Tension band wiring
1. General considerations
Stabilization of the greater trochanter
Tension band fixation is using K-wires and a figure-of-eight wire.
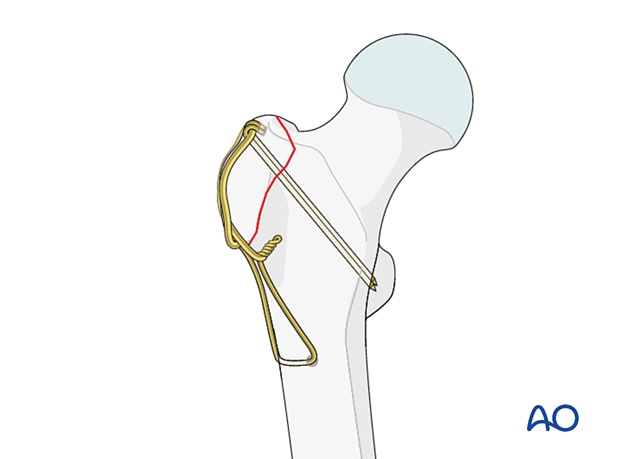
Option: tendon sutures
Sutures stitched in a Krakow fashion in the gluteus medius tendon may be used to facilitate reduction of the greater trochanter fragment.
In poor-quality bone, this can also be used to augment a tension band construct.
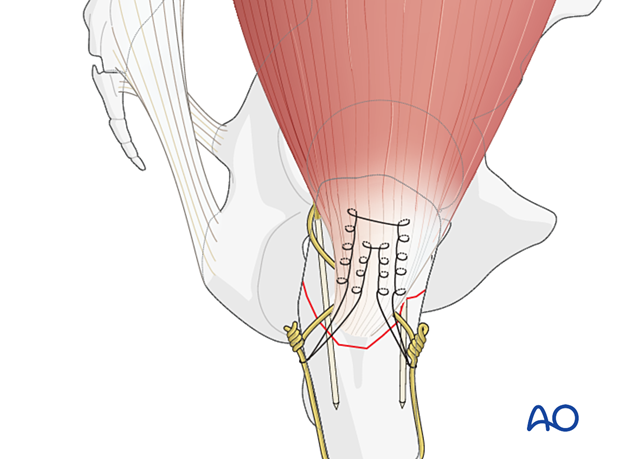
2. Patient preparation and approach
Patient positioning
Place the patient supine on a radiolucent table with a bump under the buttock.
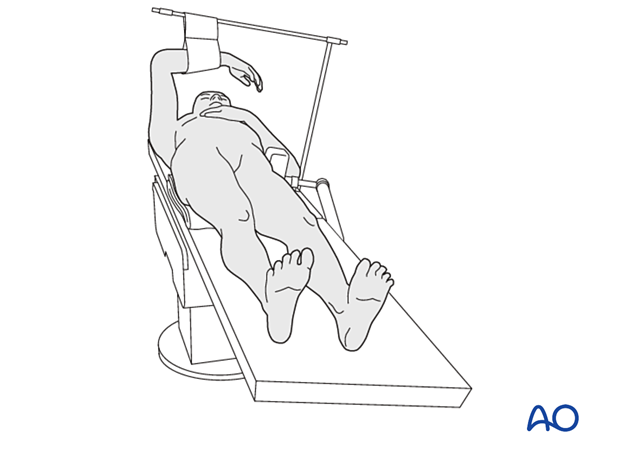
Approach
For this procedure, a direct lateral approach centered over the tip of the greater trochanter is used.
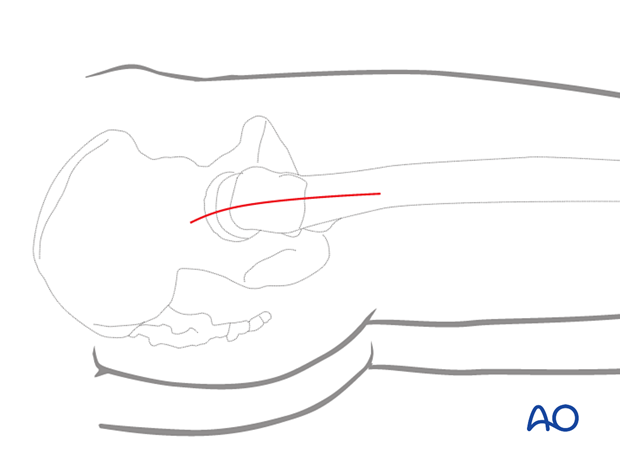
3. Reduction
Clear any hematoma.
Directly reduce the fragment and stabilize it with pointed bone reduction forceps.
The collinear reduction forceps can be extremely helpful in facilitating reduction. It is applied from the direct lateral incision with proximal extension.
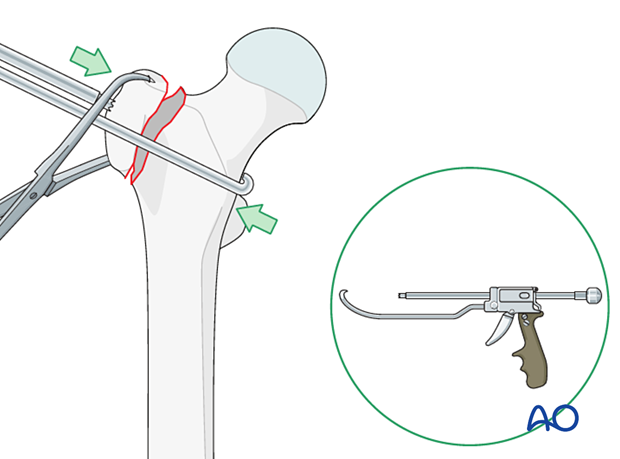
Option: tendon sutures as reduction aid
Stitch strong nonbioabsorbable sutures in a Krackow fashion on the top of the gluteus medius tendon.
At the end of the procedure, the sutures can be anchored under the loop of the wire.
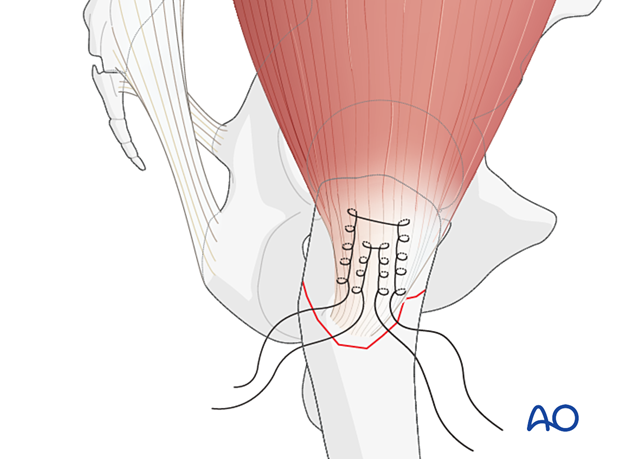
4. Tension band wiring
K-wire insertion
Drill two parallel 2.0 mm K-wires from the greater trochanteric fragment across the medial cortex. Retract the wires slightly to allow final seating after bending the proximal end. The posterior K-wire may engage in the lesser trochanter.
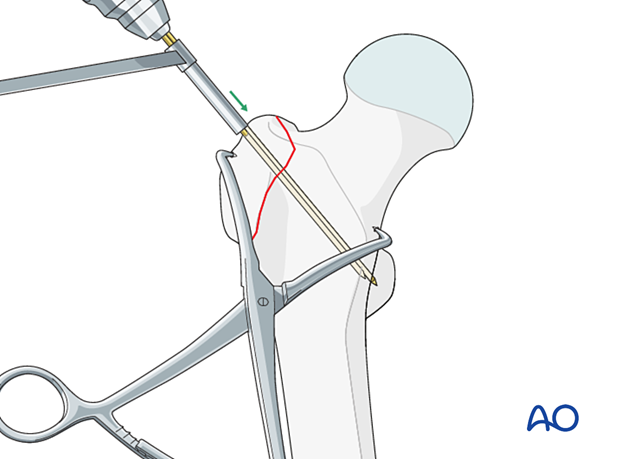
Wire positioning
Create a hole in the lateral cortex of the intact femoral diaphysis by drilling the anterior and posterior cortex separately.
Alternatively, use an anchor screw with a washer inserted from lateral.
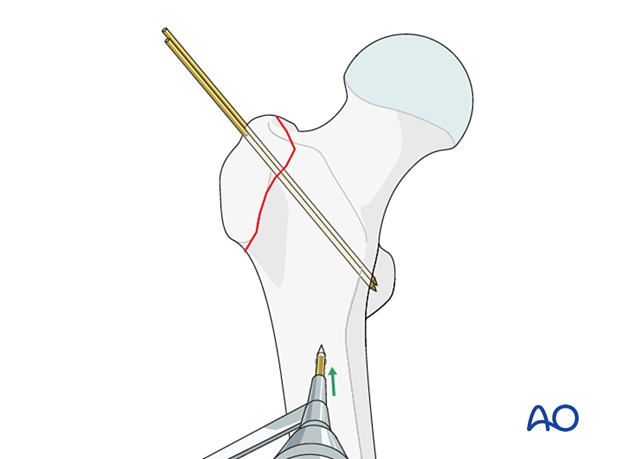
Pass an 18-gauge wire through the hole and bring it proximally in a figure-of-eight fashion around the origin of the K-wires and through the gluteus medius tendon.
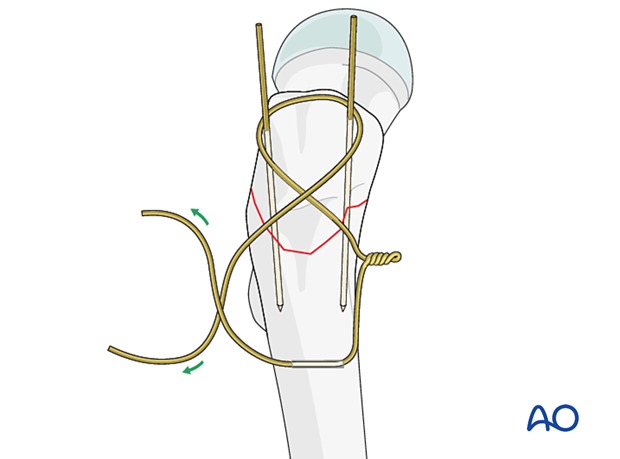
Wire tensioning
Tension the wire on both sides of the figure-of-eight in a helical manner for a minimum of four rotations.
Bend the ends of the wire and impact into the cortex of the femur so that they are not prominent.
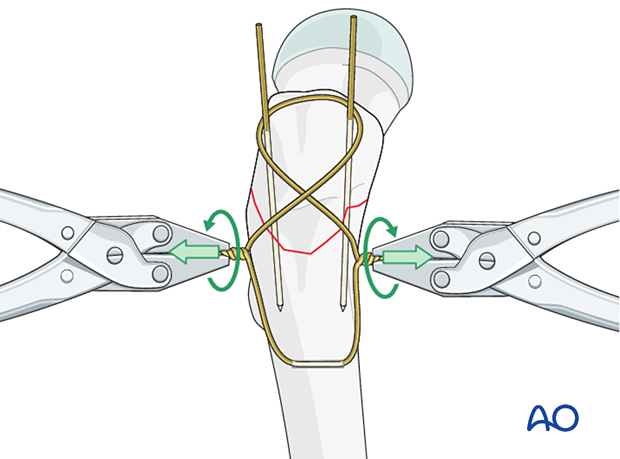
Bending the K-wires
Bend the K-wires as much as possible with a drill sleeve. If necessary, increase the bend with pliers close to the bone.
Cut the K-wires to create a sharp tip about 5 mm from the bending point.
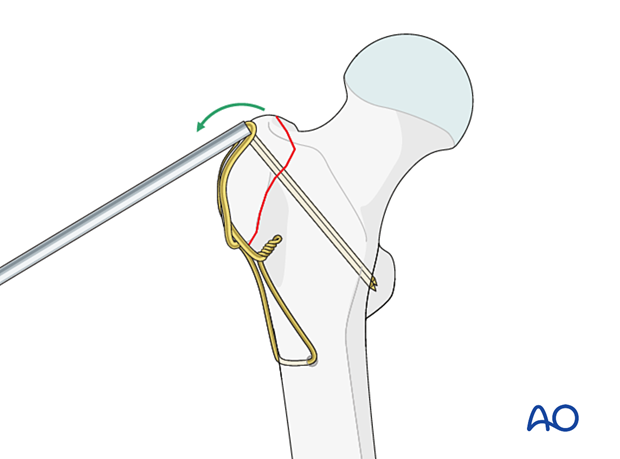
Turn the ends of the K-wires to capture the figure-of-eight wire, and then impact the K-wires firmly, so their sharp tips are buried in the bone.

Option: tendon-suture fixation
After finishing the tension band wiring, secure the ends of the tendon suture under the loop of the wire.

5. Final assessment
Confirm complete reduction, stability, and range of motion.
Obtain AP and lateral x-rays to confirm correct implant position.
6. Aftercare
Postoperative mobilization
Weight-of-the-leg weight bearing with walking aids will decrease the pull of the abductors on the fragment and is recommended for 4–6 weeks.
Pain control
To facilitate rehabilitation and prevent delirium, it is important to control the postoperative pain properly, eg, with a specific nerve block.
VTE prophylaxis
Patients with lower extremity fractures requiring treatment require deep vein prophylaxis.
The type and duration depend on VTE risk stratification.
Follow-up
Follow-up assessment for wound healing, neurologic status, function, and patient education should occur within 10–14 days.
At 3–6 weeks, check the position of the fracture with appropriate x-rays.
Recheck 6 weeks later for progressive fracture union.













