Extended deltopectoral approach to the humeral shaft
1. Introduction
The (anterior) extended deltopectoral approach can be used to access almost any humeral shaft fracture involving the proximal 4/5.
2. Anatomy of the upper arm
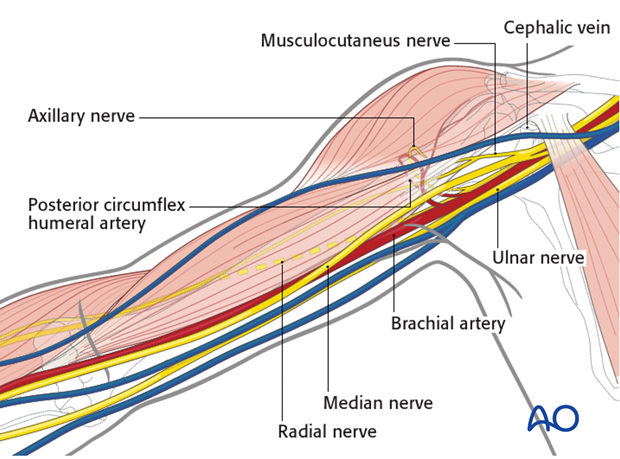
The course of the following neurovascular structures should be kept in mind:
- Cephalic vein
- Posterior circumflex humeral artery
- Axillary nerve
- Musculocutaneus nerve
- Radial nerve
- Median nerve
- Ulnar nerve
- Brachial artery
Further neurovascular structures, eg the brachial plexus, are only at risk if there is a vigorous retraction.
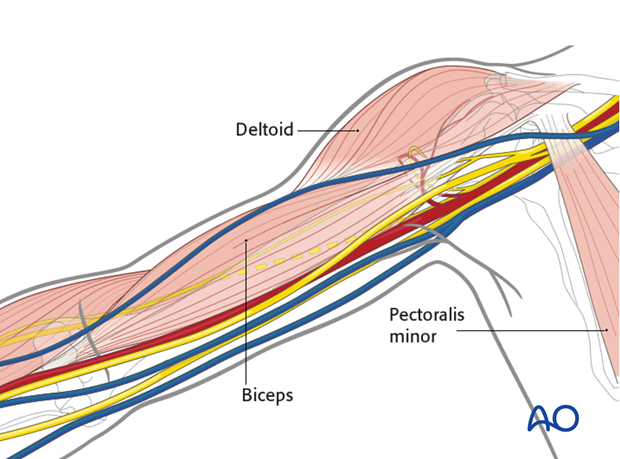
Anatomy of the arm showing the neurovascular structures in relation to the following muscles:
- Deltoid
- Biceps
- Pectoralis minor
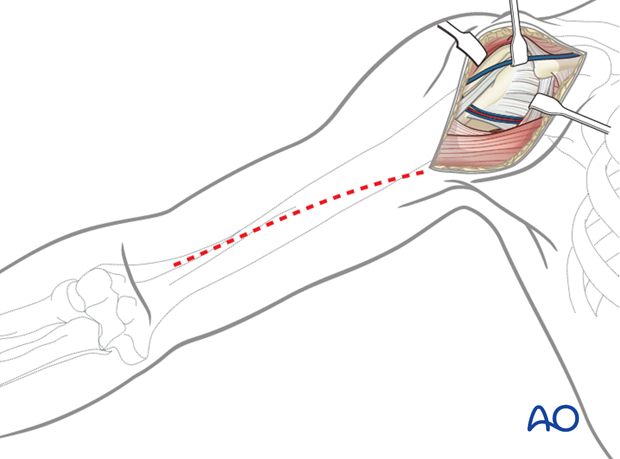
3. Skin incision
Palpable anatomical landmarks for the anterior deltopectoral approach are:
- Coracoid process
- Proximal humeral shaft (at the level of the axilla)
- Midshaft of the humerus
- Radial epicondyle of the distal humerus
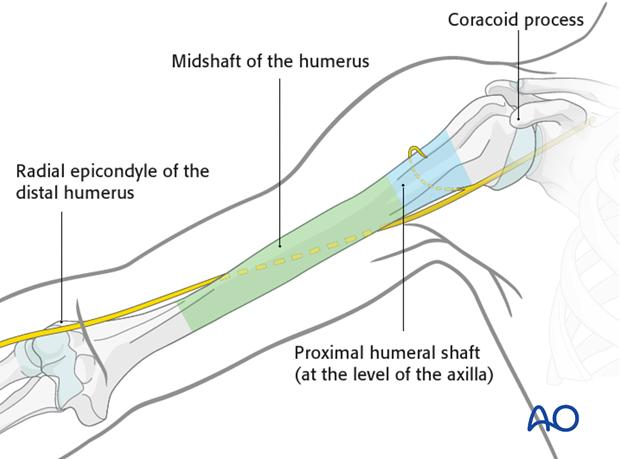
The skin incision starts at the coracoid process and follows the humeral shaft distally towards the lateral epicondyle. The length of the skin incision depends on the planned plate length.
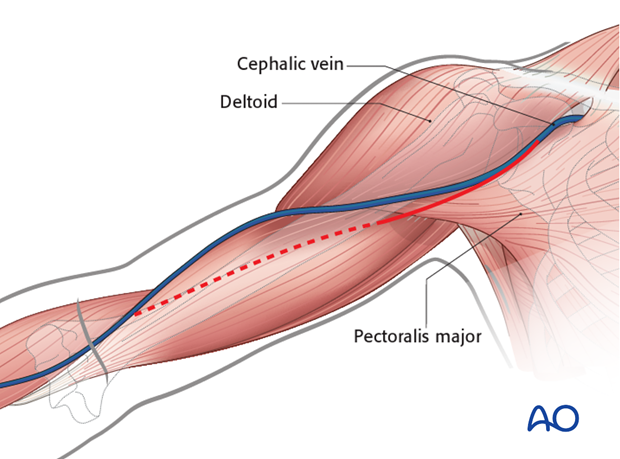
4. Exposure of the superficial fascia
Expose the deltopectoral groove with the cephalic vein. These structures can be identified by:
- The course of the muscle fibers
- The cephalic vein itself
- Fat tissue surrounding the vein
For better exposure it is recommended to dissect at the lateral border of the pectoralis major.
If in doubt, look for the deltopectoral groove at the proximal and/or distal end of the skin incision. (The sulcus is slightly more pronounced and in cases of revision surgery less scarred.)
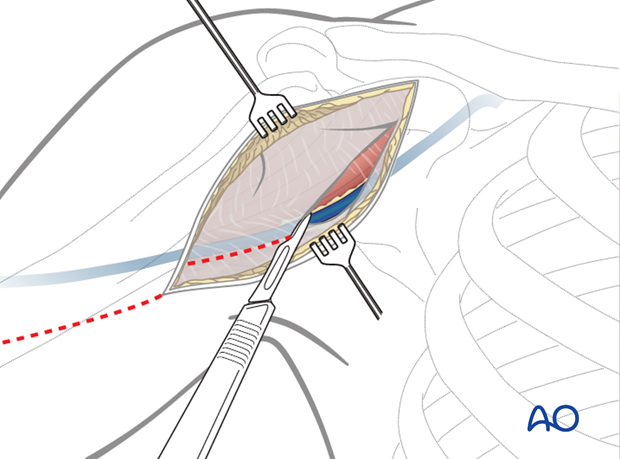
5. Dissection down to the deltopectoral groove
Retract the cephalic vein laterally and open along the groove. If retracted laterally, the anatomical drainage of blood from the deltoid muscle is respected but it is at risk of damage by retractors during surgery. In any case, preserve the cephalic vein to reduce the surgical edema of the limb.
Failure to find the deltopectoral groove can lead to difficulty in dissection of the deltoid and possibly to denervation of the anterior portion of the deltoid.
Bluntly dissect between and under the deltoid and pectoralis muscles down to expose the clavipectoral fascia.
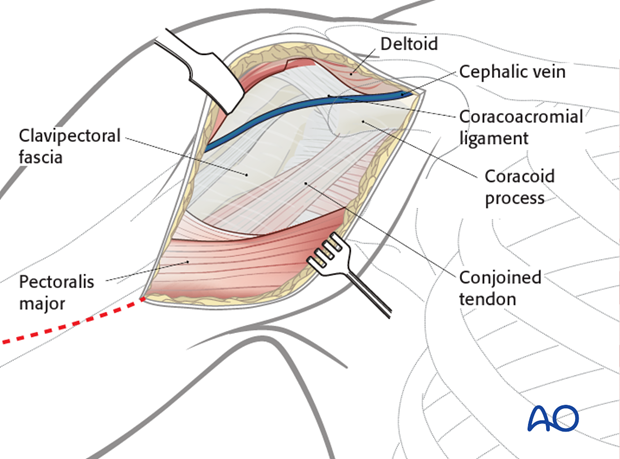
6. Exposure of the deep layers
Identify the coracoid process and the conjoined tendon.
Incise the clavipectoral fascia lateral to the conjoined tendon and inferior the coracoacromial ligament.
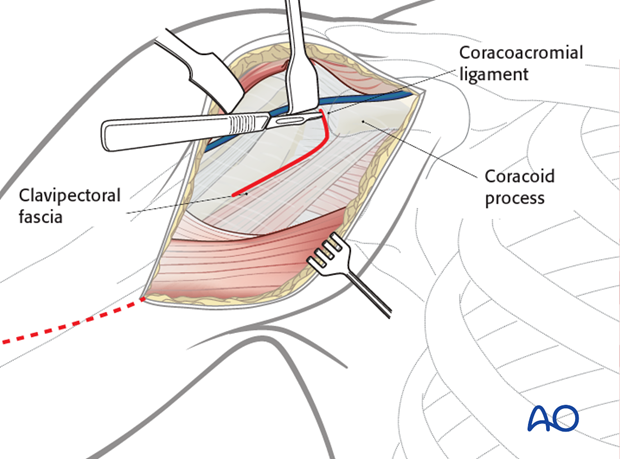
Retract the deltoid muscle laterally using a delta (modified Hohmann) retractor and the conjoined tendon medially using a Langenbeck retractor.
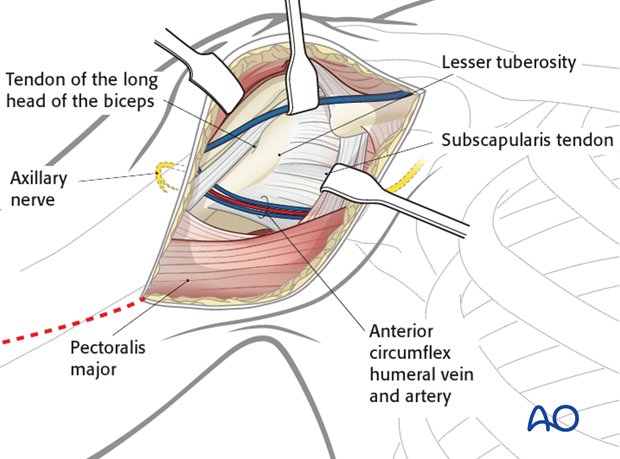
7. Exposure of the proximal humerus
Expose the main fragments of the fracture and the anatomical key structures such as
- Tuberosities
- Insertion of pectoralis major (latissimus dorsi and teres major)
- Insertion of the deltoid muscle
- Biceps
- Brachioradialis
Pitfall: axillary nerve damage
Be aware of retractor positioning (Roux or Hohmann retractor) to prevent iatrogenic damage of the axillary nerve.
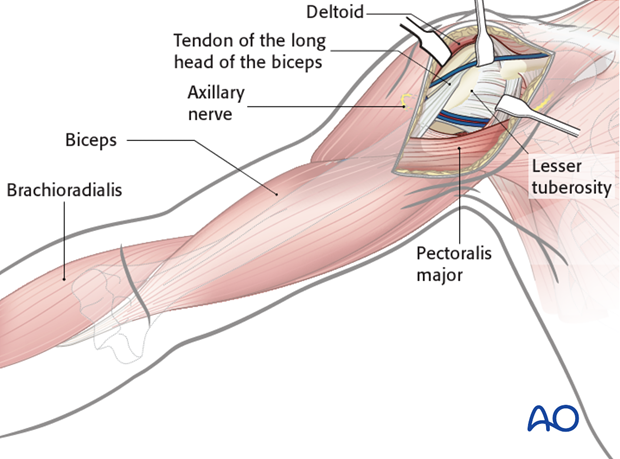
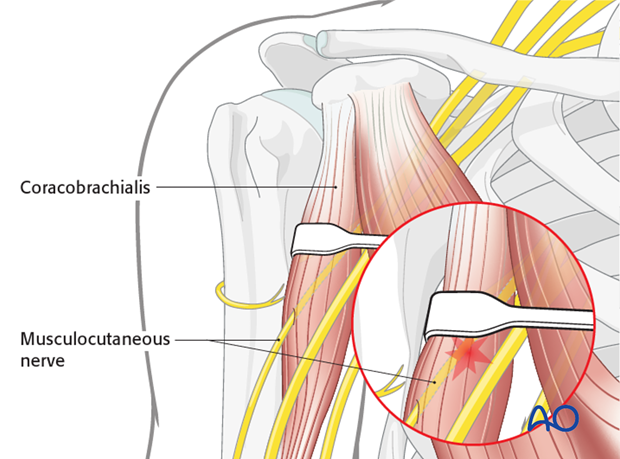
Pitfall: neurapraxia of musculocutaneous nerve
The musculocutaneous nerve enters the coracobrachialis as close as 2.5 cm distal to the tip of the coracoid. Retractors placed under the conjoined tendon can cause neurapraxia; therefore, vigorous retraction must be avoided.
Pearls
- Using an additional delta retractor might be helpful to increase exposure of the proximal humerus.
- Exposure may be increased additionally by partially releasing the insertions of deltoid and/or pectoralis major.
- Shoulder abduction decreases tension on the deltoid and makes it easier to retract laterally.
8. Distal extension of the deltopectoral approach
The deltopectoral approach can be extended distally as much as needed.
Superficial dissection
Extend the incision of the superficial fascia of the upper arm carefully between biceps/brachialis and the mobile wad distally.
Look for the lateral cutaneous nerve of the forearm crossing distally. The radial nerve is deeper. Identify the nerve in the interval between biceps and the mobile wad and follow it proximally as the incision is developed.
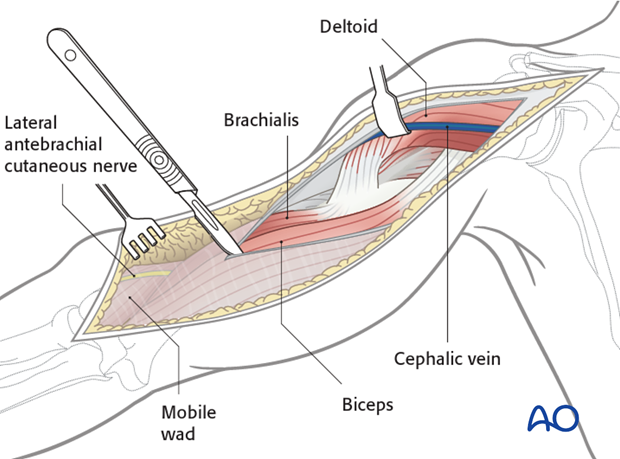
Retract the biceps medially, and the mobile wad laterally to identify the radial nerve. The brachialis is now exposed.
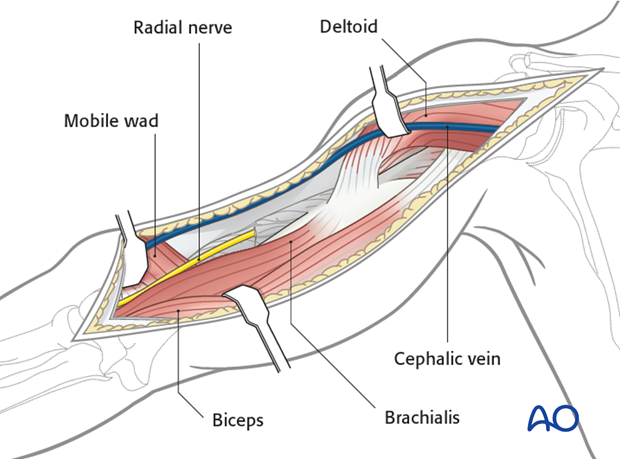
Deep dissection
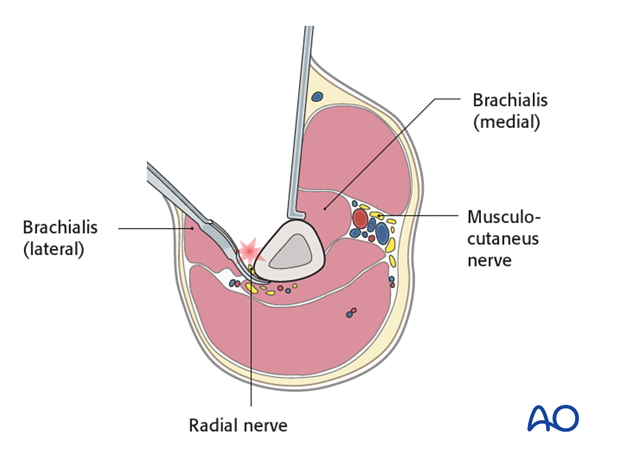
Dissect the brachialis within the neurovascular plane between the radial and the musculocutaneous nerves to maintain innervation of the brachialis.
If necessary release some of the muscle attachment proximally to allow the plate to lie on the bone.
Extend the dissection proximally, as needed, to the anterior border of the deltoid and along the deltopectoral interval.

Alternatively, the brachialis may be retracted medially. Beware that this injures the radial nerve branch to the brachialis.
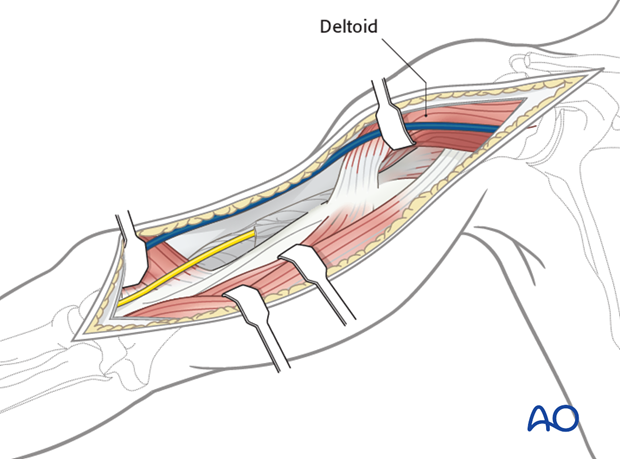
Partially release the deltoid insertion anteriorly, if necessary, and retract laterally to access the proximal humerus.
Alternatively dissect bluntly under the central deltoid insertion to allow for plate placement.
Leave as much muscle attached to bone as possible to preserve vascularity and reattach the released portion at the end of the procedure.
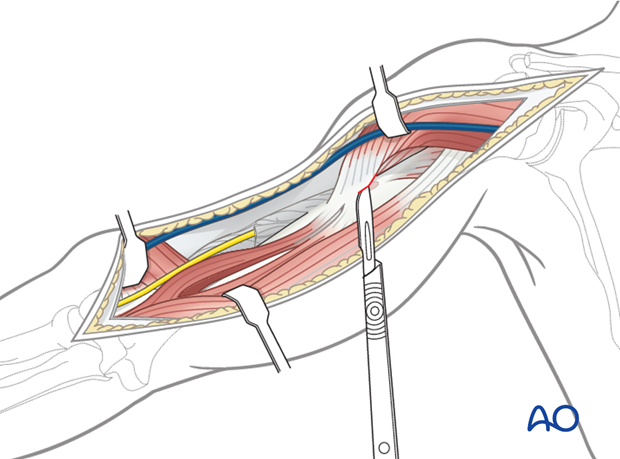
Distally, the anterior humerus has been exposed to the elbow joint, between the mobile wad and brachialis.
Mobilize the radial nerve, as needed, to access the bone. Follow the nerve to the point where it passes through the lateral intermuscular septum.

Pitfall: injury of the radial nerve
The radial nerve enters the anterior compartment by perforating the lateral intermuscular septum. The use of Hohmann retractors in the distal 2/5 of the humerus carries a high risk of iatrogenic nerve injury and should therefore be avoided.
9. Wound closure
Irrigate the wound. Placement of a drain underneath the deltoid muscle might be considered.
Close the subcutaneous tissues and the skin in layers in a standard manner.