ORIF - ilium
1. Introduction
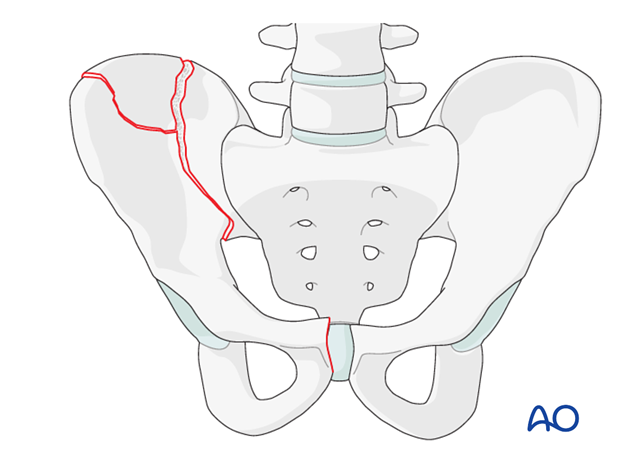
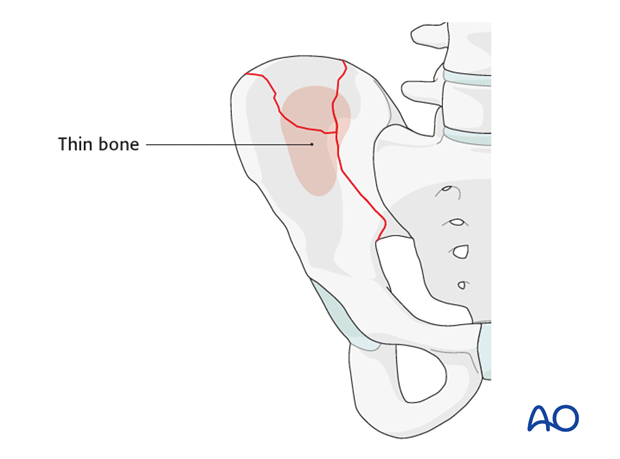
Fractures of the ilium that disrupt the continuity of the pelvic ring result in an unstable hemipelvis. Iliac fractures commonly occur in the posterior portion of the ilium as the bone is the weakest in this region.
Unstable iliac fractures are distinct from pure iliac fractures that do not disrupt pelvic ring stability. Fractures of the ilium may extend into the sacroiliac joint but these fracture types are addressed elsewhere. Iliac fractures that involve the acetabulum are described in the acetabulum module.
2. Patient preparation and approach
Patient preparation
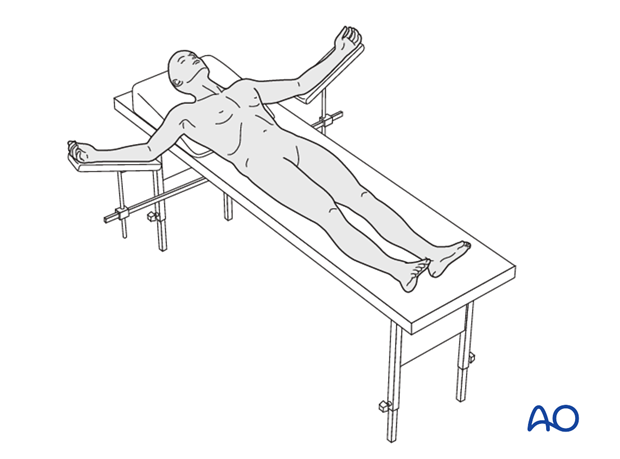
This procedure is performed with the patient in a supine position.
Approach
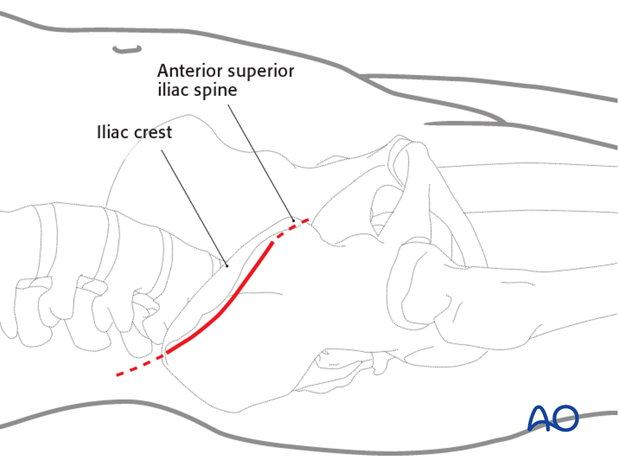
For this procedure an anterior approach to the iliac wing and SI joint is used.
3. Reduction
Options for reduction
Options for reduction include closed and open reduction techniques. The decision for open or closed reduction is dependent on the fracture pattern, patient anatomy, and surgeon's preference.
Closed reduction techniques
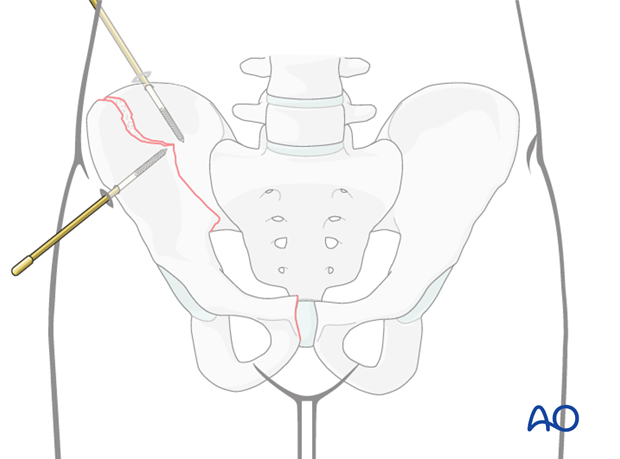
Schanz screws may be inserted percutaneously under X-ray guidance into the ilium and the fracture fragments.
These screws can be used as joy sticks for manipulating individual fragments.
Open reduction techniques
A variety of reduction tools may be used to manipulate the fracture fragments.
A clamp (eg Farabeuf) may be used to grasp the iliac crest to manipulate and reduce the fragment.
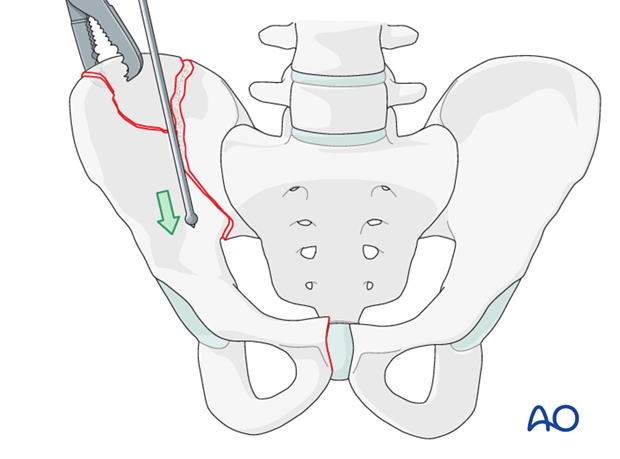
A ball spike pusher may also be used to aid in reduction. The ball spike may be placed along the pelvic brim (as illustrated) or alternatively, the ball spike may be placed at the anterior inferior iliac spine directed posteriorly.
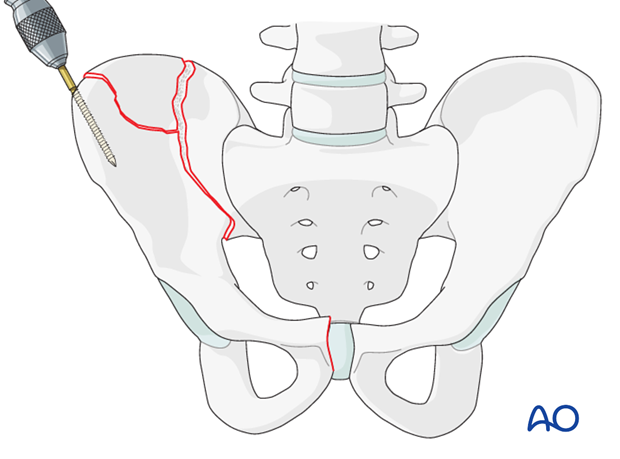
Schanz screw
A Schanz screw (joy stick) may be inserted into a fragment of the iliac wing for reduction of the fracture fragment.
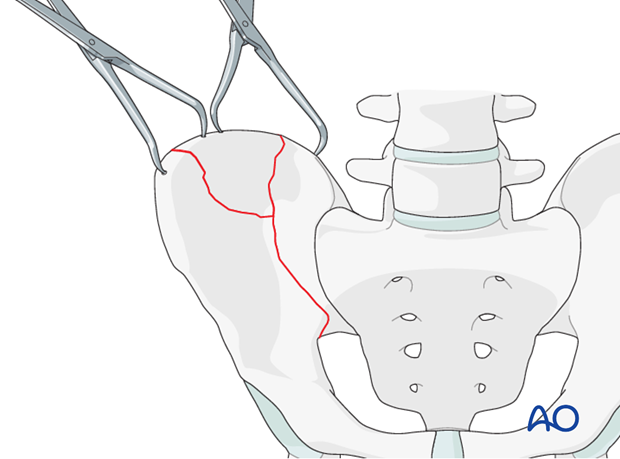
Use of pointed reduction forceps
Another method to aid in reduction is to use a pointed reduction clamp at the iliac crest to manipulate and reduce the fracture fragment.
Use of a Farabeuf or Jungbluth clamp
Alternatively, screws may be placed into the fracture fragments and grasped using either a Farabeuf or a Jungbluth clamp to achieve reduction.

Assessment of reduction
For closed techniques, the reduction is verified with X-rays in multiple planes.
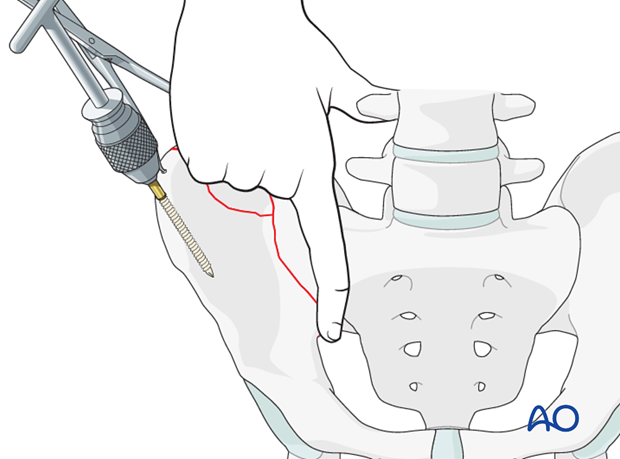
For open techniques, the reduction is verified with X-rays and also by palpation. Palpate the reduction along the ilium and at the pelvic brim.
4. Fixation
Options for fixation
After reduction is achieved, the fracture may be stabilized with plates and/or interfragmentary lag screws.
The choice of fixation is dependent on the fracture pattern, anatomy, and surgeon's preference.
Insertion of a contoured plate for stabilization
Plates are applied with balanced fixation on both sides of the fracture. The best bone for fixation is along the iliac crest and adjacent to the pelvic brim. Between these regions, the bone is thin and it is difficult to achieve satisfactory fixation.
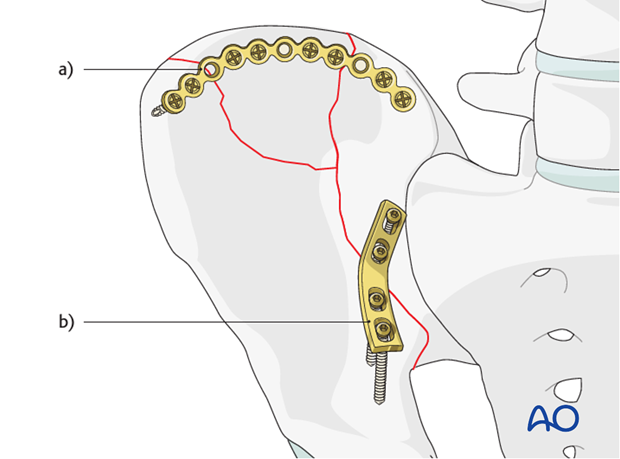
After reduction, a contoured reconstruction plate may be placed along the iliac crest.
The plate may be placed on the inner surface of the ilium (a) spanning the fracture lines with ideally two screws on each side of the fracture.
A plate may also be applied across the fracture, in compression mode, at the level of the pelvic brim (b).
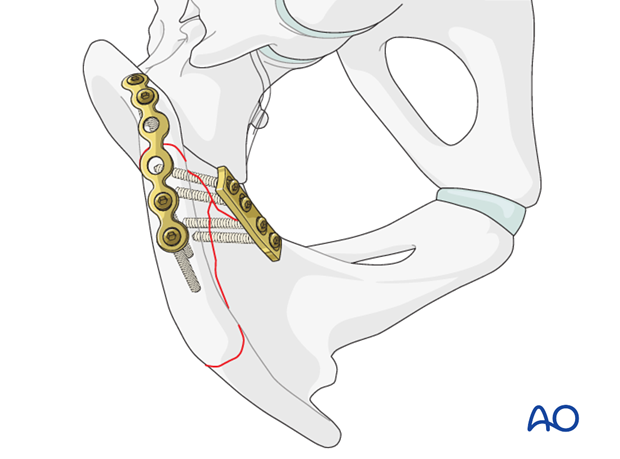
Alternatively, a plate may be applied directly to the superior surface of iliac crest. (The other plate is on the pelvic brim.)
Intramedullary screws for fixation of the crest
Fracture lines that extend to the iliac crest may be stabilized with 3.5 mm interfragmentary lag screws.
These screws are placed in an intramedullary fashion between the inner and outer table of the ilium.
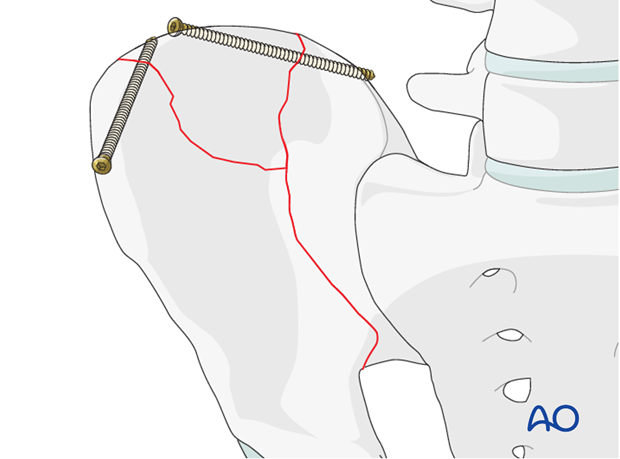
Depending on the fracture pattern, a combination of intramedullary screws and plates may be used.
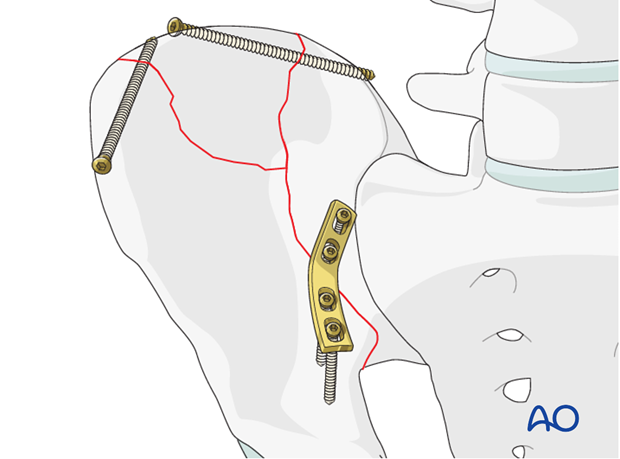
Another method of fixation is a long intramedullary lag screw that is placed from the anterior inferior iliac spine extending to the posterior ilium. This is typically a 6.5 mm or 7.3 mm partially threaded cannulated screw.
X-rays
After completion of internal fixation, confirm the final reduction and hardware position intraoperatively by AP, inlet and outlet radiographic imaging.

5. Aftercare following open reduction and fixation
Postoperative blood test
After pelvic surgery, routine hemoglobin and electrolyte check out should be performed the first day after surgery and corrected if necessary.
Bowel function and food
After extensile approaches in the anterior pelvis, the bowel function may be temporarily compromised. This temporary paralytic ileus generally does not need specific treatment beyond withholding food and drink until bowel function recovers.
Analgesics
Adequate analgesia is important. Non pharmacologic pain management should be considered as well (eg. local cooling and psychological support).
Anticoagulation
Prophylaxis for deep vein thrombosis (DVT) and pulmonary embolus is routine unless contraindicated. The optimal duration of DVT prophylaxis in this setting remains unproven, but in general it should be continued until the patient can actively walk (typically 4-6 weeks).
Drains
Dressings should be removed and wounds checked after 48h, with wound care according to surgeon's preference.
Wound dressing
Dressings should be removed and wounds checked after 48h, with wound care according to surgeon's preference.
Physiotherapy
The following guidelines regarding physiotherapy must be adapted to the individual patient and injury.
It is important that the surgeon decide how much mechanical loading is appropriate for each patient's pelvic ring fixation. This must be communicated to physical therapy and nursing staff.
For all patients, proper respiratory physiotherapy can help to prevent pulmonary complications and is highly recommended.
Upper extremity and bed mobility exercises should begin as soon as possible, with protection against pelvic loading as necessary.
Mobilization can usually begin the day after surgery unless significant instability is present.
Generally, the patient can start to sit the first day after surgery and begin passive and active assisted exercises.
For unilateral injuries, gait training with a walking frame or crutches can begin as soon as the patient is able to stand with limited weight bearing on the unstable side.
In unstable unilateral pelvic injuries, weight bearing on the injured side should be limited to "touch down" (weight of leg). Assistance with leg lifting in transfers may be necessary.
Progressive weight bearing can begin according to anticipated healing. Significant weight bearing is usually possible by 6 week but use of crutches may need to be continued for three months. It should remembered that pelvic fractures usually heal within 6-8 weeks, but that primarily ligamentous injuries may need longer protection (3-4 months).
Fracture healing and pelvic alignment are monitored by regular X-rays every 4-6 weeks until healing is complete.
Bilateral unstable pelvic fractures
Extra precautions are necessary for patients with bilaterally unstable pelvic fractures. Physiotherapy of the torso and upper extremity should begin as soon as possible. This enables these patients to become independent in transfer from bed to chair. For the first few weeks, wheelchair ambulation may be necessary. After 3-4 weeks walking exercises in a swimming pool are started.
After 6 weeks, if pain allows, the patient can start walking with a three point gait, with less weight bearing on the more unstable side.
Full weight bearing is possible after complete healing of the bony or ligamentous legions, typically not before 12 weeks.













