Nonoperative treatment
1. Principles
Anatomy
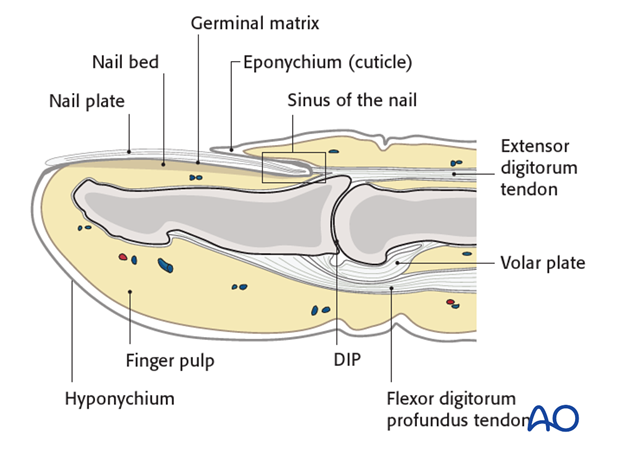
The distal phalanx is divided into three anatomical parts: most proximally, the metaphysis, followed by the diaphysis (“shaft”), and finally the ungual tuberosity (“tuft”).
The base of the distal phalanx has a prominent dorsal crest at the insertion of the extensor tendon. The tendon is also adherent to the distal interphalangeal (DIP) joint capsule.
On the palmar surface is the insertion of the flexor digitorum profundus tendon. This is also adherent to the volar plate.
The flexor tendon inserts into the whole width of the base of the distal phalanx.
The volar plate is very flexible, allowing hyperextension of the DIP joint and pulp-to-pulp pinch.
The vascularity of the extensor tendons is more precarious than that of the flexor tendons. This prolongs extensor tendon healing time.
Diagnosis
Discontinuities of the extensor insertion are often referred to as “mallet injury” or “baseball finger”. They can be purely tendinous, or bony avulsion fractures.
Diagnosis is based on
- The clinical history of the trauma
- Deformity, pain and swelling located in the dorsal aspect of the DIP joint
- Inability actively and fully to extend the DIP joint
- X-rays
AP and true lateral x-rays of the DIP joint are necessary for the diagnosis of fracture avulsions.
Low-energy radiographs, as used to visualize soft tissues, can be useful in identifying small flakes of bone.
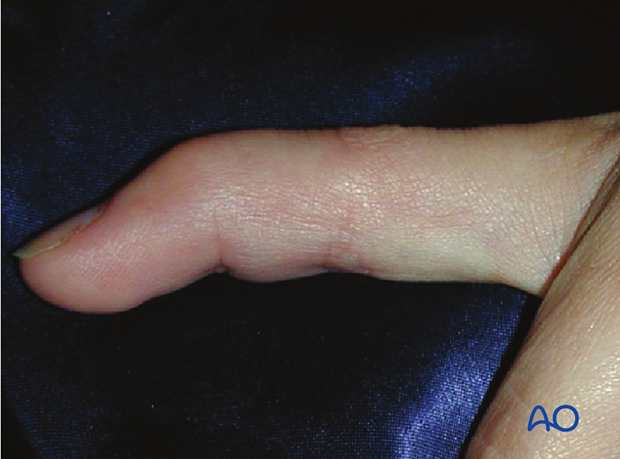
Flexion injury
The commonest cause of these injuries is forcible flexion of the actively extended DIP joint, as when stubbing a straight finger against resistance.
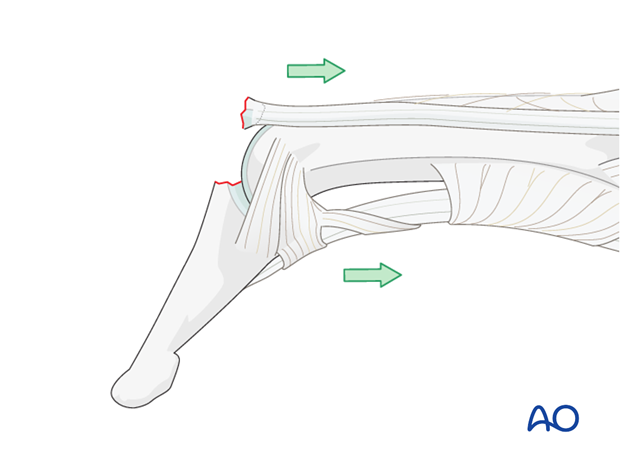
Axial compression injury
Occasionally, the injury is the result of an axial overload of the terminal segment of the finger, causing joint impaction and a dorsal marginal fracture, which is retracted by the pull of the extensor tendon.
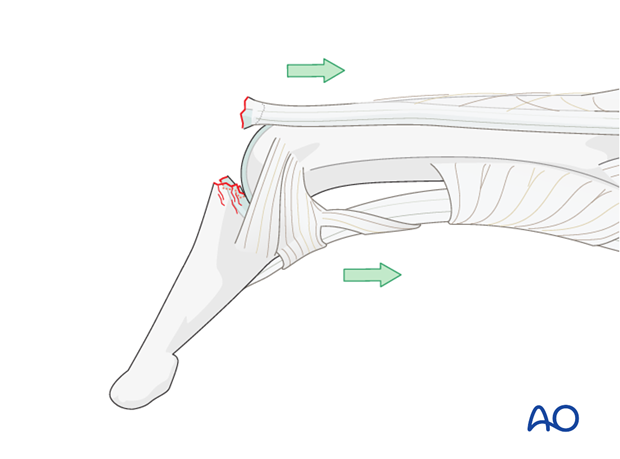
Spectrum of injury – partial disruption
These injuries may be complete disruptions or partial disruptions.
The nature of the disruption may be either a tear of the tendon insertion without fracture, or a bony avulsion of the tendon from the dorsum of the base of the distal phalanx, the bony fragment being of variable size.
In incomplete tendon injuries the resulting extension lag is no greater than 30 degrees. The patient retains a partial ability actively to extend the DIP joint.
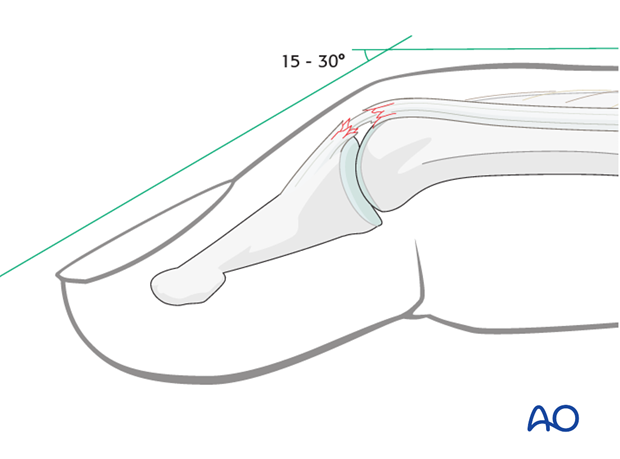
Spectrum of injury – complete disruption
In complete disruption of extensor mechanism, the patient is unable actively to extend the DIP joint.
The flexor digitorum profundus exerts a flexion deforming force onto the distal phalanx, partly counterbalanced by the intact oblique retinacular ligaments and the collateral ligaments.
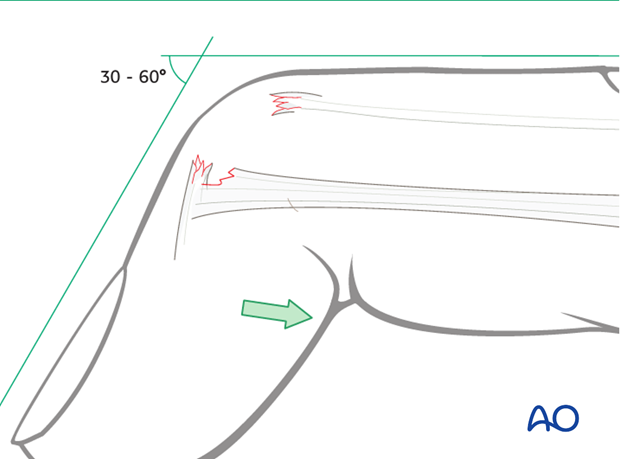
A similar clinical picture is presented by bony avulsion of the extensor mechanism at its insertion. The dorsally avulsed fragment is of variable size.
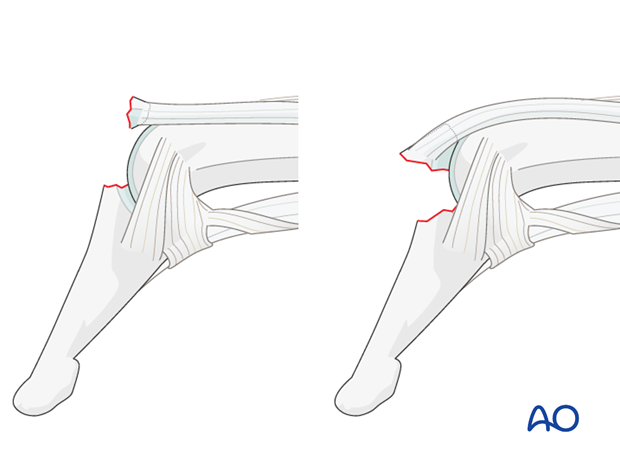
Swan-neck deformity
In some patients, elasticity of the ligaments and a lax PIP joint can result in swan-neck deformity, because after disruption of the extensor mechanism at the DIP joint, all extensor forces are concentrated on the PIP joint.
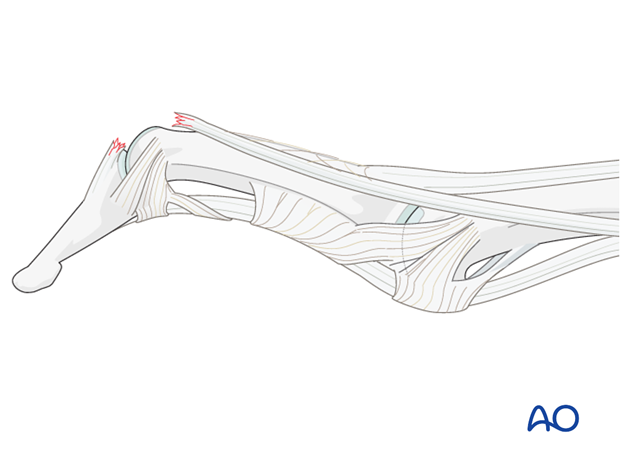
Fracture subluxation of DIP joint
An obliquely orientated axial compression force sometimes results in a dorsal marginal fracture, involving approximately half the articular surface, and can disrupt the collateral ligaments.
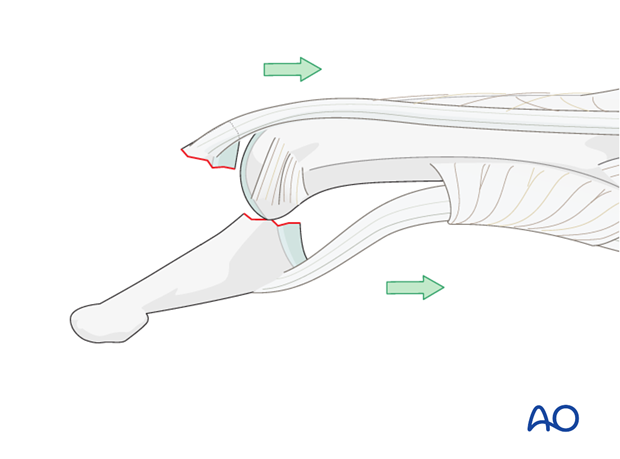
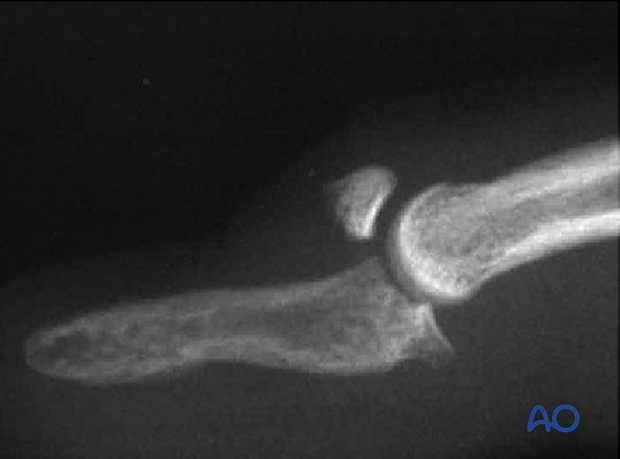
In such instances the pull of the flexor digitorum profundus results in palmar subluxation of the distal phalanx.
This injury represents a strong indication for ORIF.
2. Splinting
Anatomy
Nonoperative treatment can produce excellent results with near-normal range of motion. This is true even in the presence of persisting fragment displacement due to bone remodelling.
Nonoperative treatment is based on immobilization of the DIP joint in extension, leaving the PIP joint free.
Duration of immobilization
In the case of a disruption of the tendon, the DIP joint should be immobilized in extension for 8 weeks. It must be impressed on the patient that the DIP joint must be kept in extension at all times, even when the splint is taken off for cleaning.
It must be kept in mind that the vascularity of this area is precarious, even in healthy patients, and healing is slow. Any shorter period of immobilization risks re-rupture. Joint stiffness is unusual after these injuries.
In the case of bony avulsion injuries, an x-ray should be performed with the splint applied to confirm that no displacement has occurred. The splint must be worn at least 5 weeks when an x-ray is taken to check for bone healing.
Result
Frequently, patients may complain of a dorsal prominence, and of loss of the last 10-20 degrees of extension of the DIP joint. Dorsal tenderness rarely persists for more than a month or so after removal of the splint.
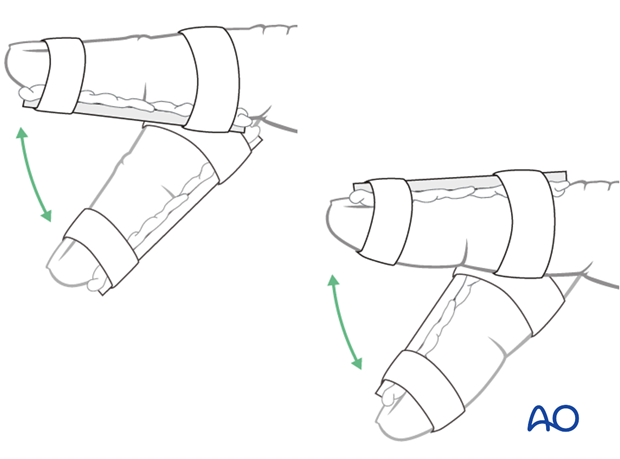
Dorsal splint vs palmar splint
Using a dorsal splint has the advantage of leaving the patient with the ability to pinch while the digit is immobilized.
However, proponents of palmar splintage argue that the palmar aspect is better cushioned than the dorsal and thereby can tolerate the splint better.
3. Contoured custom thermoplastic splint
The advantage of a custom thermoplastic splint is ...
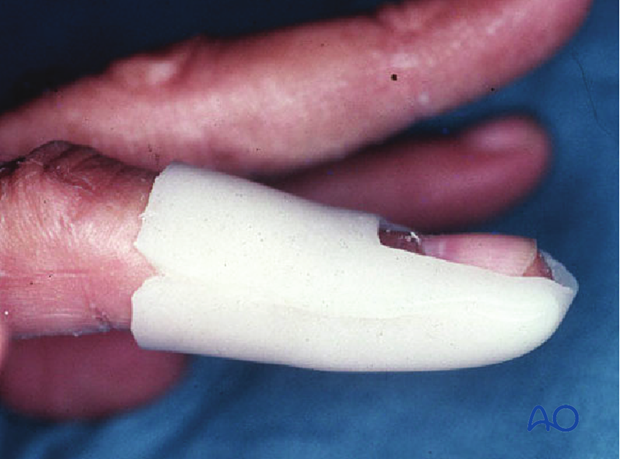
... that it is better adapted to the shape of the finger, and easier to change.
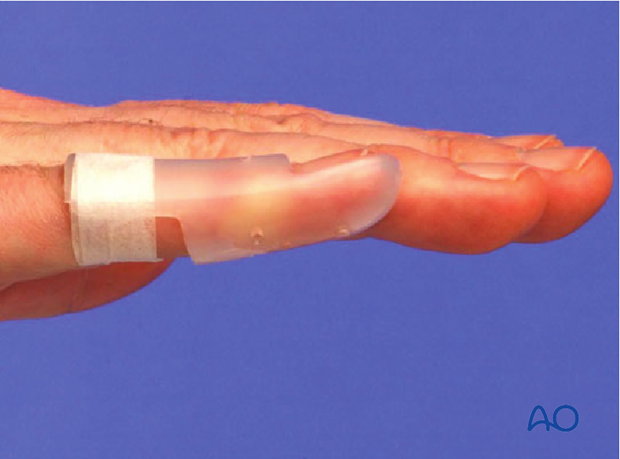
4. Cleaning
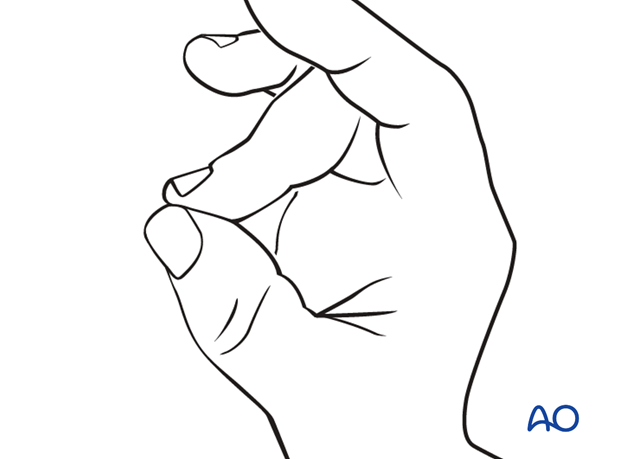
Instruct the patient to keep the finger in extension by pinching it with the thumb when the splint is taken off for cleaning, or by pressing the tip of the finger onto a table top.
Any flexing of the finger may disrupt the healing process. Removal of the splint and skin care must be performed by the patient in 1-2 day intervals.
5. Pitfalls
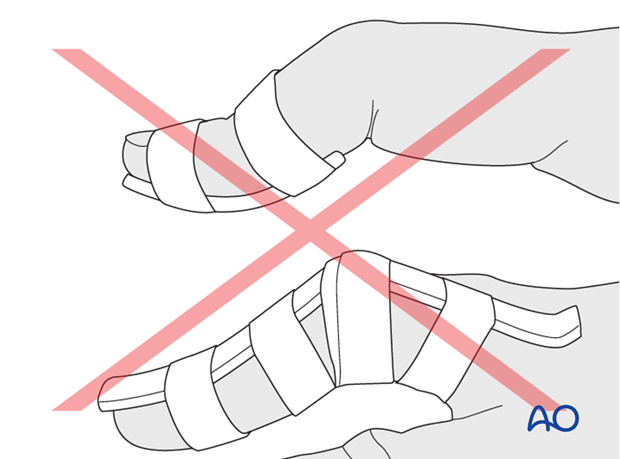
Hyperextension of the DIP joint
Do not attempt to immobilize the joint in hyperextension. This can compromise the precarious vascularization of the skin of the dorsal aspect of the joint and might provoke ischaemia and possible necrosis.
Immobilization of the PIP joint
Do not immobilize the PIP joint as this may result in flexion contraction of the joint.
6. Aftertreatment
Cleaning
Removal of the splint and skin care must be performed by the patient in 1-2 day intervals.
Functional exercises of the nonimmobilized joints can be started immediately.
Duration of immobilization
X-ray controls have to be performed immediately after the splint has been applied.
Follow-up x-rays with the splint should be taken after 1 week, and possibly after 2 weeks. Immobilization is continued until about 4 weeks after the injury. At that time an x-ray without the splint is taken to confirm healing. Splinting can then usually be discontinued and active mobilization is initiated.
If after 8 weeks radiographs confirm healing, full loading can be permitted.
Tuft fractures
In tuft fractures, splinting is mainly performed for pain treatment, and usually after 3 weeks, the splint can be discontinued. These injuries do not necessarily need x-ray control.