Complications and technical failures
1. General considerations
Complications associated with distal tibial fractures include:
- Delayed wound healing
- Infection
- Loss of reduction
- Malunion
- Growth disturbance
- Cast complications
2. Wound healing
Significant swelling, particularly when associated with blistering, may necessitate a delay in surgical treatment.
The limb is stabilized with a splint or split paster until the condition of the skin and soft-tissue envelope has improved.
In some cases, a temporary external fixator is necessary to provide sufficient stability.
Definitive surgery should be delayed until the skin and soft tissues recover.
3. Growth disturbance
The distal tibial physis contributes significantly less to longitudinal growth than the distal femur and proximal tibia. Physeal injuries in younger patients, however, may cause significant shortening and angular deformity.
Functional consequences related to premature physeal closure are unusual following transitional injuries, including Tillaux and triplane fractures. This, however, can occur particularly in younger adolescents with clinically important growth remaining. It is, therefore, necessary to keep these patients under surveillance until radiological evidence of growth plate closure.
Clinical and radiographical surveillance is essential after distal tibial physeal injuries.
If growth disturbance is suspected, MRI/CT scan is recommended.
Depending on the age of the patient, premature growth arrest can be treated with:
- Bar excision
- Osteotomy
- Leg lengthening/equalization procedures
Surveillance should continue until there is radiological evidence of normal growth.
Recommended reading:
- Nguyen JC, Markhardt BK, Merrow AC, et al. Imaging of Pediatric Growth Plate Disturbances. Radiographics. 2017 Oct;37(6):1791–1812.
4. Loss of reduction
Loss of reduction may result from inadequate fixation of an unstable injury.
This can be prevented by:
- Assessing stability after reduction
- Confirming stability after fixation
- Applying a molded cast
- Using suitable implants, eg, K-wires of appropriate size
- Application of K-wires in a stable configuration
5. Infection
Infection in children is less common than in adults.
This may complicate surgical fixation or occur as a consequence of an open fracture.
The risk is increased with:
- Unhealthy or broken skin
- Limb swelling
- Tethered skin around K-wires
- Delayed removal of protruding K-wires
6. Malunion
Malunion is usually a consequence of inaccurate reduction and ineffective fixation.
Although the pediatric skeleton has the capacity to remodel, reduction should be as accurate as is practically possible.
Malalignment may be accepted, provided there is a high probability of successful remodeling, and this requires an appreciation of the remodeling capacity at the fracture location, the age of the patient, and the plane of angulation.
7. Cast complications
Managing fractures with a cast is common in pediatric practice.
This requires attention to detail to maximize the likelihood of successful treatment. Complications may occur during application, treatment, and removal.
Preventive measures during application:
- Padding pressure points (eg, malleoli, patella, fibular head, common peroneal nerve)
- Ensuring a short leg cast is below the fibular neck to avoid common peroneal nerve compression
- Avoiding tight application of cast bandage
- Delayed completion of a cast if swelling is anticipated
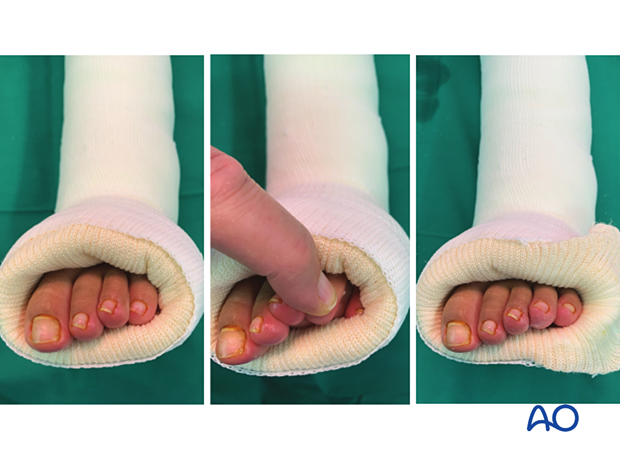
- Ensuring complete exposure of all toes to allow assessment of circulation
Preventive measures after cast application:
- Elevation of the leg
- Ensuring the cast and padding is kept dry
- Providing clear instructions to carers about monitoring toe perfusion and swelling
- Avoiding insertion of objects between cast and skin
Preventive measures during cast removal:
- Avoid thermal and direct skin injury
In the left and middle image, the fifth toe is hidden. Revision of the cast exposes all toes.
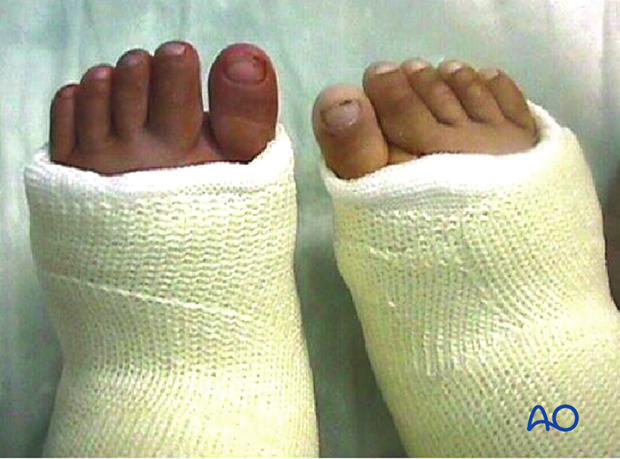
This case illustrates a cast on the left foot that has been applied too tightly.
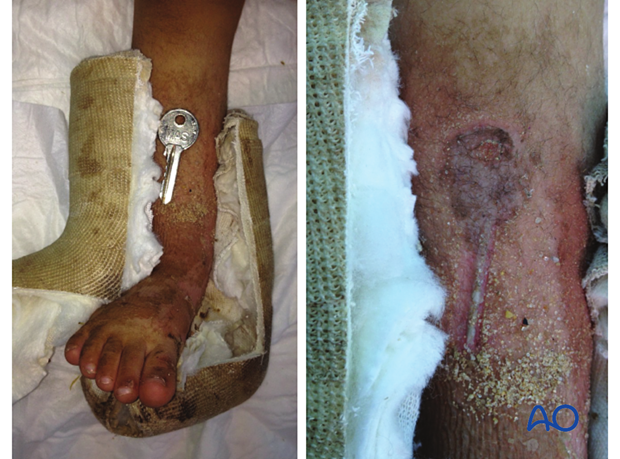
This case shows a pressure sore caused by a key inserted between the cast and the skin.
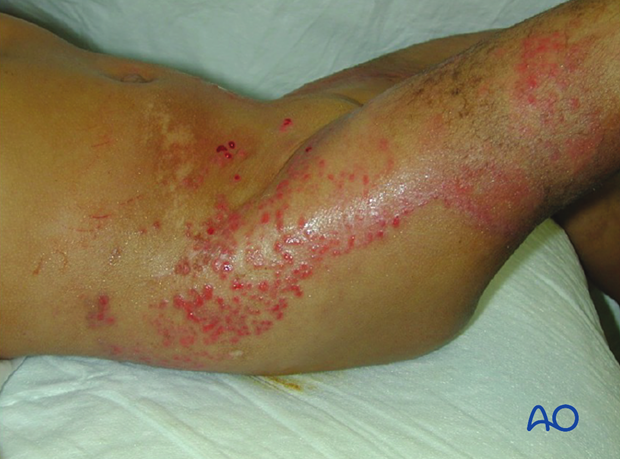
This case shows dermatitis after casting.
8. Posttraumatic arthritis
Intraarticular ankle fractures are associated with posttraumatic arthritis if anatomical reduction is not achieved and maintained.













