Proximal phalanx, base and shaft, skier’s thumb
Introduction: Avulsion / ligamentous rupture
Ulnar collateral ligament disruption is also called skier’s, or gamekeeper’s, thumb. If undiagnosed it leads to chronic instability and weakness of pinch.
Ulnar collateral ligament tears are the result of abduction forces acting on the thumb, putting the ligament under sudden excessive tension.
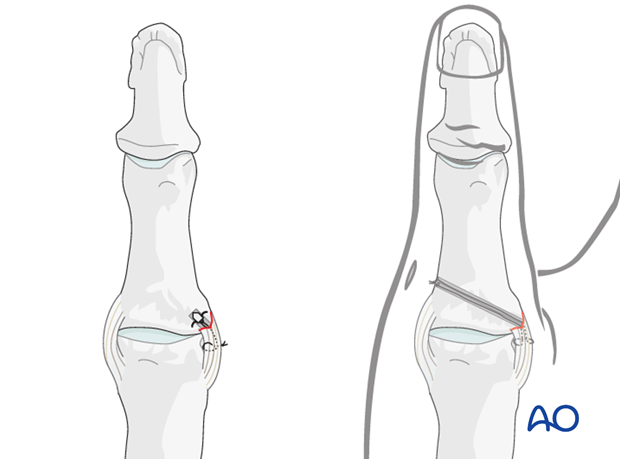
Avulsion fractures of the ulnar corner of the proximal phalangeal base of the thumb are treated in a fashion similar to the other proximal phalanges. In the thumb however, the avulsed fragment may displace dorsal to the adductor aponeurosis. Options for treatment are lag screw fixation, cerclage compression wiring, or anchor suture for comminuted fractures where the fragments will be excised.
Note: We now prefer the term “Cerclage compression wiring” to “Tension band wiring” because the tension band mechanism cannot be applied consistently to each component of the fracture fixation. An explanation of the limits of the Tension band mechanism/principle can be found here.
Diagnosis
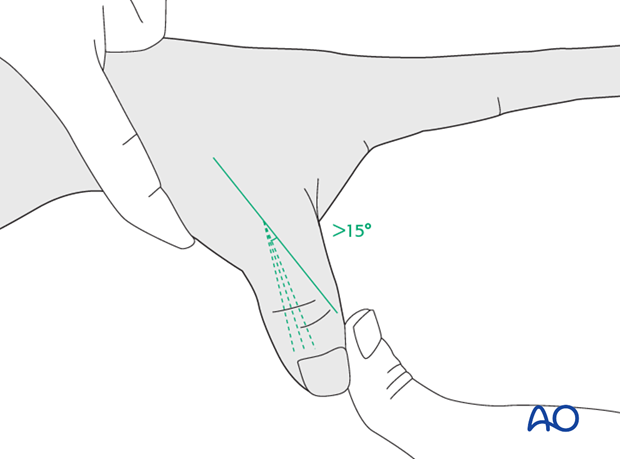
After injection of a local anesthetic into the metacarpo-phalangeal (MP) joint, stress testing is performed in 30 degrees of flexion. This is necessary in order to exclude any influence of the intact volar plate on stability when tested in full extension. Compare the test with the uninjured side. More than 15 degrees difference and a soft end point indicate a complete rupture of the ligament.
Choice of treatment
Nonoperative treatment
If the stress test under local anesthesia shows less than 15 degrees difference compared with the opposite side, and a firm end point, the injury can be treated nonoperatively with a period in a protective cast for about 4-6 weeks.
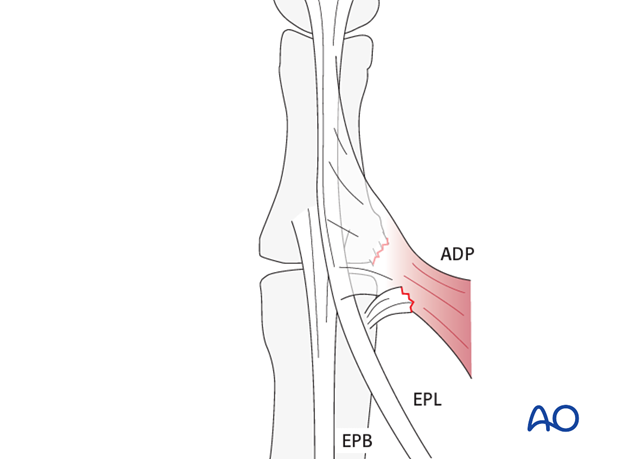
Anatomy: Stener’s lesion
The proximal edge of the adductor aponeurosis is responsible for Stener’s lesion. The ulnar collateral ligament stump is displaced dorsally to the aponeurosis, which prevents ligament healing.
Suture anchors or tunneling
Two alternative techniques are available for collateral ligament reattachment: suture anchors, or tunneling. The advantage of suture anchors is the relative ease of the procedure. Tunneling is the more demanding procedure, but it is significantly less expensive.