Lag screw with neutralization plate
1. Principles
Lag screw principles
In an oblique fracture, compression across the fracture is achieved with a lag screw.
The thread pulls the opposite bone fragment towards the head of the screw, creating compression across the fracture. The screw slides through the overdrilled near cortex.
Insert the lag screw as perpendicularly to the fracture plane as possible.
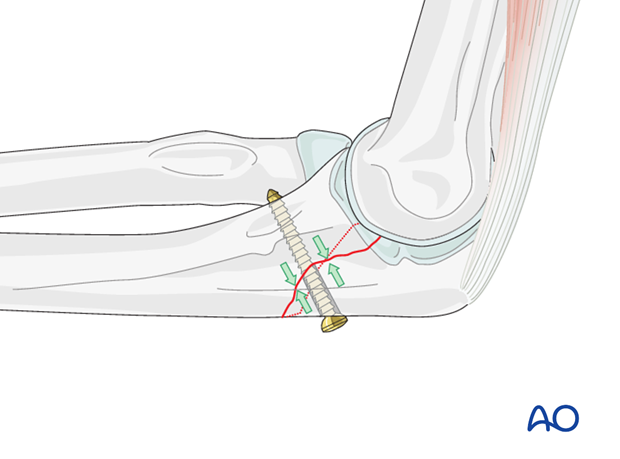
Neutralization plate
As a lag screw osteosynthesis alone is not able to resist shearing and torsion forces, a neutralization plate has to be added to allow early mobilization.
Note: Whenever possible (considering soft-tissue condition, fracture configuration, associated radial head fracture etc.), insert the lag screw through the plate to achieve better stability.
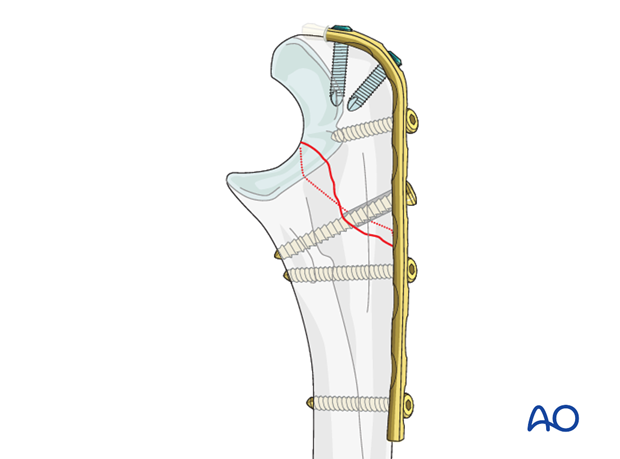
Plate selection
Plate length should be sufficient to place, usually, three screws in each fragment.
The plate may be a small fragment dynamic compression plate (3.5 DCP), or limited contact dynamic compression plate (LC-DCP), or locking plate (LCP) with conventional screws. More recently, use of 2.7 LCP has been reported.
Note: In osteoporotic bone, a LCP with locking head screws should be used, after insertion of a conventional lag screw through the plate.
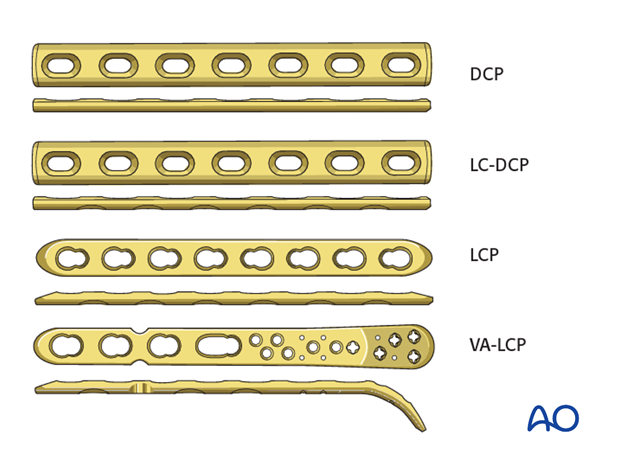
2. Positioning and approach
Positioning
This procedure is normally performed with the patient either in a lateral position or in a supine position for posterior access.
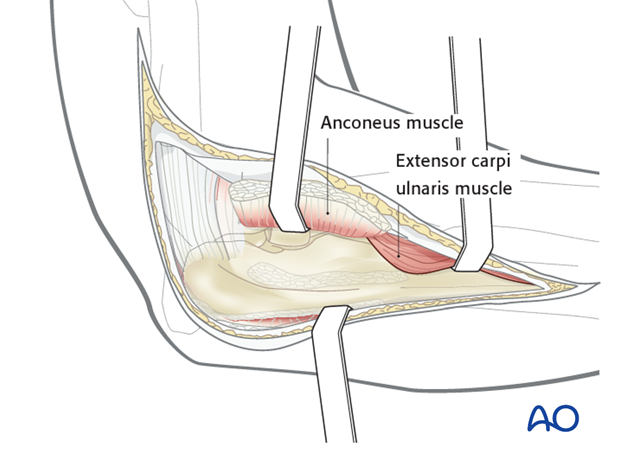
Approach
For this procedure a posterolateral approach is normally used.
3. Reduction
Cleaning the fracture site
Expose the fracture ends with minimal soft tissue dissection off the bone.
Remove hematoma and irrigate.
Check elbow stability.
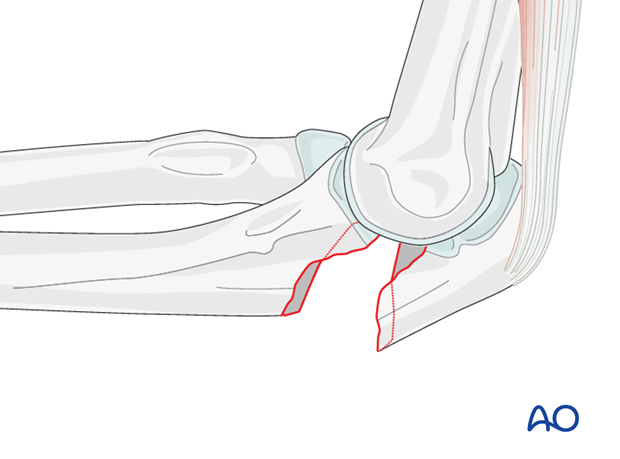
Direct reduction
Reduce the fracture with the help of small pointed reduction forceps and provisionally fix with forceps or K-wires.
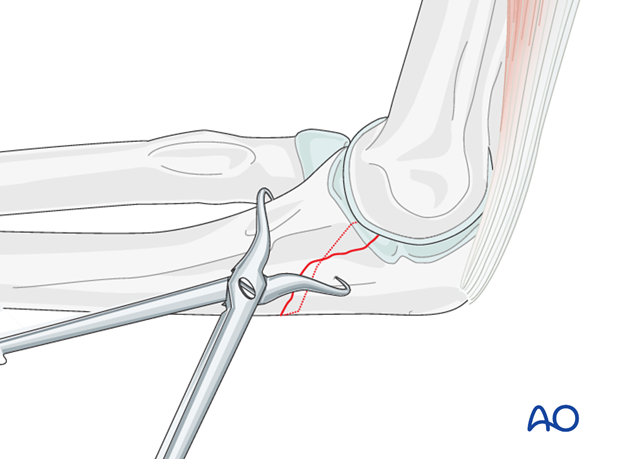
4. Lag screw insertion
Plate contouring
Contour the plate according to the posterior surface anatomy of the proximal ulna.
Contouring of the plate is achieved with bending irons or bending press.
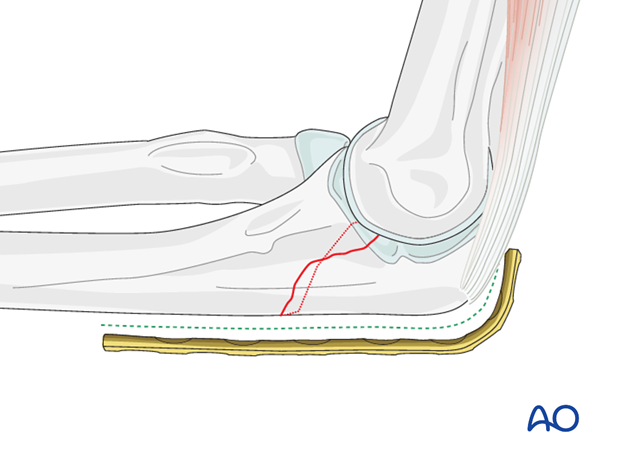
Plate application
Make a small transverse cut in the triceps tendon to slide the plate under.
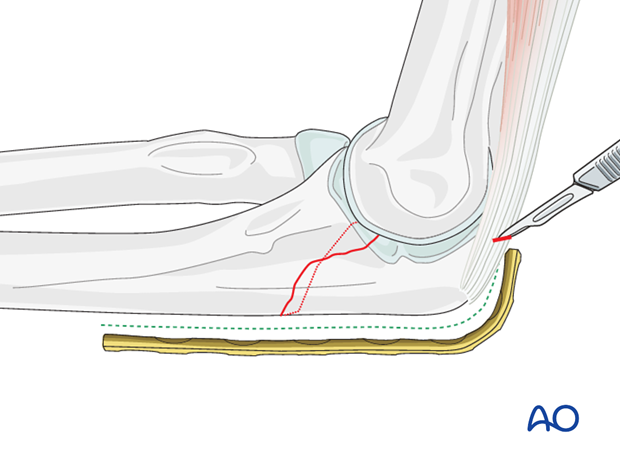
Apply plate and hold it against the bone with a bone clamp or one or two fingers.
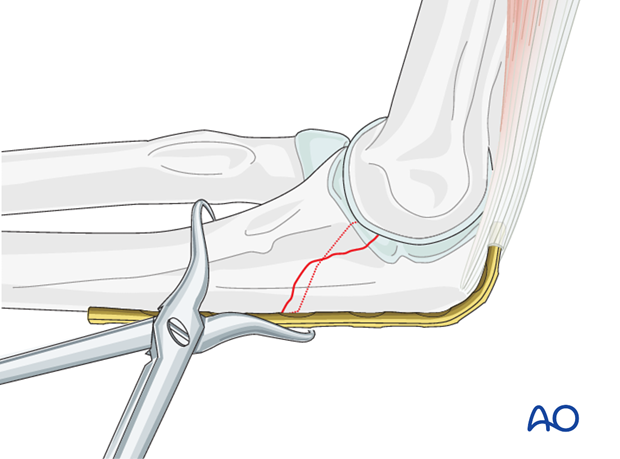
Drilling
Through the hole just proximal to the fracture drill a 3.5 mm gliding hole for the lag screw into the posterior cortical bone of the proximal fragment. The drill should be angled slightly ulnar to avoid impingement in the radio-ulnar joint.
Insert the 2.5 mm drill sleeve into the gliding hole until it reaches the far cortical bone.
Now drill the far cortex with the 2.5 mm drill bit.
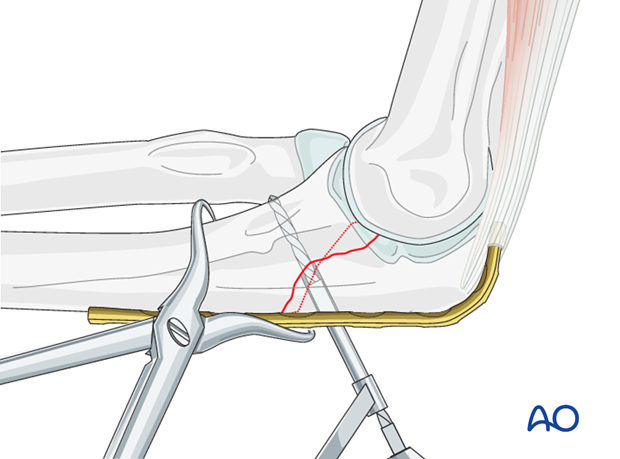
Measuring
Measure the depth of the hole with the hook of the depth gauge pointing distally.
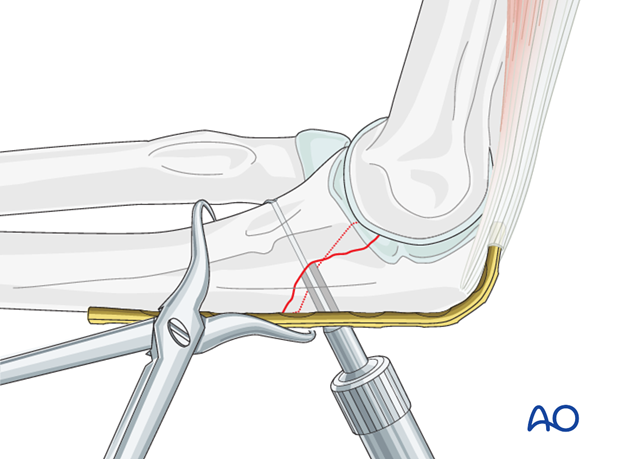
Insertion of the lag screw
Closely observe the compression effect on the fracture line while tightening the lag screw.
The reduction forceps should be removed just before the final tightening of the screw.
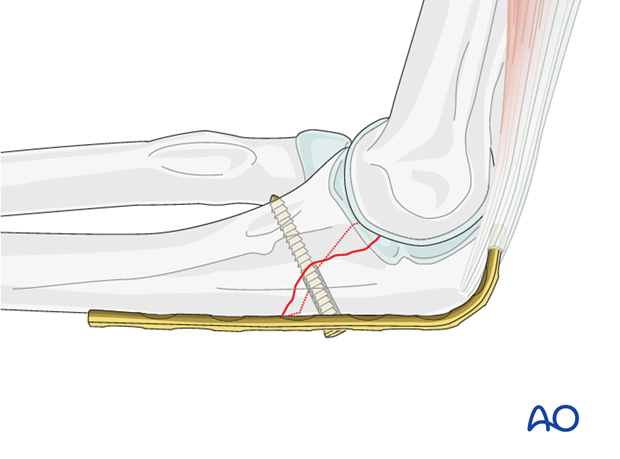
5. Finish plate fixation
Fix the plate to the bone with three screws proximal and three screws distal to the fracture in neutral position to protect the lag screw.
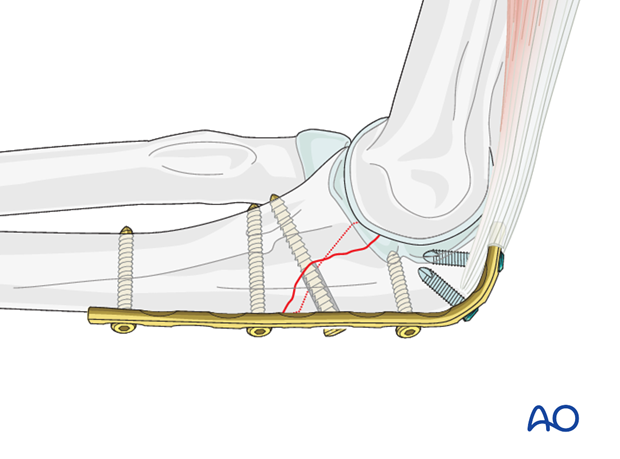
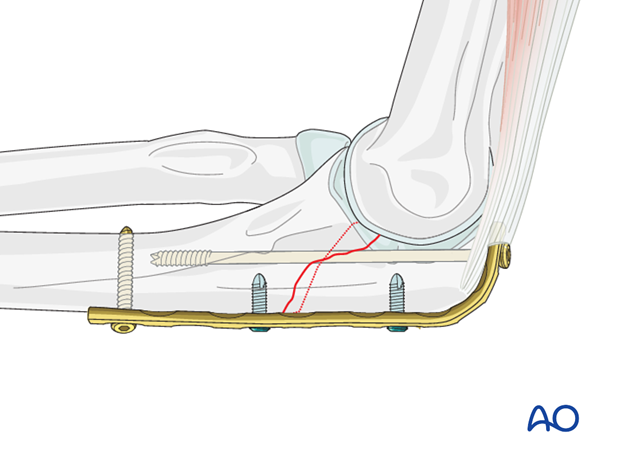
Alternatively, a so called "home run screw" can be placed as an intramedullary screw. This screw is a non-locking screw that can place thru a small stab incision in the triceps tendon. To allow passage of this long screw you can use unicortical locking screws distally. By drilling this long screw using the oscillating drilling technique there is low risk of an early extramedullary exit and/or screw interference with the more distal screws.
Assess the range of motion in pronation, supination, flexion and extension. Screw tips should not touch the radius.
Check results with image intensifier or x-ray.
Repair the small incision in the triceps over the plate.
6. Postoperative treatment following ORIF
Postoperatively, the elbow may be placed for a few days in a posterior splint for pain relief and to allow early soft tissue healing, but this is not essential. To help avoid a flexion contracture, some surgeons prefer to splint the elbow in extension.
If drains are used, they are removed after 12–24 hours.

Mobilization
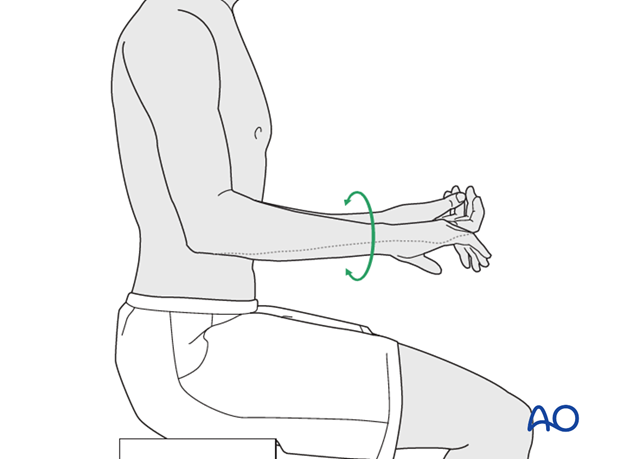
Active assisted motion is encouraged within the first few days including gravity-assisted elbow flexion and extension. Encourage the patient to move the elbow actively in flexion, extension, pronation and supination as soon as possible. Delay exercises against resistance until healing is secure.
Use of the elbow for low intensity activities is encouraged, but should not be painful.
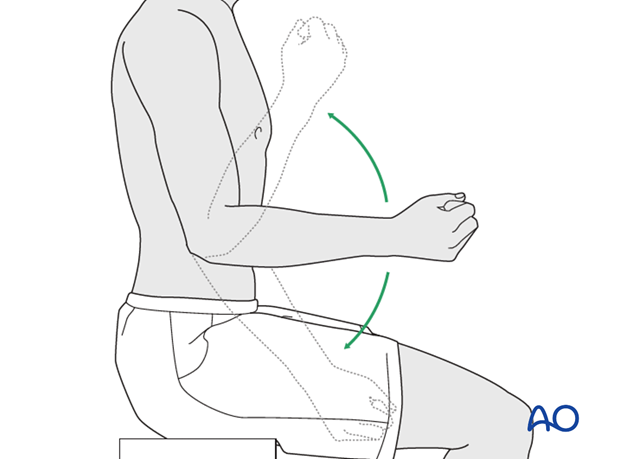
Range of motion must be monitored to prevent soft tissue contracture.
Prevent loading of the elbow for 6–8 weeks.
Monitor the patient to assess and encourage range of motion, and return of strength, endurance, and function, once healing is secure.
Follow up
The patient is seen at regular intervals (every 10–20 days at first) until the fracture has healed and rehabilitation is complete.
Implant removal
As the proximal ulna is subcutaneous, bulky plates and other hardware may cause discomfort and irritation. If so, they may be removed once the bone is well healed, 12–18 months after surgery, but this is not essential.













