Anterior approach to the pediatric distal humerus
1. Main indication for anterior approach in trauma
The main indications for an anterior approach to the distal humerus are:
- Vessel exploration
- Nerve exploration
2. Vessel exploration
Vessel/artery exploration is only indicated if a white, cold pulseless hand persists after fracture reduction and fixation.
If the patient's hand initially was pulseless and perfused, but after reduction and K-wire fixation the hand becomes pulseless and white, remove the wires and check the hand again before exploring the artery.
3. Nerve exploration
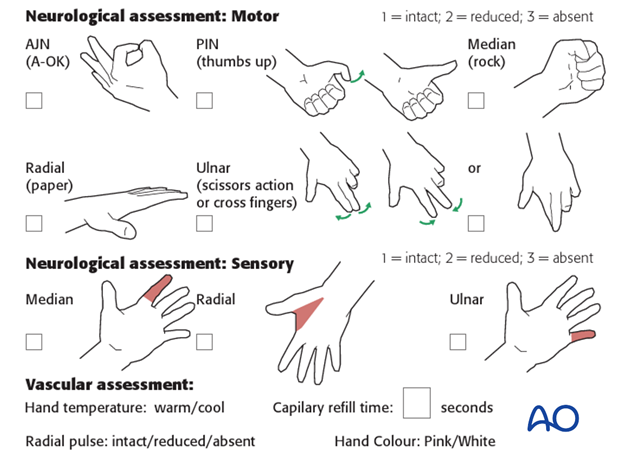
Prior to any intervention a detailed neurological examination of the limb should be undertaken and documented in a structured manner.
Partial primary impairment of function of one or more of the three main nerves (ulnar, radial, and median nerve) occurs in at least 15-20% of displaced supracondylar fractures, but is not an indication for nerve exploration.
If the nerve has normal function prior to fracture reduction and fixation, but it is impaired after reduction, consider the possibility of nerve entrapment in the fracture (median nerve) or irritation of the ulnar nerve by a K-wire. Remove any K-wire suspected of compromising a nerve. Consider whether the nerve may be entrapped between fracture fragments. Routine exploration of the nerve is not always necessary. The management of these scenarios remains controversial, nerve exploration may be indicated if the anatomical situation is unclear.
Nerve exploration is indicated in open fractures with initial total loss of function of the radial or median nerve.
4. Skin incision – closed fractures
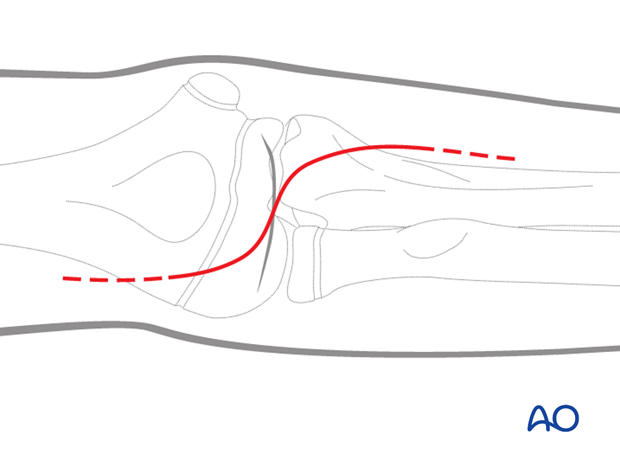
In a closed fracture, a lazy Z-shaped incision (as shown in the illustration) is recommended. The initial incision should not be made too long, as it can be extended as necessary.

5. Skin incision – open fractures
In open fractures, the existing wound should be utilized. Often, however, the initial wound has to be extended proximally and/or distally from one or other end of the wound in order to create a Z-shaped skin opening.
6. Deep exploration
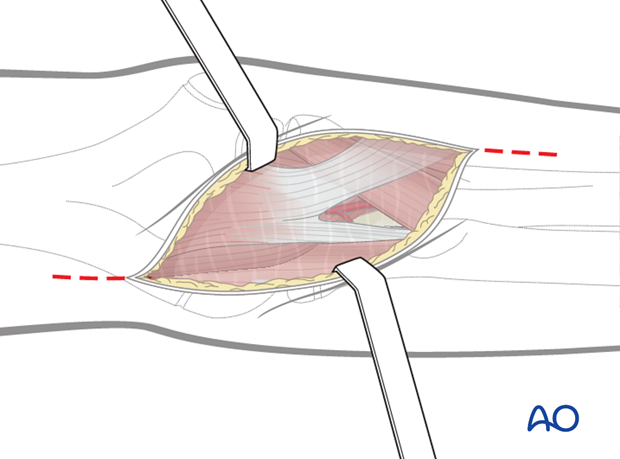
Vascular and/or nerve damage occur only in severely displaced fractures. In these cases, the sharp proximal fracture end of the distal humerus pierces most of the deep structures, such as brachialis muscles, fascia and the integument. As a result, the exposure of the vessels is already accomplished in the majority of cases. Normally, the original wound only needs to be extended for better visualization of the vessel and/or nerve.
Stabilize the fracture before nerve repair. This can be done in one of the following two ways:
- Closed reduction and pinning of the fracture in the traditional way, followed by exploration of the nerve
- Exploration of the nerve, exposure of the fracture zone by lifting up the biceps muscle, reduction under visual control and percutaneous pinning
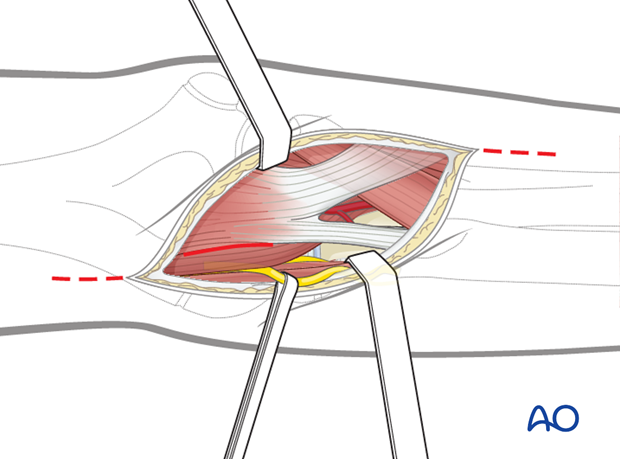
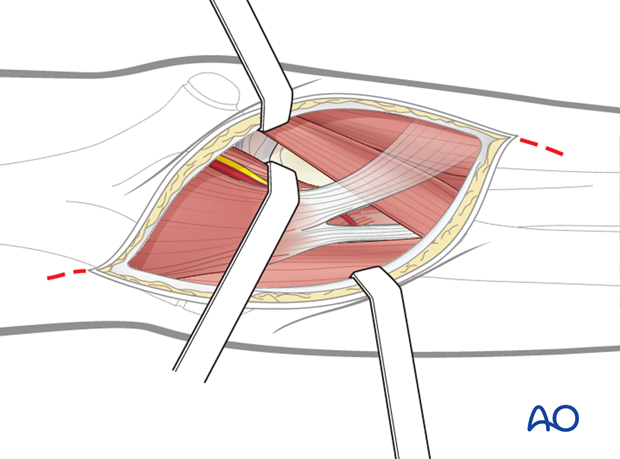
For the radial nerve, which is mostly ruptured at the level of the fracture, the exposure is along the radial border of the biceps muscle.
Because of the attachment of the brachialis muscle to the humerus at the level of the fracture, this muscle is often ruptured. The radial nerve passes along the medial side of the brachioradialis muscle. If needed, the incision and exposure can be extended distally as far as the level where the superficial and deep radial branches separate.
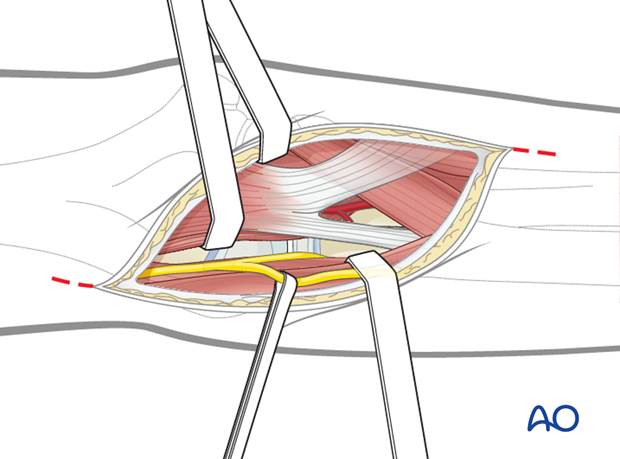
For brachial artery repair, or approach to the median nerve, the dissection must be done on the medial side of the biceps muscle. In contrast to adults, in children the biceps tendon must not be divided.
Prior to vascular repair the fracture has to be stabilized:
- Explore the artery, expose the fracture zone by retracting the biceps muscle, reduce the fracture under visual control and insert percutaneous K-wires
7. Closure
Skin and subcutaneous tissue are closed with fine resorbable sutures (this avoids any distress to the child in removing nonabsorbable sutures).













