Radiological evaluation
1. Introduction
Radiological assessment of the injured distal femur and knee requires good quality x-rays in two planes.
Further imaging with computerized tomography (CT) and magnetic resonance imaging (MRI) is often necessary.
Recommended reading:
- Nguyen JC, Markhardt BK, Merrow AC, et al. Imaging of Pediatric Growth Plate Disturbances. Radiographics. 2017 Oct;37(6):1791–1812.
2. Plain x-rays
Plain x-rays in two planes (anteroposterior (AP) and lateral) are required to:
- Identify the location and extent of injury
- Image the whole bone
- Classify the injury pattern
- Assess the degree of displacement
- Assess stability
- Identify additional injuries
- Identify preexisting contributory pathology (eg, cysts or tumors)
- Evaluate the growth plate
Further imaging with computerized tomography (CT) and magnetic resonance imaging (MRI) is often necessary.
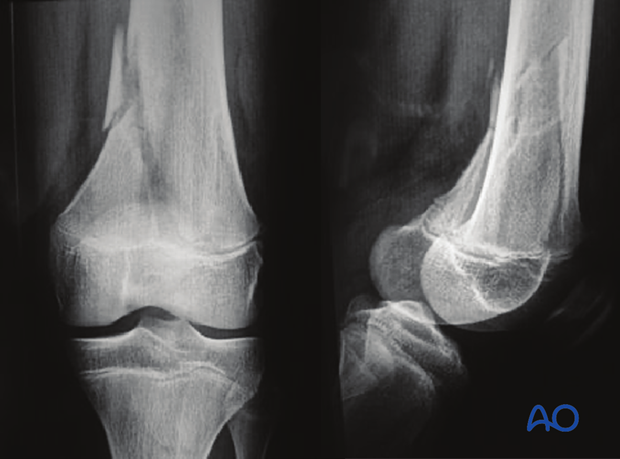
Metaphyseal corner fractures
If fractures are seen in children below walking age deliberate injury should be suspected.
In this example, metaphyseal corner fractures of the left distal femur are seen in an infant who had multiple other injuries consistent with abuse.
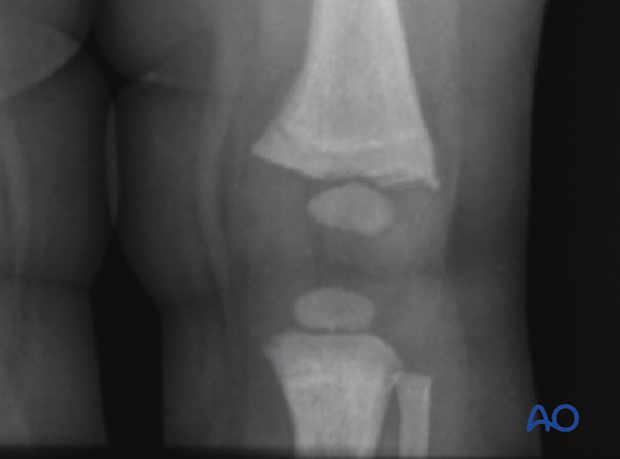
Salter-Harris II fracture
This involves a metaphyseal wedge remaining attached to the epiphyseal fragment (Thurstan Holland fragment).
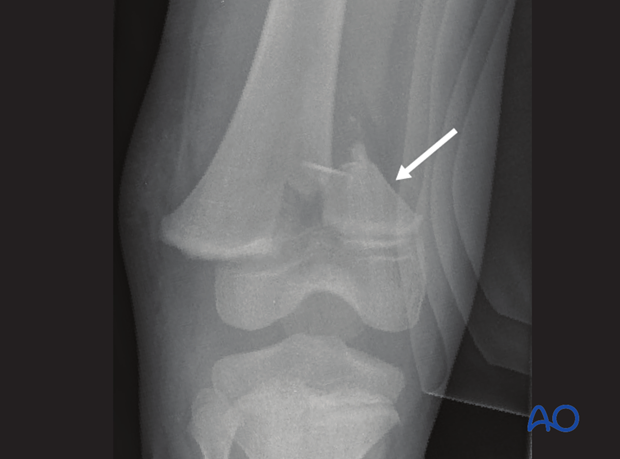
Occult or undisplaced growth plate injuries
Sports trauma can produce occult or undisplaced growth plate injuries.
Initial x-rays may show only subtle widening of the growth plate and are easily missed.
X-rays after one week may show periosteal healing or a well-defined metaphyseal (Thurstan Holland) fragment.
X-ray of a minimally displaced Salter-Harris II fracture
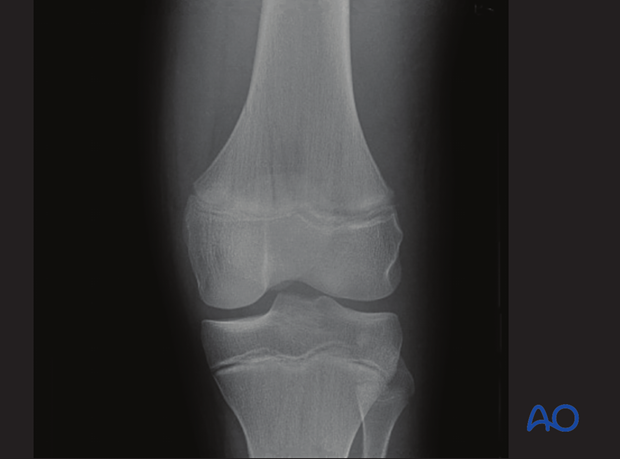
3. Intraoperative imaging
Intraoperative image intensification with stress views can be used to assess stability.
This may also demonstrate whether an intraarticular fracture is simple or multifragmentary.
4. CT imaging
The dose of ionizing radiation from a CT scan of the knee is significantly higher than from a standard x-ray.
It is therefore necessary to consider whether this is likely to provide information that cannot be obtained from plain x-rays, or MRI.
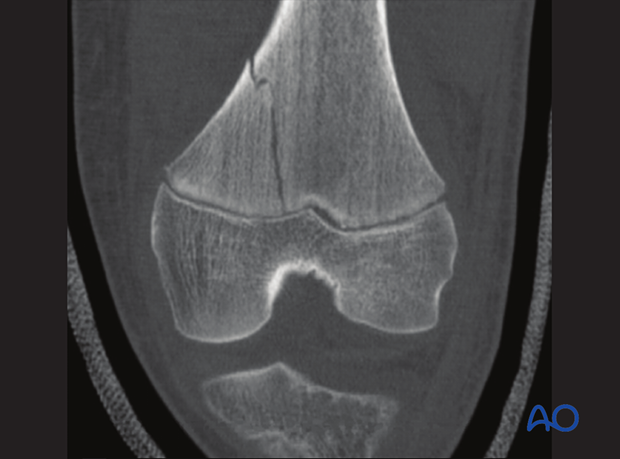
CT is the best modality for demonstrating the extent of displacement of all fracture lines. This is particularly important in intraarticular fractures.
2-D multi-planar-reformation (MPR) improves analysis of the fracture and allows accurate preoperative planning.
CT scan of a minimally displaced Salter-Harris II fracture
5. MRI
MRI is not usually part of the primary imaging in acute trauma.
Longer examination times makes it difficult for the child to stay still and the definition of the bony anatomy is inferior to information from CT scans.
MRI is more likely to be indicated, after the acute phase, to provide detailed analysis of the zone of injury, especially the soft-tissue component.
General anesthesia, specifically for MRI examination, should be avoided in an acute setting.
MRI axial and coronal views showing Salter-Harris III epiphyseal fracture
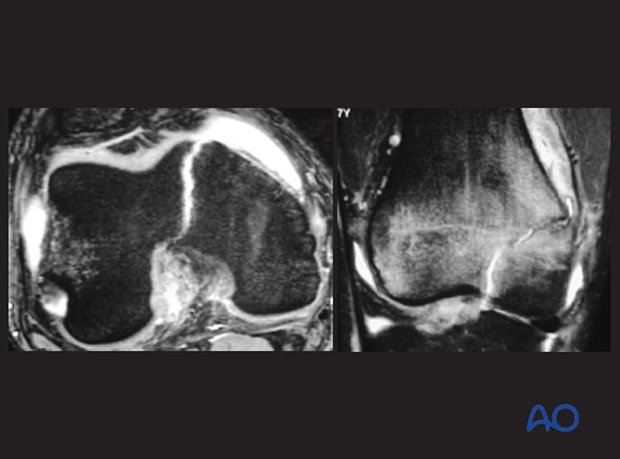
The following features can be demonstrated on an MRI:
- Bone edema, indicating bony injury without fracture, or cancellous microfracture
- Incomplete fracture lines
- Cartilage injury
- Ligament injury
- Soft-tissue injury
- Hematoma
- Vascular injury (with IV contrast)
- Pathological bone (eg, tumors and cysts)













