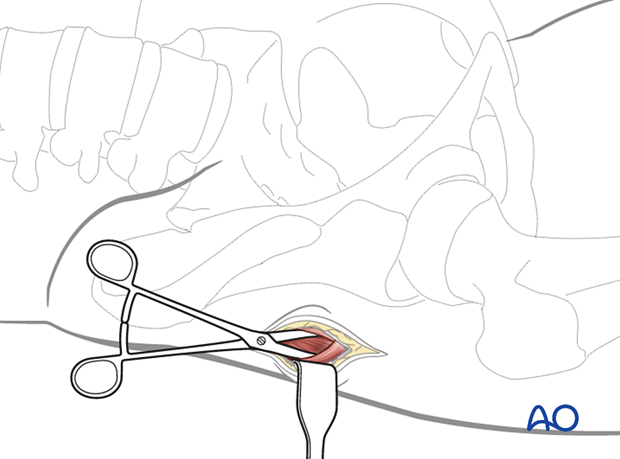
Approach for proximal femoral nailing
1. General considerations
Determination of the entry point
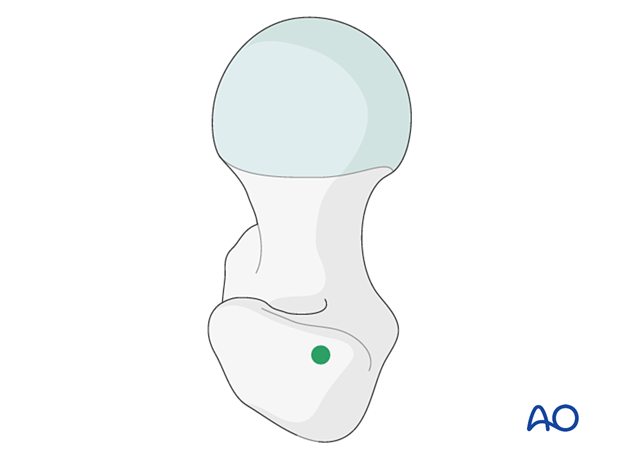
Most intramedullary nails designed for trochanteric fractures enter through the greater trochanter and not the trochanteric fossa.
The precise entry point in the greater trochanter depends upon the design of the nail. The surgeon must be familiar with the selected implant system.
Fracture deformity (typically flexion and/or abduction) may make locating the desired entry point difficult. Realigning the proximal femur with a Schanz screw and/or ball-spiked pusher, placed percutaneously, are helpful solutions.
Particularly for long nails, it is important that the incision and entry point lie somewhat posteriorly along the anatomical axis of the femur.
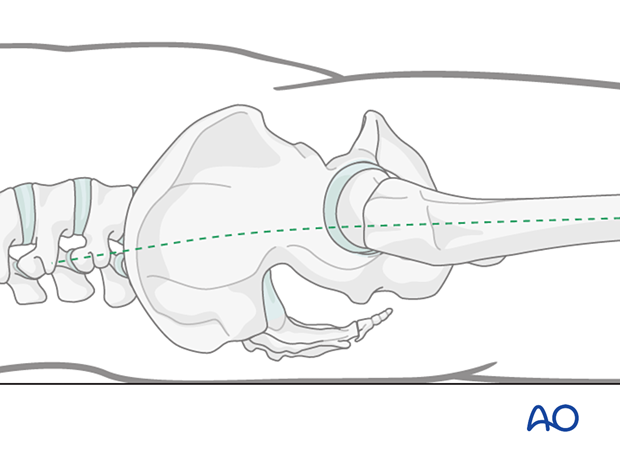
Planning for skin incision
The incision for nail insertion must lie along the curved axis (dashed line) of the femoral canal. This is somewhat posterior to what one might expect.
By making the incision in line with the path that the instruments and nail must travel, it is easier to avoid errors that may lead to eccentric reaming or perforation of the posterior femoral shaft cortex.
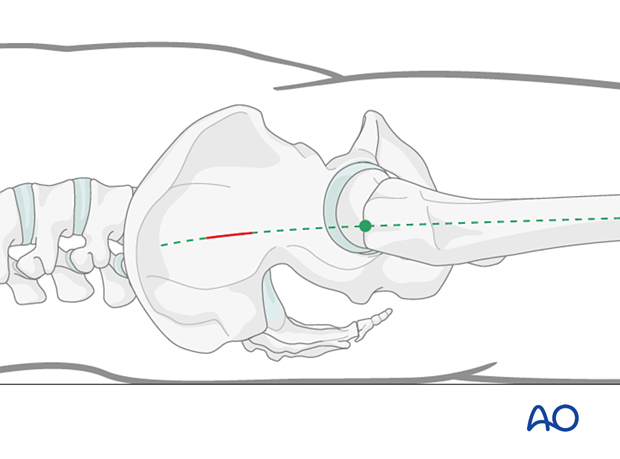
2. Skin incision
Begin by identifying the tip of the greater trochanter and the axis of the femur. Mark these on the skin with the help of the image intensifier, if necessary.

Make a 3–5 cm skin incision several centimeters proximal to the tip of the greater trochanter. As shown, this lies on the proximal extension of the bowed axis of the femoral shaft. The exact location of the skin incision depends on the soft-tissue envelope thickness of the patient and the type of insertion handle/type of nail used.
3. Deep incision
Make a 3–8 cm straight longitudinal incision in the fascia of the gluteus muscle, centered on the skin mark.
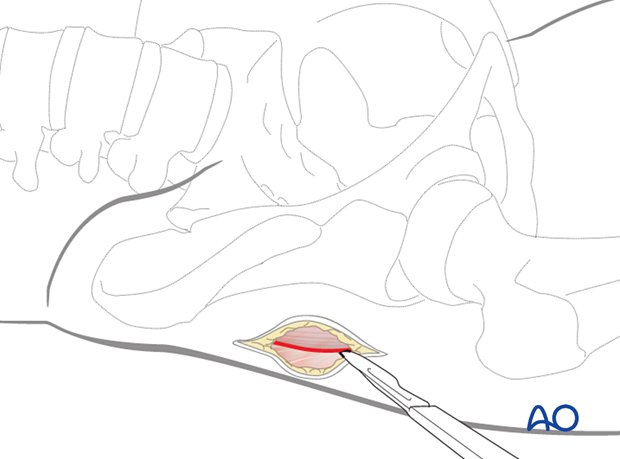
Split the fibers of the gluteal muscles by blunt dissection to gain access to the tip of the trochanter, which is best identified with a finger or instrument.