Nonoperative treatment
1. Introduction
Rolando’s fracture is a 3-part intraarticular fracture of the base of the thumb metacarpal. These T- or Y-shaped fracture patterns can occur either in the frontal, or in the sagittal plane
The causative mechanism is axial overload along the first metacarpal causing compression failure of the joint surface.
Today, the term “Rolando’s fracture” is often misused to describe multifragmentary intraarticular fractures of the thumb metacarpal base.
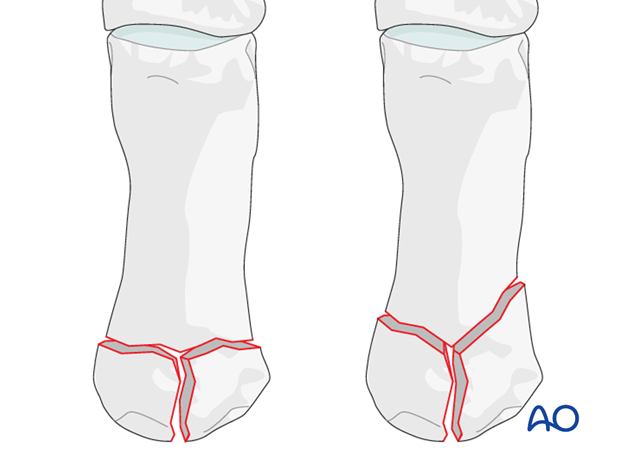
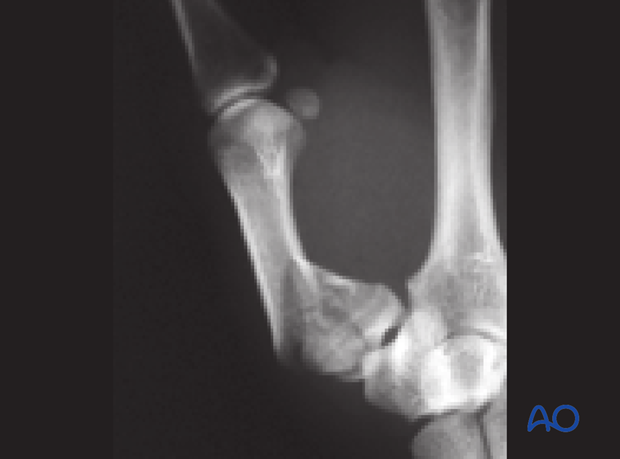
Metaphyseal and articular comminution are often more marked than apparent on the x-rays. The full extent of the comminution is often seen only after distraction of the fracture, as demonstrated in the images.
A CT scan, or traction x-rays, are advisable.
If the fracture can not be reduced anatomically, open reduction and internal fixation must be performed.
Teaching video
AO teaching video: Application of the thumb spica
2. Reduction
Apply traction
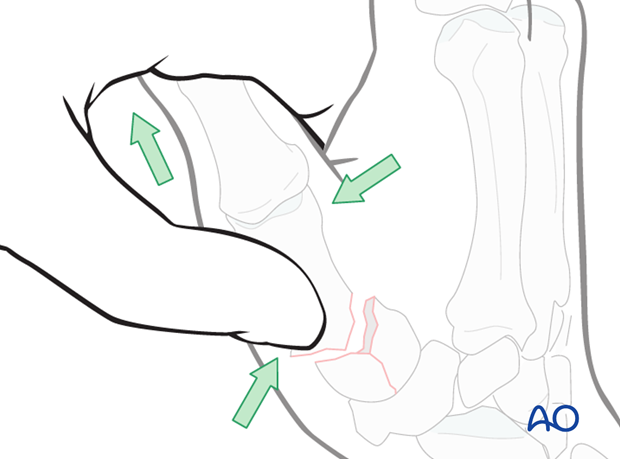
As there is usually a flexion deformity, reduction of the diaphyseal fragment to the articular fragments can be performed with axial traction on the thumb and simultaneous pressure over the dorsal aspect of the basal diaphysis near the fracture.
3. Applying cast
Maintaining reduction
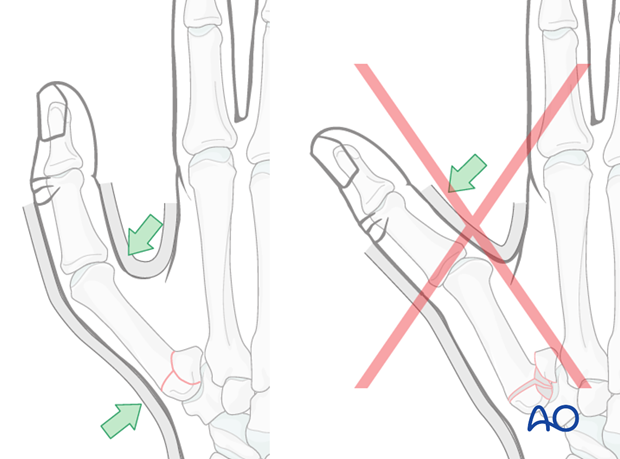
During the application of the cast, it is important to exert pressure over the dorsal aspect of the first metacarpal diaphyseal base, and from the palmar aspect over the first metacarpal head.
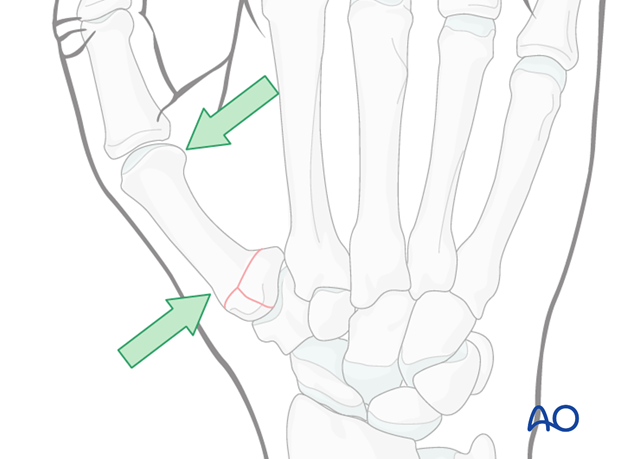
Pitfall: palmar pressure
Avoid pressing from the palmar aspect over the base of the proximal phalanx. This results in redisplacement of the fracture and hyperextension of the MCP joint.
Apply the cast
Immobilize the wrist in a well-padded below-elbow plaster with the wrist slightly extended, and the thumb immobilized in a position of slight abduction.
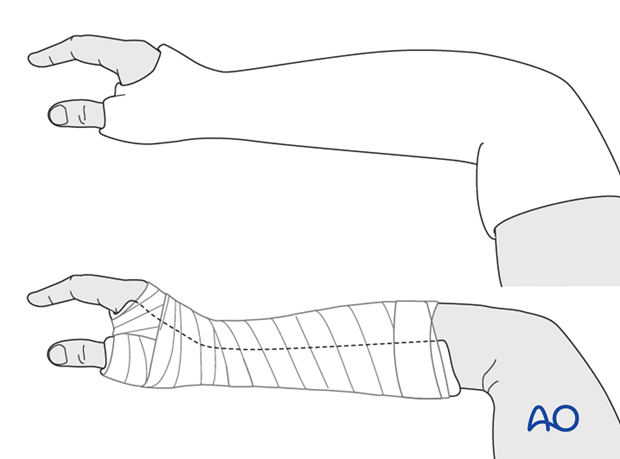
Make sure that the cast does not extend too far distally, either at the level of the finger metacarpophalangeal joints (MCP), or the interphalangeal joint of the thumb. The cast must not limit complete flexion of these joints.
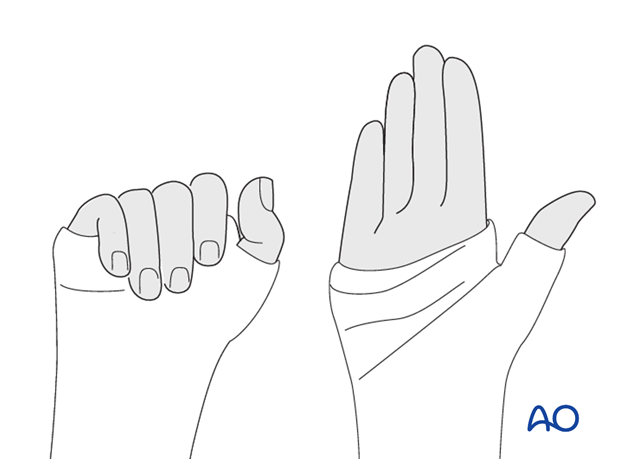
4. Aftertreatment
Confirm reduction by radiographs after the plaster has been applied. Repeat radiographs in weekly intervals until healing. Usually, immobilization for a 6 week period is sufficient.
The patient is instructed to regularly exercise the MCP joints and interphalangeal joints of the fingers, and the interphalangeal joint of the thumb.














