Lateral approach to the pediatric distal humerus
1. Main indication for lateral approach in trauma
The main indication for a lateral approach in the distal humerus are:
- Displaced lateral condylar fractures (13-E/3.1 and 13-E/4.1)
- Displaced capitellar fractures (13-E/8.1)
- Displaced, unstable avulsion of the lateral collateral ligament (13-E/7L)
- Irreducible supracondylar fractures (13-M/3).
2. Skin incision
The incision starts over the lateral supracondylar ridge, 3-5 cm (depending on the age/size of the child) proximal to the elbow joint. It passes distally to the lateral surface of the proximal forearm, posterior to the radial head.
In pediatrics the incision is slightly more posterior compared with the adult approach.
It is always possible to go more anterior from a posterior incision by extending the incision distally and or proximally and undermining.
Note: Care must be taken to protect the radial nerve, which runs close to the radial head and neck. It divides into its superficial and deep branches at the level of the radial head.
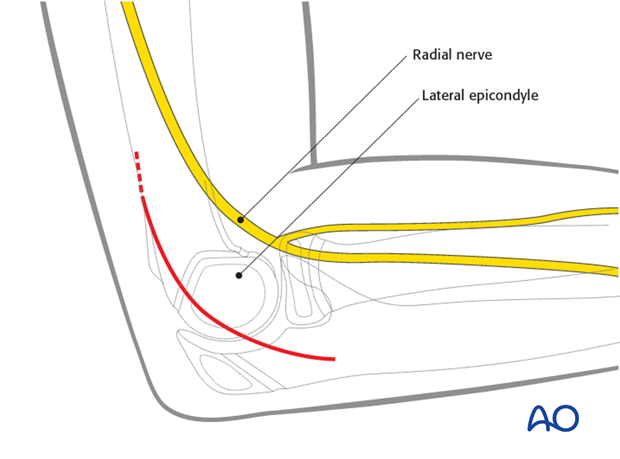
3. Deep dissection
The deep fascia is incised proximally, directly over the lateral supracondylar ridge of the humerus.
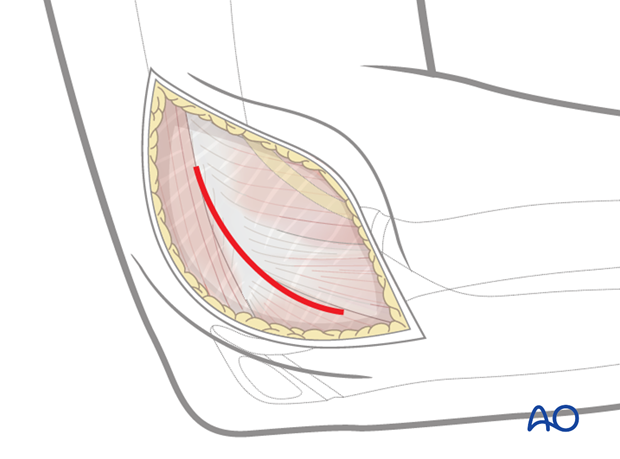
The approach is developed between the brachioradialis and the triceps muscles, down to the capitellum and then along the posterior border of the extensor muscles, in front of the anconeus muscle. The red line marks the site of the capsulotomy.
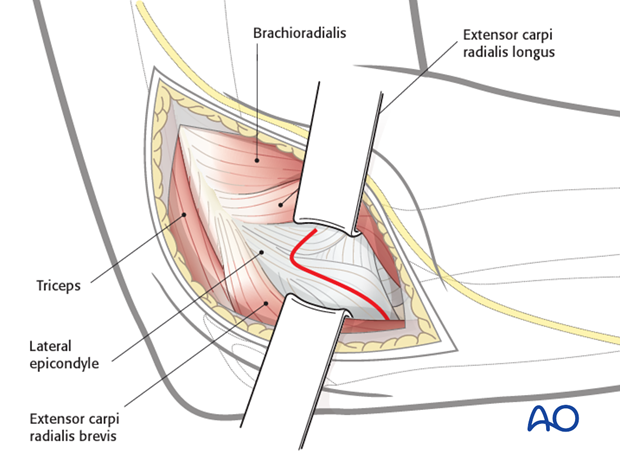
4. Opening the joint
The joint capsule is incised anteriorly over the capitellum, passing over the lateral epicondyle and distally as far as the radial head.
If wider exposure of the joint is needed, the capsule can be released from its anterior attachment to the humerus.

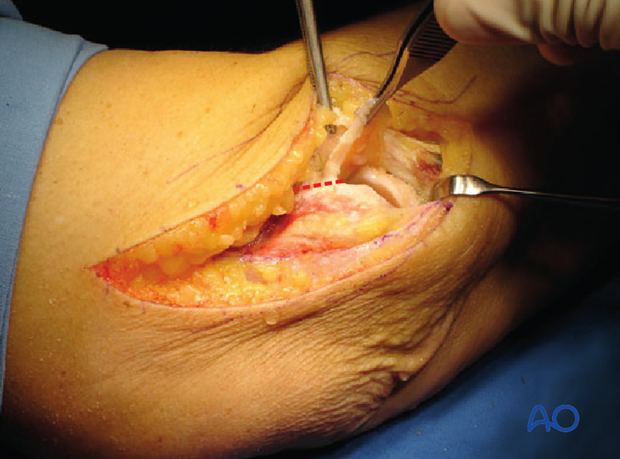
The exposure of the capitellum and the radial head is seen in this photograph.
The dotted line shows the extension for joint exposure. This extension is sometimes needed for better visualization and reduction of the joint surface for lateral condylar fractures.
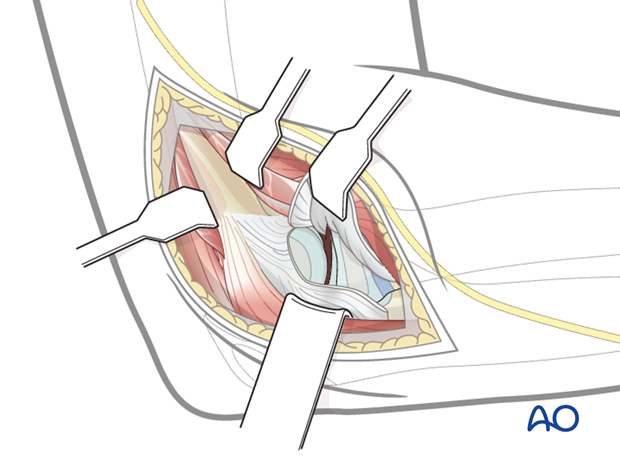
5. Further exposure
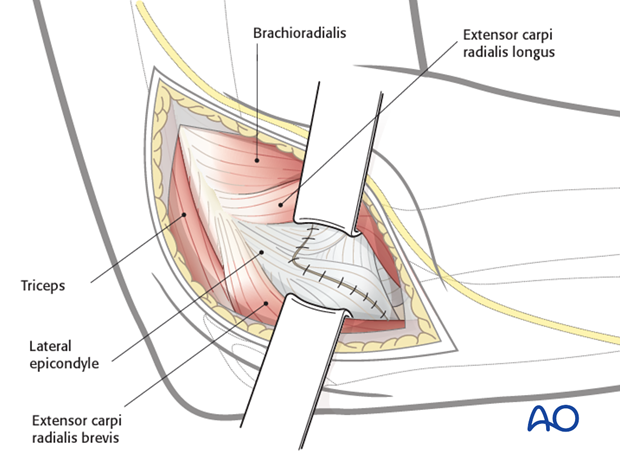
Subperiosteal partial release of the brachioradialis and extensor carpi radialis longus anteriorly, and the triceps posteriorly and their retraction will improve joint exposure.
Note: Care must be taken when placing the anterior retractor as the radial nerve is at risk.
Do not use lever retractors.
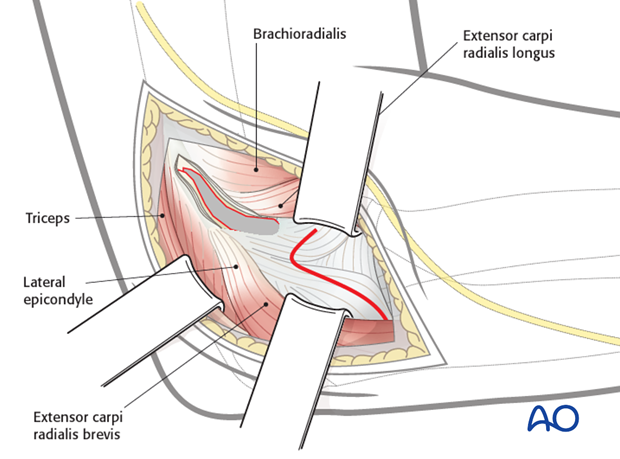
6. Approach for screw fixation of lateral condylar fracture
The following approach is used for screw fixation of lateral condylar fractures:
- Skin incision somewhat more posterior than normal
- Visualization of the joint as described above in the standard lateral approach
Subfascial exposure of the posterolateral aspect of the capitellum and metaphyseal fragment must respect the muscle attachments and vascularity, which enters the fragment from behind.
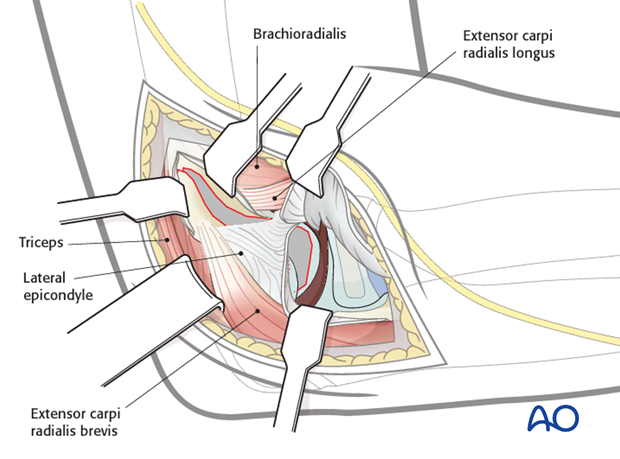
The displaced lateral condylar fragment is now ready for reduction.
7. Closure
The capsule is closed with continuous resorbable sutures (3/0).
The muscles and fascia are reattached with continuous resorbable sutures (2/0 or 3/0).
Skin and subcutaneous tissue are closed with fine resorbable sutures (this avoids any distress to the child in removing nonabsorbable sutures).