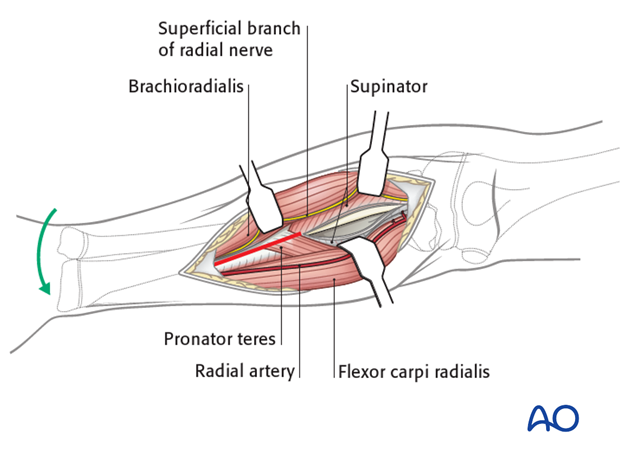
4. Deep dissection - middle third
Pronate the forearm fully to expose the lateral border of the pronator teres and its insertion.
Note: Sometimes it will be necessary to partially detach the pronator teres from the radius. Whenever possible, preserve at least some of its insertion.
5. Deep dissection - distal third
Pronate the forearm to expose the aspect of the radius lateral to the edge of the flexor carpi radialis and the radial artery. Deep to this lie flexor pollicis longus and the pronator quadratus, which become visible if the forearm is supinated.
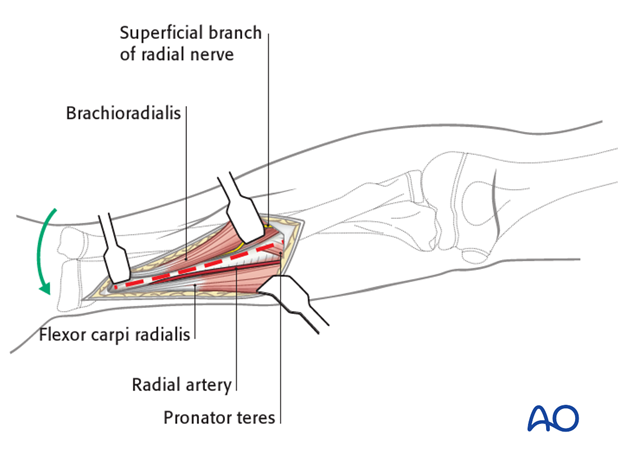
Supinate the forearm and complete the exposure of the bone by any necessary elevation of the flexor pollicis longus and, more distally, pronator quadratus.
6. Wound closure
Generally, the muscles do not need reattachment as they fall back to the anatomical position. The fascia should not be closed after forearm approaches because of the risk of compartment syndrome.
Close skin and subcutaneous tissue with fine resorbable sutures (this avoids distress to the child when removing nonabsorbable sutures).













