MIO - Iliosacral screw for sacrum
1. Introduction
Iliosacral screw (ISS) fixation is a fluoroscopically guided, percutaneous procedure. Its primary use is for fixation of satisfactorily reduced sacro-iliac joint disruptions or sacral fractures (described in a separate procedure). Anatomic reduction must be obtained before ISS insertion.
Screw placement and angulation will depend on patients specific anatomy (variations are common).
Principles of ISS fixation for SI joint
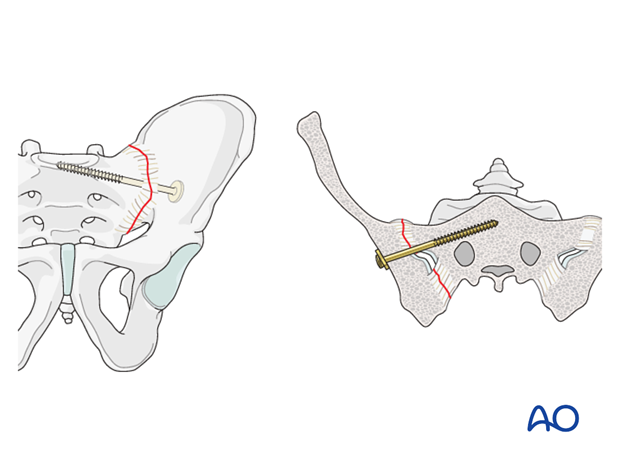
A partially threaded lag screw is used for joint compression.
A washer is necessary to maximize purchase on the ilium without burying the screw head in the bone.
Fixation failure may occur, especially with grossly unstable injuries. Fixation can be enhanced by one or more of the following:
- 1 or 2 additional screws (S1 or S2 level)
- Supplementary plates, posteriorly or anteriorly
- Anterior arch fixation increases stability
2. Preoperative planning
An explicit, written pre-operative plan is strongly encouraged. In addition to overall assessment and preoperative planning, specific considerations are required for ISS.
These are:
- Patient's individual pelvic anatomy (normal vs. dysmorphic)
- Patient's specific SI joint injury configuration
- Optimal ISS type, location. and length
- Selection of screw channels
- Need for enhanced fixation (see above)
3. Imaging
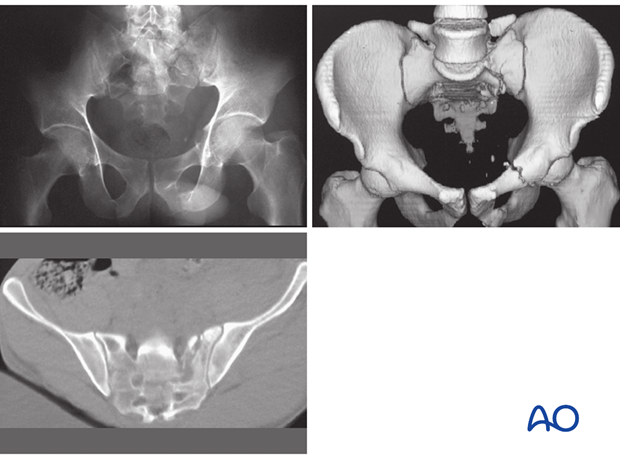
CT analysis
High quality pelvic CTs are crucial for planning reduction maneuvers and safe, effective paths for ISS placement.
In addition to trans-axial images, sagittal and coronal reconstructions should be studied, with x-ray or CT views of the entire pelvis, including 3-D images if available.
Comprehensive imaging demonstrates each site of injury, including its displacement and signs of instability, as well as base-line anatomic features, including bone quality and morphology.
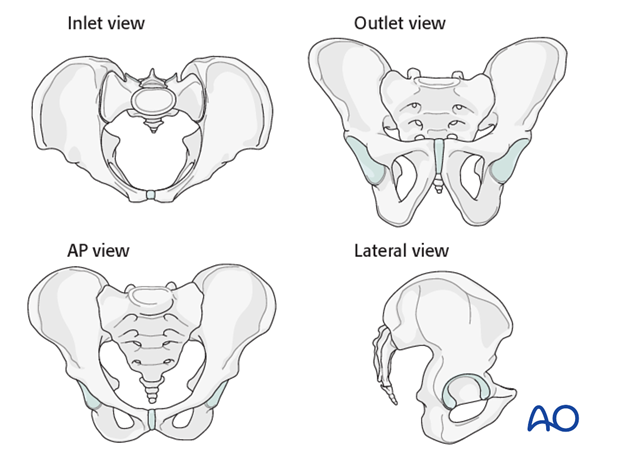
Essential C-arm views for ISS
In addition to proper AP, inlet, and outlet views, a true lateral radiograph centered on S1 is essential for IS screw insertion.
The true lateral x-ray shows the midline profile of the sacral promontory, and the iliac cortical densities, which mark the anterosuperior surface of the ala.
Confirm that the lateral view is indeed true, without rotation. The sciatic notch outlines should be superimposed.
C-arm set-up, and resulting images should finalized after the patient is anesthetized and positioned, before sterile drapes are applied.
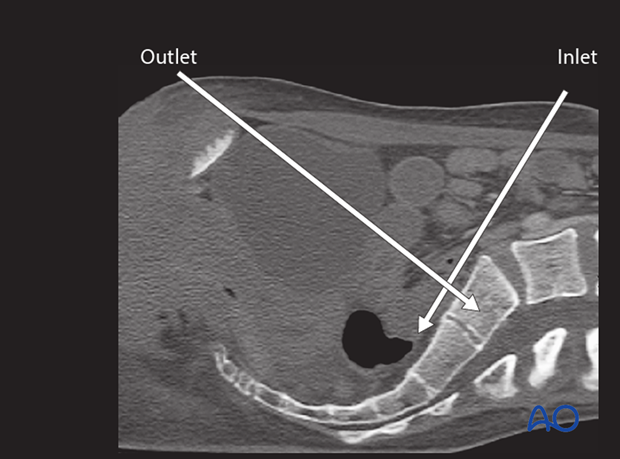
Patient-specific inlet & outlet views
Individual variation of pelvic inclination is significant enough that customized inlet and outlet angles should be chosen for use during ISS. These are based upon a midline sagittal CT reconstruction showing the sacrum. The inlet angle should be tangent to the anterior cortex of S1. The outlet angle is perpendicular to the “midline” of the trapezoidal S1 body. The C-arm must be centered over the site of interest.
An optimal outlet view shows the upper border of the pubis overlying the second sacral vertebra.
Intraoperative C-arm imaging
During setup for surgery, it is important to confirm the adequacy of C-arm imaging. This is essential to avoid errors in ISS placement.
The following should be clearly identifiable:
- sacral foramina in outlet view (outlet view)
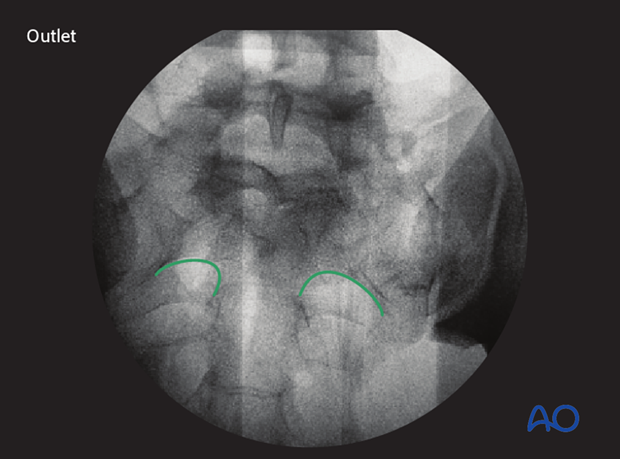
- spinal canal (inlet view)
- S1 body (inlet view)
If these structures cannot be clearly seen, a safe trajectory for the iliosacral screw cannot be determined. Fluoroscopically guided fixation must be postponed or replaced with an open procedure. (Obese patients, extensive bowel gas, and/or overlying radiographic contrast material are typical problems.).

Location of S1 nerve root tunnels
Good quality fluoroscopic views indicate the course of upper sacral nerve root tunnels.
In the outlet view, the appearance is similar to a hip spica cast, with its upper part formed by the midline sacral spinal canal, and the root tunnels being the legs of the spica.
In the inlet view, the root tunnels travel from central to anterolateral, exiting through anterior cortical lucencies.
On the lateral view the S1 root tunnel is caudal/posterior to the iliac cortical density, beneath the superior cortex of the sacral ala.
4. Sacral anatomy variations
Variable in utero segmentation of the lumbo-sacral somites produces abnormal (“dysmorphic”) upper sacral anatomy in approximately one-third of patients. These variations must be recognized because they compromise normally safe intraosseous pathways for ISS.
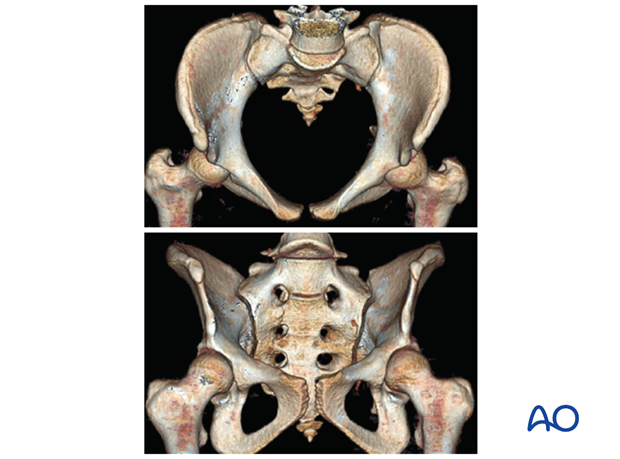
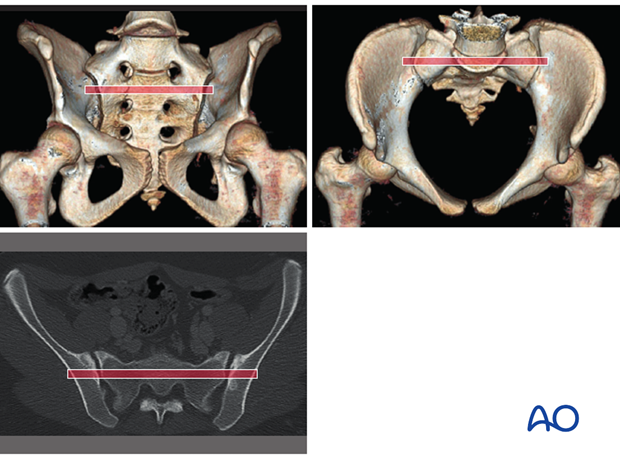
Normal vs. dysmorphic sacral anatomy
The upper images show a normal pelvis; the lower ones are of a dysmorphic pelvis.
Notice, on the 3D CTs, the differences in sacral alar anatomy, with corresponding upper sacral segment deficiencies on the dysmorphic axial CT view.
In such cases, the second sacral level may be better for an iliosacral screw
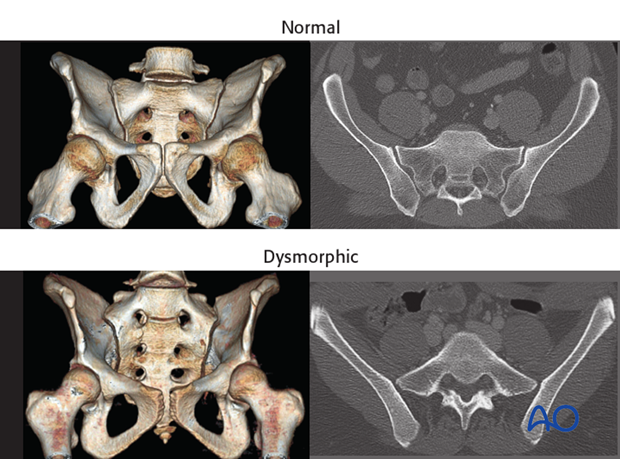
Features of dysmorphic pelvis
Sacral deformities may be unilateral or bilateral. Bilateral dysmorphism may be symmetrical, or not.
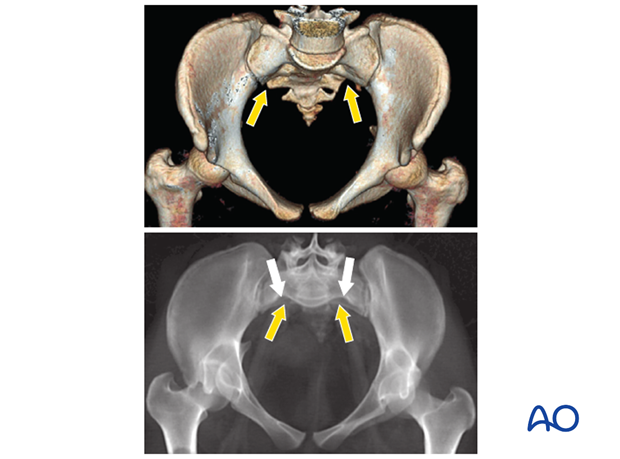
This case show an individual with symmetrical upper sacral dysmorphism.
The lumbosacral disc is near the level of the iliac crests, not below them as is normal. There is a residual disc between the upper and second sacral segments. The uppermost anterior sacral foramina are not round, as the lower ones are. The superior alar slope is steeper, from medial to lateral, and from posterior to anterior.
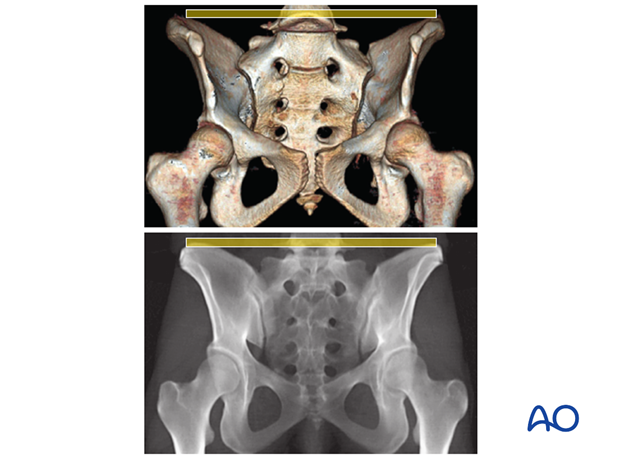
The upper sacral alar anterior cortical limit appears as an indentation (white arrows) relative to the alar anterior cortical of the second sacral segment (yellow arrows). The upper and second sacral alar anterior cortical limits are different but easily seen on the inlet view. The surgeon must understand these differences and then visualize them under image intensifier in the operating room because iliosacral screws must remain posterior to these alar cortical limits.
5. Safe screw channels for SI joint fixation
Placement of iliosacral screws should be planned on pre-operative CTs, and confirmed with post-reduction fluoroscopic images obtained intra-operatively.
ISS should be perpendicular to the plane of instability, entirely within the bone, and avoid the nerve root tunnels.
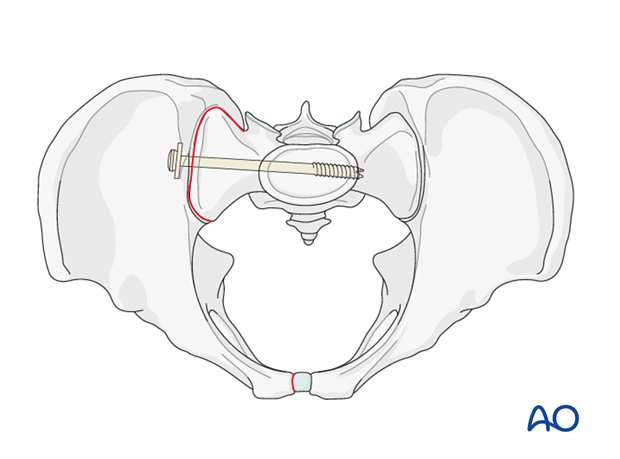
For SI joint fixation, the ISS is inserted perpendicular to the SI joint, and extends beyond the midline of the sacral body.
For sacral fractures, the ISS is horizontal, allowing it to be inserted to or through the contralateral SI joint, to optimize fixation on both sides of the sacrum.
Patients with normal anatomy
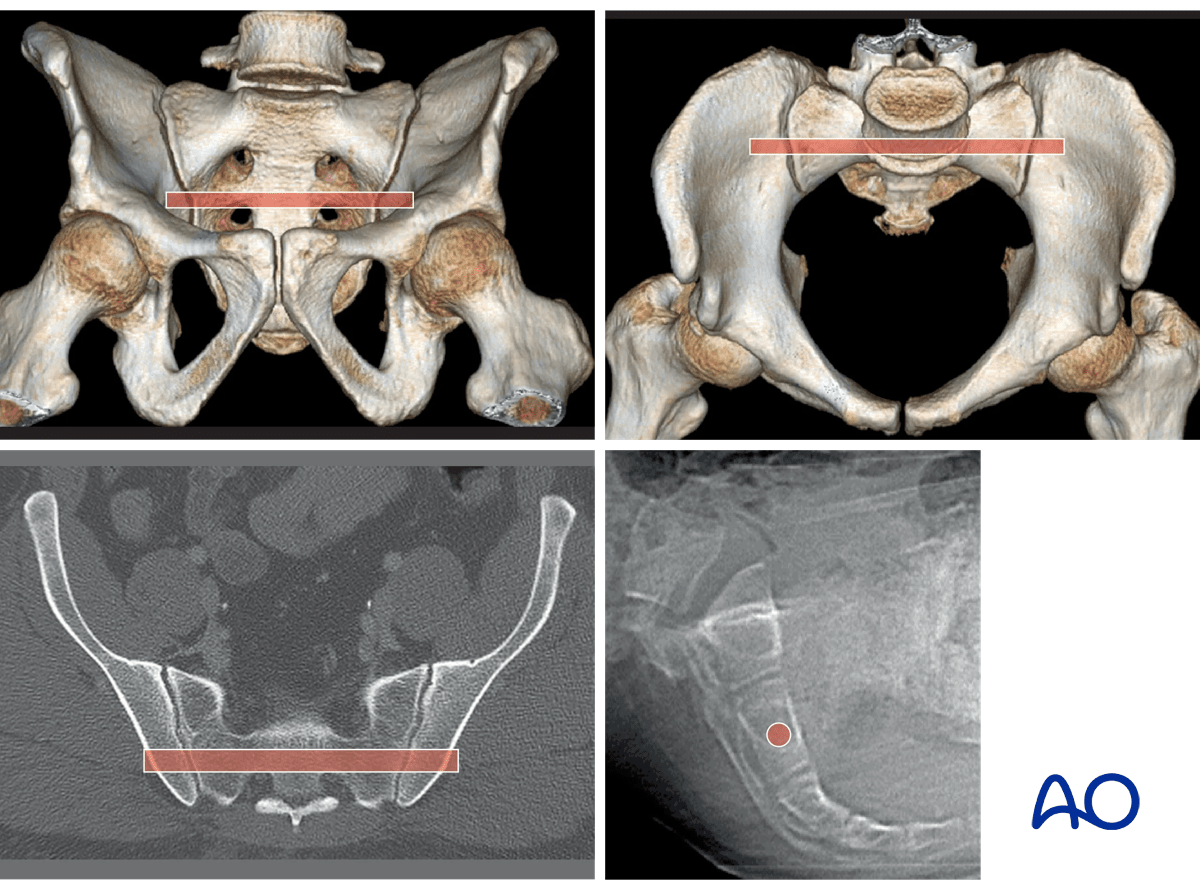
The yellow “tubes” superimposed on outlet and inlet 3D CTs show typical channels for SI joint fixation – perpendicular to the plane of the SI joint.

These images illustrate the channel for an S2 transsacral screw in a normal pelvis. This screw can supplement a standard SI joint screw, if required.
Patients with dysmorphic anatomy
In some cases, ISS can be inserted into a dysmorphic first sacral segment, using increased caudal to cranial and posterior to anterior angulation.
Note the narrowness of the safe passage through the sacral ala at this level, with the channel close and parallel to the anterior cortex, to avoid entering the spinal canal.
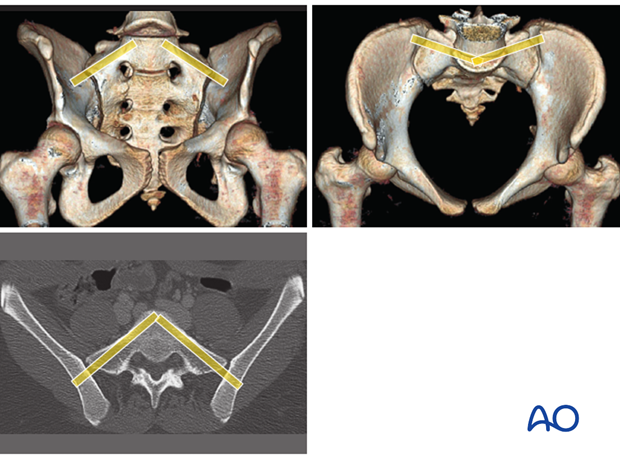
If an S2 screw will be used as well, it should be inserted second, as it will overlie the notched anterior cortex of S1 on the inlet view, and interfere with tracking the S1 screw insertion.
6. Reduction
The details of reduction depend upon the specific fracture type.
Reduction of B fractures
Unilateral Type B injuries, because of their intact posterior hinge and stable contralateral hemipelvis, can often be reduced by closed manipulation, perhaps aided by temporary external fixation.
Correction of rotational deformity should reduce the SI joint or “hinged” sacral fracture
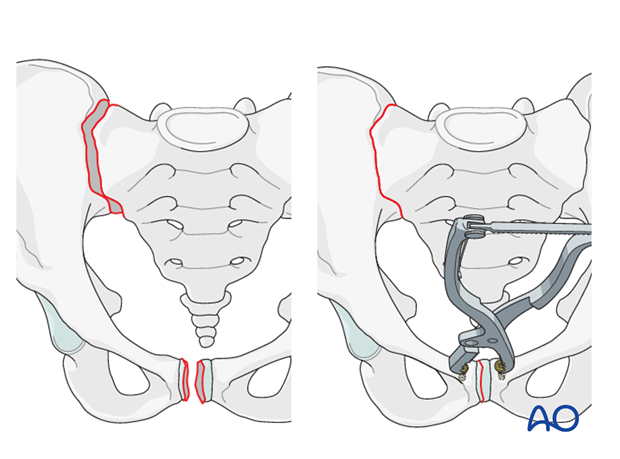
Preliminary open reduction of a disrupted pubic symphysis illustrates its utility for reducing the SI joint in B1 injuries.
Adequacy of SI reduction should be confirmed by fluoroscopy prior to definitive fixation of the symphysis, and before proceeding with ISS insertion.
If slight widening of the SI joint remains, without vertical or horizontal translation on inlet and outlet views, the ISS will compress the joint and complete the reduction.
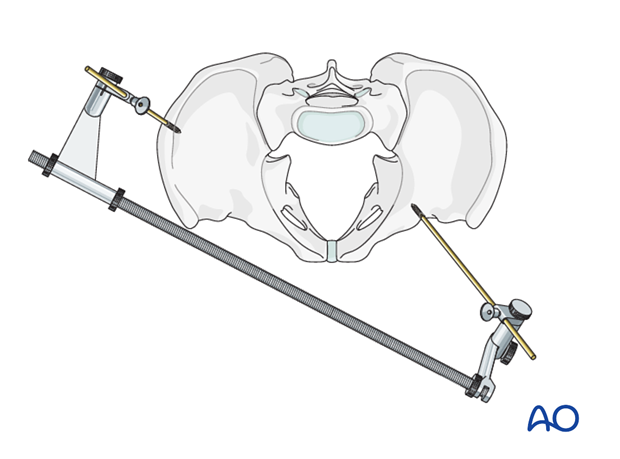
Type B2 pelvic ring injuries can often be reduced, if necessary, by externally rotating the internally rotated hemipelvis with an external fixator applied to produce or maintain distraction.
In this case, the obliquely applied external fixator corrects internal rotation and flexion of the left hemipelvis, thus reducing the ipsilateral SI joint prior to ISS insertion. The fixator can be left until pubic ramus fractures heal, or replaced with internal fixation.
Reduction of C fractures
Displacement of type C injuries is usually complex, with multiplanar displacement of the mobile hemipelvis. Typically translational (shearing) displacement occurs through the sites of injury.
- Posteriorly
- Vertically
- Laterally (distracting the injury)
- Rotational deformity may also be present.
Closed manipulative techniques, aided with percutaneous instrumentation, may succeed in achieving a satisfactory reduction, which can be stabilized provisionally (e.g. with external fixation) during ISS placement.
However, such indirect reductions, especially if delayed, are less likely to succeed, so that and appropriate open reduction must be planned. This must respect local soft tissue status as well as the injury configuration and any associated ring disruptions.
Unless the need for open reduction is convincing, closed manipulative reduction is reasonable to try first.
However, the importance of (nearly) anatomical alignment must be remembered. If it has not been achieved, through closed or open means, an alternative fixation procedure should be used instead of ISS.
Closed reduction
Correction of vertical displacement may be challenging to achieve.
In cases of vertical displacement where the contralateral hemipelvis is intact, the patient can be placed on a radiolucent traction table. Traction is applied until correct reduction can be seen on AP outlet and inlet projections. The traction is then maintained until fixation is completed.
If a radiolucent traction table is not available, the reduction can be performed with manual traction and a temporary external fixator or C-clamp.
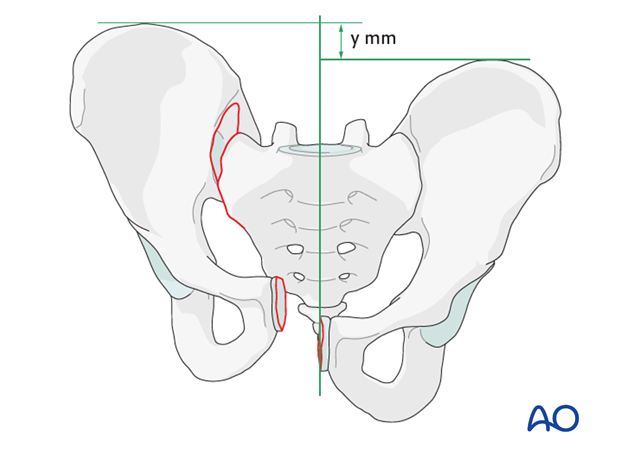
For internal and external rotation of the hemi pelvis, Schanz screws can be inserted in the supra acetabular area and/or ala. These are then used as joy sticks until reduction is achieved. The Schanz pins are held in place either manually or by attachment to an external frame (as an external fixator) until fixation is completed.
For open book fractures, it is advisable to fix both feet together in internal rotation.
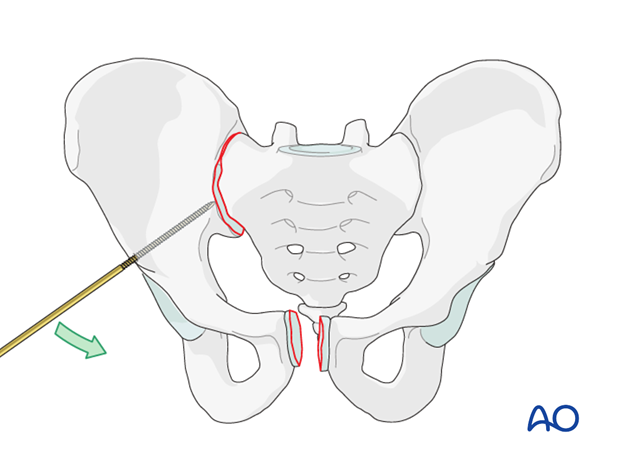
If only a minor lateral displacement is present, a ball spike can be used through a separate incision to reduce the SI joint. Temporary external fixation or C-clamp may be used for provisional stabilization during ISS insertion, if the reduction is adequate.
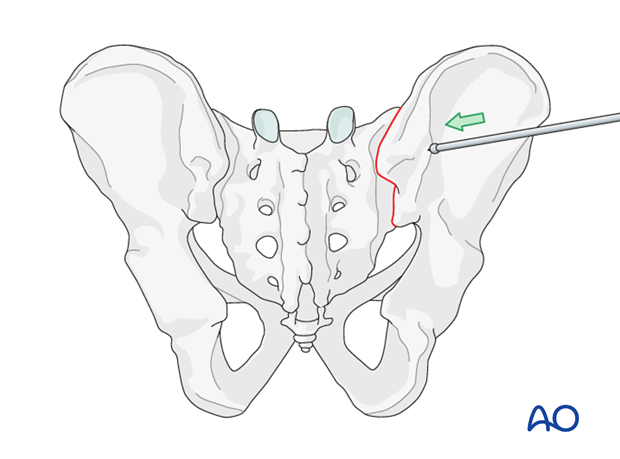
Open reduction
In case close reduction is unsuccessful, an open reduction is necessary before ISS fixation. The choice of open reduction approach (anterior vs. posterior) and technique will depend upon the individual fracture location and its configuration.
7. ISS Fixation Procedure
Before beginning an ISS screw fixation procedure, appropriate preoperative planning for screw type and location needs to be completed.
Landmarks for true lateral sacral image
On the true lateral projection, identify the S1 body and iliac cortical densities (ICDs), here overlapping correctly.
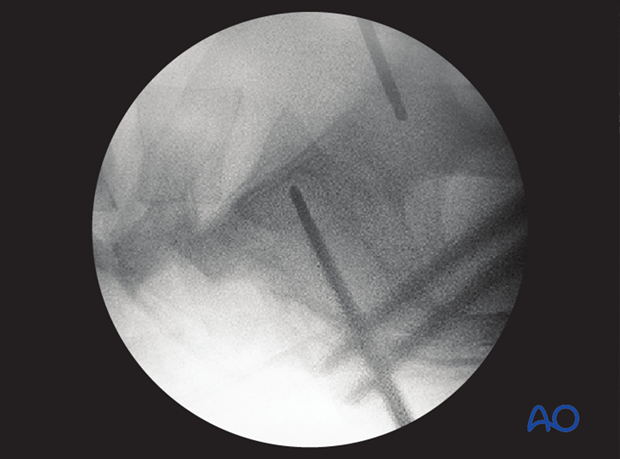
If double contours of the iliac cortical densities (ICDs) are visible, as shown here, it is likely that the radiographic central ray is striking the pelvis obliquely. The C-arm should be adjusted to obtain a true lateral view, with superimposed ICDs and S1 cortices.
(This assumes that inlet and outlet views show that the pelvic reduction is anatomical.)
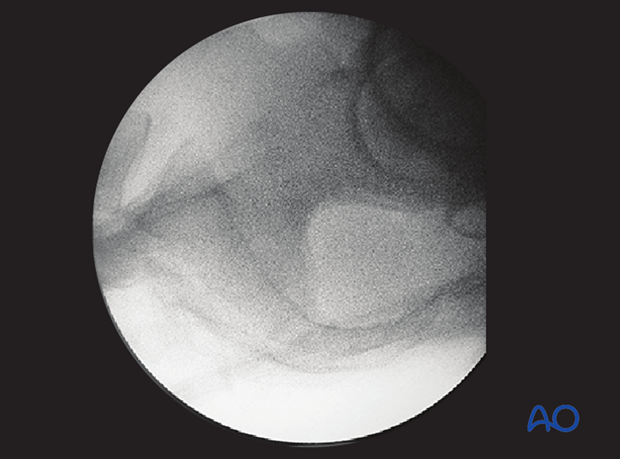
Location of screw entry point
The entry point should be anterior in S1 and inferior to the iliac cortical density (ICD), which parallels the sacral alar slope, usually slightly caudal and posterior. The ICD thus marks the anterosuperior boundary of the safe zone for an iliosacral screw which may injure the L5 nerve root if it penetrates this cortex.
An instrument handle can help to target the desired entry site for the guidewire.
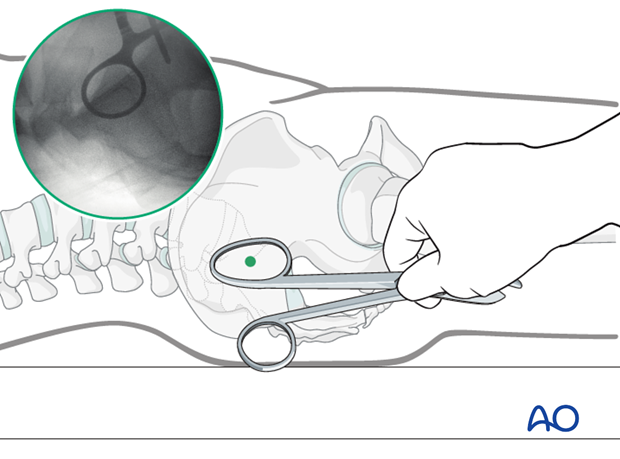
Incision
A stab incision is made at the identified site. The underlying tissues are dissected down to bone, by spreading with an appropriate blunt clamp, or with scissors if necessary.
There should be sufficient room for a protective drill sleeve, and for the planned screw and washer.
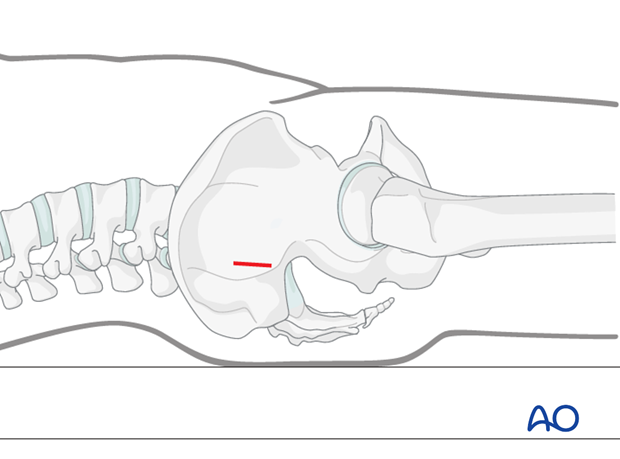
Guidewire insertion
A guidewire is tapped 2-3 mm, or drilled (oscillating mode preferred) into the planned screw entry point. This is monitored by X-ray on the true lateral projection.
Note that with a true lateral view, the power source and chuck must be removed from guidewire or drill to assess their position.
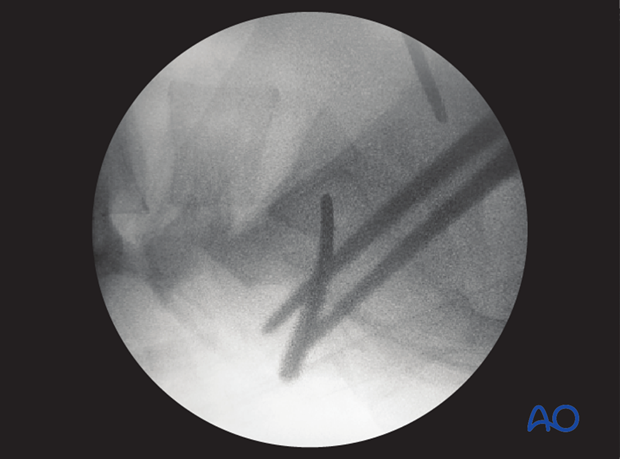
The guidewire is advanced 1 cm into the sacral ala.

The position and trajectory of the guidewire is checked in inlet and…
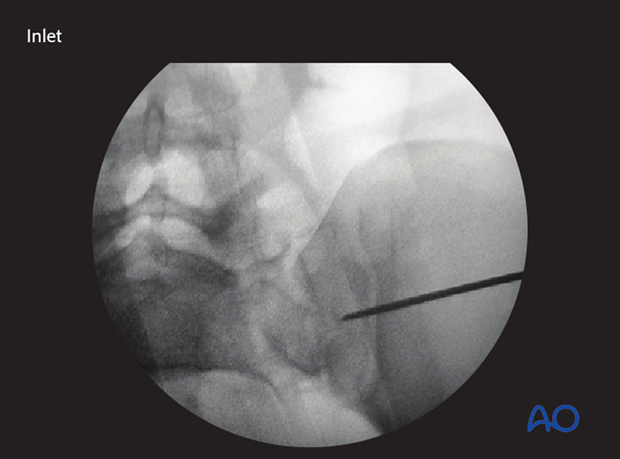
…outlet projection.
When the guidewire tip is just lateral to the neural foramen on the outlet view, pause to confirm that its position is satisfactory.
The desired trajectory is within but close to the anterior alar cortex on the inlet view, and cranial to the ventral foramen of the 1st sacral nerve root.
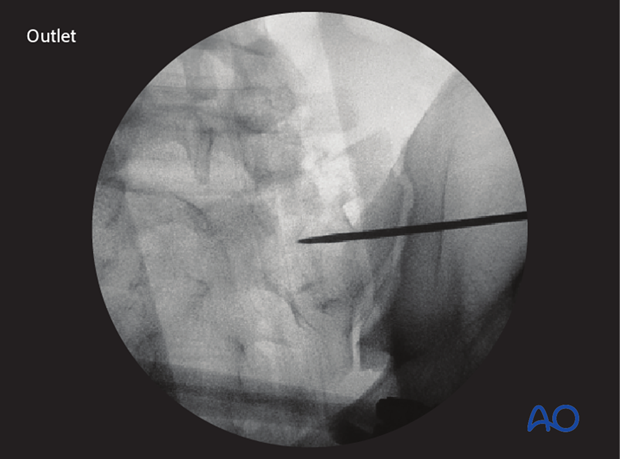
If the trajectory of the guidewire would compromise either the sacral foramen or the spinal canal, the guidewire is removed and then reinserted from a similar entry point but in the corrected trajectory.
Alternatively, the guidewire is left in place as a reference and a new one is inserted along the correct trajectory.
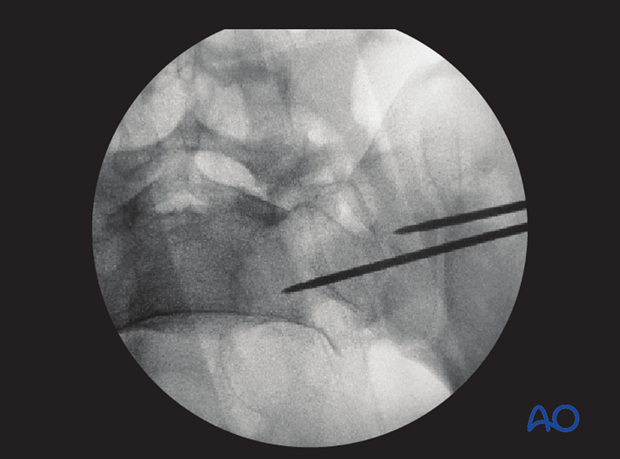
When a safe trajectory for the guidewire is confirmed, it is further advanced to the contralateral lateral border of the first sacral body.
When the guide wire reaches the center of the sacral body, the position is again verified in true lateral, inlet, and outlet view.
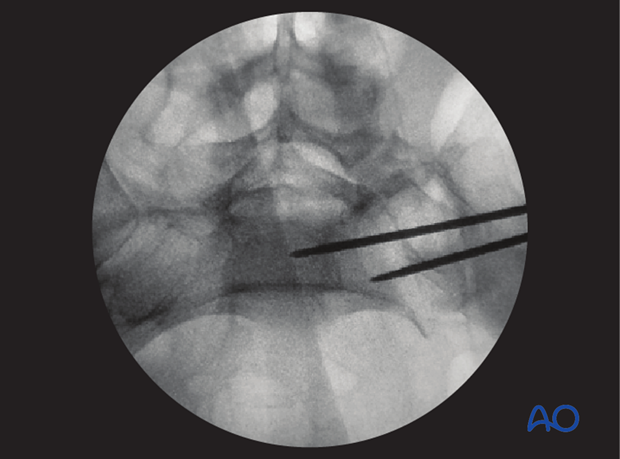
The wire must be far enough from cortices and neural foramina to accommodate the thread diameter of the planned screw.
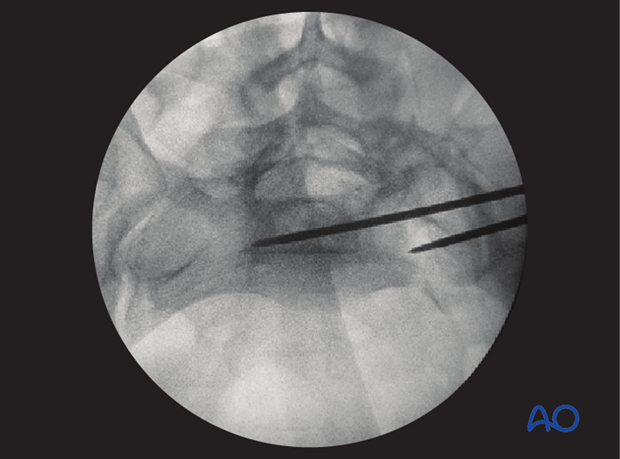
Screw insertion
The screw length is measured with a ruler or gauge suitable for the guidewire, and compared with the pre-operatively estimated length.
An appropriate screw hole is drilled over the guidewire, which should remain anchored in the bone, if it has been advanced far enough beyond the intended screw tip site.
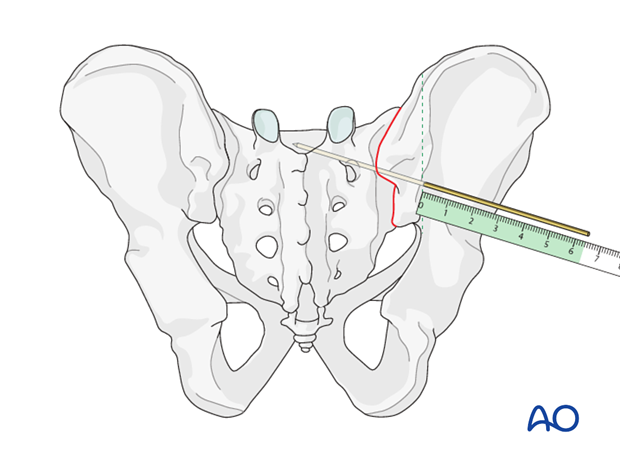
The chosen cannulated lag screw is inserted with a washer.
In case of comminution, fully threaded screws may be preferred to avoid over-compression of a sacral fracture. They may also be used to supplement an initial lag screw.
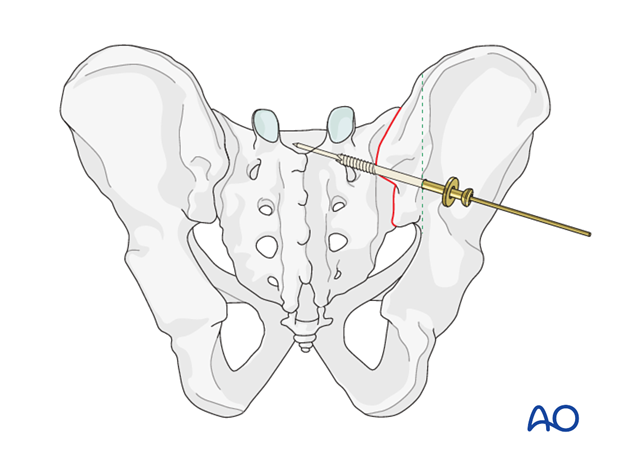
The guidewire is removed.

Pifall: Intrusion of screw head into illium
Excessive tightening of the screw will cause intrusion of the screw head into the ilium.
Such errors, which compromise fixation, are more likely with osteoporotic bone.
To help prevent such intrusion, use of a washer should be routine.
With the C-arm rotated so its central ray is tangential to the ilium at the ISS insertion site, an excellent view of bone surface, washer, and screw head is available. This permits precise tightening of the screw without intrusion of washer and screw head through the iliac cortex.
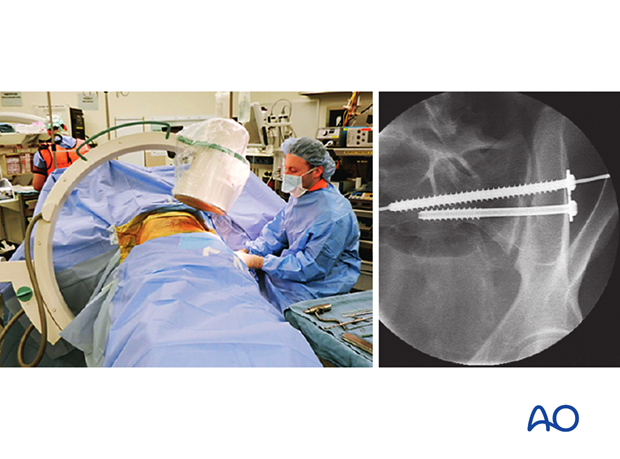
8. Check of osteosynthesis
Upon completion of the ISS procedure, use multiple C-arm images to assess
- Reduction of SI joint
- Over-all pelvic ring alignment & symmetry
- Position of each screw, within cortical boundaries, and avoiding intra-osseous neural pathways
- Confirm that all guidewires and reduction aids have been removed
- Alignment and fixation of any associated ring injuries
Assessment of ISS requires AP, Inlet, outlet, and true lateral images of the posterior pelvis. Especially for bilateral injuries (B3, C2, and C3) radiographs that show the entire pelvic ring are necessary to confirm correction of complex deformities.
Make sure that any additional injury sites have been treated as planned.

9. Aftercare following open reduction and fixation
Postoperative blood test
After pelvic surgery, routine hemoglobin and electrolyte check out should be performed the first day after surgery and corrected if necessary.
Bowel function and food
After extensile approaches in the anterior pelvis, the bowel function may be temporarily compromised. This temporary paralytic ileus generally does not need specific treatment beyond withholding food and drink until bowel function recovers.
Analgesics
Adequate analgesia is important. Non pharmacologic pain management should be considered as well (eg. local cooling and psychological support).
Anticoagulation
Prophylaxis for deep vein thrombosis (DVT) and pulmonary embolus is routine unless contraindicated. The optimal duration of DVT prophylaxis in this setting remains unproven, but in general it should be continued until the patient can actively walk (typically 4-6 weeks).
Drains
Dressings should be removed and wounds checked after 48h, with wound care according to surgeon's preference.
Wound dressing
Dressings should be removed and wounds checked after 48h, with wound care according to surgeon's preference.
Physiotherapy
The following guidelines regarding physiotherapy must be adapted to the individual patient and injury.
It is important that the surgeon decide how much mechanical loading is appropriate for each patient's pelvic ring fixation. This must be communicated to physical therapy and nursing staff.
For all patients, proper respiratory physiotherapy can help to prevent pulmonary complications and is highly recommended.
Upper extremity and bed mobility exercises should begin as soon as possible, with protection against pelvic loading as necessary.
Mobilization can usually begin the day after surgery unless significant instability is present.
Generally, the patient can start to sit the first day after surgery and begin passive and active assisted exercises.
For unilateral injuries, gait training with a walking frame or crutches can begin as soon as the patient is able to stand with limited weight bearing on the unstable side.
In unstable unilateral pelvic injuries, weight bearing on the injured side should be limited to "touch down" (weight of leg). Assistance with leg lifting in transfers may be necessary.
Progressive weight bearing can begin according to anticipated healing. Significant weight bearing is usually possible by 6 week but use of crutches may need to be continued for three months. It should remembered that pelvic fractures usually heal within 6-8 weeks, but that primarily ligamentous injuries may need longer protection (3-4 months).
Fracture healing and pelvic alignment are monitored by regular X-rays every 4-6 weeks until healing is complete.
Bilateral unstable pelvic fractures
Extra precautions are necessary for patients with bilaterally unstable pelvic fractures. Physiotherapy of the torso and upper extremity should begin as soon as possible. This enables these patients to become independent in transfer from bed to chair. For the first few weeks, wheelchair ambulation may be necessary. After 3-4 weeks walking exercises in a swimming pool are started.
After 6 weeks, if pain allows, the patient can start walking with a three point gait, with less weight bearing on the more unstable side.
Full weight bearing is possible after complete healing of the bony or ligamentous legions, typically not before 12 weeks.













