ORIF
1. General considerations
Introduction
When both the femoral head and posterior wall are fractured, preoperative imaging allows the surgeon to determine which fracture needs ORIF. If the head fracture is small and not impinging, it is neglected, and the wall fracture is treated as described in the acetabular section. If the posterior wall fracture does not need to be fixed, the femoral head fracture is treated as described in the corresponding section of the proximal femur.
When both fractures require reduction and stabilization, a trochanteric osteotomy with surgical hip dislocation allows both fractures to be managed preserving femoral head blood supply. The procedure involves exposure and fixation of the femoral head followed by stabilization of the posterior wall.
The reduction and fixation of the femoral head fracture with screws is shown in this procedure. The posterior wall fracture is reduced and fixed according to the procedures given in the acetabular module of Surgery Reference.
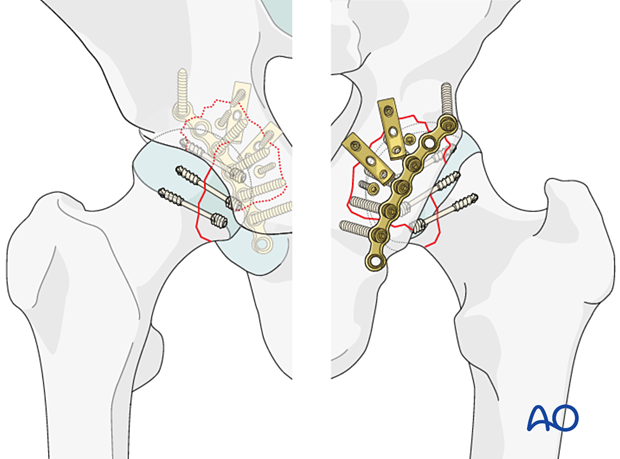
Principles of screw fixation
Articular fragments need to be reduced anatomically and may be stabilized with absorbable screws, recessed small cancellous lag screws, or headless compression screws.
For rotational stability, two screws should be used in each fragment if possible.
Prognosis of stabilized split fractures of the femoral head
The outcome of stabilized suprafoveal split fractures remains unpredictable even after anatomical joint restoration.
Implant selection
Absorbable screws do not need removing but may be relatively weak.
If metal screws are used, titanium is a better choice than steel, as it does not interfere with subsequent MRI imaging.
When inserted subchondrally, intraosseous headless compression screws cause less damage to the articular cartilage than conventional screws, and there is less risk of a prominent screw head causing secondary articular surface damage.
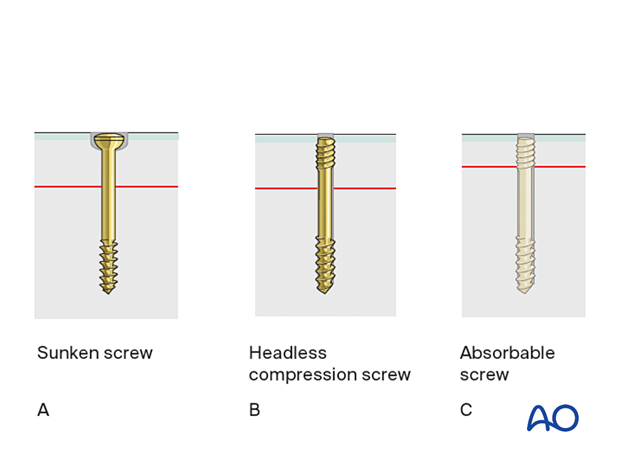
2. Patient preparation and approach
Patient preparation
Position the patient in a lateral decubitus position.
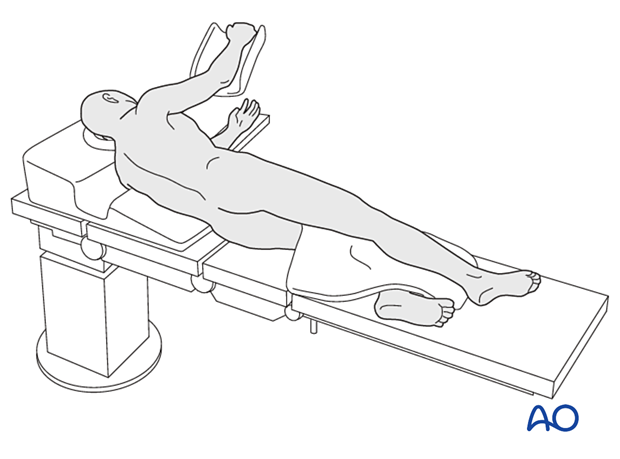
Approach
For this procedure, a trochanteric flip osteotomy should be used to address both fractures with one surgical approach.
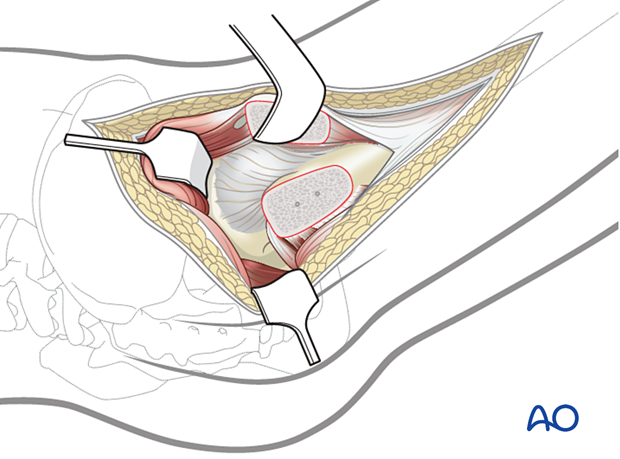
3. Reduction and fixation of femoral head split
Open reduction
Reduce the fragment directly and maintain reduction with pointed forceps.
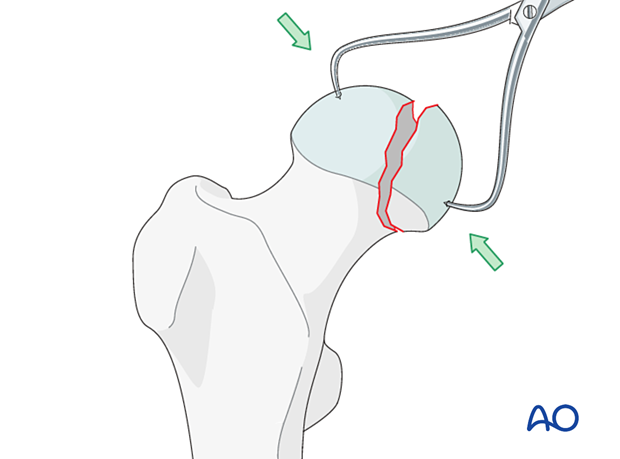
Fixation
Preliminary fixationBefore definitive fixation with screws, secure the fragment with a minimum of two K-wires to avoid rotational redisplacement during screw insertion.
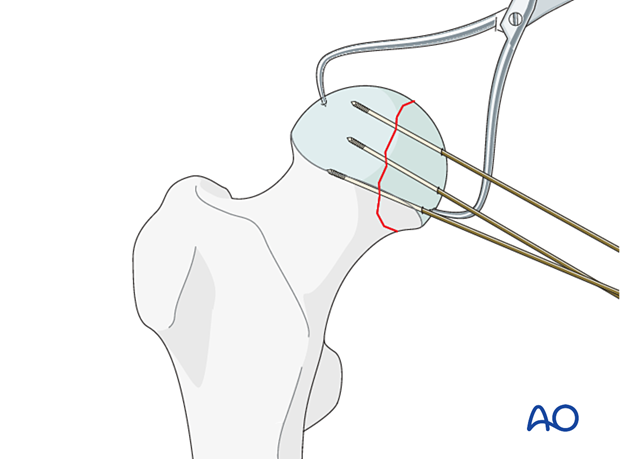
Fix the fragment with either recessed small cancellous lag screws or headless compression screws.
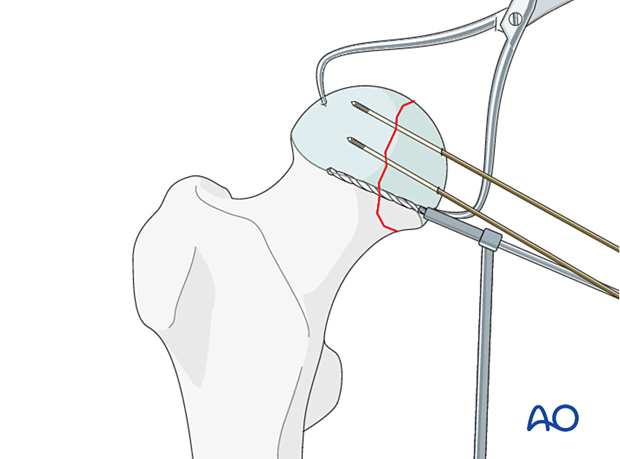
Choose screws long enough so that the thread is beyond the fracture line.
A single screw does not provide rotational stability. If the size of the fragment allows, use at least two screws.
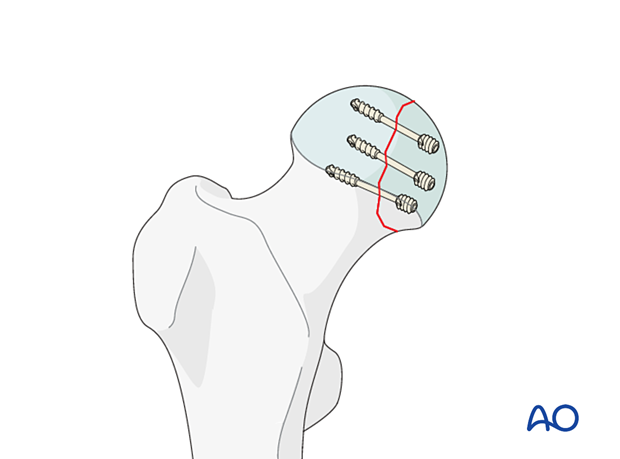
4. Reduction of hip joint
Once the head fracture is fixed, reduce the hip joint.
5. Reduction and fixation of posterior wall fracture
The posterior wall fracture is reduced and fixed according to the procedure given in the acetabular module of Surgery Reference. For details, navigate to:
- Acetabulum - Posterior wall - ORIF through trochanter osteotomy extension
At the end of this procedure, fix the trochanteric osteotomy with two or three screws.
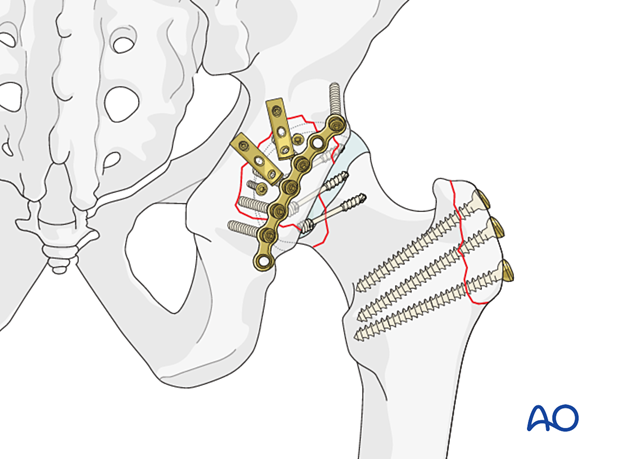
6. Final assessment
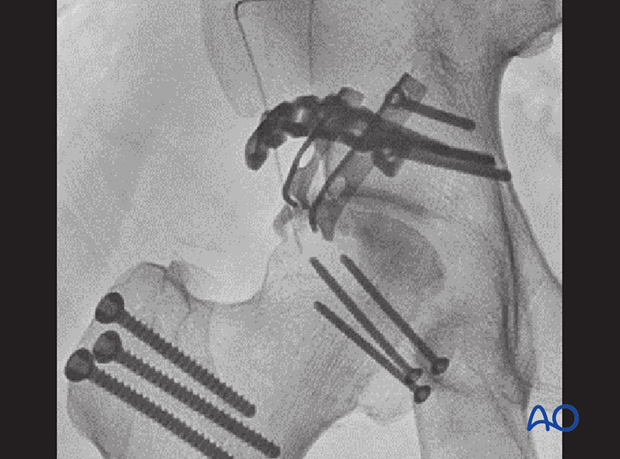
Confirm fracture stabilization, joint reduction, and implant position on AP, Judet, and lateral views.
7. Aftercare
Dislocation precautions
Since most femoral head fractures are associated with a hip dislocation, precautions against redislocation should be taken for the first 6 weeks after injury.
Low seats and toilets, flexing the hip when arising, sitting with legs crossed, as well as squatting and kneeling may also be avoided initially, as should pivoting on the affected leg. The patient and caregivers may be encouraged to use additional support when rising from a sitting position.
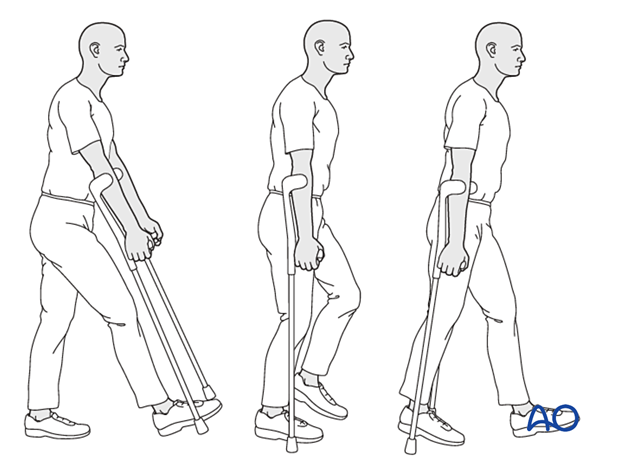
Postoperative mobilization
Since the fractures are articular, weight-of-the-leg weight bearing is advised up to 8 weeks and then advanced.
Range-of-motion exercises should start cautiously in the immediate postoperative period to prevent stiffness while avoiding dislocation.
Pain control
To facilitate rehabilitation and prevent delirium, it is important to control the postoperative pain properly, eg, with a specific nerve block.
VTE prophylaxis
Patients with lower extremity fractures requiring treatment require deep vein prophylaxis.
The type and duration depend on VTE risk stratification.
Follow-up
Follow-up assessment for wound healing, neurologic status, function, and patient education should occur within 10–14 days.
Check the condition of the injury with appropriate x-rays at six weeks.
Longer follow-up, at 6 months and 1 year, is indicated to assess the development of posttraumatic arthritis and/or avascular necrosis.













