Patient examination
1. Clinical examination
A detailed history of the traumatic event should be recorded to understand better the forces involved, which may help anticipate patterns of injury and soft tissue compromise.
Identifying pre-injury ambulatory status, nicotine use, occupational status, diabetic vasculopathy, previous bony or soft tissue injuries, or existing arthritis helps guide decision-making and estimate outcomes.
Clinical examination should include evaluation of:
- Neurological status
- Vascular status
- Skin integrity
- Swelling
- Deformities
- Stability/crepitation
- Location of pain
Neurovascular status
- Decreased sensation, typically at the plantar surface of the foot
- Neuropraxia due to trauma
Vascular status
- Decreased blood profusion to the toes
- Damage to the digital arteries
Skin integrity
- Puncture, lacerations, degloving
- Open fracture or severe soft tissue injury
Swelling
What is observed:
- Midfoot/forefoot swelling and blistering
What it indicates:
- Any bony or ligamentous mid/forefoot injury
- Potential compartment syndrome

What is observed:
- General swelling of the foot
What it indicates:
- Multiple fractures
- Potential compartment syndrome
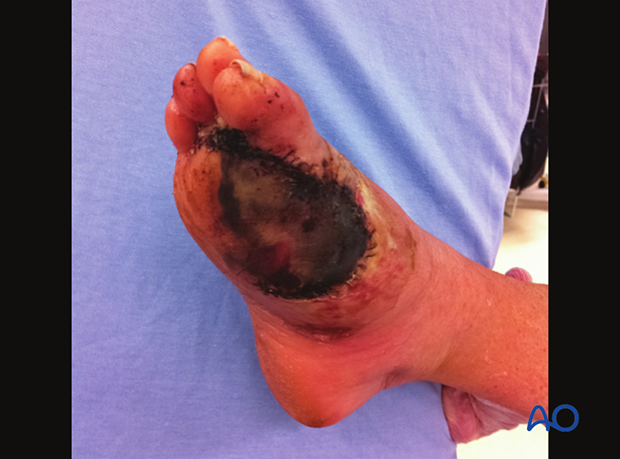
This case shows severe soft-tissue swelling and dead tissue after a forefoot crush injury.
Deformities/instabilities
What is observed:
- Deviation from normal anatomy
What it indicates:
- Displaced fractures or ligamentous injuries.
Instability tests will sometimes need to be performed with a regional block or under general anesthesia.
Pain location
Pain will indicate injuries to underlying structures.
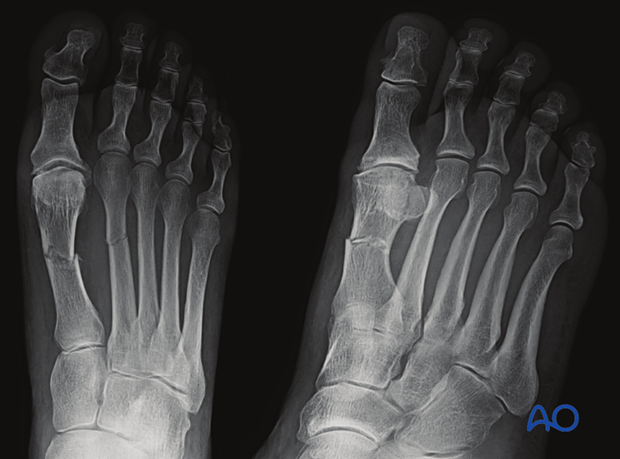
2. Radiographs
The following views should be taken:
- Lateral view
- AP view
- 45° Oblique view
The joint proximal and distal to the suspected injury should be included in the radiograph.
Fractures and dislocations are usually evident in these views.
Fractures of the proximal metatarsals should raise suspicion for Chopart and/or Lisfranc injuries.
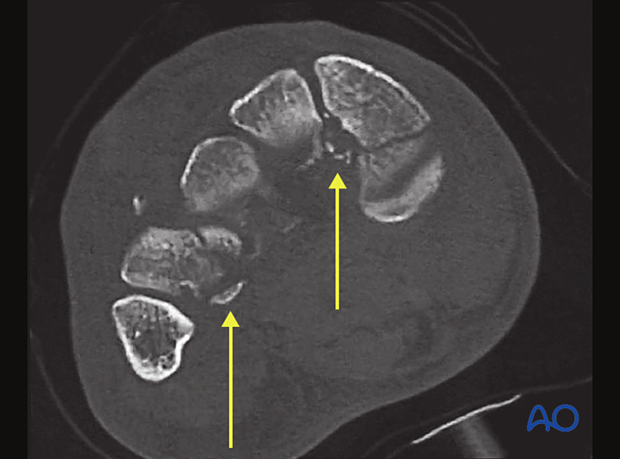
3. CT imaging
CT images are particularly useful to identify:
- Avulsion fracture of the proximal second metatarsal (Lisfranc)
- Concomitant midfoot and hindfoot fractures
- Articular fracture morphology
What is seen
- Avulsion fractures of the proximal second to fourth metatarsals
What it indicates
- Lisfranc injury