Open reduction internal fixation
1. Introduction
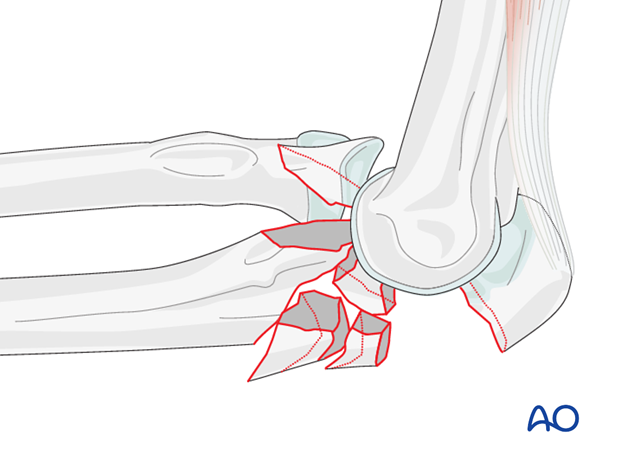
Complex fractures of the proximal ulna with anterior translation of the forearm with respect to the distal humerus are anterior (or trans-olecranon) fracture-dislocations of the elbow. The radial head is not fractured. The collateral ligaments are usually intact. When the coronoid is fractured, it is usually one large piece and is rarely fragmented.
Principles
- The radial head is not fractured.
- The collateral ligaments are usually uninjured.
- The key is restoration of the trochlear notch of the ulna by correct alignment of the coronoid and olecranon processes.
- Metaphyseal and diaphyseal fragmentation can be bridged with a long plate.
- Beware of substantial impaction in the depths of the trochlear notch. This may need a structural graft to prevent anterior subluxation of the forearm.
2. Positioning and approach
Positioning
This procedure is normally performed with the patient either in a lateral position or in a supine position for posterior access.
Approach
With the posterolateral approach a posterior skin midline incision can be used to raise both medial and lateral skin flaps.
Further dissection can proceed medially or laterally. Alternatively, raise olecranon fracture fragment with the triceps as with an olecranon osteotomy.
The Boyd approach is used to access the radial head as well as the olecranon and proximal ulna.
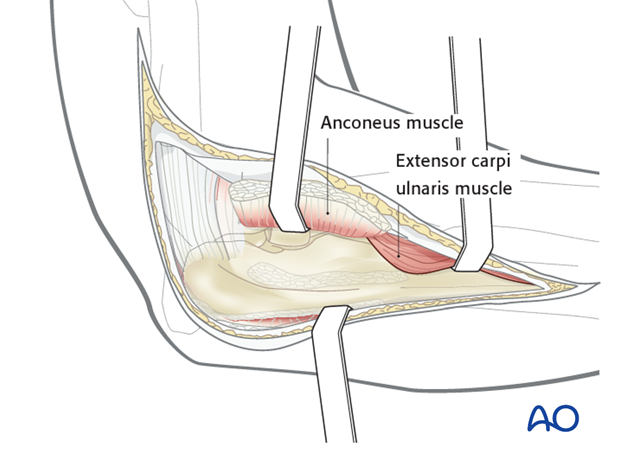
3. Fixation
Sequence of repair
- Address coronoid fracture.
- Address impaction of the articular surface in the center of the trochlear notch.
- Realign and secure the olecranon fragment

Coronoid repair
After mobilizing the olecranon process with the triceps, address the basilar coronoid fracture.
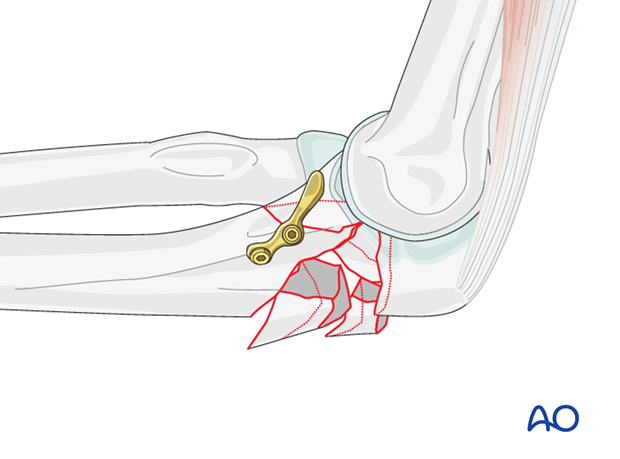
Impaction of the articular surface in the center of the trochlear notch
Realign fracture fragments in the center of the trochlear notch to ensure that the trochlea does not settle and allow the forearm to subluxate anteriorly.
Sometimes a structural bone graft from the iliac crest is helpful.
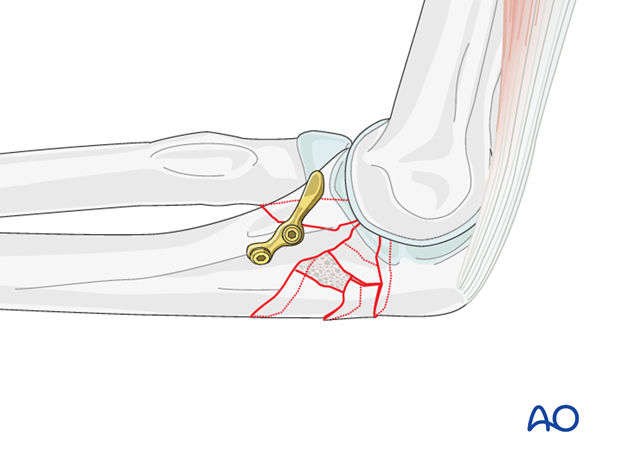
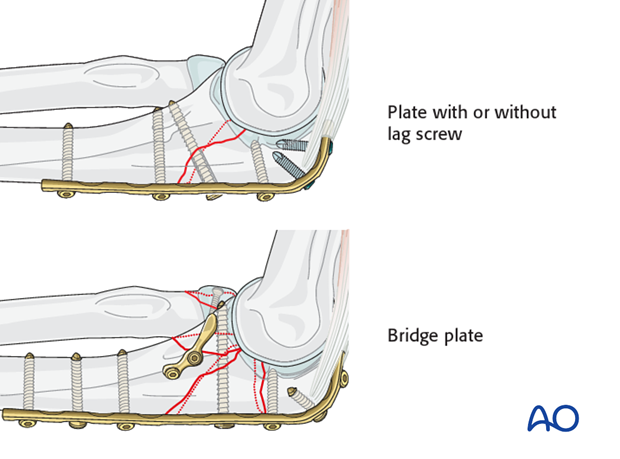
Repair the olecranon with a posterior plate
- Simple: Plate with or without lag screw
- Multifragmentary: Bridge plate
4. Final assessment
The MCL and LCL are usually intact. Fixation of the olecranon and coronoid should restore stability to the elbow. Check the alignment of the radial head with the capitellum through a full arc of elbow flexion and extension and forearm rotation to be sure there is no ulnar malalignment. Also, be sure there is no crepitation in the joint suggesting errant screws or persistent joint malalignment.
5. Case
Complex, intraarticular, proximal ulnar fracture dislocation, with associated distal ulnar shaft fracture.
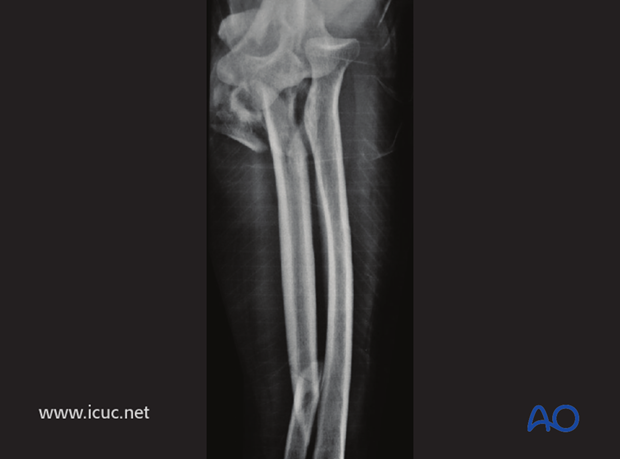
Lateral image of fractures.
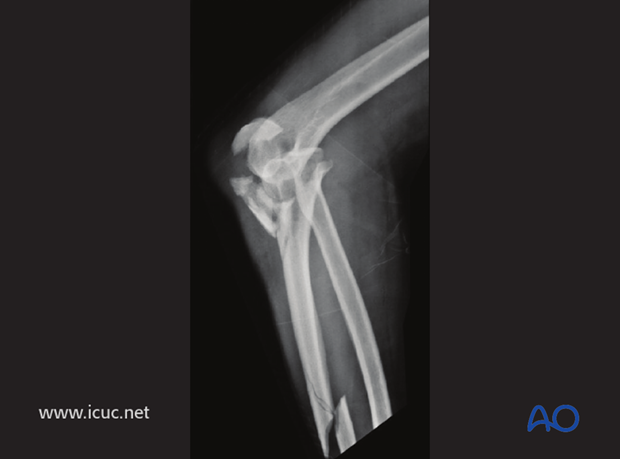
CT showing complex fracture dislocation of proximal ulna
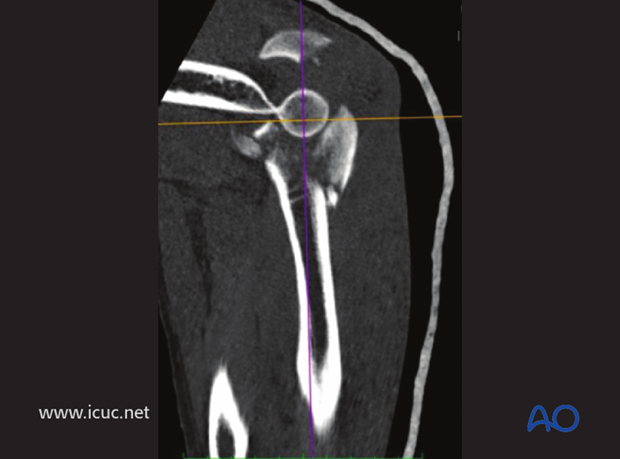
3D CT showing complex fracture dislocation.
A direct posterior approach is used, allowing exposure from the olecranon to the distal ulna because of the segmental fracture.
The complex proximal fracture is exposed, and the fragments identified.
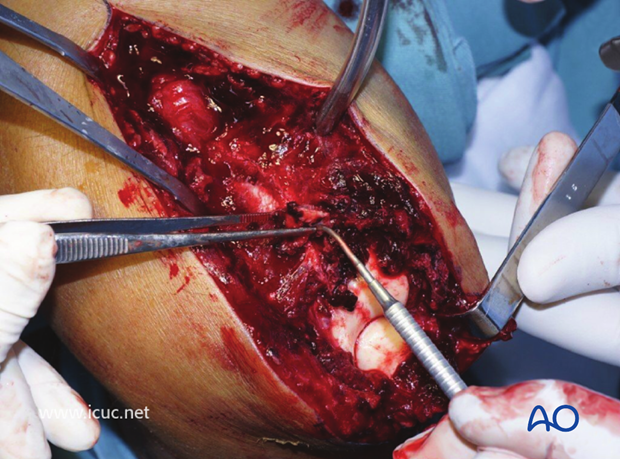
This image shows the cartilage damage after such a severe elbow injury, and one piece of unattached osteochondral bone being removed.
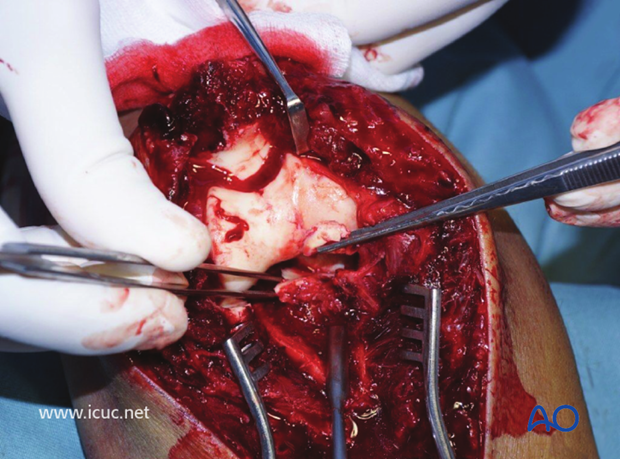
This direct posterior approach allows for the easy visualization of the coronoid fracture which in this instance is very comminuted. Here a K-wire is being placed for reconstruction of the comminuted coronoid.
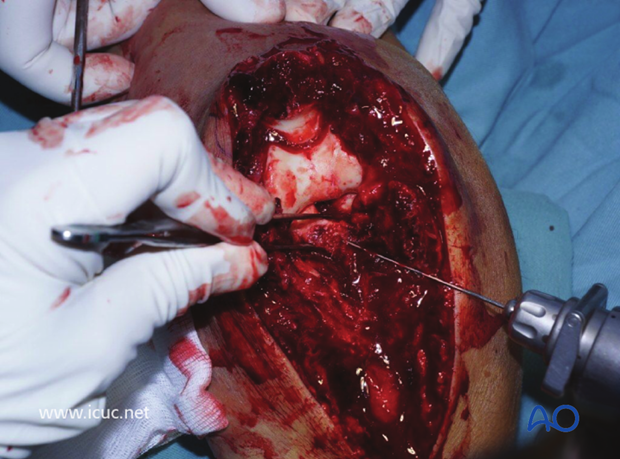
Here a K-wire is being used to reconstruct the surface of the coronoid before definitive bridging fixation.
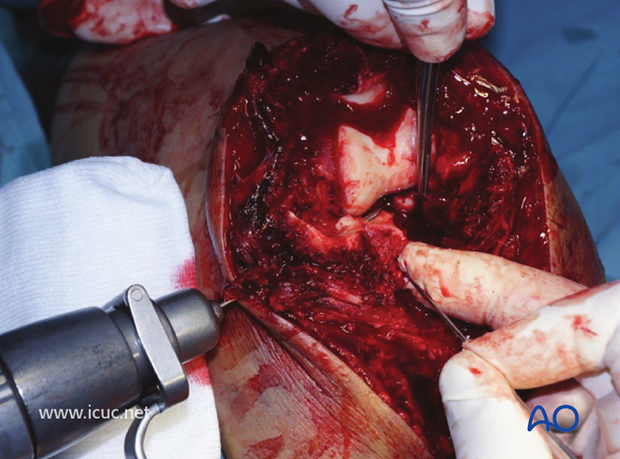
Once the coronoid is reconstructed the olecranon can be reduced to the shaft.
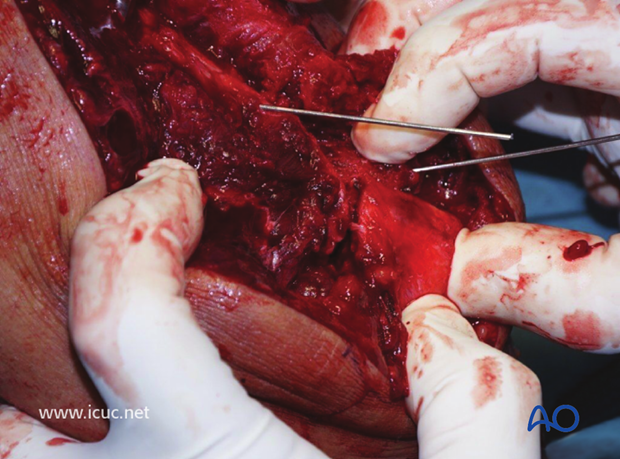
The olecranon is temporarily held with K-wires.
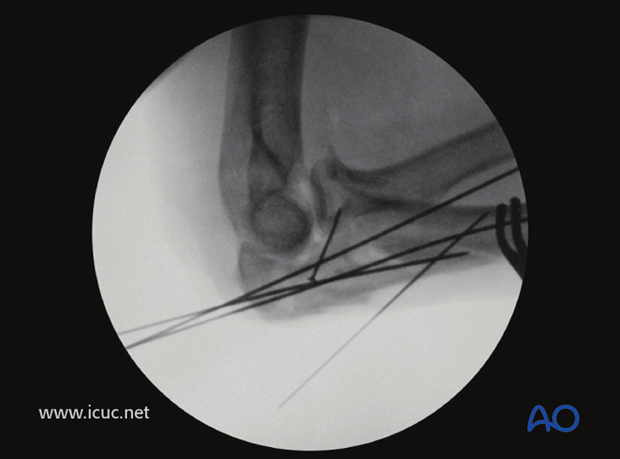
This lateral X-ray shows a single lag screw into the coronoid along with multiple K-wires temporarily holding the fracture dislocation reduced.
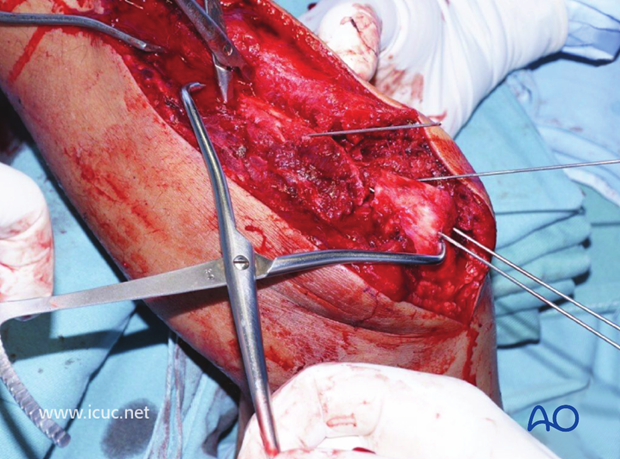
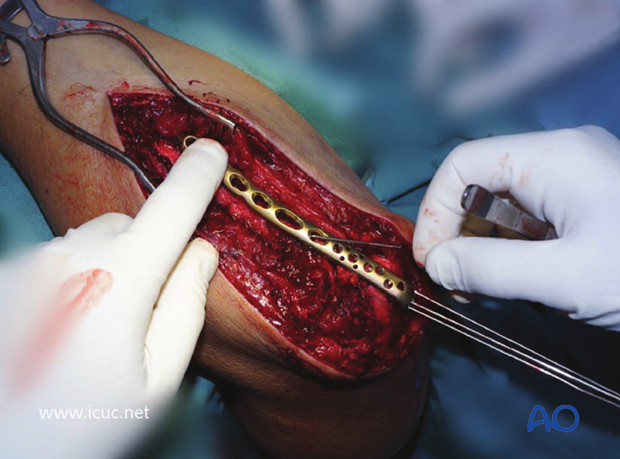
The proximal ulnar LCP is applied and the plate is firmly held against the ulna to help in the reduction of the comminuted proximal ulna.
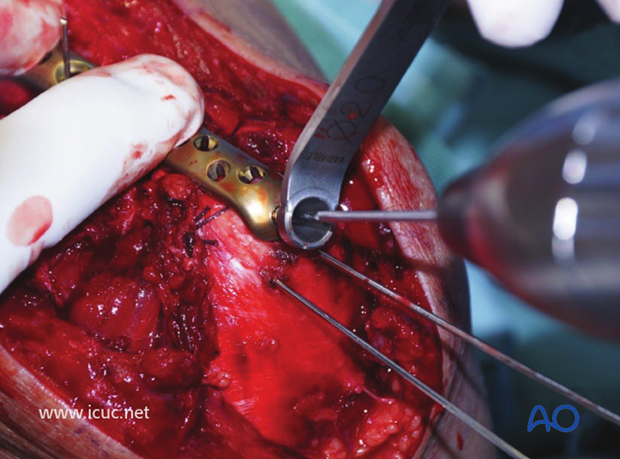
A variable angle screw is inserted into the proximal ulna to supplement the K-wire fixation.
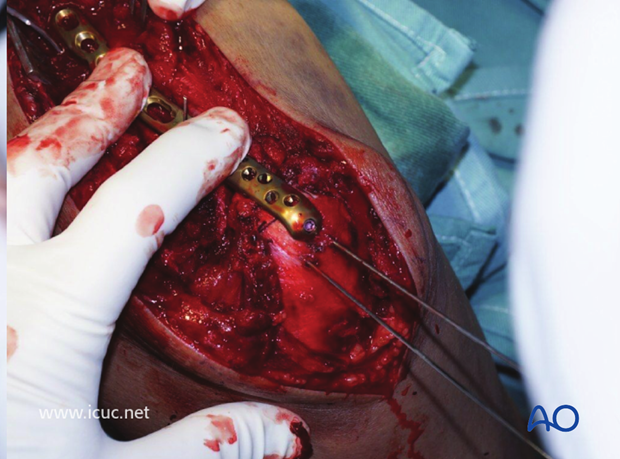
This plate does not have many points for proximal fixation, so supplementary K-wire fixation is advised as well.
Once the ulna is brought out to length, the fracture is bridged and a screw is applied to maintain length.
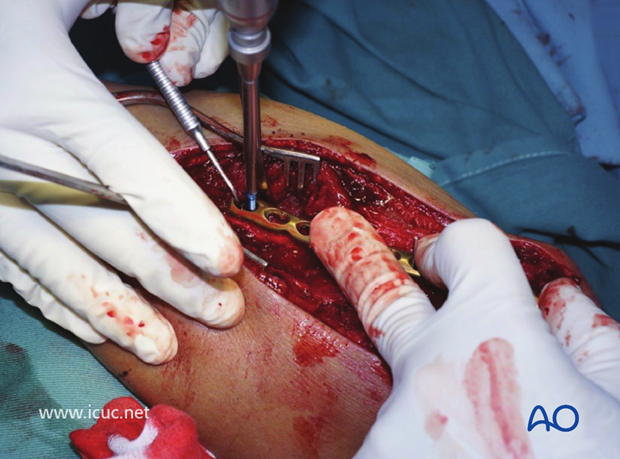
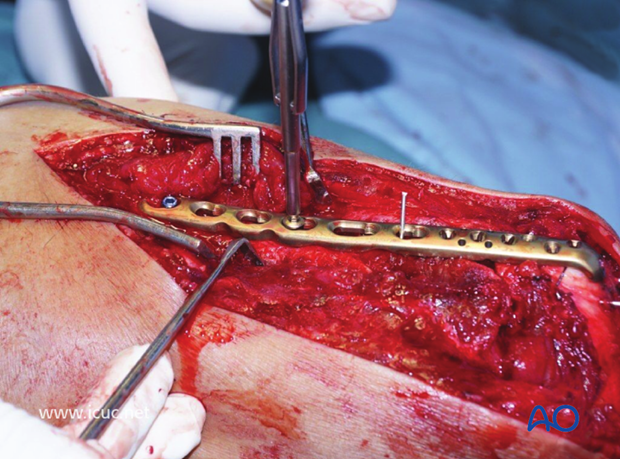
This image shows the proximal ulna reduced and bridged with both proximal and distal fixation.
AP image showing the coronoid reduction.
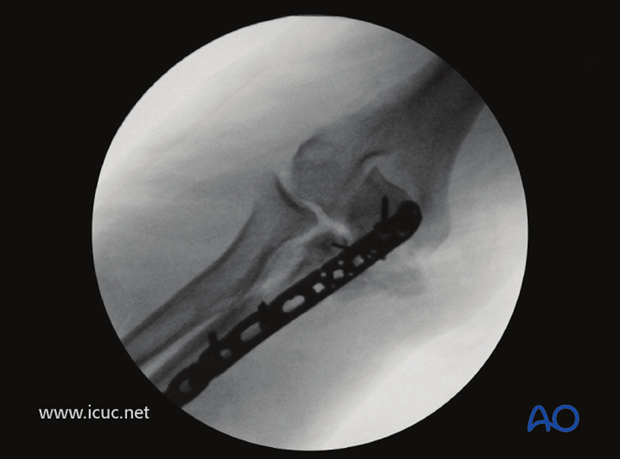
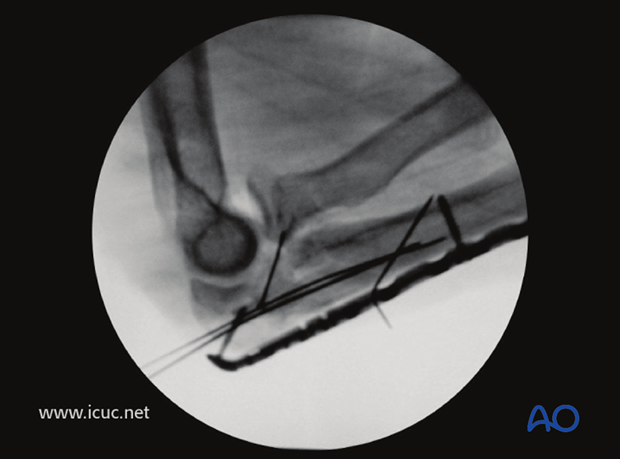
Lateral image showing satisfactory reconstruction of the proximal ulna, but the radial head is not completely reduced in the radiocapitellar joint.
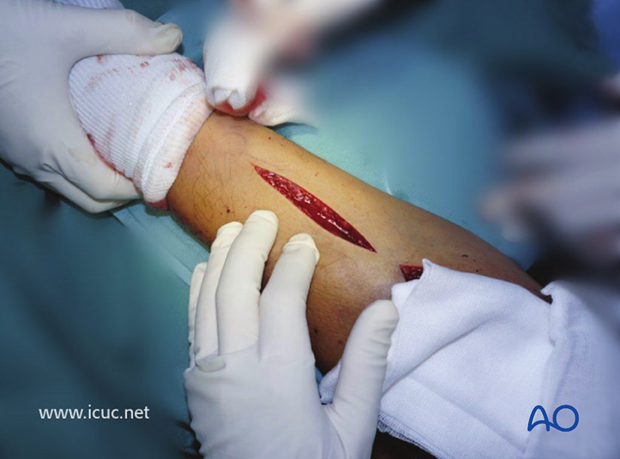
A distal incision is made to expose the distal ulnar shaft fracture. If necessary, this incision can be extended proximally to join with the distal end of the previous incision.
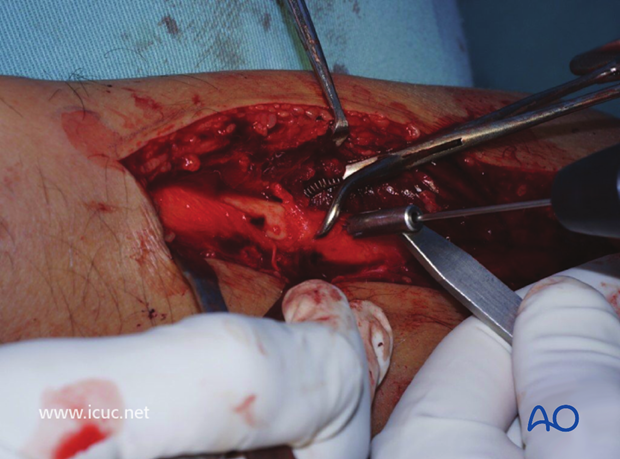
The fracture is held reduced with a clamp and a hole is drilled for lag screw.
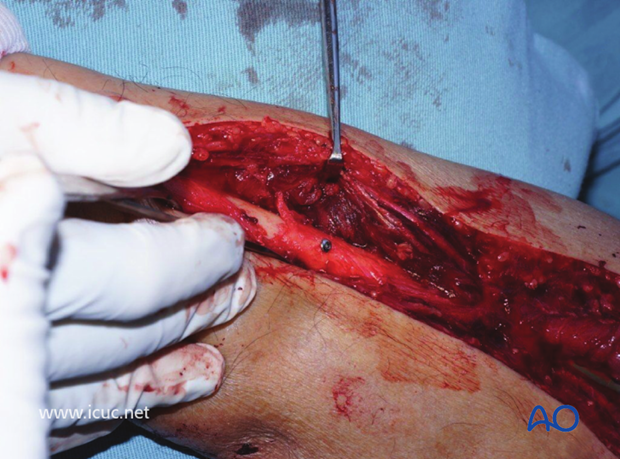
The hole is countersunk and a lag screw inserted.
A large reconstruction plate was selected and applied in neutralization mode.
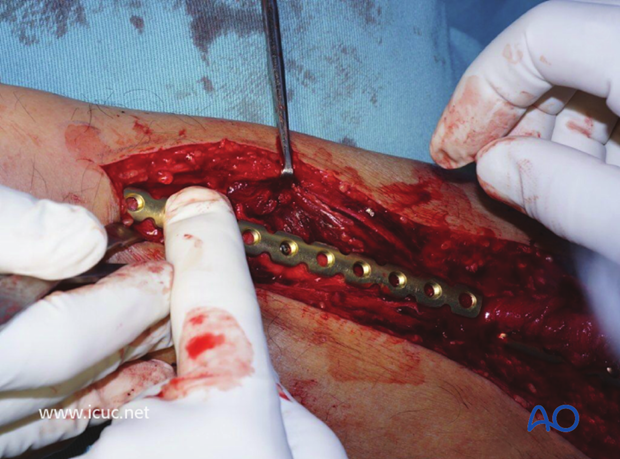
Screws are inserted in neutral mode.
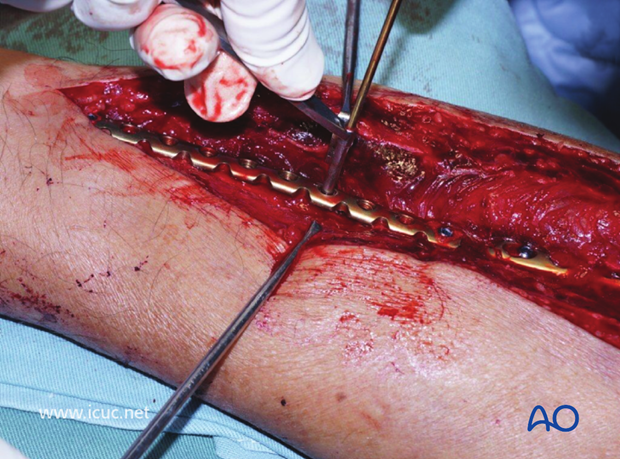
Note there is only a small gap between the two plates, which creates a stress riser. This could have been avoided if a shorter proximal VA-LCP plate had been selected. Alternatively, a longer distal plate could have been chosen so that the two plates overlapped.
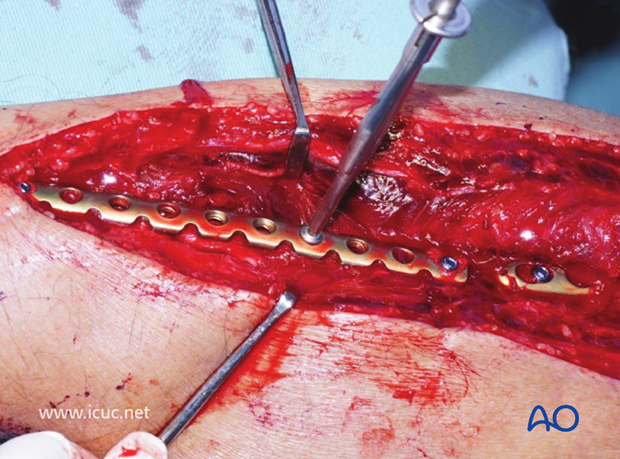
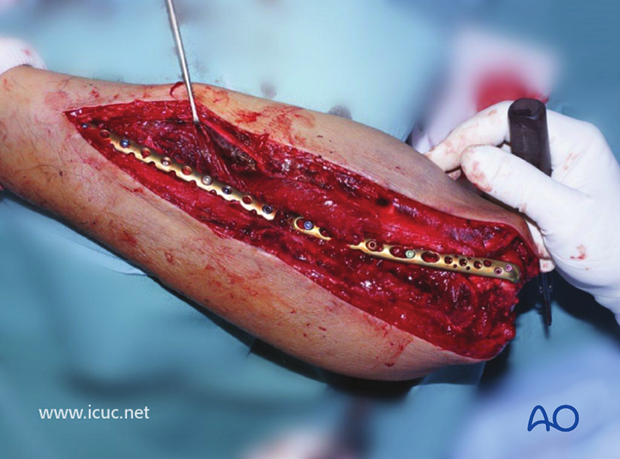
Final image prior to closure
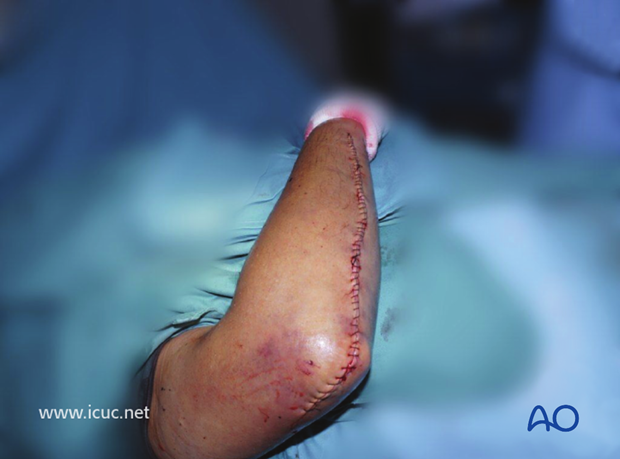
Final closure
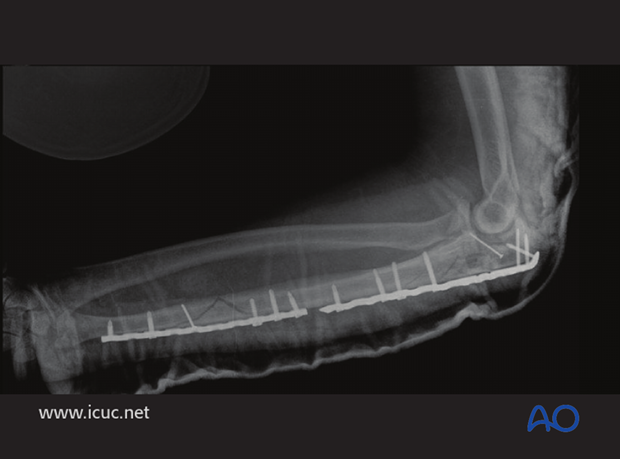
Lateral X-ray showing fixation of both fractures. The radial head is now reduced.
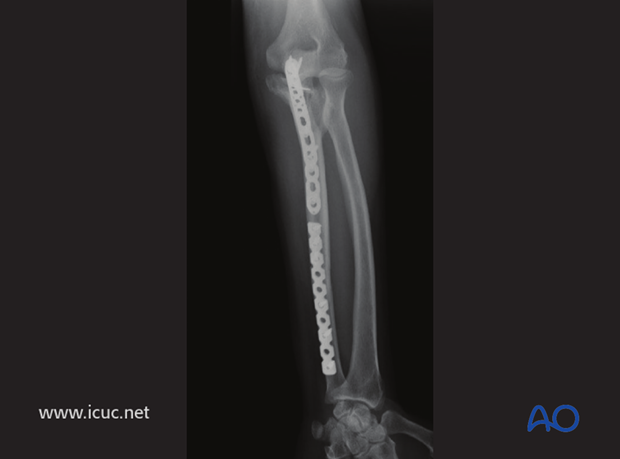
AP of elbow and forearm showing adequate reduction of the proximal ulna
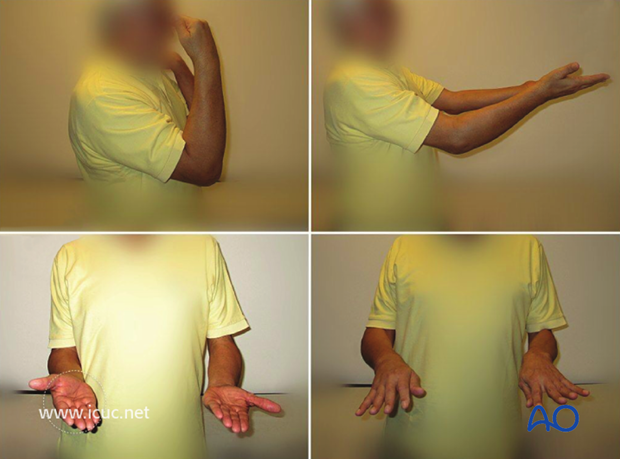
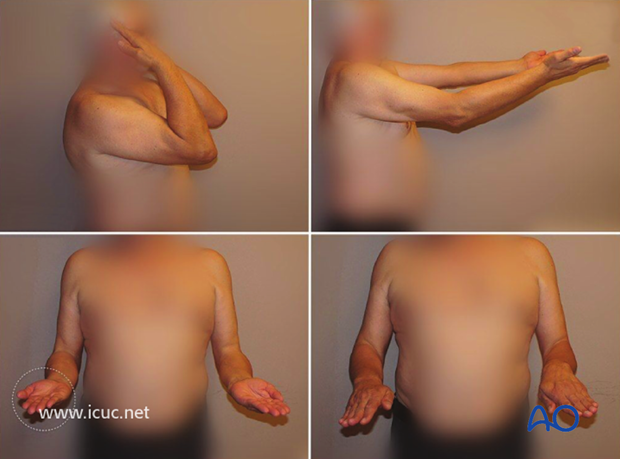
7 week clinical images showing gradual return of elbow function
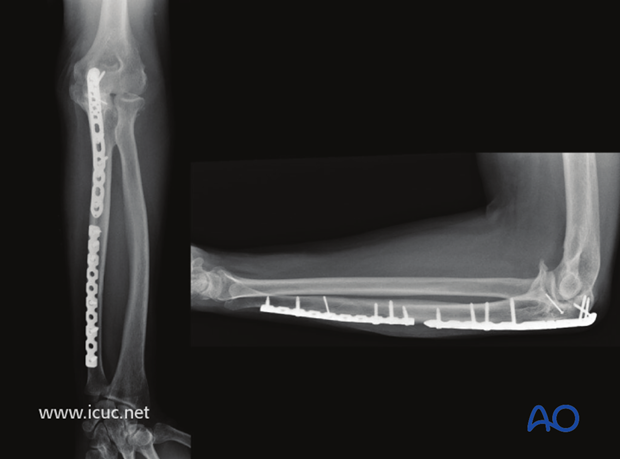
1.5 years AP and lateral X-rays showing complete healing
Final, 1.5 year clinical images showing slight loss of extension, but otherwise good elbow function.
6. Postoperative treatment following ORIF
Postoperatively, the elbow may be placed for a few days in a posterior splint for pain relief and to allow early soft tissue healing, but this is not essential. To help avoid a flexion contracture, some surgeons prefer to splint the elbow in extension.
If drains are used, they are removed after 12–24 hours.

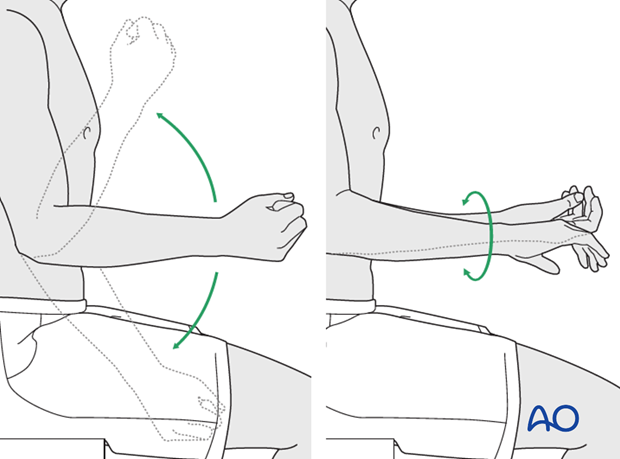
Mobilization
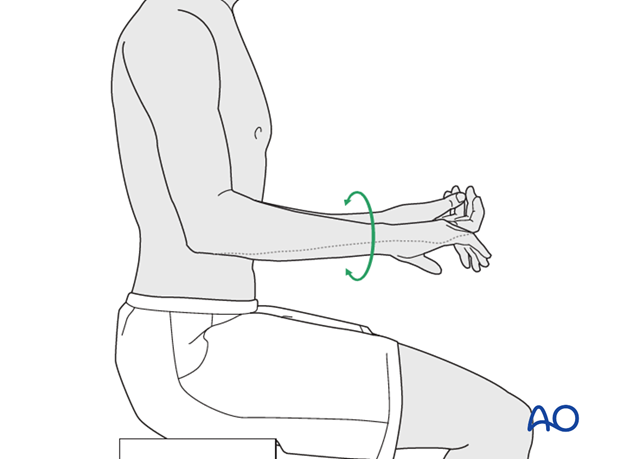
Active assisted motion is encouraged within the first few days including gravity-assisted elbow flexion and extension. Encourage the patient to move the elbow actively in flexion, extension, pronation and supination as soon as possible. Delay exercises against resistance until healing is secure.
Use of the elbow for low intensity activities is encouraged, but should not be painful.
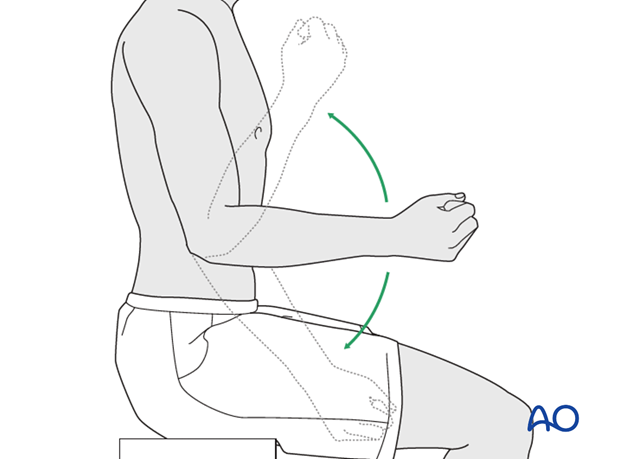
Range of motion must be monitored to prevent soft tissue contracture.
Prevent loading of the elbow for 6–8 weeks.
Monitor the patient to assess and encourage range of motion, and return of strength, endurance, and function, once healing is secure.
Follow up
The patient is seen at regular intervals (every 10–20 days at first) until the fracture has healed and rehabilitation is complete.
Implant removal
As the proximal ulna is subcutaneous, bulky plates and other hardware may cause discomfort and irritation. If so, they may be removed once the bone is well healed, 12–18 months after surgery, but this is not essential.













