K-wire fixation
1. Principles
Introduction
K-wires can be applied to many different fracture patterns. Considerations include fracture obliquity, comminution, and soft tissue status.
As K-wires cannot compress the fracture, the fracture needs to be reduced before K-wire insertion.
Threaded K-wires are generally not preferred as they are more challenging to extract and potentially maintain fracture gaps.
K-wires should be sized appropriately to the bone. Typically wires thicker than 2.0 mm are not needed.
This procedure can be performed for fractures of all distal metatarsals 1–4.
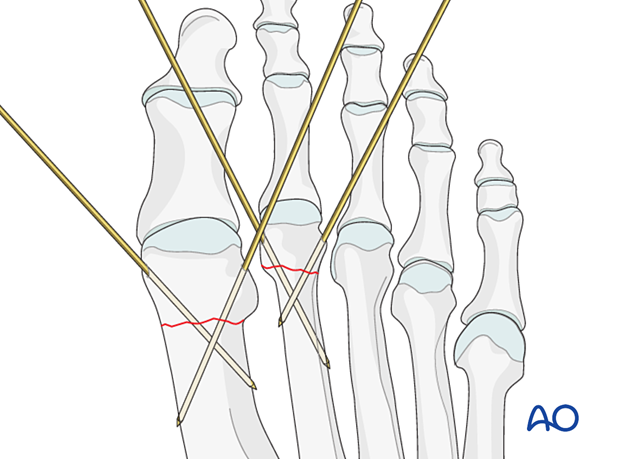
Anatomical considerations
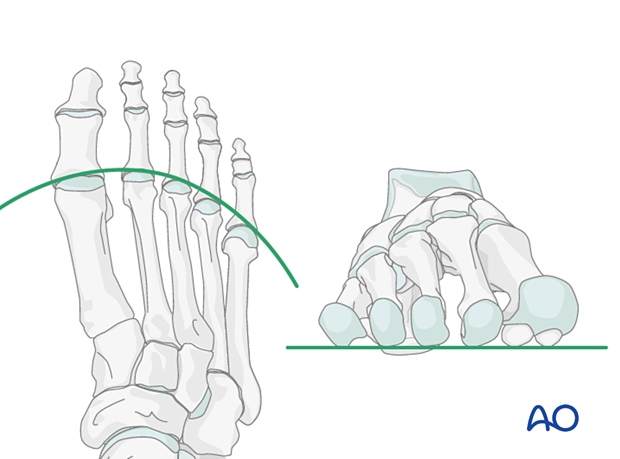
Proper alignment of the metatarsal heads is a critical goal in restoring the forefoot mechanics.
A normal curved “cascade” (Lelièvre’s parabola) appearance, which is symmetric with the other foot, is mandatory on the AP view. See illustration. This symmetry ensures that the normal length of the metatarsal is restored.
It is also critical to restore the metatarsals in their axial or horizontal plane so that all the metatarsal heads are on the same level in the axial view.
Any malalignment, particularly flexion, will recreate focally high pressure during the stance phase and toe-off, resulting in pain and subsequent callus formation.
The sesamoids, rather than the first metatarsal head, bear weight in the first row. Therefore, one must look at the sesamoid level in establishing the alignment in the axial or horizontal plane of the first metatarsal.
Timing of surgery
The timing of surgery is influenced by the soft tissue injury and the patient's physiologic status.

2. K-wire patterns
Depending on the size of the fragment, more than one K-wire may be needed to provide stability to the fracture.
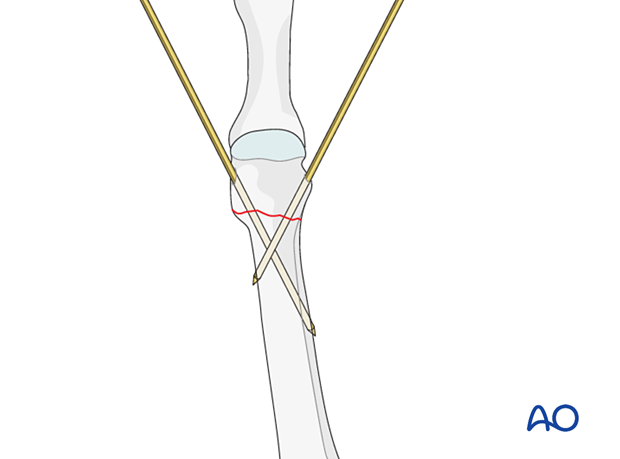
Both K-wires can be inserted from the same side of the bone in a diverging or crossing pattern.
Divergent K-wires prevent postoperative distraction of the fracture.
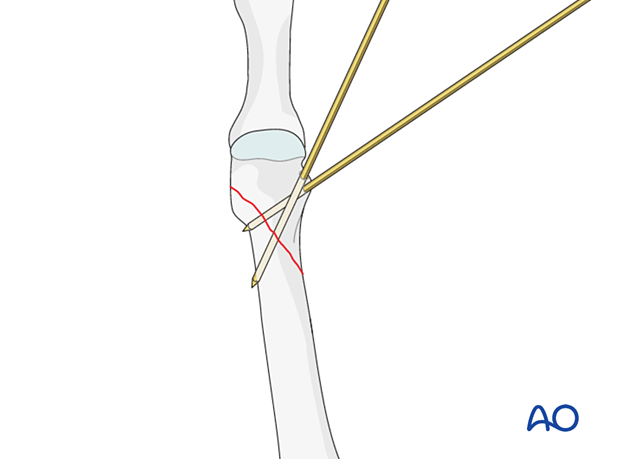
K-wires can also be inserted in a crossing manner from opposite sides.
The two K-wires should not cross at the fracture site as this would be a less stable construct.
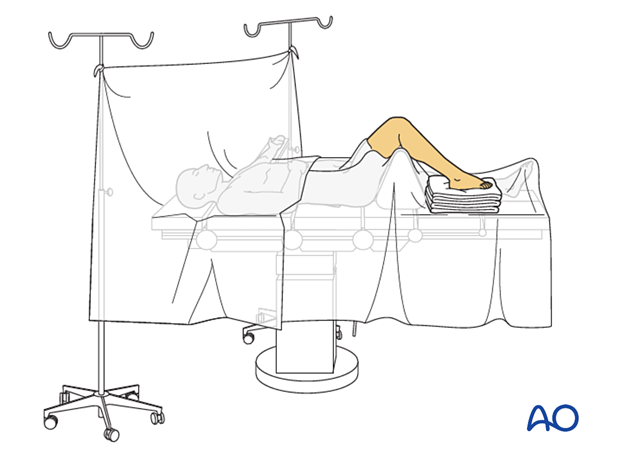
3. Patient preparation
This procedure is typically performed with the patient placed supine with the knee flexed at 90°.
4. Reduction
Indirect reduction
Closed reduction of these fractures is challenging. The primary deformity is in the sagittal plane, which may improve slightly with longitudinal traction.
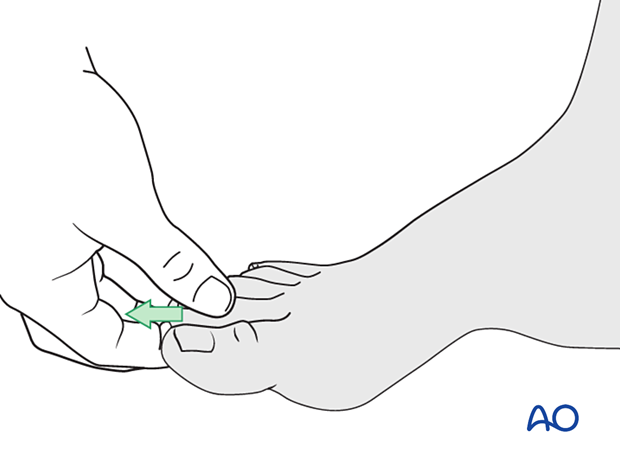
Grasp the digit’s terminus and use a combination of axial and angular traction to exaggerate the deformity.
Traction is maintained until the fixation is complete.
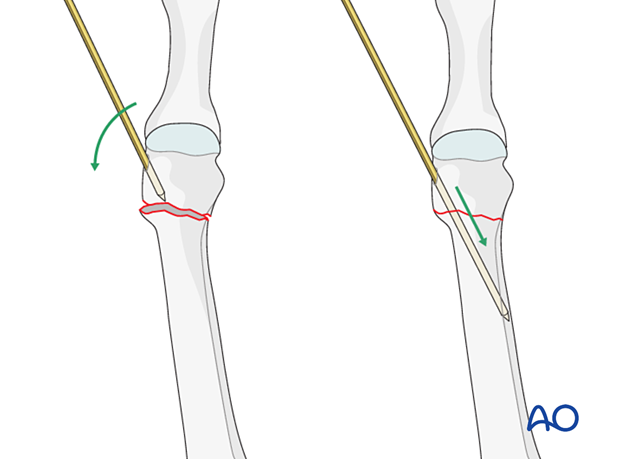
Direct reduction
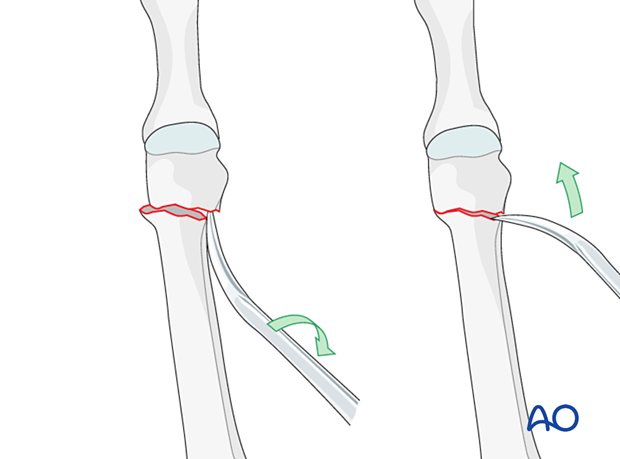
K-wires can be inserted into the distal fragment and used as a joystick.
Once reduction has been obtained, the K-wire can be further inserted to secure the reduction.
If needed, use a percutaneously placed periosteal elevator as a lever to reduce the fracture.
Restore anatomical axial rotation, length, and angulation.
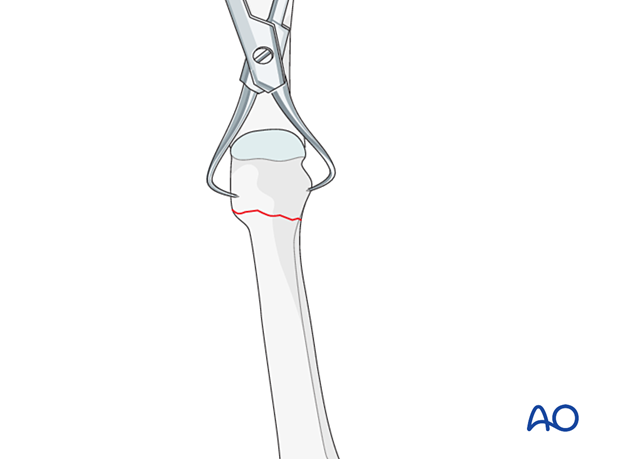
A small, pointed reduction forceps can be used to grasp and manipulate the distal fragment. Be careful not to apply excessive force as this can lead to fragmentation.
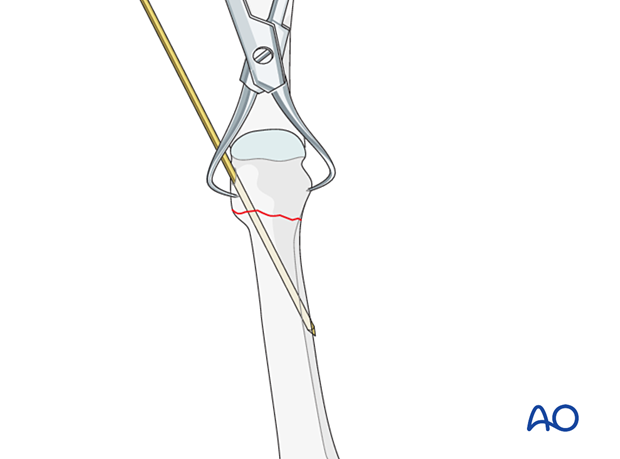
Intraoperative confirmation of reduction
Use image intensification to confirm the reduction.
5. K-wire insertion
K-wires are inserted percutaneously according to the preoperative plan.
Caution should be made to prevent thermal injury when inserting a K-wire in dense bone.
Intraoperative fluoroscopy is particularly useful to aid the correct position of the K-wire.
The stability of the reduction is assessed, and if needed, additional K-wires are inserted.
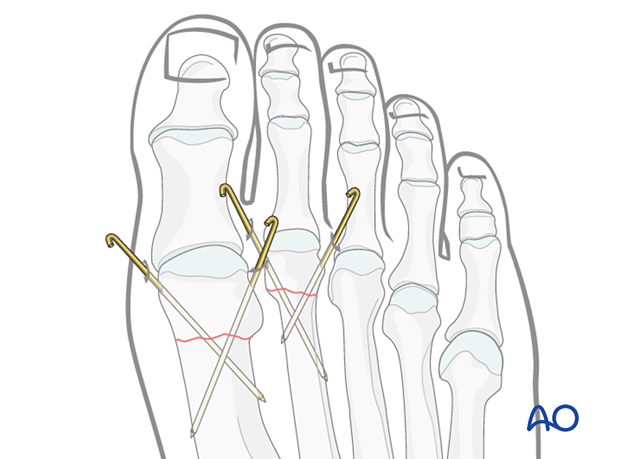
When satisfactory stability is achieved, cut the K-wires leaving adequate K-wire protruding through the skin to facilitate removal.
Assess the skin pin interface and release any excessive skin traction.
6. Aftercare
The skin-pin interface should be well padded but with dressings that can be readily removed to inspect for pin-site infection.
Immediate postoperative treatment is rest, ice, and elevation.
The patient should be encouraged to begin early weight-bearing as permitted by the stability of the fracture.
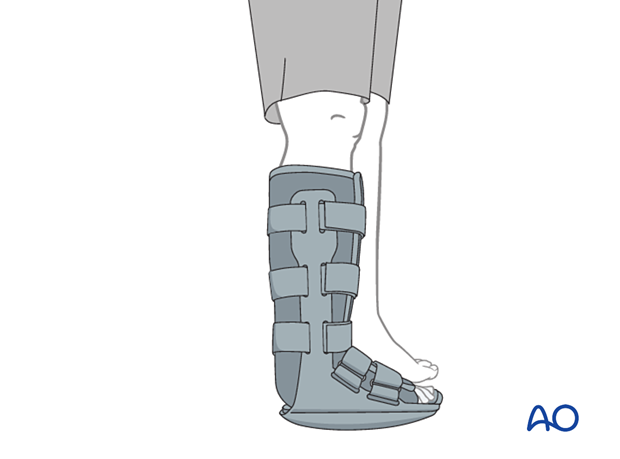
A stiff-soled shoe or a cam walker can be used to protect the surgical site. Patients must exercise their ankle and subtalar joints out of the cam walker to prevent stiffness (eg, by stretching their Achilles).
X-ray the foot at six weeks to confirm satisfactory union and remove K-wires if present. Once the fracture is united, the orthosis may be gradually discontinued.